Vol. 24 - Num. 95
Originales
Prevalencia y factores sociodemográficos asociados a la ambliopía en población preescolar
Julia Torrecillas Peraltaa, David Prieto Merinob, Jerónimo Lajara Blesac, Jorge L. Alió Sanzd, Jorge L. Alió del Barriod
aPrograma de Doctorado en Ciencias de la Salud. Universidad Católica San Antonio. Murcia. España.
bMétodos Estadísticos Aplicados en Investigación Médica. Universidad Católica San Antonio. Murcia. España. Facultad de Epidemiología y Salud de la Población. London School of Hygiene and Tropical Medicine. Londres. Reino Unido .
cFacultad de Ciencias de la Salud. Universidad Católica San Antonio. Murcia. España.
dUnidad de Córnea, Catarata y Cirugía Refractiva. Vissum Miranza. Departamento de Oftalmología. Facultad de Medicina. Universidad Miguel Hernández. Alicante. España.
Correspondencia: JL Alió. Correo electrónico: jorge_alio@hotmail.com
Cómo citar este artículo: Torrecillas Peralta J, Prieto Merino D, Lajara Blesa J, Alió Sanz JL, Alió del Barrio JL. Prevalencia y factores sociodemográficos asociados a la ambliopía en población preescolar . Rev Pediatr Aten Primaria. 2022;24:e291-e299.
Publicado en Internet: 20-09-2022 - Número de visitas: 11919
Resumen
Objetivo: estimar la prevalencia de la ambliopía y su tratamiento en niños de preescolar de la provincia de Alicante (España) durante un periodo de larga duración, así como la influencia de diferentes factores sociodemográficos.
Material y método: estudio observacional descriptivo transversal (2002-2015) mediante protocolo de detección de ambliopía validado (sensibilidad 89,3%; especificidad 93,1%) en niños escolarizados de 4 a 6 años. La variable principal fue la clasificación, de los 140 102 niños examinados, según el resultado de las pruebas (“normales”, “sospechosos de patología” o en “tratamiento previo”) y las variables explicativas: edad, sexo, curso escolar, tipo de gestión del colegio y su ubicación.
Resultados: la prevalencia de niños con sospecha de ambliopía osciló significativamente, entre los cursos escolares, desde 8,54% hasta 23,9% (p = 0,00000). Los niños de 6 años presentaron valores de sospecha de ambliopía notablemente más altos (16,68%; p = 0,00000) y los niños matriculados en colegios privados, los más bajos (8,05%; p = 0,00000). La probabilidad de que un niño “no-normal” estuviera ya tratado aumentaba con la edad (OR 2,06; p <0,001) y con el hecho de asistir a un colegio privado (OR 1,56; p = 0,001).
Conclusiones: la prevalencia de la sospecha de ambliopía fue alta en el área de estudio, siendo los niños de mayor edad y los niños pertenecientes al grupo de nivel socioeconómico más bajo los de mayor riesgo. Los programas de cribado escolar para la detección temprana de la ambliopía son recomendados para aumentar y equiparar la probabilidad de acceso al tratamiento, reduciendo así la prevalencia y la gravedad de la ambliopía en niños.
Palabras clave
● Agudeza visual ● Ambliopía ● Atención Primaria ● Disfunción visualINTRODUCCIÓN
La ambliopía se define como la reducción de la agudeza visual (AV) mejor corregida de ojos con morfología normal1,2. Acontece en edades tempranas de la infancia y da como resultado un desarrollo anormal de la vía visual cortical1. Sus factores de riesgo más frecuentes son el estrabismo y los errores de refracción2.
Existen tratamientos adecuados para la ambliopía, sobre todo cuando no está asociada a una patología estructural y se realiza una detección temprana1-3. Es considerada la causa más común de discapacidad visual monocular en niños y adultos jóvenes en Europa3,4. Su prevalencia se cifra entre el 1% y el 5% de la población a nivel mundial5, estimándose una prevalencia del 7,5 % en el caso concreto de niños españoles de entre 3 y 6 años6. La falta de unanimidad entre estudios puede deberse a las características de la población estudiada, criterios de AV y metodología empleada3. Que se conozca, en España no se han realizado estudios de larga duración sobre la prevalencia de la ambliopía en niños.
