Vol. 20 - Num. 80
Originales
¿Cómo duermen nuestros niños? Análisis de los trastornos del sueño en niños
María Álvarez Casañoa, Juana M.ª Ledesma Albarránb
aPediatra. CS Alcolea. Córdoba. España .
bPediatra. CS Delicias. Málaga. España.
Correspondencia: M Álvarez . Correo electrónico: mariaac22@hotmail.com
Cómo citar este artículo: Álvarez Casaño M, Ledesma Albarrán JM. ¿Cómo duermen nuestros niños? Análisis de los trastornos del sueño en niños. Rev Pediatr Aten Primaria. 2018;20:365-70.
Publicado en Internet: 10-10-2018 - Número de visitas: 20171
Resumen
Introducción: dada la importancia de los trastornos del sueño en la infancia, el objetivo de nuestro estudio es conocer la prevalencia de estos en la población sana.
Material y métodos: es un estudio observacional transversal descriptivo. Se realizó en el centro de Atención Primaria Las Delicias de Málaga (España). Se partió de una población a estudio correspondiente a los niños de dicho centro con edades comprendidas entre 2 y 14 años; de 2423 pacientes se seleccionaron 225, lo que constituye una muestra con una precisión del 5% y una proporción esperada del 30%. Se realizó una encuesta de preguntas con elección múltiple mediante la escala validada de trastornos del sueño de Bruni (Sleep Disturbance Scale for Children). Además, se recogieron otras variables como la presencia de patología respiratoria o el uso frecuente de aerosolterapia, para analizar si dichos pacientes con problemas respiratorios presentaban mayor prevalencia de trastornos del sueño, por posibles efectos secundarios de dicha medicación.
Resultados: el 61% del total presentó algún tipo de trastorno del sueño, predominando los problemas del sueño-vigilia (38%), seguidos por los problemas respiratorios tipo síndrome de apneas-hipopneas del sueño (18%). Presentaron problemas de inicio del sueño el 17%, hiperhidrosis el 15%, problemas del arousal el 13% y somnolencia diurna excesiva el 10%. El 23% de los niños tardan más de 30 minutos en dormirse.
Conclusiones: nuestro estudio confirma una alta prevalencia de problemas del sueño en la edad pediátrica. Por tanto, el papel del pediatra en este ámbito es de gran importancia.
Palabras clave
● Epidemiología ● Niño ● Prevalencia ● Trastornos del sueñoINTRODUCCIÓN
Los trastornos del sueño en la edad pediátrica son una patología muy frecuente que, sin embargo, es escasamente valorada por la mayoría de los profesionales. Se estima que la prevalencia de dichos trastornos en Pediatría oscila entre el 20 y el 30%. El sueño es una función básica para la vida del niño y cada vez se conocen más las influencias de las alteraciones del sueño en la infancia, repercutiendo en su vida diaria a nivel cognitivo, emocional, en la capacidad de aprendizaje, y en su relación en el ámbito familiar. Son escasos los estudios realizados sobre la patología del sueño, y la formación que recibe el pediatra en dichos trastornos es muy deficitaria, sin embargo, se estima que hasta un 4% de los niños toman alguna vez medicación hipnótica en la infancia.
El objetivo del estudio es conocer la prevalencia de las alteraciones del sueño en la edad preescolar y escolar en una población de niños sanos de un centro de salud de Málaga, que acuden a consulta por motivos distintos a dicha patología. Por otra parte, la prevalencia de niños que utilizan frecuentemente aerosolterapia como fármacos β-adrenérgicos, anticolinérgicos o corticosteroides, está aumentando en los últimos tiempos. Entre sus efectos secundarios se encuentran la taquicardia, temblor, ansiedad y nerviosismo. Por ello, en nuestro estudio se analiza si los niños con problemas respiratorios que requieren tratamiento con aerosolterapia tienen una mayor prevalencia de trastornos del sueño debido a dichos posibles efectos secundarios.
MATERIAL Y MÉTODOS
Se trata de un estudio descriptivo prospectivo de tipo observacional transversal, llevado a cabo en el centro de salud de las Delicias, en Málaga capital, durante los meses comprendidos entre mayo de 2016 y febrero de 2017.
