Vol. 19 - Num. 75
Originales
Relación entre la percepción del consumo oral de líquidos y el volumen urinario en población sana
Concepción Mir Perellóa, Concepción Sáez-Torres Barrosob, Dolores Rodrigo Jiméneza, Adrián Rodríguez Rodríguezb, Javier Lumbreras Fernándeza, Guiem Frontera Juanc, Joan Figuerola Muleta, Félix Grases Freixedasb
aServicio de Pediatría. Hospital Universitari Son Espases. Palma de Mallorca. España.
bLaboratorio de Investigación en Litiasis Renal. Instituto Universitario de Investigación en Ciencias de la Salud (IUNICS-IdISPa). Universidad de las Islas Baleares. Palma de Mallorca. España.
cUnidad de Investigación. Hospital Universitari Son Espases. Palma de Mallorca. España.
Correspondencia: C Mir. Correo electrónico: mariac.mir@ssib.es
Cómo citar este artículo: Mir Perelló C, Sáez-Torres Barroso C, Rodrigo Jiménez D, Rodríguez Rodríguez A, Lumbreras Fernández J, Frontera Juan G, et al. Relación entre la percepción del consumo oral de líquidos y el volumen urinario en población sana. Rev Pediatr Aten Primaria. 2017;19:223-9.
Publicado en Internet: 05-07-2017 - Número de visitas: 110668
Resumen
Introducción: el volumen urinario bajo (< 1 ml/kg/h) es el factor etiológico más frecuente en la litiasis renal. Frecuentemente, se asume que los niños que refieren beber mucho tienen una diuresis protectora. En este estudio analizamos el hábito de consumo de líquidos en niños sanos y su relación con el volumen urinario.
Metodología: se estudiaron 84 niños, de 5 a 17 años. Se registró la percepción de consumo habitual de líquidos como: “poco”, “normal” o “mucho” y los tipos de bebida habitual. Se cuantificó el volumen en orina de 24 h y se relacionó con la percepción de la ingesta de líquidos.
Resultados: la ingesta habitual de líquidos fue calificada como “poca” en el 23% de los casos, “normal” en un 56% y “mucha” en un 21%. El 39% de los niños (33/84) presentó una diuresis > 1 ml/kg/h que, por grupos, supone el 38,9% de los que refirieron una ingesta escasa, el 63% de los de consumo “normal” y el 73,7% de los que refirieron ingesta elevada. El 56% de los niños de los grupos de ingesta “normal” y “elevada” mostraron una diuresis < 1 ml/kg/h.
Conclusiones: la mayoría de niños mostraron una diuresis por debajo del límite recomendado, incluso entre los que refieren una ingesta “normal” o “elevada” de líquidos. Estos hallazgos hacen visible la necesidad de promover estrategias encaminadas a aumentar el consumo de agua en la población.
Palabras clave
● Ingestión de líquidos ● Litiasis renal ● Nutrición ● Volumen urinario
INTRODUCCIÓN
La adecuada ingesta de líquidos es esencial para el mantenimiento del medio interno. El consumo incrementado de agua ha sido relacionado con el retraso en la progresión de multitud de patologías de causa renal1,2 y extrarrenal3,4. Sin embargo, la patología donde hay una mayor evidencia científica del efecto terapéutico del consumo de agua elevado es la litiasis renal5,6. A pesar de que la litiasis pediátrica es menos frecuente que en el adulto7,8, la literatura médica refleja cómo la enfermedad está apareciendo cada vez más a edades tempranas y de forma grave9,10, especialmente en los adolescentes11,12.
La formación de cálculos renales es la consecuencia final de un desequilibrio entre las sustancias promotoras e inhibidoras de la cristalización, que se encuentran de forma habitual en la orina11,13. El factor que determina de forma más importante la facilidad con la que la orina cristaliza es el grado de sobresaturación. Este grado de sobresaturación de las diferentes sustancias en la orina depende de su cantidad total14 y, de forma más importante, del volumen urinario15. De este modo, una ingesta escasa de líquido será, en sí misma, un factor de riesgo para todos los tipos de litiasis porque da lugar a una orina más concentrada14 y porque aumenta su tiempo de tránsito a lo largo del tracto urinario15,16.
