Vol. 18 - Num. 70
Originales
Enfermedad celíaca: ¿qué características tienen nuestros pacientes en el momento del diagnóstico?
JM Martínez de Zabarte Fernándeza, Ruth García Romero, Ignacio Ros Arnalc, Mónica López Camposd, Eduardo Ubalde Sainze
aMIR-Pediatría. Hospital Universitario Miguel Servet. Zaragoza. España.
cHospital Universitario Miguel Servet. Zaragoza. España.
dHospital Universitario Miguel Servet. CS Sagasta-Ruiseñores. Zaragoza. España.
eZaragoza. España.
Cómo citar este artículo: Martínez de Zabarte Fernández JM, García Romero R, Ros Arnal I, López Campos M, Ubalde Sainz E. Enfermedad celíaca: ¿qué características tienen nuestros pacientes en el momento del diagnóstico? Rev Pediatr Aten Primaria. 2016;70:141-9.
Publicado en Internet: 14-06-2016 - Número de visitas: 22849
Resumen
Introducción: la enfermedad celíaca es una patología crónica que con frecuencia presenta los primeros síntomas en la edad pediátrica. En los últimos años ha aumentado el número de diagnósticos, a la vez que se ha reducido la edad a la que se realizan estos.
Material y métodos: estudio descriptivo de los antecedentes y las características epidemiológicas, clínicas y diagnósticas de 102 pacientes controlados por enfermedad celíaca en un hospital de tercer nivel.
Resultados: el 41,4% son varones y el 58,6% mujeres, la mayor parte de etnia caucásica (94,1%). El 9,8% tienen al menos un familiar de primer grado celíaco, y el 6,9% de segundo grado. La edad media al diagnóstico es 42,8 ± 35,9 meses. El 89,2% presentaban algún síntoma al diagnóstico, mientras en el 10,8% restante el diagnóstico se obtuvo en el cribado de celiaquía por presentar otra patología asociada. Síntomas más frecuentes: pérdida de peso (58%), diarrea (52%), hiporexia (40%), distensión abdominal (24%), alteración del carácter (15%), hábito malabsortivo (13%) y dolor abdominal (12%). Estudio serológico: el 95% presentó anticuerpos antitransglutaminasa positivos, el 85,2% antiendomisio positivos, el 88,4% antigliadina IgG positivos. Estudio del sistema de antígenos leucocitarios humanos (HLA): 97% DQ2, 2% DQ8. Se realizó biopsia duodenal al 62,8% (3% Marsh I, 5% Marsh II, 17% Marsh IIa, 17% Marsh IIIb, 58% Marsh IIIc).
Conclusiones: el mayor conocimiento de la enfermedad celíaca podría haber influido en la baja edad media al diagnóstico en la muestra. La aplicación de los criterios diagnósticos de la ESPGHAN de 2012 ha permitido diagnosticar a un relevante número de pacientes sin realizar biopsia.
Palabras clave
● Dieta sin gluten ● Enfermedad celíaca ● Enteropatía por glutenINTRODUCCIÓN Y OBJETIVOS
La enfermedad celíaca es una patología crónica de tipo autoinmune inducida por la ingesta de gluten, un conjunto de proteínas contenidas en la harina de los cereales de secano, fundamentalmente el trigo, pero también la cebada, el centeno y la avena.
Se desarrolla en personas que son genéticamente susceptibles con haplotipos HLA DQ-2 y/o DQ-8 y mediante la creación de unos anticuerpos específicos, que producen una enteropatía que afecta directamente al intestino delgado produciendo un aplanamiento de las vellosidades. Esto genera una disminución de la capacidad de absorción de los nutrientes de la alimentación.
En los últimos años la incidencia de esta patología ha aumentado, quizá influida por una mayor detección de la enfermedad por parte de los profesionales, lo que ha situado la prevalencia de la enfermedad en los países europeos por encima del 1%1.
La presentación clínica clásica del paciente celíaco consiste en diarrea crónica, estancamiento ponderal con hábito malabsortivo, dolor abdominal y distensión abdominal2. Sin embargo, la mayor parte de los pacientes ofrecen signos guía mucho más inespecíficos, como podrían ser alteración del carácter, ferropenia, estreñimiento, hipertransaminasemia, etc. Incluso en muchas ocasiones la enfermedad celíaca se diagnostica siendo clínicamente silente. Algunos trabajos sugieren que el diagnóstico de la enfermedad celíaca en edades precoces, y cuando se encuentra en fase silente o cuando aún presenta síntomas muy leves o indeterminados, indica un buen funcionamiento de los recursos de detección precoz3.
