Vol. 21 - Num. 83
Originales
¿Es posible detectar casos de acoso escolar a través de la presencia de problemas psicosomáticos?
Rosa M.ª Fuentes Chacóna, M.ª José Simón Saiza, Margarita Garrido Abejara, M.ª Dolores Serrano Parraa, M.ª José Díaz Valentína, Santiago Yubero Jiménezb
aFacultad de Enfermería. Universidad de Castilla-La Mancha. Cuenca. España.
bFacultad de Ciencias de la Educación y Humanidades. Universidad de Castilla-La Mancha. Cuenca. España.
Correspondencia: RM Fuentes . Correo electrónico: rosa.fuentes@uclm.es
Cómo citar este artículo: Fuentes Chacón RM, Simón Saiz MJ, Garrido Abejar M, Serrano Parra MD, Díaz Valentín MJ, Yubero Jiménez S. ¿Es posible detectar casos de acoso escolar a través de la presencia de problemas psicosomáticos? Rev Pediatr Aten Primaria. 2019;21:231-8.
Publicado en Internet: 01-08-2019 - Número de visitas: 17556
Resumen
Introducción: la elevada prevalencia del acoso escolar y sus consecuencias lo convierten en un problema de salud pública. Objetivo: analizar, en una población de adolescentes escolarizados, la prevalencia de acoso escolar y su asociación con problemas psicosomáticos.
Material y métodos: estudio transversal de una muestra representativa de 844 estudiantes en cinco institutos de educación secundaria (IES) de Cuenca (España). Mediciones principales: acoso escolar mediante la subescala aceptación social del KIDSCREEN-52 y problemas psicosomáticos con la escala PSP.
Resultados: la prevalencia de acoso escolar fue del 29,5%, sin deferencias significativas por sexo ni edad. Las chicas y los adolescentes de mayor edad presentaron problemas psicosomáticos significativamente más altos. Tanto en chicas como en chicos, una mayor presencia de estos se asoció con ser víctima de acoso escolar. Las ecuaciones de regresión realizadas para cada uno de los problemas psicosomáticos mostraron que, además de la influencia del sexo y la edad, ser víctima de acoso escolar es un predictor de peor salud psicosomática y de peor calidad de vida. Los modelos que explicaron mayor porcentaje de la varianza fueron el índice de psicosomáticos (21%), sentirse triste (15%), dolor de cabeza (10%) y dolor de estómago (11%).
Conclusiones: los problemas psicosomáticos son frecuentes en adolescentes y especialmente entre las víctimas de acoso escolar. Es aconsejable que los profesionales de la salud, especialmente médicos y enfermeras, consideren seriamente la posibilidad de estar ante una víctima de acoso cuando un adolescente exhibe sintomatología psicosomática, especialmente la relacionada con tristeza, dolor de cabeza o de estómago sin causa orgánica aparente.
Palabras clave
● Acoso escolar ● Adolescencia ● Calidad de vida relacionada con la salud ● Problemas psicosomáticosINTRODUCCIÓN
El acoso escolar es una conducta intimidatoria, agresiva y repetitiva que ejerce un miembro del grupo de pares y se manifiesta en conductas como maltrato físico o psicológico, hostigamiento o aislamiento que buscan dañar, incomodar, ridiculizar o minar la autoestima del acosado1,2. A pesar de las diferencias socioculturales entre diferentes países, el acoso escolar es un fenómeno cotidiano que está presente en múltiples contextos sociales3,4. Los estudios muestran una amplia variabilidad en cuanto a las cifras de prevalencia. Según el estudio realizado en 40 países y con una muestra de 202 056 adolescentes, la prevalencia se sitúa en un amplio rango entre 8,6-45,2% para los chicos y 4,8-35,8% entre las chicas3. Las cifras para España también recogen una amplia variabilidad, desde el 10,7% encontrado por García Continente5 al 23,7% proporcionado por Analitis6.
