Posicionamiento del Comité Español Interdisciplinario de Prevención Cardiovascular y la Sociedad Española de Cardiología en el tratamiento de las dislipemias. Divergencia entre las guías europea y estadounidense
José María Lobos Bejaranoa, Enrique Galveb, Miguel Ángel Royo Bordonadac, Eduardo Alegría Ezquerrad, Pedro Armarioe, Carlos Brotonsf, Miguel Camafortg, Alberto Cordero Fortb, Antonio Maiques Galánh, Teresa Mantilla Moratóh, Antonio Pérez Pérezi, Juan Pedro Botetj, (CEIPC) en nombre del Comité Español Interdisciplinario para la Prevención Cardiovasculark
aSociedad Española de Medicina de Familia y Comunitaria.
bSección de Riesgo Vascular y Rehabilitación Cardiaca, Sociedad Española de Cardiología. Madrid. España.
cInstituto de Salud Carlos III. Madrid. España.
dSección de Riesgo Vascular y Rehabilitación Cardiaca. Sociedad Española de Cardiología. Madrid. España.
eSociedad Española-Liga Española para la Lucha contra la Hipertensión Arterial .
fSociedad Española de Medicina Familiar y Comunitaria (SemFYC) .
gSociedad Española de Medicina Interna.
hSociedad Española de Medicina de Familia y Comunitaria. Madrid. España.
iSociedad Española de Diabetes . Madrid. España.
jSociedad Española de Arteriosclerosis .
kComité Español Interdisciplinario para la Prevención Cardiovascular.
Cómo citar este artículo: Lobos Bejarano JM, Galve E, Royo Bordonada MA, Alegría Ezquerra E, Armario P, Brotons C, et al. Posicionamiento del Comité Español Interdisciplinario de Prevención Cardiovascular y la Sociedad Española de Cardiología en el tratamiento de las dislipemias. Divergencia entre las guías europea y estadounidense. Rev Pediatr Aten Primaria. 2014;16:e161-e172.
Publicado en Internet: 29-10-2014 - Número de visitas: 27995
Resumen
La publicación en EE. UU. de la guía de 2013 de American College of Cardiology/American Heart Association para el tratamiento del colesterol elevado ha tenido gran impacto por el cambio de paradigma que supone. El Comité Español Interdisciplinario de Prevención Cardiovascular y la Sociedad Española de Cardiología han revisado esa guía, en comparación con la vigente guía europea de prevención cardiovascular y de dislipemias.
El aspecto más destacable de la guía estadounidense es el abandono de los objetivos de colesterol unido a lipoproteínas de baja densidad, de modo que proponen el tratamiento con estatinas en cuatro grupos de riesgo aumentado. En pacientes con enfermedad cardiovascular establecida, ambas guías conducen a una estrategia terapéutica similar (estatinas potentes, dosis altas). Sin embargo, en prevención primaria, la aplicación de la guía estadounidense supondría tratar con estatinas a un número de personas excesivo, particularmente de edades avanzadas. Abandonar la estrategia según objetivos de colesterol, fuertemente arraigada en la comunidad científica, podría tener un impacto negativo en la práctica clínica y crear cierta confusión e inseguridad entre los profesionales y quizá menos seguimiento y adherencia de los pacientes. Por todo ello, el presente documento reafirma las recomendaciones de la guía europea. Ambas guías tienen aspectos positivos pero, en general y mientras no se resuelvan las dudas planteadas, la guía europea, además de utilizar tablas basadas en la población autóctona, ofrece mensajes más apropiados para el entorno español y previene del posible riesgo de sobretratamiento con estatinas en prevención primaria.
Palabras clave
● Dislipemias ● Guías clínicas ● Prevención cardiovascularNota:
Artículo publicado simultáneamente en: Angiología, Clínica e Investigación en Arteriosclerosis, Enfermería Familiar y Comunitaria, Hipertensión y Riesgo Vascular, Revista Española de Cardiología, Revista Española de Salud Pública, Revista Pediatría de Atención Primaria y Semergen. Artículo publicado previamente en Rev Esp Cardiol. 2014. Disponible en http://dx.doi.org/10.1016/j.recesp.2014.05.008. Reproducido con permiso de los autores y del editor
INTRODUCCIÓN
La hipercolesterolemia afecta a una de cada dos personas adultas en España1 y es uno de los principales factores del riesgo de enfermedad vascular arteriosclerótica. Sus complicaciones aterotrombóticas mayores generan gran morbilidad y son la primera causa de muerte en el mundo2. Por lo tanto, la prevención y el tratamiento de la hipercolesterolemia en el contexto del manejo del riesgo cardiovascular total es un aspecto crucial para los médicos y otros profesionales de la salud, de modo que diversas entidades científicas elaboran guías de práctica clínica, en las que se analiza y se resume la evidencia científica disponible y se emiten recomendaciones y directrices de actuación acordes con ellas. Las guías europeas para el manejo de la dislipemia y la prevención cardiovascular, publicadas respectivamente en 2011 y 2012 por un comité conjunto de la European Society of Cardiology/European Atherosclerosis Society (ESC/EAS)3,4, han tenido buena acogida en España, con diversas iniciativas para fomentar su aplicación5,6. A finales de 2013, se publicó la guía de American College of Cardiology/American Heart Association (ACC/AHA)7, que inmediatamente ha generado polémica a ambos lados del Atlántico. Aunque las guías europeas y estadounidense coinciden en muchos aspectos, hay otros puntos importantes en los que difieren, como el cambio drástico en el enfoque para la aplicación inicial del tratamiento con hipolipemiantes y en los objetivos terapéuticos, hecho que ha causado cierta confusión e inseguridad en muchos profesionales, que se cuestionan cuál es el enfoque más apropiado a seguir. En respuesta a esta controversia, se presenta este documento, elaborado por un grupo de médicos de diferentes especialidades y ámbitos de trabajo, a iniciativa del Comité Español Interdisciplinario de Prevención Cardiovascular (Anexo 1) y la Sociedad Española de Cardiología.