El presente estudio tuvo como objetivo estimar la prevalencia de la ambliopía y su tratamiento en niños de preescolar de la provincia de Alicante, y su evolución entre los años 2002 a 2015 mediante el empleo de campañas oftalmológicas pediátricas de cribado en los colegios, así como evaluar la influencia de diferentes factores sociodemográficos.
MATERIAL Y MÉTODOS
Campañas oftalmológicas pediátricas de cribado
Estudio observacional, descriptivo y con cortes transversales anuales mediante el empleo de campañas de cribado oftalmológico, realizadas por la Fundación Jorge Alió, para evaluar el impacto de la ambliopía en la población preescolar de la provincia de Alicante (España). Las exploraciones fueron realizadas por un equipo de optometristas bajo la dirección de oftalmólogos, durante 13 cursos escolares consecutivos (2002-2015), a los niños de 4 a 6 años matriculados en todos los centros de educación infantil de la provincia de Alicante, localizados en zonas urbanas (más de 25 000 habitantes, 74,2%), zonas semiurbanas (10 000 a 25 000 habitantes, 8,2%) y zonas rurales (menos de 10 000 habitantes, 17,6%).
En función de los resultados obtenidos en las pruebas del cribado, los niños se clasificaron como “normales” (ninguna alteración que hiciese pensar en anomalía visual), “sospechosos” de ambliopía aún no tratados (la AV estaba por debajo del valor estándar correspondiente a la edad7; se detectaba una alteración en el alineamiento o motilidad ocular o el niño no pasaba el test de estereopsis2) y en “tratamiento” oftalmológico activo (niños con patología previamente diagnosticada y ya en tratamiento).
Los criterios de exclusión fueron: los niños sin el expreso consentimiento de los padres/tutores, los que no asistieron a clase el día de la revisión y los que no cooperaron durante la misma. En cada campaña se evaluaba a los niños de nuevo ingreso en el colegio de 4, 5 y 6 años, junto con los niños que habían resultado “sospechosos” en la campaña del curso anterior.
Este estudio se adhirió a los principios de la Declaración de Helsinki, siguiendo todas las normas institucionales y gubernamentales aplicables en relación con el uso ético de voluntarios humanos para el examen médico2.
Cribado visual
Se realizaron: (a) test de AV a una distancia de 3 m con símbolos Lea (casa, manzana, cuadrado y círculo), cuyo tamaño disminuye en progresión logarítmica desde 0,1 hasta 2,08; (b) estudio de la alineación del eje visual mediante la prueba de oclusión y desoclusión del ojo (cover test)9; (c) examen ocular externo con linterna evaluando párpados, transparencia corneal, estructuras de cámara anterior y fulgor pupilar (descartando leucocoria)9,10 y (d) test de estereogramas de puntos aleatorios TNO con gafas rojo-verde para la medida de estereopsis9.
La fiabilidad de las pruebas empleadas en el cribado fue validada por Casas-Llera et al.2 en un estudio publicado previamente (sensibilidad del 89,3%, especificidad del 93,1%, valor predictivo positivo del 83,3%, valor predictivo negativo del 95,7%, cociente de probabilidad positivo de 12,86 y cociente de probabilidad negativo de 0,12).
Tratamiento de los datos
Con el objetivo de reflejar la población primigenia de la base de datos, para este análisis se realizó una depuración de esta, localizando la primera visita de cada niño y eliminando las sucesivas visitas en el caso de haber sido “sospechosos”.
Se utilizó como variable principal: el resultado de la clasificación oftalmológica tras los resultados del cribado (“normales”, “sospechosos” y en “tratamiento”).
A partir de esta, se hicieron dos variables objetivo-binarias (valores sí/no): (a) la variable “resultado no-normal” (agrupando sospechosos y tratados en una sola categoría de “no-normal”) y (b) la variable “tratamiento” que toma valor “sí” en los tratados y “no” en los sospechosos no tratados, pero que no toma valor en los individuos con la prueba de visión normal, ya que no lo necesitan.
