Vol. 20 - Num. 77
Originales
Eficacia del programa Bicisalud en un grupo de escolares con peso excesivo
Enrique Rodríguez-Salinas Péreza, José Ignacio Leguina Aranzamendib, María Rosalía Martín Canoc, David Bescos Delgadod, Gonzalo de las Casas Cámarae
aPediatra. CS Colmenar Viejo Norte. Colmenar Viejo. Madrid. España.
bCiencias Biológicas. Madrid. España.
cMédico de Familia. CS Canillejas. Madrid. España.
dTécnico de Animación de Actividades Físicas y Deportivas. Estudiante de Ciencias de la Actividad Física y el Deporte. Madrid. España.
eMedicina Preventiva y Salud Pública. Hospital Universitario Rey Juan Carlos. Móstoles. Madrid. España.
Correspondencia: E Rodríguez-Salinas. Correo electrónico: erodriguez-salinas@pap.es
Cómo citar este artículo: Rodríguez-Salinas Pérez E, Leguina Aranzamendi JI, Martín Cano MR, Bescos Delgado D, de las Casas Cámara G. Eficacia del programa Bicisalud en un grupo de escolares con peso excesivo. Rev Pediatr Aten Primaria. 2018;20:53-63.
Publicado en Internet: 28-02-2018 - Número de visitas: 25582
Resumen
Introducción: ante la preocupante carga de enfermedad, debida al aumento del sedentarismo y exceso de peso infantil, se recomiendan afrontamientos multidisciplinares inductores de hábitos saludables de alimentación y ejercicio en toda la familia. Siguiendo estas recomendaciones se ha desarrollado el programa Bicisalud. La presentación de sus resultados es el principal objetivo de este trabajo.
Metodología: diseño cuasi experimental con análisis de variables en tres momentos: antes, tras la intervención y tres meses después. Entre 2016 y 2017 un total de 47 niños con sobrepeso u obesidad participaron en un programa complejo basado en salidas grupales en bicicleta, guiados por especialistas del deporte y salud, por entornos rurales. Se incluían actividades educativas sobre alimentación y ejercicio, entre otras. La variable principal fue la aptitud física a través de tres de sus principales factores. Las secundarias incluían aspectos somatométricos, de hábitos y autoconcepto.
Resultados: se consiguió una mejora estadísticamente significativa de los tres factores de la variable aptitud física y del perímetro abdominal en la evaluación inmediata al final de las actividades. Dicho efecto solo permaneció para la flexibilidad en la valoración realizada tras los tres meses de vacaciones. Los cambios en el resto de las variables no resultaron estadísticamente significativos en ningún momento.
Conclusiones: Bicisalud produjo una mejora moderada pero no mantenida en las principales variables de estudio. Programas más prolongados, que incluyan la promoción del uso habitual de la bicicleta, tienen indicios de mayor efectividad para la prevención y tratamiento del sedentarismo, el exceso de peso y sus consecuencias.
Palabras clave
● Ciclismo ● Ejercicio ● Estilo de vida sedentario ● Obesidad Infantil ● SobrepesoINTRODUCCIÓN
La creciente carga de enfermedad que genera el excesivo peso infantil, asociada al aumento del sedentarismo, puede llevar al colapso a muchos de los sistemas de salud mundiales, además de generar sufrimiento y gasto a los afectados1,2.
Esta gran carga de enfermedad se debe, por un lado, a su alta prevalencia, que alcanza a más del 40% de la población preadolescente de países como España3, con sensibles diferencias regionales y sociales4,5 y, por otro lado, a la elevada morbimortalidad derivada del binomio obesidad-sedentarismo, en forma de factores de riesgo cardiovascular, síndrome metabólico, diabetes, problemas ortopédicos, respiratorios, psicológicos y una menor esperanza de vida6-8. Los niños obesos tienen una pobre imagen de sí mismos y expresan sentimientos de inferioridad y rechazo, presentando alto riesgo de depresión y de ansiedad9-11.
Una vez establecido, el problema es difícil de revertir, al existir una clara correlación entre sobrepeso y obesidad en la infancia con los de la edad adulta7,12.
De todo esto han alertado tanto la Organización Mundial de la Salud1 como las administraciones sanitarias y sociedades científicas, generándose un sin número de recomendaciones, guías, estrategias y consensos destinados a tratar lo que ya se considera una acuciante epidemia de muy difícil afrontamiento13-17. En España, desde 2005, se desarrolla la Estrategia para la Nutrición, Actividad Física y Prevención de la Obesidad18. Su objetivo es sensibilizar a la población del problema que la obesidad representa e impulsar todas las iniciativas que contribuyan a lograr hábitos de vida saludables en la alimentación y en la práctica de actividad física regular, especialmente en los niños y jóvenes.
La obesidad sigue siendo uno de los problemas más difíciles de abordar en la práctica clínica. Los programas de tratamiento para la obesidad infantil y juvenil con enfoque multidisciplinar, donde intervienen conjuntamente distintos profesionales (psicólogos, profesionales de la actividad física, nutricionistas, médicos) implicados de forma conjunta y coordinada, han tenido mejores resultados que los programas consistentes en una única intervención19-23.
Las guías de práctica clínica actuales sobre la obesidad infantojuvenil recomiendan la instauración de programas comunitarios orientados a fomentar un estilo de vida saludable, una alimentación sana y la práctica de actividad física13,15-17.