El fenómeno afecta a una población vulnerable como son los niños y adolescentes y representa una amenaza para el desarrollo, el bienestar y la calidad de vida relacionada con la salud de estos7,8. La magnitud del problema y sus consecuencias para la salud hace que este fenómeno adquiera un interés internacional y favorece que investigadores, padres, educadores y profesionales de la salud presten atención al acoso escolar.
La intimidación en el entorno escolar adquiere características específicas, se produce en un espacio físico reducido y con una interacción prolongada en el tiempo. En el contexto educativo, la violencia entre pares subyace sin hacerse en muchos casos visible para padres y educadores9, sin embargo, los estudios indican que ser acosado tiene consecuencias físicas, psicológicas y sociales negativas para la vida de niños y adolescentes1. Ser víctima de acoso escolar predice problemas de salud física y mental10,11, problemas emocionales12 y menor percepción de calidad de vida13. Además, es razonable suponer que ser acosado tiene consecuencias para el rendimiento educativo14.
Los síntomas psicosomáticos pueden ser una expresión de malestar emocional15 y constituir una manifestación temprana de acoso. Como muestran estudios de metaanálisis recientes, los problemas psicosomáticos son frecuentes entre adolescentes víctimas de acoso escolar16. Sin embargo, a pesar de la importancia del tema, en España son escasos los estudios que relacionen acoso escolar y problemas psicosomáticos.
Con estos antecedentes nuestros objetivos fueron: determinar la prevalencia de acoso escolar y analizar la relación entre ser víctima y la presencia de síntomas psicosomáticos en adolescentes matriculados en institutos de educación secundaria (IES) de Cuenca (España).
MATERIAL Y MÉTODOS
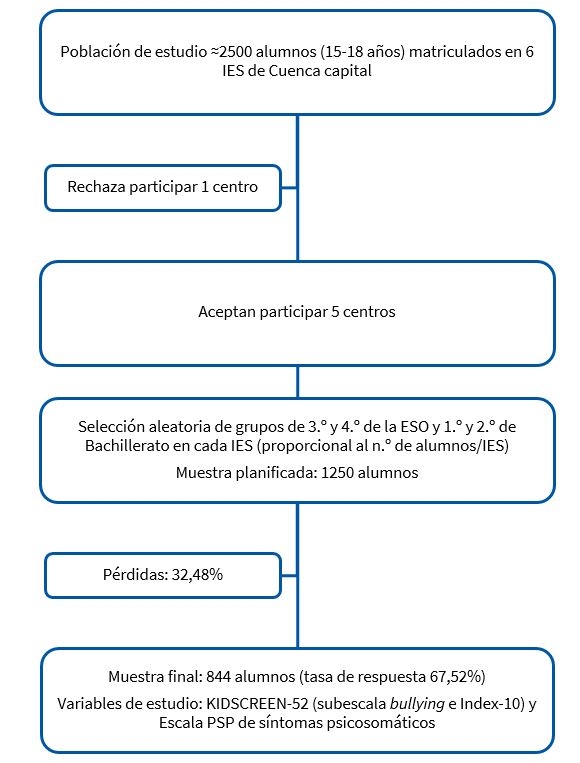
Estudio observacional, descriptivo, transversal y multicéntrico realizado en cinco IES públicos de Cuenca capital. Participaron adolescentes de edades comprendidas entre los 15 y los 18 años que cursaban 3.º y 4.º de Educación Secundaria Obligatoria (ESO) y 1.º y 2.º de Bachillerato. En cada nivel académico se seleccionaron aleatoriamente y de forma proporcional al tamaño de cada IES los grupos a los que se les administró el cuestionario (Fig. 1). Los criterios de inclusión fueron pertenecer a las clases aleatoriamente seleccionadas y entregar el consentimiento informado (otorgado por los padres en los menores y por ellos mismos en los mayores de edad). La población de estudio era de 2500, se calculó el tamaño muestral en 526 (IC = 99% y e = 2%), pero ampliamos la muestra porque esperábamos posibles pérdidas. El protocolo fue aprobado por los servicios periféricos de la Consejería de Educación, Cultura y Deporte de Castilla-La Mancha.