Las recomendaciones acerca del volumen de diuresis adecuado en población pediátrica, que resulte protector de la formación de los tipos más frecuentes de cálculos renales, varían según diferentes publicaciones y oscilan entre 0,8 y 1,4 ml/kg/h; el valor de 1 ml/kg/h es el límite más comúnmente aceptado7,17. En términos generales, por grupos de edad, la diuresis recomendada es de 750 ml/24 horas en lactantes, 1000 ml/24 horas en niños menores de cinco años, 1500 ml/24 horas en población entre cinco y diez años y más de 2000 ml/24 horas en mayores de diez años18. Por el contrario, la presencia de valores de diuresis inferiores a 0,5 ml/kg/h (considerados en rango de oliguria) conllevan un riesgo muy elevado de sobresaturación de la orina19.
El aporte de 1,5-2 l/m2/día de agua suele ser suficiente para conseguir estas cifras de diuresis, aunque esta cantidad es variable en función de las circunstancias del niño y debe ser incrementada en periodos en los que las pérdidas hídricas sean mayores. Los líquidos proporcionan habitualmente el 80% del agua total ingerida, y el 20% restante lo constituye el agua contenida en los alimentos19. La ingesta de líquidos condicionada por el reflejo de la sed constituye un mecanismo eficaz de prevención de la deshidratación, pero resulta insuficiente por sí sola para el mantenimiento de una hidratación adecuada. Para ello, es necesaria una ingesta adicional de líquido que depende de la voluntad y que, mantenida en el tiempo, logre establecer un hábito. Conseguir instaurar este hábito tiene como factor clave el que el niño (o su familia en los niños más pequeños) esté informado de la cantidad de líquido que debe beber en función de sus necesidades o actividades diarias.
Este estudio parte de la hipótesis de que la percepción subjetiva, por parte del niño o sus familias, de que realiza un consumo adecuado de cantidad de líquidos, no siempre se corresponde con unos valores de diuresis seguros para evitar la litiasis renal. Por tanto, el objetivo principal de este estudio es evaluar si el hábito de ingesta de líquidos referido en la anamnesis se corresponde con los valores de diuresis mayores o menores de 1 ml/kg/hora, cuantificados en una muestra de 24 horas. Como objetivos secundarios se plantea describir la cantidad de niños que refieren cada uno de los patrones de consumo y su diuresis, en relación con el sexo y con la edad. Asimismo, se plantea conocer las bebidas de consumo habitual de la muestra seleccionada.
MATERIAL Y MÉTODOS
Se realizó un estudio descriptivo transversal observacional en una muestra de niños sanos entre 5-17 años, procedentes de varios colegios de Mallorca (Islas Baleares, España), durante el periodo escolar de marzo del 2014 a febrero de 2015. Fueron excluidos los niños afectos de patología aguda o crónica, o que tomaran medicación en el momento del análisis. Se pidió a los participantes que no modificaran sus hábitos dietéticos y de actividad física. Se obtuvo el consentimiento informado de los padres o tutores de los niños del estudio. El estudio fue aprobado por el Comité de Ética de las Islas Baleares (IB 3152/16 PI).
Las variables recogidas fueron: edad, sexo, percepción del hábito de ingesta de líquidos y diuresis en orina de 24 horas.
A través de la anamnesis se determinó el hábito de ingesta de líquidos de cada niño referida únicamente a la percepción del propio participante, en el caso de niños mayores de 13 años, o de su familia, en el caso de menores de esa edad. Se clasificó a los niños en tres grupos: “bebe poca cantidad” (no llega a un vaso en las comidas y solo ocasionalmente entre horas), “bebe una cantidad normal” (un vaso en las comidas y alguno entre horas) o “bebe mucha cantidad” (se rellena el vaso en las comidas y varios vasos entre horas).