Como variables explicativas: la edad (4, 5 o 6 años), sexo, curso escolar (2002 a 2015), ubicación del colegio (rural, semiurbano o urbano) y tipo de gestión del colegio (público, concertado, privado).
Análisis estadístico de los datos
Se calculó la frecuencia relativa de los resultados del cribado en cada nivel de cada variable explicativa por separado. Seguidamente, se compararon los porcentajes entre niveles de la variable explicativa con una prueba de Chi-cuadrado.
En el análisis gráfico de series temporales se calculó, en cada curso escolar, la proporción de participantes en cada resultado del cribado con un intervalo de confianza del 95% y la distribución de niños por edades.
Además, se diseñaron dos modelos de regresión logística múltiple con las dos variables binarias mencionadas arriba para estudiar qué variables explicativas de las recogidas aquí pueden estar relacionadas con el hecho de que el niño no tenga una visión normal y con la probabilidad de que esté ya tratado cuando ingresa en el estudio.
RESULTADOS
En el presente estudio se incluyeron un total de 140 102 niños examinados y clasificados según el resultado de las pruebas. La distribución de dicha muestra por curso, género, edad, ubicación del colegio y tipo de gestión se muestra en las Tablas 1 y 2.
| Tabla 1. Distribución (%) de niños “normales”, “sospechosos” y en “tratamiento” por curso escolar | ||||||
|---|---|---|---|---|---|---|
| Variables | Normal | Sospechoso | Tratamiento | |||
| Curso | % | n | % | n | % | n |
| 2002-2003 | 82,17% | 13 731 | 12,12% | 2025 | 5,71% | 955 |
| 2003-2004 | 87,46% | 13 902 | 8,54% | 1358 | 3,99% | 635 |
| 2004-2005 | 86,07% | 12 755 | 9,94% | 1473 | 3,99% | 592 |
| 2005-2006 | 87,72% | 13 162 | 9,10% | 1366 | 3,18% | 477 |
| 2006-2007 | 85,05% | 5409 | 11,78% | 749 | 3,18% | 202 |
| 2007-2008 | 83,66% | 13 839 | 11,66% | 1928 | 4,69% | 775 |
| 2008-2009 | 83,61% | 13 186 | 12,80% | 2019 | 3,59% | 566 |
| 2009-2010 | 81,41% | 11 205 | 14,81% | 2039 | 3,78% | 520 |
| 2010-2011 | 78,47% | 10 200 | 17,59% | 2286 | 3,95% | 513 |
| 2011-2012 | 71,33% | 3451 | 23,89% | 1156 | 4,77% | 231 |
| 2012-2013 | 76,98% | 3511 | 18,53% | 845 | 4,49% | 205 |
| 2013-2014 | 77,94% | 1413 | 17,43% | 316 | 4,63% | 84 |
| 2014-2015 | 74,46% | 764 | 20,76% | 213 | 4,78% | 49 |
| p | 0,00000 | 0,00000 | 0,00000 | |||