El objetivo principal de este estudio consiste en estudiar las características que tienen los pacientes pediátricos diagnosticados de enfermedad celíaca en un hospital de tercer nivel tras ser remitidos desde Atención Primaria, para conocer las formas de presentación de esta enfermedad en la actualidad, para permitir así optimizar el diagnóstico ya que se estima que por cada paciente diagnosticado de celiaquía podrían existir hasta 5-10 que no son diagnosticados2.
MATERIAL Y MÉTODOS
Estudio observacional, descriptivo, transversal y retrospectivo. Se ha recogido un grupo de 102 pacientes diagnosticados de enfermedad celíaca de una consulta especializada en Gastroenterología y Nutrición pediátrica en un hospital de tercer nivel que acudieron a las consultas para el control de su enfermedad.
Los datos estudiados corresponden a los antecedentes personales y familiares de los pacientes, las manifestaciones clínicas de la enfermedad, la presencia de otras patologías asociadas, los resultados de las serologías de estudio de marcadores de enfermedad celíaca, el estudio genético de HLA, la realización de biopsias y su resultado anatomopatológico.
En cuanto a los marcadores serológicos, son considerados positivos en el laboratorio de nuestro hospital títulos de anticuerpos antitransglutaminasa IgA (Ac anti-TG) mayores de 7 U/ml, anticuerpos antiendomisio (Ac anti-E) con resultado positivo, y anticuerpos antigliadina IgG (Ac anti-DPGG) mayores de 7 U/ml.
El estudio anatomopatológico se ha realizado en aquellos casos en los que han sido necesario para confirmar el diagnóstico conforme a los criterios de la Sociedad Europea de Gastroenterología, Hepatología y Nutrición Pediátrica (ESPGHAN por sus siglas en inglés) de 20124, mediante la obtención de muestras de primera y segunda porciones duodenales y estudio anatomopatológico de las mismas estadificándose según la clasificación de Marsh5. A todos los pacientes cuyo diagnóstico fue anterior a los criterios ESPGHAN del 2012 se les realizó biopsia intestinal.
RESULTADOS
La muestra se compone de 102 pacientes, con un total de 47 varones (41,4%) y 65 mujeres (58,6%).
En el 94,1% de los casos la ascendencia de los pacientes es española o europea. En seis pacientes los padres pertenecen a otras etnias, siendo dos magrebíes, dos subsaharianos y dos latinoamericanos.
La vía de parto más frecuente es la vaginal, con 90 pacientes (88,2%) frente a los 12 pacientes nacidos mediante cesárea (11,8%). El número de pacientes alimentados con lactancia materna fue de 61 (59,8%), con una duración media de 6,3 ± 4,6 meses. Recibieron lactancia artificial 30 niños (29,4%) y en 11 casos (10,8%) no se dispone de los datos correspondientes al tipo de lactancia.
La edad media de introducción del gluten son 6,3 ± 0,6 meses. Únicamente en 23 casos (22,6%) la introducción del gluten coincidió con lactancia materna mantenida en ese momento.
No existen familiares celíacos en 85 de los pacientes (83,3%), mientras que en diez casos (9,8%) existen familiares de primer grado afectos, y de segundo grado en otros siete (6,9%).
La edad media al diagnóstico es 42,8 ± 35,9 meses. Un total de 49 pacientes (48%) han sido diagnosticados antes de los 24 meses de edad, 33 pacientes (32,4%) entre los 24-72 meses de vida y 20 pacientes (19,6%) con más de 72 meses.
En 91 pacientes (89,2%) existían síntomas compatibles con enfermedad celíaca en el momento del diagnóstico, en la Fig. 1 se muestran los síntomas más frecuentes al diagnóstico. En la Fig. 2 se describen los síntomas más frecuentes en los diferentes grupos de edad.