Se solicitó a los niños que orinaran durante 24 horas en un bote que se les entregó, explicando que debían desechar la primera orina de la mañana del día de la recogida, e incluir la primera orina de la mañana siguiente. Se determinó el volumen de orina en 24 horas y se calculó el valor de diuresis, expresándolo en ml/kg/h. Se aceptaron únicamente las muestras con creatininuria entre 15-25 mg/kg/24 h, como criterio de recogida correcta, según los puntos de corte de la población europea sana descritos por Remer20. Se valoró el resultado global de la muestra y se dividió en cuatro grupos (diuresis superior a 1 ml/kg/h, entre 0,8 y 1 ml/kg/h, entre 0,5 y 0,8 ml/kg/h e inferior a 0,5 ml/kg/h). Se consideró factor protector un valor de diuresis igual o superior a 1 ml/kg/h.
Se valoró el resultado global del grupo y se estableció la distribución del mismo por sexo y por edad, dividiéndolo en tres grupos: 5-8 años, 9-12 años y 13-17 años (adolescentes). Se realizó un análisis descriptivo de los parámetros analizados, calculando medidas de centralización adecuadas al tipo de distribución de cada variable, y su dispersión, media y desviación estándar para distribución normal, o mediana y cuartiles en el caso contrario. Para las variables categóricas (poca ingesta, normal o mucha, sexo y grupos de edad) se calcularon las proporciones, realizando la comparación entre grupos mediante el test de χ2. Se utilizó el programa estadístico SPSS® para Windows® versión 2.0. La significación estadística se definió con valores de p < 0,05.
RESULTADOS
Se estudiaron un total de 84 niños (48 niños y 36 niñas): 13 niños entre 5-8 años, 36 niños entre 9-12 años y 35 niños entre 13-17 años (adolescentes). La media de edad fue de 11,5 años.
Los resultados de la percepción de la ingesta habitual, en relación a en la cantidad (poca, normal o mucha) y su distribución por sexos se muestran en la Tabla 1. No se encontraron diferencias significativas entre los distintos grupos de edad (p < 0,05) (Tabla 2). La mediana de diuresis en 24 horas en el conjunto de la población del estudio fue de 0,93 ml/kg/h. Su distribución por sexos se describe en la Tabla 1. Por grupos de edad, fue de 0,92 ml/kg/h en los niños entre 5-8 años, de 0,97 ml/kg/h en los de 9-12 años y de 0,93 ml/kg/h en los de 13-17 años, sin diferencias significativas entre los grupos.
| Tabla 1. Edad media de la muestra, diuresis y percepción de la ingesta de líquidos del total de la muestra, y su distribución por sexos. Entre paréntesis se indica el porcentaje que supone del total del grupo | ||||
|---|---|---|---|---|
| Niños (n = 48) | Niñas (n = 36) | Total (n = 84) | ||
| Edad (media) | 11,6 años | 11,3 años | 11,5 años | |
| Diuresis | 0,93 ml/kg/h | 0,94 ml/kg/h | 0,93 ml/kg/h | |
| Percepción de la ingesta líquidos | Poca | 9 (19%) | 10 (28%) | 19 (23%) |
| Normal | 27 (56%) | 20 (55%) | 47 (56%) | |
| Mucha | 12 (25%) | 6 (17%) | 18 (21%) | |

| Tabla 2. Percepción de la ingesta de líquidos en función de los diferentes grupos de edad. Entre paréntesis se indica el porcentaje que supone del total de niños de su franja de edad | |||
|---|---|---|---|
| Percepción de la ingesta de líquidos | 5-8 años (n = 14) | 9-12 años (n = 36) | 13-17 años (n = 34) |
| Poca | 5 (35%) | 7 (20%) | 7 (20%) |
| Normal | 7 (50%) | 21 (58%) | 19 (56%) |
| Mucha | 2 (15%) | 8 (22%) | 8 (24%) |

Del total de niños estudiados, 33 de ellos (39%) mostraron una cifra de diuresis igual o superior a 1 ml/kg/h, 20 niños (24%) entre 0,8 y 1 ml/kg/h, 25 niños (29%) entre 0,8 y 0,5 ml/kg/h y en 5 participantes (6%) fue inferior a 0,5 ml/kg/h. La Tabla 3 muestra la distribución de los valores de diuresis en los diferentes grupos de edad.