| Tabla 2. Distribución (%) de niños “normales”, “sospechosos” y en “tratamiento” dependiendo de las variables explicativas: sexo, edad, ubicación y tipo de gestión del colegio | ||||||
|---|---|---|---|---|---|---|
| Variables | Normal | Sospechoso | Tratamiento | |||
| Sexo | % | n | % | n | % | n |
| Hombre | 82,96% | 59 745 | 12,84% | 9248 | 4,19% | 3020 |
| Mujer | 83,39% | 56 661 | 12,52% | 8507 | 4,09% | 2779 |
| p | 0,03393 | 0,07164 | 0,33714 | |||
| Edad | ||||||
| 4 años | 86,02% | 79 601 | 11,17% | 10 341 | 2,81% | 2600 |
| 5 años | 78,71% | 27 726 | 15,26% | 5375 | 6,04% | 2126 |
| 6 años | 74,58% | 9198 | 16,68% | 2057 | 8,74% | 1078 |
| p | 0,00000 | 0,00000 | 0,00000 | |||
| Tipo de población | % | n | % | n | % | n |
| Rural | 83,42% | 20 613 | 12,23% | 3022 | 4,35% | 1075 |
| Semiurbana | 82,63% | 9372 | 12,97% | 1471 | 4,40% | 499 |
| Urbana | 83,12% | 85 517 | 12,81% | 13 180 | 4,07% | 4192 |
| p | 0,17311 | 0,03452 | 0,05628 | |||
| Gestión del colegio | % | n | % | n | % | n |
| Pública | 83,00% | 85 711 | 12,99% | 13 410 | 4,02% | 4148 |
| Concertada | 83,25% | 27 322 | 12,19% | 4000 | 4,56% | 1496 |
| Privada | 87,59% | 1871 | 8,05% | 172 | 4,35% | 93 |
| p | 0,00000 | 0,00000 | 0,00000 | |||

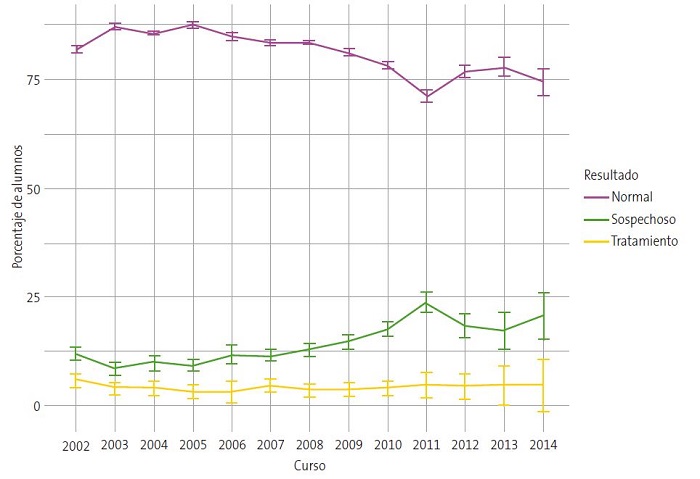
A lo largo de las 13 campañas de cribado se apreciaron diferencias muy significativas en las proporciones de niños diagnosticados como “normales”, “sospechosos” y en “tratamiento” (Tabla 1). En este sentido, la prevalencia de niños “sospechosos” osciló entre el 8,54% y 12,12% durante las seis primeras campañas. Sin embargo, a partir del curso 2008-2009 fue incrementando el valor, alcanzando un máximo del 23,89% en el curso 2011-2012. Asimismo, la distribución de niños en “tratamiento” mostró una tendencia a aumentar a partir del curso 2008-2009 (Tabla 1) (Fig. 1).
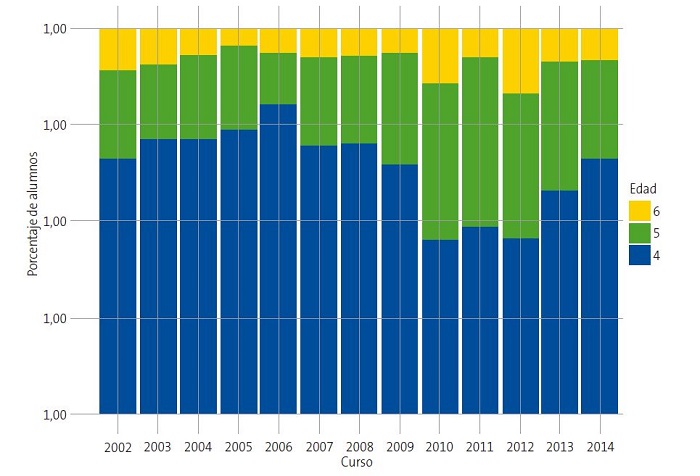
| Figura 1. Distribución de niños “normales”, “sospechosos” y en “tratamiento” por edades: evolución de los resultados del test a través de los cursos |
|---|
 |

La “sospecha” de ambliopía, no se asoció al género, encontrando cifras muy similares entre niños y niñas (12,84% y 12,52%, respectivamente). Es de destacar que los niños de 6 años presentaron una proporción de niños “sospechosos” (16,68%) notablemente superior a la observada en los niños de 4 y 5 años (Tabla 2).