Uno de los mayores problemas que surgen es el de la falta de adherencia a los programas de tratamiento y prevención. Ello va ligado a la dificultad de conseguir la fundamental motivación para el cambio de hábitos de vida21,24.
A la hora de conseguir inculcar el gusto por la actividad física diaria en los niños es fundamental que esta sea divertida. El uso de la bicicleta al aire libre tiene muchas características que pueden favorecer este objetivo. Además de elemento deportivo, siempre se ha considerado un juguete deseable en la edad infantil. Facilita la independencia en el trasporte diario y enseña a cuidar el medioambiente al no producir contaminación atmosférica25.
Los estudios sobre los efectos del uso de la bicicleta para la salud cardiovascular y la prevención y tratamiento del excesivo peso y sus comorbilidades se han centrado en el transporte diario al trabajo en los adultos o al colegio en los niños26-36. Hay sólidas evidencias de que los programas de promoción del uso cotidiano de la bicicleta producen beneficios que superan con creces a los riesgos37-44.
En consonancia con las recomendaciones de las guías y estrategias mencionadas, se ha desarrollado el programa multidisciplinar denominado Bicisalud, basado en paseos grupales en bicicleta por entornos naturales, junto a sesiones prácticas de educación sobre hábitos de vida saludables. El objetivo del presente trabajo es evaluar el impacto de dicho programa para mejorar las capacidades físicas y composición corporal de escolares con excesivo peso, así como su autoconcepto y hábitos de alimentación y ejercicio.
MATERIAL Y MÉTODOS
El estudio que se presenta tiene un diseño cuasiexperimental, con análisis de las variables de resultado antes y después de la intervención (Fig. 1). Se desarrolla desde el verano de 2015 al de 2017 en Colmenar Viejo, población de 48 000 habitantes al norte de Madrid, que cuenta con una nutrida red de caminos rurales en sus alrededores, con escaso tráfico motorizado, que permite compaginar el uso agropecuario con el ejercicio recreativo a pie o en bicicleta. Durante el primer verano, previo a su desarrollo, se contactó con instituciones locales y regionales sanitarias, para la difusión del proyecto y la obtención de la aprobación del comité ético correspondiente.
| Figura 1. Esquema del desarrollo del proyecto (2015-17) |
|---|
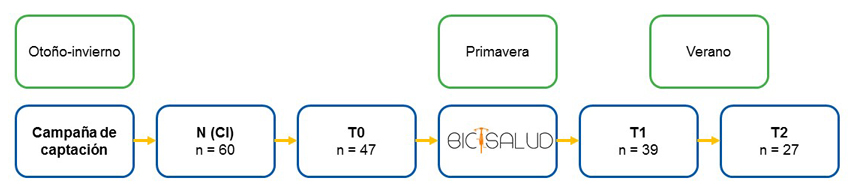 |

Muestra: los criterios de inclusión en el programa fueron: edad de 8 a 14 años, índice de masa corporal (IMC) igual o superior al p90 según las tablas de referencia del estudio de Hernández de 1988, saber montar en bicicleta y autorización paterna con consentimiento informado escrito. Los criterios de exclusión: padecer enfermedad crónica o subaguda que contraindique el ejercicio físico, participación concomitante en otros programas activos o terapias en curso medicamentosas o quirúrgicas de la obesidad.
La dificultad para reunir el grupo de voluntarios hizo necesaria una campaña intensiva de información durante las temporadas de otoño-invierno: en las consultas de los centros de salud de la zona; en la comunidad, con apoyo municipal mediante cartelería y buzoneo del material editado por el ayuntamiento (5000 folletos de mano y 80 carteles) (Fig. 2); en prensa y radio locales; en farmacias, polideportivos y en los centros escolares, mediante visitas a las aulas, que se aprovecharon para educación sobre hábitos de vida saludables a más de 2400 alumnos entre las dos temporadas. En relación con los recursos disponibles y contando con las posibles pérdidas experimentales, se decidió que habría que reunir un grupo de 45 participantes.
| Figura 2. Ejemplo de cartel editado por el Ayuntamiento de Colmenar Viejo |
|---|
 |

Variables de resultado
Principal: condición física, en sus tres principales facetas, resistencia aeróbica, fuerza y flexibilidad, que se valoró según los protocolos del EUROFIT45. Se tomaron medidas en los tres momentos: T0, T1 y T2 (Fig. 1) en las pistas deportivas de un instituto local, por los mismos observadores, pediatra y tres técnicos deportivos, que desconocían las mediciones obtenidas por los participantes en los momentos anteriores.
Tras un periodo breve de precalentamiento se registró la flexibilidad del tronco y los músculos isquiosurales con el test de Wells clásico, la fuerza explosiva de los miembros inferiores con el test de salto horizontal y la resistencia o capacidad aeróbica con el test de Course-Navette. Para el test de flexibilidad se utilizó un cajón de medición (flexómetro) y se realizaron tres intentos, escogiendo el mejor resultado. En el caso del test de fuerza se utilizó una cinta métrica e igualmente se realizaron tres intentos, escogiendo el mejor resultado. En el test de resistencia se utilizaron cuatro conos y cinta métrica para marcar el recorrido de 20 m y un ordenador con el protocolo del test, registrándose el número de ciclos ida-vuelta conseguido dividido por dos.