| Tabla 3. Diuresis en 24 horas (ml/kg/h) separados por grupos de edad. Entre paréntesis se indica el porcentaje que supone del total de niños de su franja de edad | ||||
|---|---|---|---|---|
| 5-8 años (n = 14) | 9-12 años (n = 36) | 13-17 años (n = 34) | Total (n = 84) | |
| < 0,5 ml/kg/h | 0 (0%) | 2 (5%) | 5 (15%) | 7 (8%) |
| 0,5-0,8 ml/kg/h | 3 (21%) | 10 (28%) | 7 (20%) | 20 (24%) |
| 0,8-1 ml/kg/h | 7 (50%) | 10 (28%) | 12 (35%) | 29 (35%) |
| > 1 ml/kg/h | 4(29%) | 14 (29%) | 10 (30%) | 28 (33%) |

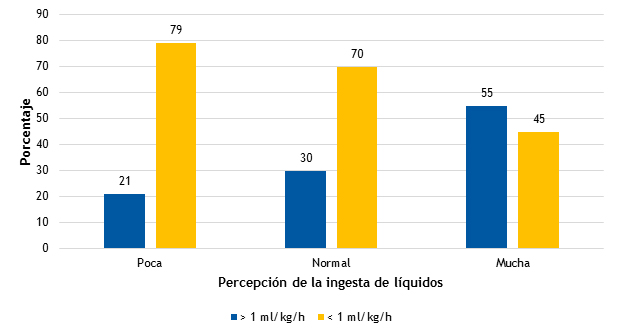
Los resultados de diuresis (superiores o inferiores a 1 ml/kg/h en 24 h) en relación al hábito referido de ingesta hídrica se muestran en la Fig. 1. No se encontraron diferencias significativas en relación a la mediana de diuresis, que fue de 0,91 ml/kg/h (P25-75: 0,76-1,01), 0,91 ml/kg/h (P25-75: 0,76-1,17), y 1,1 ml/kg/h (P25-75: 0,84-1,33), en los grupos con percepción de “poca”, “normal” o “mucha” ingesta habitual de líquido, respectivamente. Se halló un 55% (17/84) de niños con diuresis > 1 ml/kg/h en el grupo que refiere ingesta elevada de líquido, un 30% (46/84) en el de ingesta normal y un 20% (25/84) en el de ingesta escasa.
DISCUSIÓN
En el presente estudio hemos hallado mayor porcentaje de niños con un volumen urinario considerado adecuado en el grupo de los que refieren ingerir más cantidad de líquido y viceversa. A pesar de ello, coincidiendo con la hipótesis planteada, destaca el hallazgo de un número elevado de casos en los que no existe esta relación.
Con frecuencia, los pacientes creen erróneamente que sus hábitos dietéticos son saludables (en este caso en referencia a la ingesta líquidos). Aunque esto es un hecho constatado en la práctica clínica, no existen estudios que lo hayan analizado en población infantil. Los resultados de este estudio ponen en evidencia que la información que aporta el paciente en la consulta sobre sus hábitos de ingesta de líquidos no se traduce en muchos casos en la presencia de valores de diuresis saludables. De este modo, nos ha llamado la atención observar cifras de diuresis inferiores a 1 ml/kg/h en la mayoría de los niños que refieren beber normalmente una “cantidad normal” de líquido, así como en uno de cada dos niños del grupo que contestó la opción de “ingesta elevada”. Es importante destacar que este estudio se ha realizado en una población sana (sin patología aguda o crónica en el momento de la toma de la muestra) y en ausencia de condiciones climatológicas extremas. En esta misma población, en la que hallamos una proporción tan elevada de volúmenes urinarios bajos, la concurrencia de factores adicionales que aumenten las pérdidas extrarrenales de agua (tales como fiebre, vómitos, diarrea, calor importante) o condiciones que favorezcan la sobresaturación y estasis urinario (desequilibrios dietéticos, inmovilización, etc.), incrementarán considerablemente el riesgo de cristalización urinaria.