Los criterios de inclusión fueron pacientes con edad comprendida entre los 2 y 14 años, sanos, que no presentasen patologías crónicas ni agudas que interfirieran en el sueño, y que acudieran a consulta de Atención Primaria por motivos distintos a problemas del sueño.
Se excluyeron pacientes menores de 2 años o mayores de 14 años, así como pacientes con patología crónica que pudieran alterar el inicio o mantenimiento del sueño, como los niños afectos de trastorno de déficit de atención e hiperactividad, con patología neurológica o alteraciones tiroideas, hay que hacer mención de que la única enfermedad crónica que sí se aceptó fue el asma, dado que estos pacientes eran objeto de estudio. Igualmente se excluyeron aquellos que consumiesen fármacos que pudieran alterar el inicio o el mantenimiento del sueño, como el tratamiento con metilfenidato, corticoides sistémicos, benzodiazepinas… También se excluyeron aquellos pacientes que acudieran acompañados por un cuidador que no conociera las características del sueño por no dormir con él habitualmente.
Partiendo de una población accesible de 2423 pacientes, se seleccionaron 225 para constituir la muestra que estudiar con una precisión del 5% y un error α de 0,05, y una proporción esperada del 30%.
Se realizó una encuesta de preguntas cerradas con elección múltiple y respuesta única mediante la escala validada de trastornos del sueño de Bruni (Sleep Disturbance Scale for Children). Se trata de una encuesta compuesta por 27 preguntas, donde se evalúan los posibles trastornos del sueño en los últimos 6 meses. Su consistencia interna es mayor en los controles (0,79) se mantiene con un nivel satisfactorio en los niños con trastornos del sueño (0,71) y la fiabilidad es satisfactoria para el total (r = 0,71) y para cada reactivo de forma individual. Dicha escala está compuesta por preguntas cerradas, de elección múltiple y respuesta única, diseñadas para detectar posibles trastornos distintas áreas: inicio y mantenimiento del sueño, desórdenes del arousal, alteraciones del tránsito sueño-vigilia, problemas respiratorios, somnolencia excesiva e hiperhidrosis del sueño. A cada uno de los 27 ítems se les da una puntuación del 1 al 5, posteriormente se realiza el sumatorio de la puntuación, de modo que una puntuación igual o mayor a 39 puntos en el total del cuestionario indica la presencia de un trastorno del sueño.
Se obtuvo el consentimiento por parte del comité de ética del hospital de referencia, al igual que la autorización de los padres mediante la firma del consentimiento informado y se realizó enmascaramiento de las encuestas. La encuesta se entregaba por los residentes de Pediatría que durante ese periodo realizaron su rotación por Atención Primaria en dicho centro. Se realizaba en la sala de espera por el familiar de primer grado acompañante del menor.
Además de las variables incluidas en la escala, se recogieron otras como la presencia de patología respiratoria tipo asma, o el uso frecuente de aerosolterapia (considerando aquellos pacientes con más de tres episodios en los últimos 3 meses, que hayan requerido medicación inhalada con β2-adrenérgicos). La pregunta sobre el uso de aerosolterapia no se incluye en la baremación, puesto que únicamente tiene como objetivo clasificarlos en diferentes grupos. Finalmente, los datos de las encuestas se introdujeron en una base de datos utilizando el sistema estadístico SPSS versión 2.2.
Se dividieron los pacientes en tres grupos según la edad: 2-3 años, 4-6 años y 7-14 años. Se realizó un análisis descriptivo de la proporción de pacientes de cada edad, del tiempo de latencia para dormirse y de la frecuencia de cada uno de los trastornos, así como de la frecuencia global de trastornos del sueño. Posteriormente se realizaron test de contraste de hipótesis (t de Student, Anova, χ2), en donde se analizaron el grupo de pacientes asmáticos en tratamiento con aerosoles con el resto, entre otras.
RESULTADOS
Se realizaron un total de 225 encuestas. La prevalencia de trastornos del sueño en el total de niños encuestados fue del 61%. Los pacientes encuestados se distribuyeron según edad en tres grupos: 2-3 años (12%), 4-6 años (37,7%) y 7-14 años (50,2%), basándonos en la misma clasificación realizada en el estudio de Pin Arboledas.