Por otro lado, la ubicación del colegio estuvo ligeramente asociada a la prevalencia de niños “sospechosos”. Las zonas rurales presentaron el valor de prevalencia inferior (12,23%), mientras que en las zonas urbanas y semiurbanas fue levemente superior (12,81 y 12,97%, respectivamente) (Tabla 2).
El tipo de gestión de los colegios presentó un efecto significativo en la prevalencia de niños “sospechosos”, siendo los colegios de gestión privada los que presentaron valores inferiores (8,05%). Paralelamente, se observó una distribución considerablemente menor de niños en “tratamiento” en colegios públicos (4,02%) (Tabla 2).
El análisis de los factores que afectan a que un niño sea “no-normal” y la probabilidad de que ese niño sea tratado se realizó mediante dos regresiones logísticas sobre las dos variables objetivos dicotomizadas: (a) comparando niños en “normales” y “no-normales” (englobando los “sospechosos” y en “tratamiento”) y (b) dentro de los niños “no-normales” comparando los tratados con los no tratados (Tabla 3).
| Tabla 3. Modelos de regresión. Modelo 1: factores relacionados con ser un niño “no-normal”. Modelo 2: factores asociados a que un niño “no-normal” sea puesto en tratamiento | ||||||
|---|---|---|---|---|---|---|
| Modelo 1 | Modelo 2 | |||||
| Variables | OR | IC | p | OR | IC | p |
| Curso escolar | ||||||
| Curso | 1,05 | 1,05-1,06 | <0,001 | 0,92 | 0,91-0,93 | <0,001 |
| Sexo | ||||||
| Hombre | Referencia | Referencia | ||||
| Mujer | 0,97 | 0,94-1,00 | 0,048 | 1,00 | 0,94-1,06 | 0,945 |
| Edad | ||||||
| 4 años | Referencia | Referencia | ||||
| 5 años | 1,63 | 1,58-1,68 | <0,001 | 1,63 | 1,52-1,74 | <0,001 |
| 6 años | 2,07 | 1,98-2,17 | <0,001 | 2,06 | 1,88-2,25 | <0,001 |
| Tipo de población | ||||||
| Rural | Referencia | Referencia | ||||
| Semiurbana | 1,03 | 0,97-1,10 | 0,261 | 0,99 | 0,88-1,13 | 0,935 |
| Urbana | 1,01 | 0,97-1,05 | 0,544 | 0,83 | 0,77-0,90 | <0,001 |
| Gestión colegio | ||||||
| Pública | Referencia | Referencia | ||||
| Concertada | 1,00 | 0,97-1,03 | 0,972 | 1,30 | 1,21-1,40 | <0,001 |
| Privada | 0,65 | 0,57-0,74 | <0,001 | 1,56 | 1,20-2,02 | 0,001 |

En el Modelo 1 de la Tabla 3 se pudo ver que cada curso escolar aumentaba un 5% la odds de que un niño no fuera normal (p <0,001). Del mismo modo, la odds aumentó significativamente con la edad (con respecto a los 4 años, al cumplir 5 años la odds aumenta un 63% (OR 1,63; p <0,001) y a los 6 años se duplicó (OR 2,07; p <0,001)). También se observó que esa odds es levemente menor en las niñas (OR 0,97; p = 0,048). Finalmente, en los colegios de gestión privada es bastante relevante la remisión del riesgo (OR 0,65; p <0,001).
Entre los factores de riesgo que hicieron más probable que un niño “no-normal” estuviera tratado, cabe mencionar la pertenencia a colegios privados (OR 1,56; p = 0,001) y la mayor edad. Comparado con 4 años, a los 5 años, la odd sube un 63% (p <0,001) y a los 6 años se duplicó (p <0,001) (Tabla 3, Modelo 2). Por otra parte, en los colegios en zonas urbanas hubo menor probabilidad de estar tratado (OR 0,83; p <0,001) y por cada año que avanza el periodo experimental también se redujo la probabilidad de que el niño que se incorporaba al estudio estuviera ya tratado. (OR 0,92; p <0,001) (Tabla 3, Modelo 2).