El análisis de los valores de diuresis en función del sexo no ha mostrado diferencias. De este modo, la creencia generalizada de que los niños beben más (que en nuestro caso también podría estar apoyada por el hecho de observar un mayor porcentaje de varones que refieren beber “mucha agua”) no se ha podido observar a través del hallazgo de mayor volumen urinario. El diseño del estudio no permite concluir si ello es debido a que la valoración de lo que sería la “cantidad normal” de ingesta de agua es percibida de forma diferente por los niños y por las niñas, o si realmente los varones beben más, pero están también más influidos por una mayor pérdida insensible de agua producida por una tasa de actividad física más alta.
En los diferentes grupos de edad del estudio, los resultados han mostrado valores inferiores de diuresis en el grupo de los adolescentes, junto con más casos de diuresis extremadamente baja (< 0,5 ml/kg/h). Es posible que estos datos sean un reflejo de lo que ocurre en la población y que sea uno de los factores que estén favoreciendo el aumento de la incidencia de litiasis entre los jóvenes. La literatura médica señala cómo la litiasis en la adolescencia está muy condicionada por factores ambientales, tales como la presencia de un volumen de orina bajo17, en contra de lo que ocurre en pacientes de menor edad, en los que existe un predominio de las alteraciones metabólicas urinarias (sobre todo en los niños menores de diez años). En consecuencia, la necesidad de tratamiento farmacológico es más frecuente en los niños más pequeños, mientras que entre los adolescentes hay más casos en los que las modificaciones dietéticas por sí solas son suficientes para prevenir las recurrencias17.
Entre las modificaciones dietéticas causantes del aumento de litiasis en la adolescencia, se debe prestar especial atención al hábito de consumo de líquido, ya que el descenso de los valores de diuresis que hemos observado puede estar explicado por la incorporación de patrones dietéticos que incluyen un menor consumo de agua21, a pesar de que, como se refleja en el presente estudio, ello no sea percibido como tal por el propio adolescente.
En relación al riesgo litógeno, es importante tener en cuenta tanto la cantidad como el tipo de bebida que se consume. El agua debe ser la bebida principal ingerida en la población, siendo esta una de las recomendaciones de la Organización Mundial de la Salud18. Otras bebidas como la leche resultan esenciales para el crecimiento y el desarrollo de la población infantil. Por otra parte, los zumos naturales, cuyo aporte de inhibidores de la cristalización urinaria, como el citrato, y de otros micronutrientes saludables, son también recomendables22. En la adolescencia, el consumo de agua, leche y zumos naturales se ve desplazado por el aumento de consumo de otras bebidas23 (entre las que destacan de forma importante los refrescos de cola y bebidas blandas), cuyo elevado contenido en fósforo y oxalato se ha relacionado con un mayor riesgo de formación de cálculos3,21,24,25.
CONCLUSIONES
En la mayoría de niños estudiados la ingesta de líquidos no se ha traducido en una diuresis deseable, incluso entre aquellos que perciben que beben mucho.
Estos hallazgos apoyan la necesidad de informar sobre el hábito saludable de ingesta de líquidos en cada edad y de promover estrategias encaminadas a aumentar el consumo de agua en la población como medida de prevención primaria y secundaria de la litiasis renal. En este sentido resulta esencial el papel del pediatra de Atención Primaria, ya que tiene la posibilidad de actuar en un periodo de la vida clave para la adquisición de hábitos y de detectar pacientes y situaciones de riesgo susceptibles de ser corregidas ya desde edades tempranas. En los pacientes que precisen mantener un volumen urinario elevado, el cumplimiento de las recomendaciones hídricas debe contrastarse con datos objetivos de diuresis.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
BIBLIOGRAFÍA
- Nagao, S, Nishii, K, Katsuyama, M. Increased water intake decreases progression of polycystic kidney disease in the PCK rat. J Am Soc Nephrol. 2006;17:2220-7.
- Wang CJ, Creed C, Winklhofer FT. Water prescription in autosomal dominant polycystic kidney disease: a pilot study. Clin J Am Soc Nephrol. 2011;6:192-7.
- Vitoria I, Dalmau J. El agua: bebida recomendable para una adecuada nutrición en la infancia. Acta Pediatr Esp. 2011;69:259-66.
- Manz F, Wentz A. The importance of good hydration for the prevention of chronic diseases. Nutr Rev. 2005;63:2S-5S.