COMENTARIO A LA METODOLOGÍA DE AMBAS GUÍAS
El sistema de gradación de la evidencia y el formato de las recomendaciones es similar en las guías europea y estadounidense. Ambas utilizan el sistema COR/LOE (class of recommendation/level of evidence); la ESC/EAS lo combina con el sistema GRADE (grading of recommendations assessment, development, and evaluation)3,4, y la recomendación puede ser fuerte o débil, y ACC/AHA aplica una gradación propia del National Heart and Blood Institute, que va desde la clase A (recomendación fuerte) a la clase E (opinión de expertos)7.
Mientras que la guía europea presenta un amplio compendio de información clínica que abarca todo el espectro de la prevención cardiovascular, la estadounidense revisa sucintamente los aspectos que los expertos han considerado críticos. Así, la guía europea trata el proceso de detección, manejo y tratamiento del paciente con dislipemia de manera integral, abordando el cálculo del riesgo cardiovascular, la evaluación de los parámetros de laboratorio, los objetivos terapéuticos, las modificaciones de estilo de vida recomendadas, los fármacos que han mostrado su utilidad en el tratamiento de la dislipemia, como los valores bajos de colesterol unido a lipoproteínas de alta densidad y la hipertrigliceridemia, el tratamiento de las dislipemias en situaciones especiales, la monitorización en el paciente con tratamiento farmacológico y, finalmente, las medidas para mejorar la adherencia de estos pacientes al tratamiento. Frente a este planteamiento, la guía de ACC/AHA responde a cuestiones clínicas muy seleccionadas, identificadas como relevantes, relativas a la evidencia sobre el uso de objetivos terapéuticos y la eficacia y la seguridad de los fármacos hipolipemiantes, y de las estatinas en particular, en prevención cardiovascular.
Una limitación importante de la guía de ACC/AHA es que solo incluye datos provenientes de ensayos clínicos aleatorizados, basándose en las recomendaciones del Institute of Medicine8. Esto complica la generalización de sus resultados a la población general, ya que los participantes en los ensayos son habitualmente individuos de alto riesgo, por lo que, siendo estrictos, las recomendaciones de la guía estadounidense solo serían aplicables a sujetos de características similares. Además, los tratamientos farmacológicos son más susceptibles de evaluación mediante ensayos clínicos aleatorizados que las intervenciones dirigidas a modificar estilos de vida, por lo que la exclusión de otro tipo de evidencia, proveniente de estudios observacionales (cohortes y casos y controles), encuestas y registros, puede resultar en una guía que promueva un uso excesivo de medicamentos, en detrimento de la promoción de una alimentación saludable, la práctica de actividad física y el abandono del tabaquismo.
Las personas asintomáticas o con enfermedad subclínica perciben el riesgo de maneras distintas y la aceptación y la adherencia a largo plazo del tratamiento farmacológico resulta más complicada que en los pacientes que precisan atención médica tras presentar un evento cardiovascular agudo9. Además, el balance neto beneficio-riesgo del tratamiento con estatinas se va diluyendo cuanto menor es el riesgo cardiovascular10. Por lo tanto, en prevención primaria, la decisión de tratar con estatinas o no debería tomarse considerando las preferencias de las personas susceptibles de intervención, tras valorar seriamente las medidas no farmacológicas (dieta, actividad física y cese del tabaquismo) y discutir en profundidad con el paciente el balance entre los posibles beneficios y riesgos de la intervención. Sin embargo, la guía estadounidense, pese a su pretendido enfoque centrado en el paciente, al que se haría partícipe de las decisiones, hace una recomendación firme de tratamiento con estatinas para personas con riesgo cardiovascular ≥7,5% (race- and sex-specific pooled cohort equations). Aunque no sean directamente comparables, esto equivaldría a un riesgo intermedio de la escala de Framingham tradicional. Por el contrario, la guía europea, para personas con riesgo moderado (SCORE [systematic coronary risk evaluation] >1% pero <5%), recomienda considerar el tratamiento farmacológico únicamente cuando con las demás medidas no se ha alcanzado el objetivo de control de colesterol unido a lipoproteínas de baja densidad (cLDL).
PUNTOS DE CONSENSO
Aunque habitualmente son más llamativas las discrepancias existentes, la guía europea y la nueva guía estadounidense tienen una serie de puntos en común (que son mayoría) que merece la pena resaltar:
- Ambas destacan la preponderancia del cLDL como factor de riesgo principal y la importancia de reducirlo para prevenir y tratar la enfermedad cardiovascular (ECV).
- Ambas enfatizan la importancia de la estratificación del riesgo en prevención cardiovascular y recomiendan la estimación del riesgo total de ECV, no solo el coronario, como elemento esencial en la decisión de iniciar tratamiento hipolipemiante.