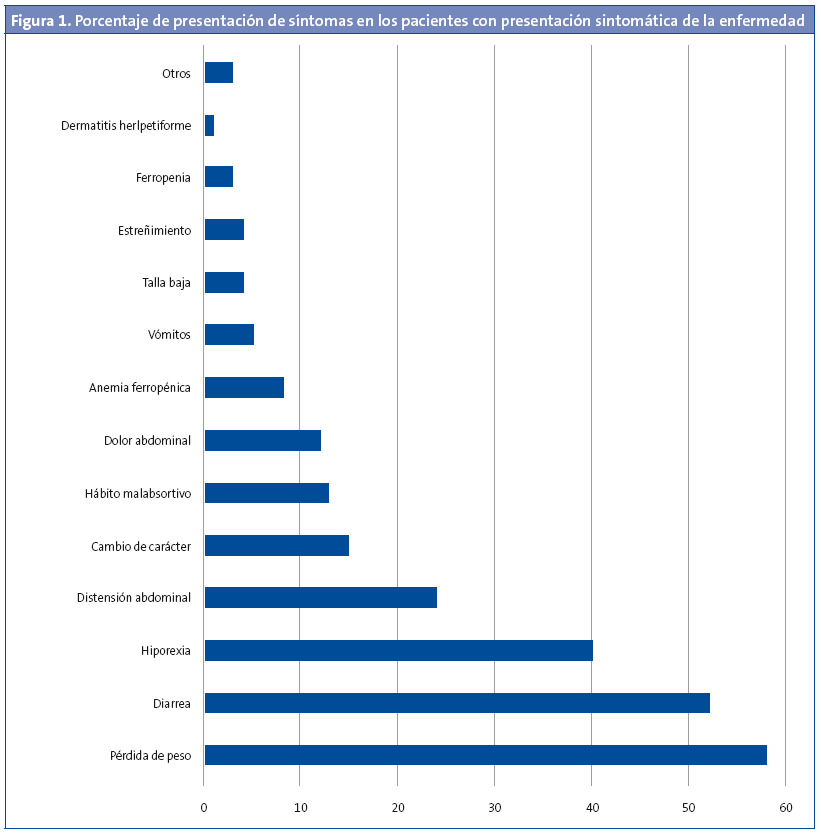

En 11 pacientes (10,8%) la presentación fue silente y el diagnóstico de celiaquía se realizó en contexto de estudio por presentar otra patología, destacando: dos pacientes con diabetes mellitus tipo 1, dos pacientes estudiados por presentar un familiar de primer grado celíaco, y un paciente con síndrome de Down.
En tres de los niños (2,7%) se diagnosticó déficit de IgA, en cuatro (3,6%) existía algún tipo de patología tiroidea, asociaban diabetes mellitus tipo 1 en dos ocasiones (2%) y dos de ellos tenían síndrome de Down (2%).
Todos los pacientes de la muestra, a excepción de uno, que presentaba biopsia compatible con enfermedad celíaca (1%), presentaban positividad de alguno de los marcadores serológicos de celiaquía. En la Tabla 1 se muestra la frecuencia con la que se han hallado los diferentes marcadores de enfermedad celíaca en nuestro estudio.

El estudio genético del HLA se realizó a 100 pacientes (98%), encontrándose 97 pacientes DQ2 (97%), dos pacientes DQ8 (2%), un paciente DQ2/DQ8 (1%).
Se realizó una biopsia duodenal en 64 de los casos (62,8%) para confirmar el diagnóstico. En la Fig. 3 se describen los hallazgos anatomopatológicos obtenidos en la biopsia.
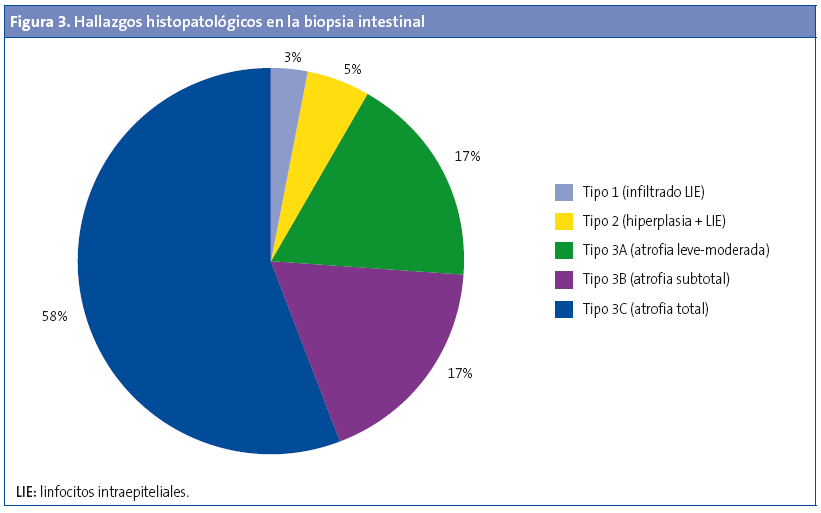
En todos los pacientes se ha establecido una dieta estrictamente exenta de gluten como tratamiento y se realizan controles de seguimiento con colaboración del especialista en gastroenterología pediátrica y el pediatra de Atención Primaria.