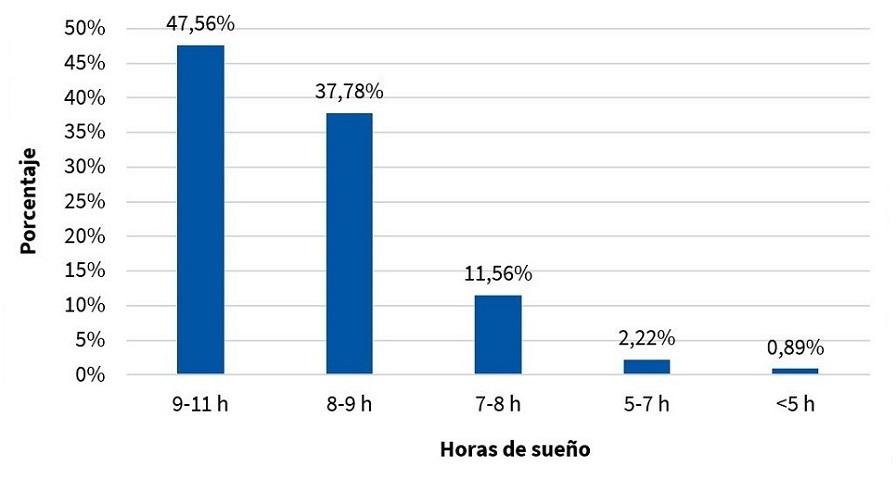
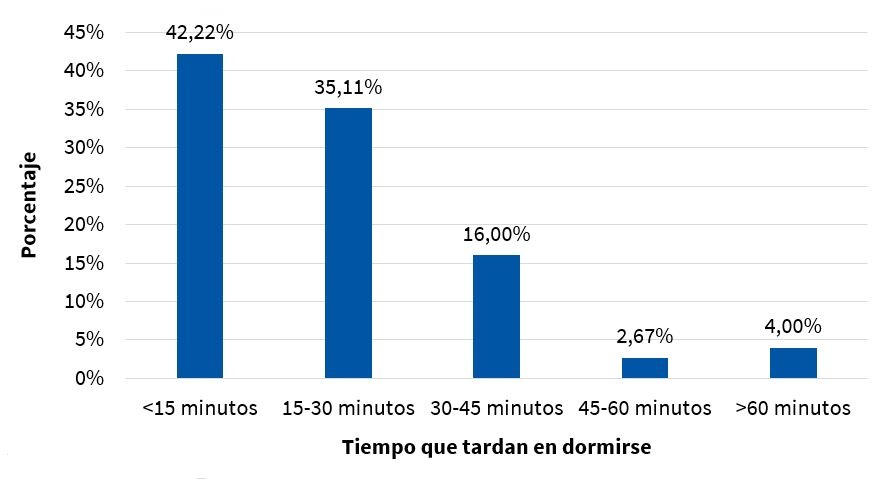
En cuanto a las horas de sueño, un 14,6% de los niños dormían menos de 8 horas (Fig. 1) y, al clasificarlos por grupos de edad, se observó cómo los niños de menor edad presentaban más alteraciones en cuanto a las horas de sueño (Fig. 2). En cuanto a la latencia del sueño, el 23% de los niños tardaban más de 30 minutos en dormirse (Fig. 3).