Secundarias: IMC; perímetro abdominal; autoconcepto; hábitos de alimentación y ejercicio.
Otros dos observadores en el centro de salud, médicos que desconocían igualmente los resultados de medidas anteriores, registraron en los tres momentos (T0, T1, T2) peso y talla, con ropa ligera y descalzos y cintura abdominal a la altura del ombligo, empleando los mismos instrumentos: báscula, tallímetro y cinta métrica, con precisiones de 100 g, 1 mm y 5 mm, respectivamente.
El IMC, con su percentil y número de desviaciones estándar (DE) (puntuación-z), se obtuvo mediante la calculadora virtual de la web EndocrinoPed”46. Para las variables psicológicas y conductuales se utilizaron el cuestionario de autoconcepto abreviado (CAF)47 y la batería Kreceplus para hábitos de alimentación-sedentarismo48.
Variable de intervención
Es la aplicación del programa multicomponente de educación grupal denominado Bicisalud. Comprende ejercicio físico e información interactiva sobre alimentación sana y valores medioambientales.
El ejercicio físico empleado fue montar en bicicleta. Los participantes debían utilizar obligatoriamente casco y un chaleco reflectante durante las actividades, así como cumplir las normas de seguridad vial. Se consiguieron hasta nueve bicicletas donadas para los que no tenían disponibilidad de una propia. El programa consistió en recorridos grupales por cañadas campestres, de dificultad creciente, fuera del horario escolar, a lo largo de doce semanas, con un total de 24 sesiones en cada temporada (Tabla 1). Los participantes se dividieron en dos grupos según edades, capacidad física o habilidad con la bicicleta. El grupo de menor edad o capacidad realizaba circuitos más cortos y sencillos (6-8 km) que el de mayor edad o habilidad (10-12 km). Ambos grupos eran guiados y dinamizados por al menos dos profesionales de la educación física o del ámbito de la salud. En casi todas las salidas participaron también familiares u otros voluntarios locales.
| Tabla 1. Esquema del desarrollo de las actividades en bicicleta del programa Bicisalud | ||||
|---|---|---|---|---|
| Semana | Sesiones/semana | Tiempo (min.) | Terreno | Dificultad |
| 1-3 | 1 | 60 | Fácil, llano | Ligera |
| 4-6 | 2 | 60 | Variable | Moderada |
| 7-9 | 3 | 90 | Complicado | Vigorosa |
| 10-12 | 3 | 90 | Exigente | Vigorosa |

Con objeto de reafirmar el carácter educativo del programa, se realizaron visitas a distintos espacios naturales y centros sociales relevantes de la localidad, como la dehesa, con sus yacimientos arqueológicos y riqueza ornitológica, el centro de acogida de animales, el centro para personas con discapacidad o la casa museo. De forma adicional, se realizaron tres talleres informativos en el centro de salud, con participación de familiares sobre: alimentación, compra saludable y riesgos/beneficios del uso de la bicicleta. El taller de alimentación fue dirigido por una nutricionista, una bióloga, una médica de familia y cuatro enfermeras. Se dividió en dos sesiones simultáneas, una para niños y niñas y otra para sus familiares. El de compra saludable lo impartió un pediatra e incluyó una visita a los puestos de fruta, verdura y pescado del comercio cercano. El de uso de la bicicleta lo guiaron dos de los técnicos que dirigían los paseos. Se creó un grupo de comunicación por teléfono móvil para facilitar la participación y concertar las citas o comunicar incidencias.
Al final de las salidas al campo se compartía una merienda saludable a base de fruta de temporada.
Análisis estadístico
Se realizó un análisis descriptivo univariado de la muestra. Las variables cuantitativas fueron descritas con medidas de tendencia central (media o mediana) y de dispersión (desviación estándar o rango intercuartílico). Previa comprobación de su distribución normal, se compararon las medias de las variables cuantitativas de los tres momentos mediante la prueba ANOVA para medidas repetidas (contrastándose el supuesto de homogeneidad de varianzas), los tres pares de momentos se compararon con la prueba t de Student para muestras relacionadas penalizándose por el método de Bonferroni, por lo que se fijó el nivel significación en 0,016. Para todo ello se utilizó la aplicación estadística SPSS® versión 18.
RESULTADOS
De los 60 candidatos (26 de 2016 y 34 de 2017) que firmaron el consentimiento informado para participar en Bicisalud, cumplieron criterios de inclusión 47 (25 + 22) que, tras las mediciones de las variables principales y secundarias (T0), comenzaron el programa de actividades que se desarrolló durante dos primaveras según el calendario flexible de salidas y talleres que se iba determinando. La media de edad al comienzo fue de 11,2 años (DE: 1,52), siendo el 57,45% de ellos niños y el 42,55% niñas. La mediana de asistencias a las actividades programadas fue de 16 (rango intercuartílico: 11-19).