El modelo de predicción de quién tenía tratamiento fue muy preciso con un error medio de 0,96% y una Chi-cuadrado de diferencia predicho/observado de 0,21 datos no mostrados. Los resultados de agrupar los individuos ordenados según su riesgo predicho, en 10 grupos (deciles) de tamaño similar, no difirieron mucho de lo observado (Tabla 4).
| Tabla 4. Calibración de la casuística estimada y observada según los gradientes de riesgo de ser tratados los niños “no-normales” | |||||
|---|---|---|---|---|---|
| Decil | n | Riesgo medio estimado | Riesgo medio observado | IC 95% | |
| Observado inferior | Observado superior | ||||
| D1 | 2512 | 14,33% | 13,69% | 12,35% | 15,04% |
| D2 | 2484 | 17,04% | 17,59% | 16,10% | 19,09% |
| D3 | 2007 | 18,91% | 19,38% | 17,65% | 21,11% |
| D4 | 2468 | 20,89% | 19,49% | 17,93% | 21,05% |
| D5 | 2524 | 22,70% | 23,73% | 22,07% | 25,39% |
| D6 | 2155 | 24,66% | 23,53% | 21,74% | 25,32% |
| D7 | 2311 | 26,37% | 28,17% | 26,34% | 30,00% |
| D8 | 2291 | 29,12% | 28,68% | 26,83% | 30,53% |
| D9 | 2263 | 33,23% | 32,57% | 30,64% | 34,50% |
| D10 | 2304 | 40,24% | 40,58% | 38,58% | 42,59% |

DISCUSIÓN
La prevalencia de niños “sospechosos” en los 140 102 niños alicantinos de 4 a 6 años estudiados, tuvo variaciones a lo largo de las distintas campañas oftalmológicas pediátricas, siendo el valor máximo alcanzado de 23,9% y el valor mínimo, de 8,54% (Tabla 1). Ambos valores están muy por encima de la media internacional, establecida en torno al 1 y 5%5,11,12. Si bien los valores más bajos resultan más concordantes con los valores establecidos en estudios de prevalencia para otras zonas españolas (7,5-9,8%)13,14.
La alta prevalencia de niños “sospechosos” a partir del curso 2008-2009 (12,80-23,89%) (Tabla 1), podría atribuirse a las diferencias observadas en la composición de la muestra por grupos de edad en cada curso (Fig. 2). Dada la asociación entre “sospechosos” de ambliopía y edad (Tabla 2 y Fig. 1) y entre “sospechosos” de ambliopía y curso del periodo experimental (Tabla 1 y Fig. 1), los cursos con niños más mayores aumentan la proporción de niños “sospechosos” (Fig. 2). Estos resultados vienen a coincidir con los obtenidos por otros autores sobre la importancia de las campañas de detección muy tempranas para lograr un tratamiento precoz en los niños15-19. Por otra parte, la disparidad en los resultados de prevalencia de ambliopía, entre los distintos estudios publicados, podría deberse a la falta de unanimidad de criterios para determinar la edad más adecuada de la población infantil, pruebas de cribado específicas, criterios de diagnóstico o preparación del personal evaluador, entre otros factores20-22.
Al igual que en otros estudios previos23,24, en la población objeto de estudio no se detectó efecto del sexo en la prevalencia de “sospechosos” (Tabla 2), lo que podría atribuirse al alto equilibrio entre niñas y niños en la muestra (datos no mostrados).
La literatura existente respecto a la prevalencia de la ambliopía en niños de poblaciones rurales es bastante contradictoria25-27. Los resultados obtenidos muestran una prevalencia levemente inferior en zona rural respecto a las semiurbanas y urbanas25 (Tabla 2), a pesar de que la población rural suele presentar mayores dificultades para acceder a una sanidad de calidad (pública o privada)28. Este hecho podría adscribirse a que los niños de zonas rurales viven en un ambiente mucho más saludable que los de zonas urbanas o semiurbanas.