- Ambas consideran que las modificaciones del estilo de vida constituyen la piedra angular en la promoción de la salud y la reducción del riesgo de ECV.
- Para individuos con riesgo moderado en los que el juicio clínico indica que puede estar subestimado, la guía europea resalta la importancia de la historia familiar de ECV prematura e indica la posibilidad de determinar la proteína C reactiva de alta sensibilidad, el fibrinógeno, la homocisteína, el índice tobillo-brazo, el grosor intimomedial carotídeo, el calcio intracoronario e incluso la prueba de esfuerzo. Aunque la guía estadounidense es más conservadora en lo concerniente a los posibles marcadores de riesgo/técnicas de imagen, coincide con la europea en incluir la historia familiar de ECV prematura, la proteína C reactiva de alta sensibilidad, el índice tobillo-brazo y el calcio intracoronario.
- Para los pacientes de muy alto riesgo, la guía europea incluye como opcional una reducción al 50% del valor basal si no se alcanza el objetivo terapéutico de cLDL <70 mg/dl (<1,8 mmol/l). La guía estadounidense recomienda utilizar directamente tratamiento con estatinas de alta intensidad, que reducen el cLDL por debajo del 50%.
- Para los pacientes con intolerancia a las estatinas, ambas guías recomiendan reducir la dosis, considerar combinaciones u otras alternativas.
- En prevención primaria y para pacientes con cLDL ≥190 mg/dl (>4,9 mmol/l), la guía estadounidense recomienda tratamiento con estatinas de alta intensidad o, si no se toleran, de intensidad moderada, solas o en combinación con terapias alternativas cuando no haya respuesta suficiente a la dosis máxima tolerada de estatina. La guía europea señala como objetivo concentraciones de cLDL <100 mg/dl y, si no se alcanza con la estatina, considera añadir un segundo fármaco.
- Para pacientes con diabetes mellitus y otros factores de riesgo o lesión de órgano diana, ambas guías recomiendan el tratamiento más intensivo (objetivo de cLDL <70 mg/dl [<1,8 mmol/l] para la de ESC/EAS y tratamiento de alta intensidad para la de ACC/AHA), mientras que para los pacientes con diabetes mellitus de riesgo bajo, ambas guías recomiendan un tratamiento menos intensivo (objetivo de cLDL <100 mg/dl [<2,5 mmol/l] para ESC/EAS y tratamiento de moderada intensidad para ACC/AHA).
- Por último, ambas guías recomiendan una actitud más conservadora en pacientes >75 años, si bien la estadounidense incluye explícitamente esta edad como determinante de la intensidad del tratamiento.
ASPECTOS DIFERENCIALES
Las funciones propuestas para la estimación del riesgo cardiovascular total en prevención primaria en una y otra guía presentan diferencias notables:
- La franja de edades es más amplia en la función estadounidense (35-64 años en SCORE y 35-79 años en race- and sex-specific pooled cohort equations).
- Los eventos cardiovasculares de interés en SCORE solo incluyen los episodios mortales (riesgo de un primer evento mortal cardiovascular aterosclerótico, incluidos todos los diagnósticos de la Clasificación Internacional de Enfermedades relacionados con la arteriosclerosis), mientras que en la función estadounidense se incluyen también los no mortales (riesgo de morbimortalidad cardiovascular, que incluye enfermedad coronaria, ictus y enfermedad arterial periférica). No obstante, la guía europea hace una aproximación al riesgo cardiovascular total incluyendo la morbilidad, con lo que el riesgo es aproximadamente tres veces superior al observado en las tablas, aunque este factor varía con la edad y el sexo.
- La guía estadounidense incluye la diabetes mellitus y el tratamiento de la hipertensión arterial entre las variables predictivas, además de las incluidas en la europea: edad, colesterol total y colesterol unido a lipoproteínas de alta densidad, presión arterial sistólica y tabaquismo.
- Para la evaluación y comunicación del riesgo de personas jóvenes, la guía europea propone el cálculo del riesgo relativo o la edad vascular, mientras que la estadounidense propone la estimación del riesgo cardiovascular a 30 años.
- Finalmente, la guía europea incluye en la evaluación del riesgo explícitamente los factores psicosociales, a los que se concede un apartado específico.
Las diferencias son más importantes en las recomendaciones del tratamiento de la hipercolesterolemia, especialmente en la definición de las categorías de riesgo y los objetivos terapéuticos (Tabla 1). La guía europea define cuatro categorías de riesgo y objetivos terapéuticos acordes con ellas, mientras que la estadounidense, en lugar de categorías de riesgo, establece cuatro grupos de pacientes para los que está indicado el tratamiento con estatinas y las dosis que se debería utilizar en cada caso. La estrategia de la guía estadounidense se basa en que los ensayos clínicos aleatorizados, para reducir la morbimortalidad cardiovascular, han utilizado dosis fijas de estatina (frente a placebo, frente a otra estatina y/u otras dosis), mientras que no se ha evaluado el uso de estatinas con dosis ajustada al cumplimiento de objetivos terapéuticos. Este razonamiento está alineado con el actual borrador de la guía británica del National Institute for Health and Care Excellence sobre la evaluación del riesgo cardiovascular y la modificación de los lípidos para la prevención cardiovascular11.