| Figura 1. Proceso de selección de la muestra |
|---|
 |

Instrumentos
La recogida de datos se hizo mediante cuestionario autoadministrado que incluyó variables sociodemográficas como edad y sexo y los siguientes instrumentos estandarizados:
- Los síntomas psicosomáticos se evaluaron mediante la escala PSP17 que hace referencia a ocho problemas comunes: dolor de cabeza y estómago, falta de apetito, dificultad para dormir, tristeza, mareo, nerviosismo y problemas de concentración; los ítems se evalúan mediante una escala tipo Likert. Los valores de los ítems se sumaron para formar un índice que osciló entre 0 y 32, siendo los valores más altos indicativos de síntomas más frecuentes. La escala mostró una buena consistencia interna (α de Cronbach = 0,76).
- El acoso escolar se evaluó mediante la subescala aceptación social del cuestionario de calidad de vida relacionada con la salud (CVRS) KIDSCREEN-5218, igual que en otros artículos similares6. Incluye tres ítems: “¿Has tenido miedo de otros/as chicos/as?”; “¿Se han burlado de ti otros/as chicos/as?” y “¿Te han amenazado o maltratado (física o psicológicamente) otros/as chicos/as?”. Las puntuaciones se calculan, de acuerdo con los métodos descritos por los autores de la escala original mediante el uso de análisis de Rash, así las puntuaciones de aceptación social o acoso escolar se estandarizan a una media de 50 y una desviación estándar de 1019. Las puntuaciones más altas indican ausencia de acoso escolar. La consistencia interna de la subescala fue aceptable (α de Cronbach = 0,77).
- La calidad de vida se evaluó mediante el KIDSCREEN-Índex10, una medida sumaria derivada del KIDSCREEN-52. Puntuaciones más altas significan mejor calidad de vida.
Análisis de datos
El análisis y procesamiento de los datos se hizo con Statistical Package for the Social Sciences (SPSS versión 23). Para determinar la prevalencia de acoso escolar se siguieron los criterios utilizados en estudios similares6, de forma que trasformamos la variable cuantitativa en una variable dicotómica considerando dos categorías: víctima de acoso escolar los que obtuvieron puntuaciones de <40 y no víctima de acoso escolar para los que puntuaron >40. Utilizamos la prueba t de Student para testar las diferencias en la presencia de síntomas psicosomáticos y CVRS entre las víctimas y las no víctimas.
Finalmente realizamos análisis multivariantes (regresión lineal por pasos), considerando como variable dependiente cada uno de los síntomas psicosomáticos, el índice de estos y la CVRS. Como variables control, en el primer paso se introduce la edad y el sexo y en el segundo paso la variable independiente (víctima de acoso escolar), al objeto de determinar la modificación en la varianza explicada (R2).
RESULTADOS
De los 844 participantes el 55,7% fueron chicas. La media de edad fue de 16,3 ± 1 años.
La prevalencia de acoso escolar encontrada fue del 29,5%, sin diferencias significativas por sexo (Tabla 1). Respecto a los síntomas psicosomáticos, las chicas presentan valores significativamente más altos en el índice (11 ± 4,6 frente a 7,7 ± 4,2 en chicos) y en cada uno de los síntomas psicosomáticos analizados. En ambos sexos, los síntomas psicosomáticos que se presentaron con mayor asiduidad fueron: dificultad de concentración (1,8 ± 0,9 frente a 1,9 ± 0,9 en chicas), dolor cabeza (0,9 ± 0,9 frente a 1,4 ± 0,9 en chicas), sentirse tenso (1,1 ± 1,0 frente a 1,4 ± 1,0 en chicas) y sentirse triste (0,9 ± 0,9 frente a 1,4 ± 1,0 en chicas). En cuanto a la calidad de vida, los chicos presentaron valores significativamente más altos (48,1 ± 6,7 frente a 44,6 ± 7,2).