Los resultados obtenidos tras la dicotomización de los datos en niños “normales” y “no-normales” apoyan la idea de que los niños de colegios privados presentan mayor probabilidad de acceder al tratamiento de la ambliopía respecto a los niños de otros colegios (Tabla 3) por las razones socioeconómicas apuntadas. El hecho de que la probabilidad de acceso al tratamiento sea superior en niños de mayor edad no puede adscribirse al efecto de concienciación de los padres por las campañas de cribado realizadas, ya que los datos utilizados provienen de niños cribados por primera vez. Quizás la causa del comportamiento observado sea que a mayor edad los síntomas de la ambliopía se hacen más evidentes y los niños pueden colaborar en mayor medida.
La disminución de la probabilidad de acceder al tratamiento de la ambliopía a lo largo del periodo experimental y en zonas urbanas resulta difícil de explicar (Tabla 3), y esencialmente en este último caso por la facilidad de acceso a la sanidad pública y/o privada. Sin embargo, el muy bajo error de predicción del modelo utilizado induce a pensar en la intervención de causas tales como una disminución de los diagnósticos tempranos de la ambliopía infantil y la consiguiente puesta en tratamiento.
Los resultados de esta investigación han demostrado que existe una elevada prevalencia de niños sospechosos de ambliopía en la provincia de Alicante, principalmente en los niños cribados de mayor edad y en los grupos de nivel socioeconómico más bajo. Por tanto, es razonable concluir enfatizando la gran importancia de las campañas de prevención y detección de la ambliopía en niños de preescolar, dado que la eficacia de su tratamiento depende de la precocidad del diagnóstico, equiparando consecuentemente la probabilidad de acceso al tratamiento de la ambliopía. Resulta imprescindible que los organismos internacionales normalicen distintos criterios tales como la edad más adecuada de la población preescolar para estas pruebas, así como determinar las pruebas de cribado específicas, los criterios de diagnóstico y la cualificación del personal evaluador, con el fin de facilitar la investigación sobre la prevalencia.
CONFLICTO DE INTERESES
Jorge l. Alió es el presidente de la Fundación que lleva su nombre. El resto de los autores no tienen intereses comerciales relevantes que declarar para el presente estudio.
Financiación. El estudio se ha realizado y en parte financiado en el marco de la Red Temática de Investigación Cooperativa en Salud (RETICS), número de referencia RD16/0008/0012.
ABREVIATURAS
AV: agudeza visual.
AGRADECIMIENTOS
A la Fundación Jorge Alió por poner a nuestra disposición los datos de tantos años de trabajo. Al Dr. Alejandro Galindo, de la Universidad de Sevilla, por su ayuda e interés mostrado.
BIBLIOGRAFÍA
- Braverman RS. Introduction to Amblyopia. En: American Academy of Ophthalmology [en línea] [consultado el 23/08/2022]. Disponible en www.aao.org/disease-review/amblyopia-introduction
- Casas-Llera P, Ortega P, Rubio I, Santos V, Prieto MJ, Alió JL. Validation of a school-based amblyopia screening protocol in a kindergarten population. Eur J Ophthalmol. 2016;26:505-9.
- Rajavi Z, Sabbaghi H, Baghini AS, Yaseri M, Moein H, Akbarian, et al. Prevalence of amblyopia and refractive errors among primary school children. J Ophthalmic Vis Res. 2015;10:408-16.
- Wallace DK, Repka MX, Lee KA, Melia M, Christiansen SP, Morse CL, et al. Amblyopia Preferred Practice Pattern. Ophthalmology. 2018;125:105-42.
- Li YP, Zhou MW, Forster SH, Chen SY, Qi X, Zhang HM, et al. Prevalence of amblyopia among preschool children in central south China. Int J Ophthalmol. 2019;12:820-5.
- Martínez J, Cañamares S, Saornil MA, Almaraz A, Pastor JC. Prevalence of amblyogenic diseases in a preschool population sample of Valladolid, Spain. Strabismus. 1997;5:73-80.
- Merchante Alcántara M. Ambliopía y estrabismo. Pediatr Integral. 2018;XXII:32-44.
- Becker R, Hübsch S, Gräf MH, Kaufmann H. Examination of young children with Lea symbols. Br J Ophthalmol. 2002;86:513-6.