En la Fig. 1 se detalla el efectivo muestral en cada momento (T0, T1, T2), ilustrando las pérdidas experimentales. Los resultados, meramente descriptivos, de las diferentes variables se exponen en la Tabla 2. El interés de esta tabla es únicamente el de documentar el trabajo que han supuesto las pérdidas experimentales, necesariamente eliminadas del análisis que se expone en las Tablas 3 y 4.
| Tabla 2. Resultados (M [DE]) de las medidas de las distintas variables en los tres momentos | |||
|---|---|---|---|
| T0 (n = 47) | T1 (n = 39) | T2 (n = 27) | |
| RA | 9,65 (4,25) | 12,95 (5,20) | 10,87 (4,67) |
| FL | 18,02 (7,01) | 19,77 (8,43) | 21,04 (8,01) |
| FU | 121,37 (21,7) | 129,21(21,76) | 126,65 (19,92) |
| IMC | 25,15 (2,58) | 24,60 (2,72) | 25,45 (3,2) |
| IMC-z | 2,38 (0,75) | 2,12 (0,83) | 2,34 (1,0) |
| PA | 86,96 (8,23) | 84,71 (8,24) | 88,46 (10,7) |
| KN | 6,89 (1,86) | 7 (1,92) | 6,04 (2,36) |
| KA | 5,83 (2,09) | 5,9 (2,16) | 5,59 (2,22) |
| AC | 28,02 (4,02) | 29,67 (4,50) | 28,81 (4,65) |

| Tabla 3. Resultados (M [DE]) de las medidas de las distintas variables en los tres momentos | ||||
|---|---|---|---|---|
| T0 | T1 | T2 | p* | |
| Variables | M (DE) | M (DE) | M (DE) | |
| RA n = 26 | 10,4 (5,1) | 13,7 (5,6) | 10,8 (4,7) | 0,003 |
| FL n = 26 | 19,1 (7,2) | 20,6 (8,7) | 21,0 (8,0) | 0,012 |
| FU n = 26 | 122,9 (18,8) | 129,2 (23,1) | 126,7 (19,9) | 0,014 |
| AC n = 27 | 28,0 (4,3) | 29,9 (4,5) | 28,8 (4,7) | 0,103 |
| Peso n = 27 | 55,1 (11,3) | 55,6 (11,7) | 58,5 (12,4) | <0,0001 |
| Talla n = 27 | 147 (9,4) | 149,5 (9,5) | 150,8 (9,2) | <0,0001 |
| IMC n = 27 | 24,9 (2,7) | 24,6 (2,9) | 25,5 (3,2) | <0,0001 |
| IMC-z n = 27 | 2,3 (0,8) | 2,1 (0,9) | 2,34 (1,0) | 0,002 |
| PA n = 27 | 87,2 (8,9) | 84,9(9,0) | 88,5 (10,7) | <0,0001 |
| KN n = 27 | 6,6 (1,8) | 7,0 (1,7) | 6,0 (2,4) | 0,036 |
| KA n = 27 | 5,5 (2,4) | 5,7 (2,4) | 5,6 (2,2) | 0,81 |

| Tabla 4. Resultados (M [DE]) de las medidas de las distintas variables en los tres momentos | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| T1-T0 | T2-T1 | T2-T0 | |||||||
| Variables | DM (DE) | IC 95 | p* | DM (DE) | IC 95 | p* | DM (DE) | IC 95 | p* |
| RA n = 26 | 3,3 (4,5) | 1,5 a 5,1 | 0,001 | -2,8 (4,7) | -4,7 a 0,92 | 0,005 | 0,44 (4,5) | -1,4 a 2,3 | 0,622 |
| FL n = 26 | 1,5 (2,9) | 0,3 a 2,7 | 0,015 | 0,4 (2,7) | -0,7 a 1,5 | 0,43 | 1,9 (3,1) | 0,7 a 3,2 | 0,004 |
| FU n = 26 | 6,3 (9,7) | 2,2 a 10,3 | 0,004 | -2,5 (11,3) | -7,1 a 2,0 | 0,264 | 3,7 (9,9) | -0,25 a 7,7 | 0,065 |
| AC n = 27 | 1,9 (4,3) | 0,2 a 3,6 | 0,032 | -1,1 (5,3) | -3,2 a 0,9 | 0,287 | 0,8 (4,7) | -1,1 a 2,6 | 0,399 |
| Peso n = 27 | 0,5 (2,4) | -0,4 a 1,5 | 0,257 | 2,9 (1,7) | 2,3 a 3,6 | 0,001 | 3,5 (2,9) | 2,3 a 4,7 | 0,001 |
| Talla n = 27 | 1,6 (0,7) | 1,3 a 1,9 | 0,001 | 1,4 (1,3) | 0,9 a 1,9 | 0,001 | 2,9 (1,3) | 2,4 a 3,5 | 0,001 |
| IMC n = 27 | -0,3 (1,1) | -0,7 a 0,2 | 0,185 | 0,8 (0,8) | 0,5 a 1,2 | 0,001 | 0,5 (1,3) | 0,04 a 1,0 | 0,036 |
| IMC-z n = 27 | -0,2 (0,4) | -0,36 a 0,04 | 0,019 | 0,20 (0,30) | 0,09 a 0,32 | 0,001 | 0,01 (0,5) | -0,17 a 0,18 | 0,947 |
| PA n = 27 | -2,2 (4,4) | -3,9 a 0,5 | 0,013 | 3,5 (3,7) | 2,0 a 4,9 | 0,001 | 1,2 (4,5) | -0,5 a 3,0 | 0,164 |
| KN n = 27 | 0,4 (1,8) | -0,32 a 1,06 | 0,284 | -0,92 (1,7) | -1,6 a 0,25 | 0,009 | -0,55 (2,0) | -1,3 a 0,22 | 0,154 |
| KA n = 27 | 0,22 (1,8) | -0,48 a 0,93 | 0,523 | -0,11 (1,9) | -0,88 a 0,66 | 0,77 | 0,11 (1,6) | -0,53 a 0,75 | 0,725 |

En estas se detalla el desarrollo del análisis estadístico de la muestra de participantes que terminó el programa, es decir solo los 27 (44,5% niños y 55,5% niñas) que fueron medidos en los tres momentos, si bien una de ellas faltó a las medidas de aptitud física.