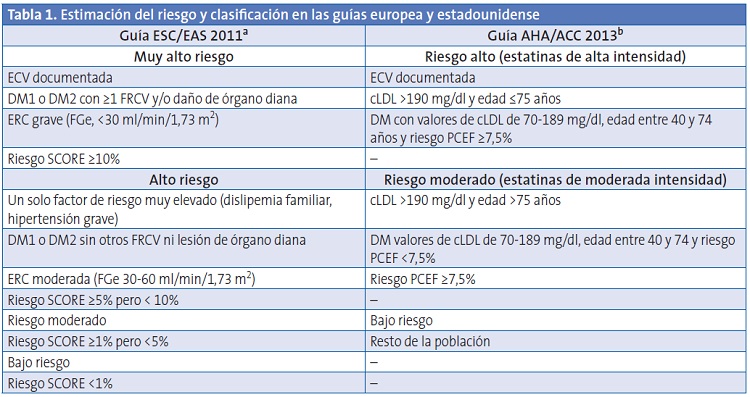
AHA/ACC: American Heart Association/American College of Cardiology; cLDL: colesterol unido a lipoproteínas de baja densidad; DM1: diabetes mellitus tipo 1; DM2: diabetes mellitus tipo 2; ECV: enfermedad cardiovascular; ERC: enfermedad renal crónica; ESC/EAS: European Society of Cardiology/European Atherosclerosis Society; FGe: filtrado glomerular estimado; FRCV: factores de riesgo cardiovascular; PCEF: pooled cohort equations function; SCORE: systematic coronary risk evaluation.
aClaramente definidos en la guía europea. bNiveles de riesgo basados en los cuatro grupos identificados de mayor beneficio documentado en ensayos clínicos con estatinas.
Por último, la guía estadounidense centra sus recomendaciones en la utilización de estatinas, y define tres niveles de tratamiento: intensidad alta, moderada y baja, según las diferentes estatinas y su dosificación. El uso de otros hipolipemiantes (fibratos, ácido nicotínico, resinas de intercambio iónico, inhibidores de la absorción de colesterol y ácidos grasos omega-3), sobre los que no hay evidencia que demuestre su eficacia en la disminución de eventos cardiovasculares como tratamiento aislado o asociado a estatina, se considera una opción solo para los individuos de riesgo alto con intolerancia definitiva a estatinas, tras reducción de dosis e incluso cambio de estatina. El fenofibrato se puede considerar junto con una estatina de intensidad baja o moderada solo si se estima que los beneficios de la reducción del riesgo cardiovascular, o de la disminución de triglicéridos cuando sean >500 mg/dl, superan el riesgo potencial de efectos adversos (clase IIb). Sin embargo, en la guía europea se incluyen estos grupos farmacológicos en tres situaciones clínicas: a) en caso de intolerancia a las estatinas: resinas de intercambio (clase IIa/B), ezetimiba sola o en combinación con resinas (clase IIb/C); b) si no se alcanzan los objetivos de control de cLDL con la máxima dosis tolerada de estatinas: estatina + ezetimiba o resinas de intercambio (clase IIb/C), y c) pacientes de alto riesgo con hipertrigliceridemia: fibratos (clase I/B) o combinación con fibratos (no gemfibrozilo) + estatina (clase IIa/C). Se destaca también la hipertrigliceridemia como causa de pancreatitis, incluso desde concentraciones de 450-900 mg/dl, y la importancia del tratamiento no farmacológico (reducción calórica, abstinencia de alcohol, control de la diabetes mellitus, etc.) y farmacológico (fibratos).
IMPLICACIONES PARA LA PRÁCTICA CLÍNICA
En prevención secundaria, la guía europea marca un objetivo terapéutico de cLDL <70 mg/dl o reducción ≥50% del cLDL, en tanto que la estrategia de la guía estadounidense se aparta claramente de los objetivos de control, lo que supone un drástico cambio de paradigma en la práctica clínica seguida durante años por los profesionales. Alcanzar cifras de cLDL <70 mg/dl en la mayoría de los pacientes requiere una estrategia de estatinas de «alta intensidad», como propone la guía estadounidense, por lo que, en la práctica, la diferencia entre ambas estrategias se reduce. Además, aunque se abandonen los objetivos lipídicos absolutos, de manera implícita se asume que el objetivo terapéutico es una reducción porcentual de cLDL determinada en cada uno de los grupos definidos. La ausencia de objetivos lipídicos en la guía estadounidense hace innecesario controlar sus niveles; sin embargo, se recomienda para evaluar posibles efectos adversos (por ejemplo, miopatía), sobre todo si hay síntomas o factores de riesgo, y para ayudar a mejorar el cumplimiento. Efectivamente, esta nueva estrategia conlleva la desaparición del concepto de control asociado a un objetivo terapéutico e implica perder una herramienta útil para optimizar la adherencia12. Aunque esta recomendación supondría simplificar el tratamiento y el seguimiento, las guías no especifican durante cuánto tiempo debe mantenerse este tratamiento.