- Hernandez JD, Ellison JS, Lendvay TS. Current trends, evaluation, and management of pediatric nephrolithiasis. JAMA Pediatr. 2015;169:964-70.
- Fink H, Wilt T, Eidman K, Garimella P, MacDonald R, Monga M, et al. Medical management to prevent recurrent nephrolithiasis in adults: a systematic review for an American College of Physicians Clinical Guideline. Ann Inter Med. 2013;158:535-43.
- Penido MG, Tavares Mde S. Pediatric primary urolithiasis: symptoms, medical management and prevention strategies. World J Nephrol. 2015;4:444-54.
- Sarica K. Pediatric urolithiasis: etiology, specific pathogenesis and medical treatment. Urol Res. 2006;34:96-101.
- Valentini RP, Lakshmanan Y. Nephrolithiasis in children. Adv Chronic Kidney Dis. 2011;18:370-5.
- Van Dervoort K, Wiesen J, Frank R, Vento S, Crosby V, Chandra M, Trachtman H. Urolithiasis in pediatric patients: a single center study of incidence, clinical presentation and outcome. J Urol. 2007;177:2300-5.
- Alpay H, Ozen A, Gokce I. N. Clinical and metabolic features of urolithiasis and microlithiasis in children. Pediatr Nephrol. 2009;24:2203-9.
- Tasian GE, Copelovitch L. Evaluation and medical management of kidney stones in children. J Urol. 2014;192:1329-36.
- Daudon M, Hennequin C, Boujelben G, Lacour B, Jungers P. Serial crystalluria determination and the risk of recurrence in calcium stone formers. Kidney Int. 2005;67:1934-43.
- Cameron M, Sakhaee K, Moe O. Nephrolithiasis in children. Pediatr Nephrol. 2005;20:1587-92.
- Borghi L, Meschi T, Amato F, Briganti A, Novarini A, Giannini A. Urinary volume, water and recurrences in idiopathic calcium nephrolithiasis: a 5-year randomized prospective study. J Urol. 1996;155:839-43.
- Anastasio P, Cirillo M, Spitali L. Level of hydration and renal function in healthy humans. Kidney Int. 2001;60:748-75.
- Cambareri GM, Kovacevic L, Bayne AP, Giel D, Corbett S, Schurtz E, et al. National multi-institutional cooperative on urolithiasis in children: age is a significant predictor of urine abnormalities. J Pediatr Urol. 2015;11:218-23.
- Guidelines for drinking-water quality: incorporating first addendum. Vol. 1, Recommendations, 3.ª ed. En: Organización Mundial de la Salud [en línea] [consultado el 05/07/2017]. Disponible en www.who.int/water_sanitation_health/dwq/gdwq0506begin.pdf
- Taylor E, Fung T, Curhan G. DASH-style diet associates with reduced risk for kidney stones. J Am Soc Nephrol. 2009;20:2253-9.
- Remer T, Neubert A, Maser-Gluth C. Anthropometry-based reference values for 24-h urinary creatinine excretion during growth and their use in endocrine and nutritional research. Am J Clin Nutr 2002;75:561-9.
- Comité de Nutrición de la Asociación Española de Pediatría. Consumo de zumos de frutas y de bebidas refrescantes por niños y adolescentes en España. Implicaciones para la salud de su mal uso y abuso. An Pediatr (Barc). 2003;58:584-93.
- Meschi T, Maggiore U, Fiaccadori E, Schianchi T, Bosi S, Adorni G, et al. The effect of fruits and vegetables on urinary stone risk factors. Kidney Int. 2004;66:2402-10.
- Prezioso D, Strazzullo P, Lotti T, Bianchi G, Borghi L, Caione P, et al. Dietary treatment of urinary risk factors for renal stone formation. A review of CLU Working Group. Arch Ital Urol Androl. 2015;87:105-20.
- Rodgers A. Effect of cola consumption on urinary biochemical and physicochemical risk factors associated with calcium oxalate urolithiasis. Urol Res. 1999;27:77-81.
- Vitoria I, Dalmau J, Castells X, Calatayud O, Arias T. Fosfatos en colas y otras bebidas refrescantes. Riesgo de hipocalcemia en la infancia. An Pediatr (Barc). 2002;56:18.