A excepción del autoconcepto y la puntuación del cuestionario Kreceplus-Actividad, se identificó que, para el resto de las variables, las medias fueron diferentes en alguno de los momentos.
En relación con el periodo “finalización de la intervención (T1)” con respecto al “basal (T0)” se produjeron incrementos en la fuerza, la resistencia aeróbica, la flexibilidad y la talla, así como disminución del perímetro abdominal. Sin embargo, a los tres meses de seguimiento posintervención (T2) con respecto al momento T1, se produjeron disminuciones en la resistencia aeróbica y de la puntuación del cuestionario Kreceplus-Nutrición e incrementos en el peso, el IMC (y su distribución-z) y el perímetro abdominal, continuando el aumento de la talla. Los cambios observados entre la evaluación en T2 respecto a la situación basal, T0, fueron aumentos en la flexibilidad, peso y talla.
En pocas palabras, se puede decir que la aplicación del programa se acompañó de una mejora significativa rápida sobre la variable principal (aptitud física), que no se mantuvo tras los tres meses de vacaciones, salvo para el factor flexibilidad, que sí persistió en la mejoría. Las modificaciones encontradas en las otras variables no resultaron estadísticamente significativas.
Durante los dos periodos de actividades (tres meses/participante) se produjeron escasas caídas y pequeños accidentes que no supusieron lesiones de importancia ni alteración de la continuidad de la sesión en ninguno de los casos.
Hay que mencionar que el desarrollo del programa Bicisalud ha supuesto un ejemplo de actuación interactiva, con aspectos muy positivos, aunque no cuantificables, entre el centro de salud, la escuela primaria y secundaria, las instituciones deportivas, los participantes con sus familias, los monitores, además de grupos culturales, de acción social y medioambiental, en el marco de lo que se vienen denominando redes de promoción de salud local49.
Todo ello ha devenido en la financiación municipal para la próxima temporada de un nuevo programa Bicisalud, que se ofrece en esta ocasión a escolares independientemente de su IMC.
DISCUSIÓN
Bicisalud ha conseguido producir mejoras en la aptitud física de los niños participantes, como era el objetivo principal del programa, pero solo en el corto plazo. Este efecto desaparece en la valoración del mantenimiento que se realizó después de las vacaciones de verano, a excepción de la flexibilidad, que se mantuvo significativamente mejor que en la línea de base.
Al preguntar a los participantes sobre las actividades realizadas durante las vacaciones veraniegas y en particular sobre el uso de la bicicleta u otros ejercicios físicos, la mayoría de ellos contestaba que sus veranos habían sido bastante sedentarios y con un uso anecdótico de la bicicleta.
Esto concuerda con el gran incremento del sedentarismo a nivel global, que sin duda constituye uno de los puntales etiológicos de la creciente epidemia del excesivo peso y sus deletéreas consecuencias50-52. Es claramente visible cómo los niños se entretienen, a edades cada vez más tempranas, con actividades como contemplar de modo hipnótico el smartphone de los padres, hasta que obtienen el suyo, también cada vez antes. Es por esto por lo que el programa Bicisalud, aunque incluyendo también otros componentes, tenga su fundamento en la promoción de un ocio activo y también divertido mediante el ejercicio en bicicleta junto a compañeros de semejantes características.
El descenso que se consiguió en alguna de las variables secundarias como el IMC, la más atractiva socialmente, no llegó a la significación estadística y tampoco se mantuvo tras el verano. Por otro lado, en el mismo sentido, sí que resultó significativamente mejorado el perímetro abdominal, también indicador del exceso de grasa corporal, aunque también volviera a la línea basal tras el más inactivo verano. Otros investigadores han encontrado parecidas dificultades para estos objetivos con intervenciones de mayor envergadura21,23,28,51,53.
En el autoconcepto físico se produjo también una moderada mejoría, mantenida en este caso tras el verano, pero sin alcanzar significación estadística en ningún momento. La baja autoestima de los niños con sobrepeso u obesidad constituye un factor acompañante del problema, que es tanto causa como efecto y, aunque se tratase de un objetivo secundario para el proyecto, hubiera sido muy deseable conseguir sobre él una mejoría más consistente9-11.
Los aspectos en los que Bicisalud ha alcanzado los resultados menos favorables han sido las valoraciones en los test de hábitos de alimentación y ejercicio, los acreditados y conocidos Kreceplus19,21,24,48. Una explicación plausible de la ineficacia en este sentido es la necesidad de actuaciones de mayor intensidad y duración a través de diversos canales de comunicación para conseguir pequeñas modificaciones en los hábitos de vida, sobre todo cuando para ello se hace necesaria la implicación del conjunto del sistema familiar. Además, hay que tener en cuenta las presiones sociales que facilitan el ocio sedentario y nefastos hábitos de alimentación54.