La clasificación estadounidense de las estatinas según la potencia es una aportación positiva porque indica qué estatinas utilizar de forma preferente y a qué dosis, en función del riesgo individual12. De los tres grupos definidos en prevención primaria, la recomendación de tratar con estatinas de alta intensidad a los sujetos de edad ≥21 años con cLDL >190 mg/dl (consideran que la mayoría son hiperlipemias genéticas) obligaría a tratar a más pacientes y con dosis más altas. Para el grupo de diabéticos de 40-75 años con valores de cLDL entre 70 y 189 mg/dl y sin ECV establecida, la recomendación es similar a la europea, aunque queda la duda de qué hacer con los pacientes <40 años. Para el tercer grupo de personas con valores de cLDL entre 70 y 189 mg/dl y estimación de riesgo cardiovascular a 10 años ≥7,5%, la controversia es máxima, pues se emplea una calculadora de riesgo basada en cohortes estadounidenses de razas blanca y afroamericana, que ha sido criticada por sobrestimar el riesgo estableciendo un umbral arbitrario del 7,5% y aplicando modificadores de riesgo si está entre el 5 y el 7,5%. Por el contrario, la guía europea recomienda las tablas SCORE (población europea, incluida población española), y tanto la guía de la International Atherosclerosis Society de 201313 como la del National Institute for Health and Care Excellence de 201411 recomiendan utilizar tablas basadas en la población autóctona, por lo que no resulta aconsejable el empleo de tablas basadas en poblaciones con riesgos muy diferentes, como es el caso objeto de discusión.
La utilización de los fármacos hipolipemiantes alternativos a las estatinas (fibratos, ezetimiba, resinas de intercambio, etc.), que no cuentan con evidencia científica sobre su beneficio para el pronóstico cardiovascular en prevención secundaria, queda relegada a un segundo plano en la guía estadounidense, mientras que en la europea se recomienda, especialmente cuando una estatina potente no logra el control lipídico recomendado. Las combinaciones serían acordes a una estrategia dirigida a alcanzar unos valores objetivo exigentes.
Finalmente, la guía estadounidense define bien los factores de riesgo de efectos adversos de las estatinas y señala que la determinación de la creatincinasa no debe ser sistemática, sino solo en caso de síntomas o antes del tratamiento en situaciones con riesgo de miotoxicidad, lo que evitaría controles innecesarios y, muy posiblemente, suspensiones incorrectas del tratamiento farmacológico12. En comparación con la europea, quizá porque la estadounidense implica mayor uso de estatinas, de más potencia y a dosis superiores, se insiste en la prudencia ante los posibles efectos adversos, cuando en la práctica, con amplísima evidencia en cuanto a seguridad y experiencia de uso, se sabe que su incidencia, con repercusiones clínicas relevantes, es muy baja.
IMPLICACIONES SOCIOECONÓMICAS EN ESPAÑA
La evaluación económica de intervenciones sanitarias se considera un elemento de gran utilidad en la toma de decisiones sobre la incorporación de innovaciones sanitarias y el buen uso de los recursos. En la situación de crisis económica actual, la necesidad de aplicar criterios de eficiencia en la asignación de unos recursos limitados se ha exacerbado. En las evaluaciones económicas, las estatinas son coste-efectivas respecto a los tratamientos no activos en prevención secundaria de la ECV y en prevención primaria de pacientes de alto riesgo, pero su relación coste-efectividad se va haciendo más incierta conforme disminuye el riesgo14. En este contexto, es importante determinar la repercusión económica que conllevaría el drástico cambio que supone aplicar la nueva estrategia de tratamiento de la guía estadounidense.
Las evaluaciones económicas disponibles no aportan evidencia de que unas estatinas sean más coste-efectivas que otras en dosis equipotentes en prevención primaria o secundaria. El consumo de hipolipemiantes en España se ha incrementado entre 2000 y 2012 un 442% (de 18,9 dosis diarias definidas en 2000 a 102,6 en 2012) y las estatinas representaron el 89,3% del uso de hipolipemiantes en 2012 (atorvastatina y simvastatina fueron el 78,2% de ese consumo)15. Sin embargo, el aumento del 26,4% en el uso de estatinas en el trienio 2009-2011 se acompañó de un descenso en los costes de 622 millones a 366 millones de euros, lo que se explica porque casi todas la estatinas están ya disponibles como genéricos, lo que minimiza el impacto económico de una mayor utilización y a dosis más altas16.
El coste del tratamiento hipolipemiante recomendado en la guía depende de la población diana que cumple los criterios y de la intensidad del tratamiento. Esta proviene de los objetivos de cLDL marcados, como en la guía europea, o de una terapia de moderada o alta intensidad en función de las dosis de estatinas, como en la estadounidense. Respecto a la población diana subsidiaria de tratamiento farmacológico, la guía europea incluye específicamente el subgrupo de pacientes con insuficiencia renal. Faltaría por conocer qué población incluye cada uno de los umbrales establecidos con las respectivas tablas de riesgo. En Estados Unidos se estima que, con la aplicación de la nueva guía, el 32,8% de la población de 40-79 años (el 44,3% de los varones y el 22,5% de las mujeres) superaría el nivel de riesgo del 7,5%17, si bien las tablas podrían sobrestimar ese riesgo entre un 75 y un 15018.