| Tabla 1. Características generales de la muestra diferenciadas por sexo | |||||||
|---|---|---|---|---|---|---|---|
|
M ± DE |
Chicos M ± DE |
Chicas M ± DE |
p |
Edad 15-16 M ± DE |
Edad 17-18 M ± DE |
p | |
| Prevalencia acoso escolar | 29,5% | 29,9% | 29,1% | 0,801 | 28,9% | 30,3% | 0,704 |
| Índice de problemas psicosomáticos | 9,5 ± 4,7 | 7,7 ± 4,2 | 11,0 ± 4,6 | 0,000 | 8,8 ± 4,7 | 10,5 ± 4,6 | 0,000 |
| Dificultad para concentrarse | 1,9 ± 0,9 | 1,8 ± 0,9 | 1,9 ± 0,9 | 0,006 | 1,7 ± 0,9 | 2,0 ± 0,9 | 0,000 |
| Dificultad para dormir | 1,1 ± 1,0 | 0,9 ± 1,0 | 1,2 ± 1,0 | 0,001 | 1,0 ± 1,0 | 1,2 ± 1,0< | 0,010 |
| Dolor de cabeza | 1,2 ± 0,9 | 0,9 ± 0,9 | 1,4 ± 0,9 | 0,000 | 1,1 ± 0,9 | 1,4 ± 0,9 | 0,000 |
| Dolor de abdomen | 1,1 ± 0,9 | 0,8 ± 0,7 | 1,3 ± 0,9 | 0,000 | 1,0 ± 0,8 | 1,2 ± 0,9 | 0,004 |
| Sentirse tenso | 1,3 ± 1,0 | 1,1 ± 1,0 | 1,4 ± 1,0 | 0,000 | 1,2 ± 1,0 | 1,5 ± 1,0 | 0,000 |
| Poco apetito | 0,9 ± 0,9 | 0,6 ± 0,8 | 1,2 ± 1,0 | 0,000 | 0,9 ± 1,0 | 0,9 ± 0,9 | 0,322 |
| Sentirse triste | 1,1 ± 1,0 | 0,9 ± 0,9 | 1,4 ± 1,0 | 0,000 | 1,0 ± 1,0 | 1,3 ± 1,0 | 0,001 |
| Sentirse mareado | 0,7 ± 0,8 | 0,4 ± 0,6 | 0,8 ± 0,9 | 0,000 | 0,6 ± 0,8 | 0,7 ± 0,8 | 0,003 |
| Aceptación social (acoso escolar) | 46,9 ± 9,9 | 46,9 ± 9,4 | 47,0 ± 10,2 | 0,857 | 46,7 ± 9,7 | 47,2 ± 10,1 | 0,452 |
| KIDSCREN-Índex 10 | 46,1 ± 7,2 | 48,1 ± 6,7 | 44,6 ± 7,2 | 0,000 | 46,7 ± 7,2 | 45,4 ± 7,1 | 0,008 |

Respecto a la relación entre ser víctima de acoso y la presencia de problemas psicosomáticos, los resultados se pueden observar en la Tabla 2, e indican que ser víctima de acoso se asocia de forma significativa con valores más altos en todos los problemas psicosomáticos analizados, así como con peor percepción de calidad de vida. Sin embargo, estos resultados varían cuando los análisis se realizan de forma diferenciada según el sexo. En el caso de los chicos víctimas, la asociación se produjo con dolor de cabeza, dolor de estómago, sentirse tenso, poco apetito, sentirse triste y mareado; mientras que en las chicas lo hizo con dificultad de concentración, dificultad para dormir, dolor de cabeza, sentirse tensa, sentirse triste y sentirse mareada.