La captación de participantes ha constituido uno de los principales escollos del proyecto Bicisalud. No es fácil que un niño o niña con sobrepeso dé el paso de inscribirse y por tanto reconocer el problema ante su comunidad. Esta dificultad para poder reunir la muestra total requerida fue el motivo de fragmentar el estudio en dos periodos. Por otro lado, fue un reto que, una vez superado, ha contribuido a generar cohesión y entusiasmo en todo el grupo de niños y colaboradores.
A pesar del carácter lúdico y aventurero de cada ruta ciclista y de la diversidad de actividades y personas que han dado dinamismo al programa, las pérdidas experimentales no fueron desdeñables lo que ha podido afectar los resultados finales.
En conclusión:
- Bicisalud es un programa con un perfil característico, novedoso y prometedor, para afrontar el grave problema de la inactividad y el sobrepeso en preadolescentes.
- Ha conseguido resultados positivos a corto plazo en la aptitud física de los participantes, aunque solo mantenidos a medio plazo para la flexibilidad.
- Sería interesante replicarlo con muestras mayores y aumentando su motivación para minimizar los abandonos durante el transcurso experimental, que han podido interferir el deseable escenario de pérdidas mínimas.
- Un aspecto clave para futuros diseños de mayor efectividad es conseguir duraciones mayores en la aplicación de la estrategia y, sobre todo, normalizar el uso de la bicicleta u otros sistemas de trasporte activo en la vida diaria de los escolares, sus vecinos y familiares.
ANEXOS
Se adjuntan tres documentos anexos disponibles en la página web de la revista:
- Relación de agradecimientos (Anexo 1).
- Tabla de resúmenes bibliográficos estructurados (Anexo 2).
- Álbum de fotos (Anexo 3).
CONFLICTO DE INTERESES
Los autores son usuarios asiduos de la bicicleta para el transporte o el ejercicio físico habitual.
ABREVIATURAS
CAF: cuestionario de autoconcepto abreviado • DE: desviación estándar • IMC: índice de masa corporal.
FINANCIACIÓN
I Beca AMPap de investigación en Pediatría de Atención Primaria. Ayuntamiento Colmenar Viejo. Fondos propios.
BIBLIOGRAFÍA
- Estrategia mundial sobre régimen alimentario, actividad física y salud. Sobrepeso y obesidad infantiles. En: Organización Mundial de la Salud [en línea] [consultado el 27/02/2018]. Disponible en www.who.int/dietphysicalactivity/childhood/es/
- Ding D, Lawson KD, Kolbe-Alexander TL, Finkelstein EA, Katzmarzyk PT, van Mechelen W, et al. The economic burden of physical inactivity: a global analysis of major non-communicable diseases. Lancet. 2016;388:1311-24.
- Estudio ALADINO 2015: Estudio de Vigilancia del Crecimiento, Alimentación, Actividad Física, Desarrollo Infantil y Obesidad en España 2015. En: Agencia Española de Consumo, Seguridad Alimentaria y Nutrición. Ministerio de Sanidad, Servicios Sociales e Igualdad [en línea] [consultado el 27/02/2018]. Disponible en www.aecosan.msssi.gob.es/AECOSAN/docs/documentos/nutricion/observatorio/Estudio_ALADINO_2015.pdf
- Sánchez Echenique M. Aspectos epidemiológicos de la obesidad infantil. Rev Pediatr Aten Primaria Supl. 2012;21:S9-14.
- Ninatanta Ortiz JA, Núñez Zambrano LA, García Flores SA, Romaní Romaní F. Factores asociados a sobrepeso y obesidad en estudiantes de educación secundaria. Rev Pediatr Aten Primaria. 2017;19:209-21.
- Baker JL, Olsen LW, Sorensen TI. Childhood body-mass index and the risk of coronary heart disease in adulthood. N Engl J Med. 2007;357:2329-37.
- Steinberger J, Moran A, Hong CP, Jacobs DR,Jr, Sinaiko AR. Adiposity in childhood predicts obesity and insulin resistance in young adulthood. J Pediatr. 2001;138:469-73.
- Paffenbarger RS Jr, Kampert JB, Lee IM, Hyde RT, Leung RW, Wing AL. Changes in physical activity and other lifeway patterns influencing longevity. Med Sci Sports Exerc. 1994;26:857-65.
- Erermis S, Cetin N, Tamar M, Bukusoglu N, Akdeniz F, Goksen D. Is obesity a risk factor for psychopathology among adolescents? Pediatr Int. 2004;46:296-301.
- D’Autume C, Musher-Eizenman D, Marinier E, Viarme F, Frelut ML, Isnard P. Eating behaviors and emotional symptoms in childhood obesity: a cross-sectional exploratory study using self-report questionnaires in 63 children and adolescents. Arch Pediatr. 2012;19:803-10.
- Ortega MA, Muros JJ, Palomares J, Martín JA, Cepero M. Influencia del índice de masa corporal en la autoestima de niños y niñas de 12-14 años. An Pediatr (Barc). 2015;83:311-7.
- Baird J, Fisher D, Lucas P, Kleijnen J, Roberts H, Law C. Being big or growing fast: systematic review of size and growth in infancy and later obesity. BMJ. 2005;331:929.