Aplicando la nueva guía, con el perfil de factores de riesgo de la cohorte del NHANES-III (National Health and Nutrition Examination Survey-III), 2005-2010 (3773 participantes) extrapolado a toda la población estadounidense 40-75 años (115,4 millones de personas), el número de sujetos susceptibles de tratamiento con estatinas aumentaría de 43,2 millones (37,5%) a 56 millones (48,6%), y la mayor parte de esta diferencia (10,4 de 12,8 millones) serían personas sin ECV19. En el subgrupo de 60-75 años (prevención primaria), aumentaría del 30,4 al 87,4% de los varones y del 21,2 al 53,6% de las mujeres. Usando datos del Swiss CoLaus Study, sobre una muestra de 3297 personas entre 50 y 75 años, se estima que el uso de las nuevas tablas estadounidenses, en comparación con las europeas, multiplicaría por más de dos el número de sujetos susceptibles de tratamiento hipolipemiante, diferencia que es mucho mayor en el grupo de 50-60 años20. Extrapolando los datos a la población suiza, la aplicación de la guía estadounidense supondría un incremento de los costes anuales del tratamiento en prevención cardiovascular de 333,7 millones de euros.
Finalmente, la guía estadounidense no aconseja o restringe mucho el uso de otros tratamientos hipolipemiantes como ezetimiba o los fibratos combinados con estatinas, mientras que la europea admite su uso, aun con un nivel de evidencia subóptimo, para alcanzar los objetivos terapéuticos. Esta circunstancia repercutiría en un mayor coste directo del tratamiento.
ANÁLISIS FINAL Y RECOMENDACIONES DEL COMITÉ ESPAÑOL INTERDISCIPLINARIO DE PREVENCIÓN CARDIOVASCULAR Y DE LA SOCIEDAD ESPAÑOLA DE CARDIOLOGÍA
La nueva estrategia del ACC/AHA, basada en el tratamiento con estatinas de alta o moderada intensidad para cuatro grupos de pacientes bien identificados, representa un cambio sustancial respecto de las recomendaciones de las guías europea y del anterior Adult Treatment Panel-III (centradas en los objetivos específicos de cLDL, en función de las concentraciones lipídicas basales y del riesgo cardiovascular), basadas también en los resultados de los grandes ensayos clínicos aleatorizados y metanálisis realizados en los últimos 20 años21-23. No obstante, conviene subrayar que la citada propuesta no implica grandes diferencias en las recomendaciones para pacientes de alto y muy alto riesgo. Sin embargo, parece claro que su aplicación en la práctica clínica llevaría a sobretratar en prevención primaria, particularmente a personas de edad avanzada, dentro de la categoría de riesgo moderado-alto, tanto por la recomendación de tratamiento farmacológico sistemático como por el predominio de la estrategia de alta intensidad sobre la de moderada intensidad24. Paradójicamente, se desestiman opciones de tratamiento disponibles y actualmente utilizadas que ayudan a alcanzar los objetivos de control.
Este cambio de paradigma, que induce a abandonar los controles analíticos, podría tener un impacto negativo en los pacientes (percepción de menos seguimiento y control, pérdida de adherencia) y los médicos, poco habituados a tratar a ciegas y habituados a un método de trabajo, fuertemente arraigado, basado en conocer y aplicar las guías de práctica clínica y sus objetivos de control, ampliamente difundidos y aceptados en la comunidad científica durante años24. Quizá uno de los puntos fuertes de la guía europea, que más ha contribuido a su implementación en España, sea la definición de objetivos claros en función del riesgo cardiovascular, priorizando a los pacientes con más riesgo para concentrar en ellos la intensidad de las intervenciones preventivas. Los indicadores basados en la consecución de objetivos han permitido conocer el grado de aplicación de las guías en distintos contextos, a través de amplios estudios de evaluación, y después establecer las estrategias de mejora de la calidad de la atención clínica para pacientes y poblaciones concretas25. Además, medir las concentraciones lipídicas puede servir como indicador de la respuesta terapéutica, mejorar la adherencia al tratamiento, ayudar a insistir en los cambios de estilos de vida e identificar situaciones en las que el tratamiento combinado estaría indicado.
El posicionamiento conjunto actual del Comité Español Interdisciplinario de Prevención Cardiovascular y la Sociedad Española de Cardiología (Tabla 2) se reafirma en las recomendaciones de las guías europeas de dislipemias y de prevención cardiovascular en la práctica clínica actualmente vigentes, sobre las cuales ambas entidades realizaron en su momento sus puntualizaciones y comentarios5,6. Las guías deben ser un instrumento dinámico, abierto a nuevas evidencias y aportaciones, y flexible en su aplicación según los distintos entornos sanitarios. Es positivo analizar los cambios de enfoque que se producen en otros entornos, pero esto no debe desviarnos de una línea de trabajo basada en la mejor evidencia científica disponible con criterios de coste-efectividad (lo que no se reduce a los grandes ensayos clínicos aleatorizados), así como en una consolidada estrategia de educación, formación, conocimiento y aplicación de las guías, que persigue mantener y mejorar los resultados en salud de los pacientes y la población general.