| Tabla 2. Relación entre síntomas psicosomáticos y acoso escolar. Diferencias por sexo | |||||||
|---|---|---|---|---|---|---|---|
| Chicos | Chicas | Total | |||||
| (M ± DE) | p | (M ± DE) | p | (M ± DE) | p | ||
| Índices psicosomáticos | Víctimas | 9,3 ± 4,4 | 0,000 | 13,0 ± 4,5 | 0,000 | 11,3 ± 4,8 | 0,000 |
| No víctimas | 7,1 ± 4 | 10,2 ± 4,5 | 8,8 ± 4,5 | ||||
| Dificultad para concentrarse | Víctimas | 1,9 ± 1 | 0,113 | 2,2 ± 0,9 | 0,000 | 2,1 ± 0,9 | 0,000 |
| No víctimas | 1,7 ± 0,9 | 1,8 ± 0,8 | 1,8 ± 0,9 | ||||
| Dificultad para dormir | Víctimas | 1,1 ± 1 | 0,126 | 1,4 ± 1 | 0,015 | 1,2 ± 1 | 0,005 |
| No víctimas | 0,9 ± 1 | 1,1 ± 1 | 1,0 ± 1 | ||||
| Dolor de cabeza | Víctimas | 1,2 ± 0,9 | 0,003 | 1,6 ± 1 | 0,004 | 1,4 ± 1 | 0,000 |
| No víctimas | 0,9 ± 0,8 | 1,4 ± 0,9 | 1,1 ± 0,9 | ||||
| Dolor de abdomen | Víctimas | 0,9 ± 0,7 | 0,034 | 1,4 ± 0,8 | 0,055 | 1,2 ± 0,8 | 0,008 |
| No víctimas | 0,7 ± 0,7 | 1,2 ± 0,9 | 1,0 ± 0,9 | ||||
| Sentirse tenso | Víctimas | 1,5 ± 1 | 0,000 | 1,7 ± 1 | 0,000 | 1,6 ± 1 | 0,000 |
| No víctimas | 1,0 ± 1 | 1,3 ± 1 | 1,2 ± 1 | ||||
| Tener poco apetito | Víctimas | 0,7 ± 0,8 | 0,032 | 1,3 ± 0,9 | 0,059 | 1,0 ± 0,9 | 0,010 |
| No víctimas | 0,5 ± 0,8 | 1,1 ± 1 | 0,8 ± 0,9 | ||||
| Sentirse triste | Víctimas | 1,2 ± 0,9 | 0,000 | 1,9 ± 1 | 0,000 | 1,62 ± 1 | 0,000 |
| No víctimas | 0,7 ± 0,8 | 1,2 ± 0,9 | 1,0 ± 0,9 | ||||
| Sentirse mareado | Víctimas | 0,6 ± 0,7 | 0,005 | 1,0 ± 0,9 | 0,002 | 0,8 ± 0,9 | 0,000 |
| No víctimas | 0,4 ± 0,6 | 0,7 ± 0,8 | 0,62 ± 0,8 | ||||
| Calidad vida Index-10 | Víctima | 45,2 ± 6,1 | 0,000 | 41,5 ± 5,5 | 0,000 | 43,1 ± 6,1 | 0,000 |
| No víctima | 48,3 ± 6,6 | 45,9 ± 7,5 | 47,3 ± 7,3 | ||||

Al objeto de evaluar la influencia que tiene ser acosado sobre las variables dependientes (percepción global de CVRS, índice de síntomas psicosomáticos y cada uno de ellos), elaboramos diferentes modelos de regresión lineal por pasos controlando en todos ellos el sexo y la edad. Nuestros resultados mostraron que, excepto la variable falta de apetito, todas las demás variables estudiadas se vieron afectadas de forma significativa por el hecho de sentirse acosado. Los modelos que explicaron mayor porcentaje de la varianza fueron los elaborados para el índice de psicosomáticos (21%), el índice global de CVRS (15%), sentirse triste (15%), dolor de cabeza (10%) y dolor abdominal (11%).
DISCUSIÓN
Nuestro estudio muestra que ser víctima de acoso es un predictor de riesgo de presentar síntomas psicosomáticos entre adolescentes escolarizados de 15 a 18 años. Los datos indican que ser acosado tiene también influencia sobre la CVRS. El efecto de ser acosado es más intenso y afecta especialmente a síntomas como sentirse triste y a la CVRS.