- Grupo de trabajo de la Guía de Práctica Clínica sobre la Prevención y el Tratamiento de la Obesidad Infantojuvenil. Centro Cochrane Iberoamericano, coordinador. Guía de Práctica Clínica sobre la Prevención y el Tratamiento de la Obesidad Infantojuvenil [versión resumida]. Plan de Calidad para el Sistema Nacional de Salud del Ministerio de Sanidad y Política Social. Agència d´Avaluació de Tecnologia i Recerca Mèdiques; 2009. Guías de Práctica Clínica en el SNS: AATRM N.º 2007/25. Disponible en www.guiasalud.es/GPC/GPC_452_obes_infantojuv_AATRM_compl.pdf
- Waters E, de Silva-Sanigorski A, Burford BJ, Brown T, Campbell KJ, Gao Y, et al. Interventions for preventing obesity in children. Cochrane Database Syst Rev. 2005;3:CD001871.
- Lau DC, Douketis JD, Morrison KM, Hramiak IM, Sharma AM, Ur E, et al. 2006 Canadian clinical practice guidelines on the management and prevention of obesity in adults and children [summary]. CMAJ. 2007;176:S1-13.
- National Clinical Guideline Centre. Obesity: identification, assessment and management of overweight and obesity in children, young people and adults. Londres: National Institute for Health and Care Excellence (NICE); 2014.
- August GP, Caprio S, Fennoy I, Freemark M, Kaufman FR, Lustig RH, et al. Prevention and treatment of pediatric obesity: an endocrine society clinical practice guideline based on expert opinion. J Clin Endocrinol Metab. 2008;93:4576-99.
- Estrategia para la Nutrición, Actividad Física y Prevención de la Obesidad (NAOS). En: Agencia Española de Consumo, Seguridad Alimentaria y Nutrición. Ministerio de Sanidad, Servicios Sociales e Igualdad [en línea] [consultado el 27/02/2018]. Disponible en www.aecosan.msssi.gob.es/AECOSAN/web/nutricion/seccion/estrategia_naos.htm
- Gussinyer S, Garcia-Reyna NI, Carrascosa A, Gussinyer M, Yeste D, Clemente M, et al. Cambios antropométricos, dietéticos y psicológicos tras la aplicación del programa “niños en movimiento” en la obesidad infantil. Med Clin (Barc). 2008;131:245-9.
- Serra-Paya N, Ensenyat A, Blanco A. Intervención multidisciplinar y no competitiva en el ámbito de la salud pública para el tratamiento del sedentarismo, el sobrepeso y la obesidad infantil: Programa NEREU. Apunts. Educación Física y Deportes. 2014;117:7-22.
- Rajmil L, Bel J, Clofent R, Cabezas C, Castell C, Espallargues M. Intervenciones clínicas en sobrepeso y obesidad: revisión sistemática de la literatura 2009-2014. An Pediatr (Barc). 2017;86:197-212.
- Fundación Thao. Programa Thao-salud infantil [en línea] [consultado el 27/02/2018]. Disponible en https://programathao.com/que-es/
- Pérez Solís D, Díaz Martín JJ, Álvarez Caro F, Suárez Tomás I, Suárez Menéndez E, Riaño Galán I. Efectividad de una intervención escolar contra la obesidad. An Pediatr (Barc). 2015;83:19-25.
- Gorrotxategi Gorrotxategi P, Leizaola Olarreaga L, Solorzano Sánchez C, García Conde G, Aguirre Sorondo B, Totoricaguena Imaz A, et al. Protocolo del estudio: abordaje del sobrepeso en Atención Primaria. Papel de la entrevista motivacional. Rev Pediatr Aten Primaria. 2014;16:e199-e207.
- Rissel CE, New C, Wen LM, Merom D, Bauman AE, Garrard J. The effectiveness of community-based cycling promotion: findings from the Cycling Connecting Communities project in Sydney, Australia. Int J Behav Nutr Phys Act. 2010;7:8.
- Grøntved A, Koivula RW, Johansson I, Wennberg P, Østergaard L, Hallmans G, et al. Bicycling to work and primordial prevention of cardiovascular risk: a cohort study among swedish men and women. J Am Heart Assoc. 2016;5:1-12.
- Chillón P, Villén-Contreras R, Pulido-Martos M, Ruiz JR. Desplazamiento activo al colegio, salud positiva y estrés en niños españoles. SPORT TK. 2017;6:117-24.
- Rosenberg DE, Sallis JF, Conway TL, Cain KL, McKenzie TL. Active transportation to school over 2 years in relation to weight status and physical activity. Obesity (Silver Spring). 2006;14:1771-6.
- Macridis S, García Bengoechea E. Adoption of safe routes to school in Canadian and the United States contexts: best practices and recommendations. J Sch Health. 2015;85:558-66.
- De Nazelle A, Nieuwenhuijsen MJ, Antó JM, Brauer M, Briggs D, Braun-Fahrlander C, et al. Improving health through policies that promote active travel: a review of evidence to support integrated health impact assessment. Environ Int. 2011;37:766-77.
- Ostergaard L, Børrestad LA, Tarp J, Andersen LB. Bicycling to school improves the cardiometabolic risk factor profile: a randomised controlled trial. BMJ Open. 2012;2.pii:e001307.
- Østergaard L, Grøntved A, Børrestad LA, Froberg K, Gravesen M, Andersen LB. Cycling to school is associated with lower BMI and lower odds of being overweight or obese in a large population-based study of danish adolescents. J Phys Act Health. 2012;9:617-25.