- Méndez Llatas M, Delgado Domínguez JJ. Oftalmología: exploración del niño estrábico; detección precoz. Detección precoz de los trastornos de refracción y ambliopía. Pediatr Aten Primaria. 2011;13:163-88.
- Parra B AJ. Tamización de ambliopía en cuidado primario. Universitas Médica. 2009;50:225-36 [en línea] [consultado el 23/08/2022]. Disponible en www.redalyc.org/articulo.oa?id=231018809008
- Thompson JR, Woodruff G, Hiscox FA, Strong N, Minshull C. The incidence and prevalence of amblyopia detected in childhood. Public Health. 1991;105:455-62.
- Hartmann EE, Dobson V, Hainline l, Marsh-Tootle W, Quinn GE, Ruttum MS, et al. Preschool vision screening: summary of a task force report. Ophthalmology. 2001;108:479-86.
- Gil de Gómez G. Detección de anomalías oculares. Acta Estrabológica. 1986;14:51-61.
- Fernández-Valles MC. Estudio epidemiológico de la ambliopía en la población infantil de nuestra área hospitalaria [tesis doctoral]. Universidad de Sevilla. 2003. 214 pp.
- Jensen H, Goldschmidt E. Visual acuity in Danish school children. Acta Ophthalmol (Copenh). 1986;64:187-91.
- Eibschitz-Tsimhoni M, Friedman T, Naor J, Eibschitz N, Friedman Z. Early screening for amblyogenic risk factors lowers the prevalence and severity of amblyopia. J AAPOS. 2000;4:194-9.
- Al-Tamimi E, Shakeel A, Yassin SA, Ali SI, Khan UA. A clinic-based study of refractive errors, strabismus, and amblyopia in pediatric age-group. J Family Community Med. 2015;22:158-62.
- Ehrlich MI, Reinecke RD, Simons K. Preschool vision screening for amblyopia and strabismus. Programs, methods, guidelines, 1983. Surv Ophthalmol. 1983:28:145-63.
- Mocanu V, Horhat R. Prevalence and Risk Factors of Amblyopia among Refractive Errors in an Eastern European Population. Medicina (Kaunas). 2018;54:1-11.
- Martín Martín R, Bilbao Sustacha JA, Collado Cuco A. Cribado visual en atención primaria, ¿cómo se realiza? Rev Pediatr Aten primaria. 2013;15:221-7.
- Powell C, Porooshani H, Bohorquez MC. Screening for amblyopia in childhood. Cochrane Database Syst Rev. 2005:CD005020.
- Kemper AR, Margolis PA, Downs SM, Bordley WC. A Systematic Review of Vision Screening Tests for the Detection of Amblyopia. Pediatrics. 1999;104;1220-2.
- Yekta A, Hashemi H, Azizi E, Rezvan F, Ostadimoghaddam H, Derakhshan A, et al. The prevalence of amblyopia and strabismus among schoolchildren in Northeastern Iran, 2011. Iran J Ophthalmol. 2012;24:3-10.
- Rezvan F, Khabazkhoob M, Fotouhi A, Hashemi H, Ostadimoghaddam H, Heravian J, et al. Prevalence of refractive errors among school children in Northeastern Iran. Ophthalmic Physiol Opt. 2012;32:25-30.
- Padhye AS, Khandekar R, Dharmadhikari S, Dole K, Gogate P, Deshpande M. Prevalence of uncorrected refractive error and other eye problems among urban and rural school children. Middle East Afr J Ophthalmol. 2009;16:69-74.
- Verma R, Rathi M, Dhull CS, Sachdeva S, Phogat J. Prevalence and causes of low vision among urban and rural school children. Int J Community Med Public Health. 2018;5:5310-5.
- Lu W, Yu X, Zhao l, Zhang Y, Zhao F, Wang Y et al. Enhanced Gray Matter Volume Compensates for Decreased Brain Activity in the Ocular Motor Area in Children with Anisometropic Amblyopia. Neural Plast. 2020;2020(ID8060869):1-7.
- Sharma A, Wong AM, Colpa l, Jin YP. Socioeconomic status and utilization of amblyopia services at a tertiary pediatric hospital in Canada. Can J Ophthalmol. 2016;51:452-8.