| Figura 2. Relación entre edad y horas de sueño. Se observa que en los menores de tres años es mayor el porcentaje de niños que duermen menos horas |
|---|
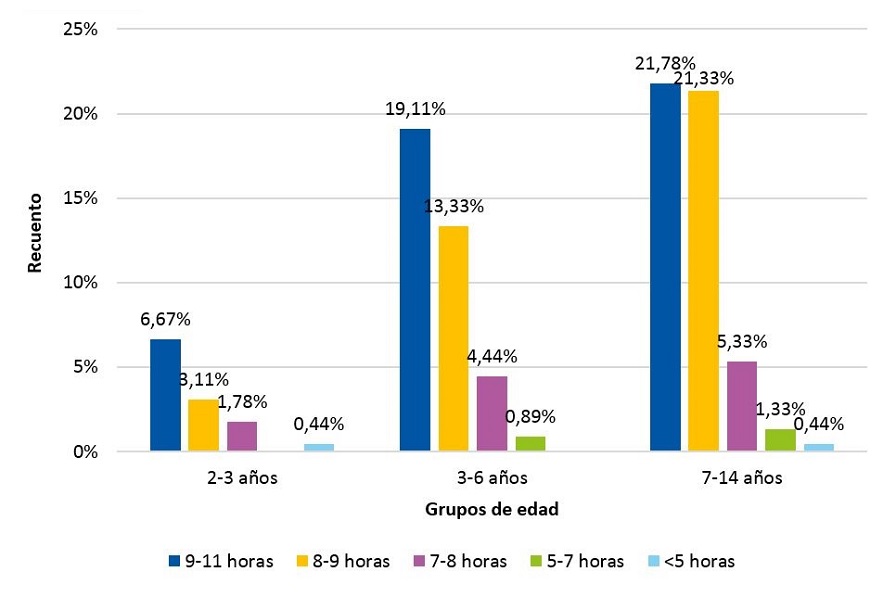 |

Los trastornos del sueño más frecuentes fueron los problemas del sueño-vigilia (38%), seguido por los problemas respiratorios, sospechándose en estos casos un síndrome de apneas-hipopneas del sueño (18%). De igual modo, presentaron problemas en el inicio del sueño el 17% de los casos, hiperhidrosis del sueño el 15%, problemas del arousal el 13% y somnolencia diurna excesiva el 10% de los casos.
Por otra parte, se analizó la asociación entre aquellos pacientes asmáticos y los trastornos del sueño, mediante el análisis estadístico χ2, obteniéndose un resultado p = 0,07, lo cual no apoya la hipótesis de que los efectos secundarios derivados del uso de la aerosolterapia determinen un mayor riesgo de padecer problemas del sueño. Igualmente, se analizó si existía alguna asociación entre el uso de aerosolterapia y cada uno de los trastornos del sueño de manera individualizada, sin obtener relación entre ambas. Al intentar relacionar las horas de sueño con la existencia de trastorno del sueño, no se encontró asociación, realizándose mediante método Anova.
DISCUSIÓN
Los resultados obtenidos en nuestro estudio demuestran que existe una alta prevalencia de trastornos del sueño en la edad pediátrica (61%).
Dicho estudio pretende dar una idea general sobre la importancia de estos trastornos y cómo pasan desapercibidos tanto para las familias, que no suelen referir dichos síntomas en la consulta, como para los profesionales sanitarios, que tampoco hacen hincapié en la anamnesis a la hora de indagar sobre dichos problemas.
Como limitaciones del estudio, hay que destacar la escasa bibliografía científica, ya sean artículos o revisiones sobre los trastornos del sueño en Pediatría, así como la arbitrariedad de las encuestas utilizadas en los distintos estudios, sin que exista un acuerdo sobre cuál debe ser la encuesta de elección. En nuestro estudio elegimos la encuesta de Bruni, por tratarse de una encuesta validada, aunque nos obligó a excluir a los pacientes menores de dos años. Igualmente, en cuanto al sistema de entrega de las encuestas, tuvimos como limitación que esta se entregaba a los padres por distintas personas no expresamente formadas para este fin y sin saber si entendían la encuesta, así como el lugar de la recogida de estas, que probablemente no era el más idóneo.
La Academia Americana de Pediatría informó de una prevalencia de trastornos del sueño en la edad pediátrica de entre el 20 y el 30%. Sin embargo, otros estudios describen una prevalencia de hasta el 45%. En nuestro estudio, la prevalencia estimada de los trastornos del sueño fue del 61%. Llama la atención la discordancia existente, que probablemente se deba a que no se ha empleado la misma encuesta en los distintos estudios descriptivos y a las diferencias en cuanto al tamaño muestral. La comparación de nuestros resultados con los de otras series es difícil, ya que se han aplicado distintos criterios para hacer el diagnóstico de trastorno del sueño, así como la subjetividad de las encuestas, los intervalos de edades elegidos y los tamaños de las muestras analizadas.