DISCUSIÓN
La relación de mujeres/hombres es 1,4:1. En algunos trabajos descriptivos esta relación alcanza el 2:1 a favor de las mujeres; al parecer esto podría deberse a una mayor presencia de los haplotipos HLA DQ2 y DQ8 en el sexo femenino6.
La prevalencia de enfermedad celíaca en los familiares de los pacientes de nuestro estudio se corresponde con los datos de otros estudios, donde se citan cifras de 4-12% en familiares de primer y segundo grado7.
Es reseñable la edad al diagnóstico de nuestros pacientes, ya que en casi la mitad se establece el diagnóstico antes de los dos años de vida, y en el 80% antes de los seis años de vida. Este dato contrasta con otras publicaciones en las que hasta un 90% de los diagnósticos se establecen a partir de los seis años de edad3,8.
Con frecuencia, la sospecha diagnóstica se establece por las manifestaciones clínicas en el paciente. En nuestra muestra la diarrea está presente en aproximadamente la mitad de los pacientes al diagnóstico, tal y como se describe en otros estudios9. Sin embargo en otros trabajos la presencia de diarrea alcanza el 82,1%6, posiblemente debido a que el diagnóstico se realizaba más tardíamente.
En ocasiones la enfermedad celíaca puede producir manifestaciones extraintestinales, como cefalea, dermatitis herpetiforme, tetania, miopatía, osteoporosis, hiperparatiroidismo, amenorrea, atrofia esplénica y alteraciones neuropsiquiátricas10. En nuestros pacientes el síntoma extraintestinal más frecuente son las alteraciones del comportamiento, seguidas de anemia ferropénica, ferropenia y dermatitis.
Hay que tener presente que la mayor parte de los pacientes diagnosticados de celiaquía podrían presentarse de forma silente o con síntomas que no son los que clásicamente se han asociado a la enfermedad, especialmente en los momentos iniciales11. En los pacientes con sospecha de enfermedad celíaca silente, el hallazgo de marcadores elevados suele realizarse en contexto de estudio por antecedentes familiares o porque presenta otra patología que asocia un mayor riesgo de desarrollar celiaquía: diabetes mellitus tipo 1, patología tiroidea autoinmune, hepatitis autoinmune, déficit selectivo de IgA, síndrome de Down, síndrome de Williams y síndrome de Turner2,4.
Ante la sospecha de celiaquía debe realizarse un estudio serológico mediante los anticuerpos Ac anti-TG, Ac anti-E y antigliadina. Para reforzar la sospecha diagnóstica, a la positividad de estos anticuerpos debe sumarse un fenotipo HLA compatible (DQ2, DQ8).
Pese a que la prevalencia de celiaquía en la población es importante y que se considera una entidad infradiagnosticada, en múltiples trabajos en los que se ha estudiado la posibilidad de realizar despistaje poblacional de celiaquía mediante pruebas serológicas no se ha llegado a establecer esta táctica como adecuada12,13.
En 2012 la ESPGHAN estableció unos criterios que permiten diagnosticar enfermedad celíaca en un paciente sin necesidad de comprobar la alteración histopatológica en biopsias duodenales, siempre y cuando se cumplan los siguientes requisitos: paciente con síntomas típicos de enfermedad celíaca, con haplotipo DQ2/DQ8 de riesgo, valores de Ac anti-TG elevados más de diez veces por encima del valor de corte del laboratorio y Ac anti-E positivos4. Estos criterios han permitido diagnosticar a más de un tercio de los pacientes de nuestra consulta sin necesidad de realizar estudio histopatológico. Un estudio de 2015 realizado para valorar el protocolo de la ESPGHAN de 2012 encontró como resultado que el 98,2% de los pacientes que cumplían los criterios para diagnóstico de enfermedad celíaca se hubieran diagnosticado adecuadamente sin necesidad de realizar biopsia, y con esto se hubieran disminuido casi un 50% las endoscopias realizadas de forma anual. No obstante, en este mismo trabajo se publican cuatro casos de pacientes que cumplen los criterios diagnósticos sin presentar signos compatibles con celiaquía en la biopsia duodenal. En el seguimiento, dos de ellos presentan una evolución favorable con mejoría de los títulos de anticuerpos anti-TG y en los otros dos se repitió la biopsia a los dos años, con diagnóstico de celiaquía en uno de ellos14.