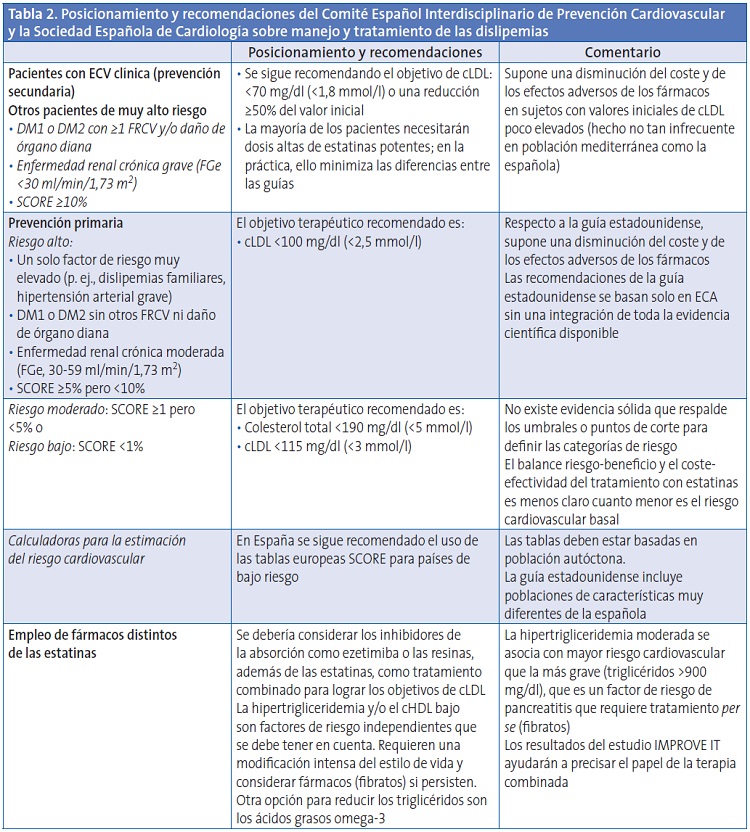
cHDL: colesterol unido a lipoproteínas de alta densidad; cLDL: colesterol unido a lipoproteínas de baja densidad; DM1: diabetes mellitus tipo 1; DM2: diabetes mellitus tipo 2; ECA: ensayos clínicos aleatorizados; ECV: enfermedad cardiovascular; ERC: enfermedad renal crónica; FGe: filtrado glomerular estimado; FRCV: factores de riesgo cardiovascular; IMPROVE-IT: IMProved Reduction of Outcomes Vytorin Efficacy International Trial; SCORE: systematic coronary risk evaluation.
CONCLUSIONES
La publicación de la guía de 2013 de ACC/AHA pone de relieve que hay algunos aspectos por aclarar respecto al tratamiento de la dislipemia y muchos otros puntos de total consenso. El papel central del cLDL para el diagnóstico y el tratamiento y la terapia con estatinas son los dos elementos de acuerdo indiscutible de ambas guías. Sin embargo, la guía europea de 2011 ofrece unas pautas de estratificación del riesgo mucho mejor validadas que las propuestas por la estadounidense, que además supondrían el aumento de personas que deberían recibir tratamiento hipolipemiante, con el riesgo evidente de tratamiento farmacológico innecesario en prevención primaria, particularmente para personas mayores. El objetivo de tratamiento de la guía estadounidense es que los pacientes reciban la intensidad de tratamiento con estatinas acorde con su riesgo individual, mientras que la europea propone objetivos concretos de cLDL para cada categoría de riesgo. Esta diferencia en el paradigma podría confundir a los médicos, lo que levantaría una nueva barrera a la aplicación de la guía, y tener repercusiones para los pacientes, que podrían traducirse en la percepción de menos seguimiento y control y la pérdida de adherencia al tratamiento. Por lo tanto, ambas guías tienen aspectos positivos pero, en general y mientras no se resuelvan las dudas planteadas, la guía europea proporciona mensajes más apropiados para el entorno español y previene del posible sobretratamiento en prevención primaria.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS: ACC/AHA: American College of Cardiology / American Heart Association • cLDL: colesterol unido a lipoproteínas de baja densidad • COR/LOE: class of recommendation/level of evidence • ECV: enfermedad cardiovascular • ESC/EAS: European Society of Cardiology/European Atherosclerosis Society • GRADE: grading of recommendations assessment, development, and evaluation • NHANES-III: National Health and Nutrition Examination Survey-III • SCORE: systematic coronary risk evaluation.
BIBLIOGRAFÍA
- Guallar-Castillón P, Gil-Montero M, León-Muñoz LM, Graciani A, Bayán-Bravo A, Taboada JM, et al. Magnitud y manejo de la hipercolesterolemia en la población adulta de España, 2008-2010: el estudio ENRICA. Rev Esp Cardiol. 2012;65:551-8.
- Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380:2095-128.
- Reiner Z, Catapano AL, De Backer G, Graham I, Taskinen MR, Wiklund O, et al; ESC Committee for Practice Guidelines (CPG) 2008-2010 and 2010-2012 Committees. ESC/EAS Guidelines for the management of dyslipidaemias: the Task Force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and the European Atherosclerosis Society (EAS). Eur Heart J. 2011;32:1769-818.
- Perk J, De Backer G, Gohlke H, Graham I, Reiner Z, Verschuren M, et al; European Association for Cardiovascular Prevention & Rehabilitation (EACPR); ESC Committee for Practice Guidelines (CPG). European Guidelines on cardiovascular disease prevention in clinical practice (version 2012). The Fifth Joint Task Force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice (constituted by representatives of nine societies and by invited experts). Eur Heart J. 2012;33:1635-701.
- Anguita M, Alegría E, Barrios V, Casasnovas JA, Escobar C, León M, et al. Comentarios a las guías de práctica clínica sobre manejo de las dislipemias de la Sociedad Europea de Cardiología y la Sociedad Europea de Aterosclerosis 2011. Un informe del Grupo de Trabajo del Comité de Guías de Práctica Clínica de la Sociedad Española de Cardiología. Rev Esp Cardiol. 2011;64:1090-5.