La prevalencia de víctimas de acoso encontrada es del 29,5% sin diferencias significativas por sexo ni grupo de edad. En la literatura científica se constata una amplia variabilidad3,5,6, que puede deberse tanto a las diferentes metodologías utilizadas en los estudios como a que los adolescentes no siempre se reconocen como acosados. Los instrumentos que incluyen el término acoso escolar ofrecen cifras de prevalencia más bajas, mientras que los que lo evalúan considerando el acoso escolar observado (conductas identificadas con acoso), como ocurre en nuestro estudio, ofrecen cifras más altas20. En consecuencia, cabe añadir que la mayoría de las conductas de acoso pueden permanecer clandestinas, ser banalizadas o trivializadas como normales entre los adolescentes y no como verdadera violencia21. Esta situación puede implicar la aceptación de las conductas de abuso y la percepción de que esas conductas son aceptables para resolver conflictos y obtener beneficios22. La disparidad en los datos habla de la complejidad del fenómeno y no resta importancia al problema, indica que es necesario contar con medidas precisas y fiables que no sobreestimen ni infravaloren el problema.
El acoso escolar no siempre deja lesiones observables, especialmente en el caso de las formas de maltrato más frecuentes (psicológico y relacional). Sin embargo, como muestran los estudios, puede tener efectos graves en la salud, el desarrollo socioemocional y el rendimiento académico de los adolescentes, generando problemas que pueden perdurar e influir en la vida adulta23,24. Probablemente, una de las primeras consecuencias detectables en las víctimas sea el aumento de mayores niveles de estrés y ansiedad social, que pueden manifestarse mediante múltiples problemas psicosomáticos, lo que permite sugerir que pueden estar afrontando una situación vital estresante.
Por lo tanto, la presencia de problemas psicosomáticos puede estar revelando una situación de acoso y pueden actuar como signos de alarma de un fenómeno que en muchas ocasiones permanece oculto y no es identificado en el contexto familiar, educativo o sanitario.
En nuestro estudio observamos que los adolescentes víctimas de acoso presentan valores más altos en todos los síntomas psicosomáticos estudiados, así como en el índice global; estos resultados confirman lo reseñado en estudios similares11,25. El síntoma psicosomático que, según nuestros resultados, fue el más afectado por el acoso escolar fue el sentimiento de tristeza. El acoso escolar se comporta como un fuerte predictor de sintomatología depresiva26 y como señalan los estudios, la presencia en las víctimas de esta sintomatología puede generar daños sobre su salud a corto, medio y largo plazo23. El acoso escolar puede dejar cicatrices muy significativas, en algunos casos, minimizar o banalizar este problema ha llevado a los adolescentes acosados a un inmenso malestar emocional que puede conducirle a provocarse daños, a veces, irreparables, como puede ser la pérdida de la vida27.
Como se ha señalado, el acoso escolar puede tener un efecto negativo sobre la salud mental individual, pero como muestra el estudio de Modin de 2015 también afecta al clima escolar general que puede traducirse en una “amenaza ambiental”28. En las clases donde la intimidación es frecuente, las no víctimas pueden percibir un riesgo potencial de convertirse en objetivo futuro, lo que les puede conducir a elevar el nivel de estrés; así, las clases con más estudiantes acosados, presentan más problemas psicosomáticos29. Lo que sugiere que el fenómeno de victimización entre iguales afecta negativamente a aquellos que están expuestos directamente, así como a sus compañeros de clase.
Este estudio presenta algunas limitaciones que conviene reconocer en la interpretación de resultados. Aunque parece razonable suponer una relación causal entre ser víctima de acoso y problemas psicosomáticos, es necesario considerar que, al tratarse de un estudio transversal, no proporciona información sobre la dirección causal de las asociaciones observadas y por lo tanto no nos dicen si ser acosado conduce a un aumento de los problemas de salud o si los adolescentes con problemas de salud están más expuestos a ser intimidados. Futuras investigaciones de tipo longitudinal permitirían aclarar estas cuestiones, aunque hay estudios que apuntan que la asociación puede ser bidireccional30.
CONCLUSIONES
Los hallazgos de este estudio pueden tener implicaciones importantes para los profesionales de la salud. La valoración cuidadosa de la salud debería incluir la valoración de los problemas psicosomáticos como expresiones de malestar emocional15 que podrían ser una señal de alerta de estar ante una posible víctima de acoso escolar.