La prueba que permite confirmar el diagnóstico en los pacientes que no cumplan los criterios de la ESPGHAN y es gold standard en el diagnóstico de la enfermedad celíaca es la endoscopia digestiva alta4, para la obtención de biopsias de primera y segunda o tercera porciones duodenales; es importante tomar muestras de diferentes zonas en duodeno ya que la afectación puede ser parcheada14. Sobre estas muestras se realiza el estudio anatomopatológico que clasifica la afectación vellositaria según la clasificación de Marsh, de forma que los grados 2-3 de atrofia permiten establecer el diagnóstico definitivo5.
Es importante confirmar el diagnóstico en aquellos pacientes que no cumplan estos criterios ya que algunos de estos pacientes con positividad de los marcadores de enfermedad celíaca podrían presentar un estado normal de sus vellosidades intestinales sin poder establecerse el diagnóstico en ese momento15,16. Incluso se ha sugerido en algunos estudios la posibilidad de que los marcadores de enfermedad celíaca pudieran elevarse de forma transitoria en relación con el desarrollo de enfermedades autoinmunitarias, enfermedad inflamatoria intestinal, hepatopatías, infecciones virales y otros procesos patológicos que afecten a la mucosa intestinal en ese momento, con posterior normalización14,17, si bien es cierto que en estos pacientes con marcadores elevados debe realizarse un estrecho seguimiento, ya que podría tratarse de una fase latente de la enfermedad4.
El diagnóstico precoz de la enfermedad celíaca, donde juega un papel fundamental el pediatra de Atención Primaria, es muy importante ya que reduce la probabilidad de que estos pacientes desarrollen las múltiples complicaciones derivadas de esta patología.
El tratamiento de la celiaquía se basa en seguir una dieta completamente exenta de gluten4. Tras el inicio de la dieta, un 70% de los pacientes sintomáticos refieren mejoría de la clínica a las dos semanas18. Esta mejoría cínica no está presente en los pacientes diagnosticados en una fase silente o con manifestaciones mínimas de la enfermedad, y esto podría justificar que realicen un peor seguimiento de la dieta y transgresiones con mayor frecuencia19.
Además de la mejoría clínica, un adecuado seguimiento de la dieta permite limitar la aparición de las posibles complicaciones derivadas de un mal control de la enfermedad: carencias nutricionales por malabsorción de nutrientes (ferropenia, osteoporosis), mayor riesgo de desarrollar otras enfermedades autoinmunes (tiroiditis autoinmune, diabetes mellitus tipo 1, hepatitis autoinmune), duodenoyeyunitis erosiva e incluso el desarrollo de neoplasias como el linfoma de células T y adenocarcinoma de intestino delgado4,20.
Para el seguimiento y control de los pacientes diagnosticados de enfermedad celíaca se monitorizan los niveles de Ac anti-TG (salvo en pacientes con déficit selectivo de IgA, en los que se emplearán los Ac anti-DPGG) que deberían negativizarse a los pocos meses de iniciar una dieta completamente exenta de gluten. Estos controles se realizan con mayor frecuencia tras el diagnóstico, y una vez se han negativizado y estabilizado estos marcadores, es importante mantener al menos un control anual o bianual para corroborar el adecuado cumplimiento de la dieta y controlar la posible aparición de otras patologías autoinmunes asociadas y alteraciones derivadas de una malabsorción de nutrientes como las citadas anteriormente4.
En nuestro estudio destaca la baja edad al diagnóstico de nuestros pacientes: esto se debe probablemente al buen funcionamiento del primer nivel de entrada al sistema sanitario en nuestro entorno, que es la Atención Primaria, y al corto espacio de tiempo transcurrido desde el establecimiento de la sospecha diagnóstica y el diagnóstico de celiaquía. Es destacable también el número de nuestros pacientes que son diagnosticados sin necesidad de realizar estudio endoscópico, mediante la aplicación de los criterios ESPGHAN 2012. Creemos que es importante recalcar la importancia de mantener un adecuado nivel de conocimiento y alerta en los profesionales sanitarios acerca de la celiaquía, para así lograr un adecuado y precoz diagnóstico, tratamiento y seguimiento de los pacientes celíacos en nuestro medio.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS: Ac anti-DPGG: anticuerpos antigliadina IgG · Ac anti-E: anticuerpos antiendomisio · Ac anti-TG: anticuerpos antitransglutaminasa IgA · ESPGHAN: Sociedad Europea de Gastroenterología, Hepatología y Nutrición Pediátrica · HLA: sistema de antígenos leucocitarios humanos.