- Royo-Bordonada MA, Lobos Bejarano JM, Villar Álvarez F, Sans S, Pérez A, Pedro-Botet J, et al. Comentarios del Comité Español Interdisciplinario de Prevención Cardiovascular (CEIPC) a las guías europeas de prevención cardiovascular 2012. Rev Esp Salud Pública. 2013;87:103-20.
- Stone NJ, Robinson J, Lichtenstein AH, Merz CN, Blum CB, Eckel RH, et al. 2013 ACC/AHA Guideline on the Treatment of Blood Cholesterol to Reduce Atherosclerotic Cardiovascular Risk in Adults: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;129(25 Suppl 2):S1-45.
- Institute of Medicine (US) Committee. En: Clinical practice guidelines we can trust. Washington: National Academies Press; 2011.
- Sackett DL. The arrogance of preventive medicine. CMAJ. 2002;167:363-4.
- Reiner Z. Statins in the primary prevention of cardiovascular disease. Nat Rev Cardiol. 2013;10:453-64.
- National Institute for Health and Care Excellence. Lipid modification. Cardiovascular risk assessment and the modifications of blood lipids for the primary and secondary prevention of cardiovascular disease. NICE guideline. Draft for consultation, February 2014 [en línea] [consultado el 25/03/2014]. Disponible en www.nice.org.uk/nicemedia/live/13637/66552/66552.pdf
- Civeira F, Ascaso J, Masana L. Should we forget about low-density lipoprotein cholesterol. J Am Coll Cardiol. 2014;63:1228-9.
- International Atherosclerosis Society. Informe de la Sociedad Internacional de Ateroesclerosis: Recomendaciones generales para el tratamiento de las dislipidemias [en línea] [consultado el 25/03/2014]. Disponible en www.athero.org/download/IASGuidelines_FullText_SPANISH_20140107.pdf
- Ward S, Lloyd Jones M, Pandor A, Holmes M, Ara R, Ryan A, et al. A systematic review and economic evaluation of statins for the prevention of coronary events. Health Technol Assess. 2007;11:1-160.
- Informe de utilizacio´n de medicamentos U/HLP/V1/17012014. Utilización de medicamentos hipolipemiantes en España durante el periodo 2000-2012. Madrid: Agencia Española de Medicamentos y Productos Sanitarios; 2014 [en línea] [consultado el 25/03/2014]. Disponible en www.aemps.gob.es/medicamentosUsoHumano/observatorio/docs/hipolipemiantes-2000-2012.pdf
- Huerta Caballo A, Molina Ortiz R, Molina Úbeda JJ. Consumo de estatinas en España (2009/2011). Farmacéuticos Comunitarios. 2012; 4 Supl 1 [en línea] [consultado el 25/03/2014]. Disponible en www.farmaceuticoscomunitarios.org/journal-article/consumo-estatinas-espana-2009-2011
- Goff DC, Lloyd-Jones DM, Bennett G, Coady S, D’Agostino RB, Gibbons R, et al. 2013 ACC/AHA Guideline on the Assessment of Cardiovascular Risk: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;129 (25 Suppl 2):S49-73.
- Ridker PM, Cook NR. Refining the American guidelines for prevention of cardiovascular disease - Authors’ reply. Lancet. 2014;383:600.
- Pencina MJ, Navar-Boggan AM, D’Agostino RB, Williams K, Neely B, Sniderman AD, et al. Application of new cholesterol guidelines to a population-based sample. N Engl J Med. 2014;370:1422-31.
- Vaucher J, Marques-Vidal P, Preisig M, Waeber G, Vollenweider P. Population and economic impact of the 2013 ACC/AHA guidelines compared with European guidelines to prevent cardiovascular disease. Eur Heart J. 2014;35:958-9.
- Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study of cholesterol lowering with simvastatin in 20,536 high-risk individuals: a randomised placebo-controlled trial. Lancet. 2002;360:7-22.
- Cannon CP, Braunwald E, McCabe CH, Rader DJ, Rouleau JL, Belder R, et al; Pravastatin or Atorvastatin Evaluation and Infection Therapy-Thrombolysis in Myocardial Infarction 22 Investigators. Intensive versus moderate lipid lowering with statins after acute coronary syndromes. N Engl J Med. 2004;350:1495-504.
- Cholesterol Treatment Trialists Collaboration, Baigent C, Blackwell L, Emberson J, Holland LE, Reith C, Bhala N, et al. Efficacy and safety of more intensive lowering of LDL cholesterol: a meta-analysis of data from 170,000 participants in 26 randomised trials. Lancet. 2010;376:1670-81.
- Ray KK, Kastelein JJ, Boekholdt SM, Nicholls SJ, Khaw KT, Ballantyne CM, et al. The ACC/AHA 2013 guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular disease risk in adults: the good the bad and the uncertain: a comparison with ESC/EAS guidelines for the management of dyslipidaemias 2011. Eur Heart J. 2014;35:960-8.
- Kotseva K, Wood D, De Backer G, De Bacquer D, Pyorala K, Keil U; EUROASPIRE Study Group. EUROASPIRE III: a survey on the lifestyle, risk factors and use of cardioprotective drug therapies in coronary patients from 22 European countries. Eur J Cardiovasc Prev Rehabil. 2009;16:121-37.