El papel fundamental en el acoso escolar lo tiene la comunidad educativa, (alumnos, profesores y padres); sin embargo, los profesionales de salud de Atención Primaria también desempeñan un papel importante por su conocimiento previo del adolescente y su entorno familiar31. Aunque los efectos de la intimidación son raramente obvios y es poco probable que un adolescente verbalice que está siendo intimidado, en las consultas de Atención Primaria, pediatras y enfermeras pueden identificar las situaciones de acoso, aconsejar a las familias, tratar a los afectados y abogar por programas de prevención del acoso escolar en el contexto educativo22. En esta línea, es aconsejable que los profesionales de la salud, especialmente pediatras y enfermeras, consideren seriamente la posibilidad de estar ante una víctima de acoso cuando un adolescente exhibe varios problemas psicosomáticos sin causa orgánica, especialmente los relacionados con estado de ánimo deprimido.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS
CVRS: calidad de vida relacionada con la salud · ESO: Educación Secundaria Obligatoria · IC: intervalo de confianza · IES: institutos de educación secundaria.
BIBLIOGRAFÍA
- Olweus D. School bullying: development and some important challenges. An Rev Clin Psychol. 2013;9:751-80.
- Armero Pedreira P, Bernardino Cuesta B, Bonet de Luna C. Acoso escolar. Rev Pediatr Aten Primaria. 2011;13:661-70.
- Craig W, Harel-Fisch Y, Fogel-Grinvald H, Dostaler S, Simons-morton B, Molcho M, et al. A cross-national profile of bullying and victimization among adolescents in 40 countries. Int J Public Heal. 2009;54:216-24.
- Romera EM, Rey R, Ortega R. Prevalencia y aspectos diferenciales relativos al género del fenómeno bullying en países pobres. Psicothema. 2011;23:624-9.
- García Continente X, Pérez Giménez A, Manel Nebot A. Factores relacionados con el acoso escolar (bullying) en los adolescentes de Barcelona. Gac Sanit. 2010;24:103-8.
- Analitis F, Velderman MK, Ravens-Sieberer U, Detmar S, Erhart M, Herdman M, et al. Being Bullied: Associated Factors in Children and Adolescents 8 to 18 Years Old in 11 European Countries. Pediatrics. 2009;123:569-77.
- Chester KL, Spencer NH, Whiting L, Brooks FM. Association between experiencing relational bullying and adolescent health-related quality of life. J Sch Health. 2017;87:865-72.
- Hellfeldt K, Gill PE, Johansson B. Longitudinal analysis of links between bullying victimization and psychosomatic maladjustment in swedish schoolchildren. J Sch Violence. 2016;17:1-13.
- Informe del Defensor del Pueblo. Violencia escolar: el maltrato entre iguales en la Educación Secundaria Obligatoria 1999-2006. En: Defensor del Pueblo [en línea] [consultado el 30/07/2019]. Disponible en www.defensordelpueblo.es/informe-monografico/violencia-escolar-el-maltrato-entre-iguales-en-la-educacion-secundaria-obligatoria-1999-2006-nuevo-estudio-y-actualizacion-del-informe-2000-2007/
- Nielsen MB, Hetland J, Matthiesen SB, Einarsen S. Longitudinal relationships between workplace bullying and psychological distress. Scand J Work Environ Health. 2012;38:38-46.
- Gini G, Pozzoli T. Association between bullying and psychosomatic problems: a meta-analysis. Pediatrics. 2009;123:1059-65.
- Bond L, Carlin JB, Thomas L, Rubin K, Patton G. Does bullying cause emotional problems? A prospective study of young teenagers. BMJ. 2001;323:480-4.
- Hidalgo-Rasmussen C, Molina T, Molina R, Sepúlveda R, Martínez V, Montaño R, et al. Bullying y calidad de vida relacionada con la salud en adolescentes escolares chilenos. Rev Med Chi. 2015;143:716-23.