CONCLUSIONES
Nuestro estudio confirma una prevalencia mayor a la esperada de trastornos del sueño en la edad pediátrica, que se eleva al 61% de los niños encuestados. Por tanto, el papel del pediatra en este ámbito es fundamental y es importante remarcar la necesidad de que sea el propio pediatra quien indague sobre dichas alteraciones en la anamnesis habitual.
CONFLICTO DE INTERESES
Las autoras declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
BIBLIOGRAFÍA RECOMENDADA
- Alberola López S, Pérez García I, Casares Alonso I, Cano Garcinuño A, Andrés de Llano JM. C-2. Estudio de las características del sueño en niños preescolares de nuestro medio. Rev Pediatr Aten Primaria. 2010;12:e57.
- American Academy of Sleep Medicine. International classification of sleep disorders, third edition: diagnostic and coding manual. Westchester (ILL): American Academy of Sleep Medicine; 2014.
- Bruni O, Octaviano S, Guidetti V, Romoli M, Innocenzi M, Cortesi F, et al. The Disturbance Scale for Children (SDSC). Construction and validation of an instrument to evaluate sleep disturbances in childhood and adolescence. J Sleep Res. 1996;5:251-61.
- Estivill E. Situación actual de los trastornos del sueño en niños. Rev Pediatr Aten Primaria. 2002;4:563-5.
- Giménez Badia S, Albares Tendero J, Canet Sanz T, Jurado Luque MJ, Madrid Pérez JA, Merino Andreu M,et al. Trastorno de retraso de la fase del sueño y del despertar. Síndrome de retraso de fase. Rev Pediatr Aten Primaria. 2016;18:129-39.
- Goodlin-Jones BL, Sitnick SL, Tang K, Liu J, Anders TF. The children’s sleep habits questionnaire in toddlers and preschool children. J Dev Behav Pediatr. 2008;29:82-8.
- Gradisar M, Dohnt H, Gardener G, Paine S, Starkey K, Menne A, et al. A randomized controlled trial of cognitive-behavior therapy plus bright light therapy for adolescent delayed sleep phase disorder. Sleep. 2011;34:1671-80.
- Hernández Delgado MJ, García Rebollar C. Estudios sobre los hábitos del sueño en niños. Rev Pediatr Aten Primaria. 2006;8:334-6.
- Herzog R, Cunningham-Rundles S. Pediatric asthma: natural history, assessment, and treatment. Mt Sinai J Med. 2011;78:645-60.
- Pedemonte V, Gandaro P, Scavone C. Trastornos del sueño en una población de niños sanos de Montevideo. Primer estudio descriptivo. Arch Pediatr Uruguay. 2014:85:4-8.
- Pin Arboledas G, Soto Insuga V, Jurado Luque MJ, Fernández Gomáriz C, Hidalgo Vicario I, Lluch Rosello A. Insomnio en niños y adolescentes. Documento de consenso. An Pediatr (Barc). 2017;86:165.e1-165.e11.
- Pin Arboledas G, Ugarte Libano R. Lo que el pediatra de Atención Primaria debería saber sobre el sueño. Rev Pediatr Aten Primaria. 2010;12:s219-s230.
- Pin Arboledas G, Ugarte Libano R. Taller de sueño infantil. Herramientas para su interpretación por el pediatra de Atención Primaria. Rev Pediatr Aten Primaria. 2009;11:s399-s404.
- Suárez P, Ortiz P, Ayala Curiel J. El sueño en la infancia. Rev Pediatr Aten Primaria. 2002;4:639-55.
- Tomás Vila M, Miralles Torres A, Beseler Soto B. Versión española del Pediatric Sleep Questionnaire. Un instrumento útil en la investigación de los trastornos del sueño en la infancia. Análisis de su fiabilidad. An Pediatr (Barc). 2007;66:121-8.
- Wilhelmsen-Langeland A, Saxvig IW, Pallesen S, Nordhus IH, Vedaa Ø, Lundervold AJ,et al. A randomized controlled trial with bright light and melatonin for the treatment of delayed sleep phase disorder: effects on subjective and objective sleepiness and cognitive function. J Biol Rhythms. 2013;28:306-21.