- Villa-González E, Ruiz JR, Ward DS, Chillón P. Effectiveness of an active commuting school-based intervention at 6-month follow-up. Eur J Public Health. 2016;26:272-6.
- Lu W, McKyer EL, Lee C, Ory MG, Goodson P, Wang S. Children’s active commuting to school: an interplay of self-efficacy, social economic disadvantage, and environmental characteristics. Int J Behav Nutr Phys Act. 2015;12:29.
- Lubans DR, Boreham CA, Kelly P, Foster CE. The relationship between active travel to school and health-related fitness in children and adolescents: a systematic review. Int J Behav Nutr Phys Act. 2011;8:5.
- Andersen LB, Lawlor DA, Cooper AR, Froberg K, Anderssen SA. Physical fitness in relation to transport to school in adolescents: the Danish youth and sports study. Scand J Med Sci Sports. 2009;19:406-11.
- Janssen I, Leblanc AG. Systematic review of the health benefits of physical activity and fitness in school-aged children and youth. Int J Behav Nutr Phys Act. 2010;7:40.
- Embree TE, Romanow NT, Djerboua MS, Morgunov NJ, Bourdeaux JJ, Hagel BE. Risk factors for bicycling injuries in children and adolescents: a systematic review. Pediatrics. 2016;138.pii:e20160282.
- Johan de Hartog J, Boogaard H, Nijland H, Hoek G. Do the health benefits of cycling outweigh the risks? Environ Health Perspect. 2010;118:1109-16.
- Sánchez Ruiz-Cabello, FJ. Prevención en la actividad física y el deporte. Recomendación. En: PrevInfad/PAPPS [en línea] [actualizado el 04/08/2007; consultado el 27/02/2018]. Disponible en http://previnfad.aepap.org/recomendacion/deporte-rec
- Rasmussen MG, Grøntved A, Blond K, Overvad K, Tjønneland A, Jensen MK, et al. Associations between recreational and commuter cycling, changes in cycling, and type 2 diabetes risk: a cohort study of Danish men and women. PLoS Med. 2016;13:e1002076.
- Oja P, Titze S, Bauman A, de Geus B, Krenn P, Reger-Nash B, et al. Health benefits of cycling: a systematic review. Scand J Med Sci Sports. 2011;21:496-509.
- Dudas RA, Crocetti M. Association of bicycling and childhood overweight status. Ambul Pediatr. 2008;8:392-5.
- Yang L, Sahlqvist S, McMinn A, Griffin SJ, Ogilvie D. Interventions to promote cycling: systematic review. BMJ. 2010;341:c5293.
- Consejo de Europa. Comité para el desarrollo del Deporte. EUROFIT. Test Europeo de Aptitud Física. MEC. Madrid: CSD; 1992.
- Antropometría. En: Web PEDiatrica [en línea] [consultado el 27/02/2018]. Disponible en www.webpediatrica.com/endocrinoped/antropometria.php
- Rodríguez-Fernández A, Axpe I, Goñi A. Propiedades psicométricas de una versión abreviada del Cuestionario de Autoconcepto Físico (CAF). Actas Esp Psiquiatr. 2015;43:125-32.
- Serra Majem L, Aranceta Bartrina J, Rivas Barba L, Sangil Monroy M, Pérez Rodrigo C. Crecimiento y desarrollo: dimensión alimentaria y nutricional. En: Serra Majem L, Aranceta Bartrina J, Rivas Barba L (eds.) Crecimiento y desarrollo. Estudio en Kid-Kreceplus. Barcelona: Masson; 2003. p. 45-55.
- Implementación Local de la Estrategia de Promoción de la Salud y Prevención en el SNS. En: Ministerio de Sanidad, Servicios Sociales e Igualdad [en línea] [consultado el 27/02/2018]. Disponible en www.msssi.gob.es/profesionales/saludPublica/prevPromocion/Estrategia/Implementacion_Local.htm
- Montil M, Barriopedro MI, Oliván J. El sedentarismo en la infancia. Los niveles de actividad física en niños/as de la comunidad autónoma de Madrid. Educación Física y Deportes. 2005;82:5-11.
- Ruiz JR, Rizzo NS, Hurtig-Wennlöf A, Ortega FB, Wärnberg J, Sjöström M. Relations of total physical activity and intensity to fitness and fatness in children: the European Youth Heart Study. Am J Clin Nutr. 2006;84:299-303.
- Wafa SW, Aziz NN, Shahril MR, Halib H, Rahim M, Janssen X. Measuring the daily activity of lying down, sitting, standing and stepping of obese children using the ActivPALTM activity monitor. J Trop Pediatr. 2017;63:98-103.
- Martínez Vizcaíno V, Salcedo Aguilar F, Franquelo Gutiérrez R, Solera Martínez M, Sánchez López M, Serrano Martínez S, et al. Assessment of an after-school physical activity program to prevent obesity among 9- to 10-year-old children: a cluster randomized trial. Int J Obes (Lond). 2008;32:12-22.
- Casabona Monterde C. Sobrepeso y obesidad infantil: no tiramos la toalla. En: AEPap (ed.). Curso de Actualización Pediatría 2017. Madrid: Lúa Ediciones 3.0; 2017. p. 39-52.