- Penning SL, Bhagwanjee A, Govender K. Bullying boys: the traumatic effects of bullying in male adolescent learners. J Child Adolesc Ment Heal. 2010;22:131-43.
- Fuentes Chacón RM, Simón Saiz MJ, Garrido Abejar M, Serrano Parra MD, Larrañaga Rubio ME, Yubero Jiménez S. Síntomas psicosomáticos como expresión del deterioro de la calidad de vida relacionada con la salud en adolescentes. Aten Primaria. 2017;50:493-9.
- Gini G, Pozzoli T. Bullied children and psychosomatic problems: a meta-analysis. Pediatrics. 2013;132:720-9.
- Hagquist C. Psychometric properties of the PsychoSomatic Problems scale: A Rasch analysis on adolescent data. Soc Indic Res. 2008;86:511-23.
- Rajmil L, Alonso J, Berra S, Ravens-Sieberer U, Gosch A, Simeoni MC, et al. Use of a children questionnaire of health-related quality of life (KIDSCREEN) as a measure of needs for health care services. J Adolesc Health. 2006;38:511-8.
- Ravens-Sieberer U, Gosch A, Rajmil L, Erhart M, Bruil J, Power M, et al. The KIDSCREEN-52 quality of life measure for children and adolescents: Psychometric results from a cross-cultural survey in 13 European countries. Value Heal. 2008;11:645-58.
- Sánchez-Queija I, García-Moya I, Moreno C. Trend analysis of bullying victimization prevalence in spanish adolescent youth at school. J Sch Health. 2017;87:457-64.
- Oñate A, Piñuel I. Informe Cisneros X. Acoso y violencia escolar en España. En: Bienestar y protección infantil [en línea] [consultado el 30/07/2019]. Disponible en www.bienestaryproteccioninfantil.es/fuentes1.asp?sec=27&subs=281&cod=2356&page=
- Buitrago Ramírez F, Ciurana Misol R, Chocrón Bentata L, Fernández Alonso M del C, García Campayo J, Montón Franco C, et al. Recomendaciones para la prevención de los trastornos de la salud mental en Atención Primaria. Aten Primaria. 2016;48:77-97.
- Sigurdson JF, Undheim AM, Wallander JL, Lydersen S, Sund AM. The long-term effects of being bullied or a bully in adolescence on externalizing and internalizing mental health problems in adulthood. Child Adolesc Psychiatry Ment Health. 2015;9:42.
- Vivolo-Kantor A, Martell B, Holland K, Westby R. A systematic review and contenct analysis of bullying and cyber-bullying measurement strategies. Aggress Violent Behav. 2014;19:423-34.
- Fekkes M, Pijpers F, Verloove-Vanhorick S. Bullying behavior and associations with psychosomatic complaints and depression in victims. J Pediatr. 2004;144:17-22.
- Pham TB, Adesman A. Increased risk of sadness and suicidality among victims of bullying experiencing additional threats to physical safety. Int J Adolesc Med Health. 2017;1:1-9.
- Kelly EV, Newton NC, Stapinski LA, Slade T, Barrett EL, Conrod PJ, et al. Suicidality, internalizing problems and externalizing problems among adolescent bullies, victims and bully-victims. Prev Med. 2015;73:100-5.
- Modin B, Låftman SB, Östberg V. Bullying in context: an analysis of psychosomatic complaints among adolescents in Stockholm. J Sch Violence. 2015;14:382-404.
- Laftman SB, Modin B. Peer victimization among classmates—associations with students’ internalizing problems, self-esteem, and life satisfaction. Int J Environ Res Public Health. 2017;14. pii: E1218.
- Fekkes M, Pijpers F, Fredriks A, Vogels T, Verloove-Vanhorick S. Do bullied children get ill, or do ill children get bullied? a prospective cohort study on the relationship between bullying and health-related symptoms. Pediatrics. 2006;117:1568-74.
- Galardi Andonegui M, Ugarte Líbano R. Maltrato entre iguales (bullying) en la escuela. ¿Cuál es el papel de los pediatras de Atención Primaria? Rev Pediatr Aten Primaria. 2005;7:11-9.