BIBLIOGRAFÍA
- Greco L, Timpone L, Abkari A, Abu-Zekry M, Attard T, Bouguerrà F, et al. Burden of celiac disease in the Mediterranean area. World J Gastroenterol. 2011;17:4971-8.
- Marugán de Miguelsanz JM. Diagnóstico clínico y cribado de la enfermedad celíaca. Rev Pediatr Aten primaria. 2008;10(Supl 2):s29-s38.
- Mora M, Litwin N, Toca C, Azcona MI, Neffa RS, Ortiz G, et al. Prevalencia de enfermedad celíaca: estudio multicéntrico en población pediátrica en cinco distritos urbanos de Argentina. Rev Argent Salud Pública. 2010;1:26-31.
- Husby S, Koletzko S, Korponay-Szabo IR, Mearin ML, Phillips A, Shamir E, et al. European Society for Pediatric Gastroenterology, Hepatology, and Nutrition guidelines for the diagnosis of coeliac disease. J Pediatr Gastroenterol Nutr. 2012;54:136-60.
- Rubio-Tapia A, Hill ID, Kelly CP, Calderwood AH, Murray JA. ACG clinical guidelines: diagnosis and management of celiac disease. Am J Gastroenterol. 2013;108:656-76.
- Llanos O, Matzumura M, Tagle M, Huerta-Mercado J, Cedrón H, Scavino J, et al. Celiac disease: descriptive study at the anglo american clinic. Rev Gastroenterol Perú. 2012;32:134-40.
- Rodrigo L, Riestra S, Fuentes D, González S, López-Vázquez A, López-Larrea C. Diverse clinical presentations of celiac disease in the same family. Rev Esp Enferm Dig. 2004;96:612-6;416-9.
- Castaño L, Blarduni E, Ortiz L, Núñez J, Bilbao JR, Rica I, et al. Prospective population screening for celiac disease: high prevalence in the first 3 years of life. J Pediatr Gastroenterol Nutr. 2004;39:80-4.
- Rodrigo L, Fuentes D, Riestra S, Nico P, Álvarez N, López Vázquez A, et al. Prevalencia aumentada de enfermedad celíaca en familiares de primer y segundo grado:descripción de una familia con 19 miembros estudiados. Rev Esp Enferm Dig. 2007;99:149-55.
- James MW, Scott BB. Coeliac disease: the cause of the various associated disorders? Eur J Gastroenterol Hepatol. 2001;13:1119-21.
- Fernández A, González L, de-la-Fuente J. Coeliac disease: clinical features in adult populations. Rev Esp Enferm Dig. 2010;102:466-71.
- Collin P. Should adults be screened for celiac disease? What are the benefits and harms of screening? Gastroenterology. 2005;128:S104-8.
- Dorn SD, Matchar DB. Cost-effectiveness analysis of strategies for diagnosing celiac disease. Dig Dis Sci. 2008;53:680-8.
- Gidrewicz D, Potter K, Trevenen CL, Lyon M, Butzner JD. Evaluation of the ESPGHAN celiac guidelines in a North American pediatric population. Am J Gastroenterol. 2015;110:760-7.
- Cueto Rua E, Guzmán L, Nanfito G, Barrera S, Drut R. Celiaquía, una enfermedad paradigmática. Arch Argent Pediatr. 2008;106:143-54.
- Dickey W, Hughes DF, McMillan SA. Patients with serum IgA endomysial antibodies and intact duodenal villi: clinical characteristics and management options. Scand J Gastroenterol. 2005;40:1240-3.
- Bizzaro N, Villalta D, Tonutti E, Doria A, Tampoia M, Bassetti D, et al. IgA and IgG tissue transglutaminase antibody prevalence and clinical significance in connective tissue diseases, inflammatory bowel disease, and primary biliary cirrhosis. Dig Dis Sci. 2003;48:2360-5.
- Pink IJ, Creamer B. Response to a gluten-free diet of patients with the coeliac syndrome. Lancet. 1967;1:300-4.
- Fasano A. European and North American populations should be screened for coeliac disease. Gut. 2003;52:168-9.
- Vera A, Frisancho O, Yábar A, Carrasco W. Enfermedad celíaca y obstrucción intestinal por linfoma de células T. Rev Gastroenterol Peru. 2011;31:278-81.




