Vol. 23 - Num. 91
Originales
Situación de los cuidados paliativos pediátricos en el ámbito de Atención Primaria
Lucía Morán Roldána, Cristina García-Mauriño Alcázarb
aPediatra. CS San Fermín. Madrid. España.
bPediatra. The Institute of Global Health. Kensington. Londres. Reino Unido.
Correspondencia: L Morán. Correo electrónico: lucmoran@hotmail.com
Cómo citar este artículo: Morán Roldán L, García-Mauriño Alcázar C. Situación de los cuidados paliativos pediátricos en el ámbito de Atención Primaria. Rev Pediatr Aten Primaria. 2021;23:261-72.
Publicado en Internet: 10-09-2021 - Número de visitas: 13589
Resumen
Introducción: los pediatras de Atención Primaria (PAP) son un pilar esencial en el manejo de niños con necesidad de cuidados paliativos pediátricos (CPP). Este estudio pretende realizar un análisis descriptivo de la situación de estos profesionales en la Comunidad de Madrid.
Material y métodos: estudio descriptivo y transversal. Se diseñaron, pilotaron y enviaron encuestas digitalizadas previamente a los PAP en activo en la Comunidad de Madrid utilizando listas corporativas.
Resultados: se recibieron un total de 199 encuestas. La mayoría (97%) identificaron correctamente el concepto de niño con necesidad de CPP; solo 24,6% reportó atender algún paciente con estas características. Los pacientes oncológicos fueron el grupo identificado como el más prevalente y casi la mitad de los profesionales identificaron una unidad de CPP en hospitales donde no la hay. Una gran mayoría (70,8%) nunca habían recibido formación en CPP. Más de la mitad reconocieron no sentirse integrados en los equipos específicos de CPP (UCPP), identificándose comunicación entre PAP y las UCPP en no más del 35% de los casos. Solo 14% respondieron sentirse capacitados para manejar estos niños. El 99% manifestó su deseo de participar en su abordaje integral.
Conclusiones: existen importantes carencias y limitaciones respecto a los CPP por parte de los PAP. La formación deficitaria y la falta de cohesión entre niveles asistenciales son factores importantes. Es necesario implementar programas de formación concretos y favorecer un mayor trabajo en red.
Palabras clave
● Atención Primaria ● Cuidados paliativos ● Necesidades y demandas de servicios de saludINTRODUCCIÓN
La Atención Primaria (AP) se define como la asistencia sanitaria centrada en las necesidades y circunstancias de las personas, las familias y las comunidades, abordando la salud y el bienestar físico, psicológico y social.
Esto implica un abordaje integral, desde la promoción y prevención de la salud, hasta el tratamiento, rehabilitación y cuidados paliativos, para satisfacer así las necesidades sanitarias a lo largo de la vida de una persona1.
Todo lo anterior, unido a la filosofía de los profesionales que trabajan en este ámbito, justifican y convierten la AP en un pilar imprescindible en el cuidado de pacientes con patología crónica y complejidad y de pacientes con necesidades de cuidados paliativos (CP).
En este punto, es importante aclarar conceptos en el ámbito pediátrico. Bajo el término de pacientes con patología crónica y complejidad (PPCC) englobaremos pacientes con una enfermedad crónica conocida o desconocida pero sospechada, grave o asociada a fragilidad; con limitaciones funcionales importantes, a menudo dependientes de tecnología; con alta necesidad de recursos y carga familiar2.
Entendemos los cuidados paliativos pediátricos (CPP) como la atención y los cuidados que se proporcionan a pacientes con enfermedades avanzadas, incurables e irreversibles, en los que la evolución clínica de la enfermedad les condiciona una situación de extrema fragilidad que amenaza y limita sus vidas; siendo los objetivos principales mejorar la calidad de vida de los pacientes y sus familias y aliviar su sufrimiento.
Pese a las diferencias conceptuales ambos se caracterizan por un abordaje integral del paciente y sus familias, en respuesta a sus necesidades y problemas físicos, psicológicos, sociales y espirituales.
Continuando con la justificación de este estudio, es relevante señalar el aumento de documentos oficiales nacionales e internacionales que hacen hincapié en la necesidad de la participación de la AP en los CP; y en la importancia de implicar a los pediatras de AP (PAP) en los CPP; considerando esta actividad una competencia más en su práctica diaria, y destacando la necesidad de facilitar formación específica3-7.
Además, son crecientes las referencias desde las asociaciones de Pediatría (Asociación Española de Pediatría, Asociación Española de Pediatría de Atención Primaria, Asociación Madrileña de Pediatría de Atención Primaria), sobre la importancia de integrar al PAP en el cuidado de estos pacientes8-11.
Si analizamos las publicaciones realizadas acerca del abordaje realizado a PPCC y con necesidades de CP por parte de los Equipos de Atención Primaria (EAP), son numerosos y recientes los referidos a adultos12-16. Sin embargo, y pese a que cada año se estima que en España puede haber entre 5500 y 7500 niños entre 0 y 19 años con necesitad de CPP17 (cifra que irá en aumento gracias a avances médicos, mejora de los cuidados, mayor concienciación, aumento de las redes de apoyo, etc.), apenas hay estudios actualizados que reflejen la labor de los pediatras en el cuidados de estos niños18,19 (lo que contrasta con la bibliografía extranjera de los últimos años, donde la AP en CPP cada vez adquiere más protagonismo20-22).
Por lo tanto, ante la evidencia de la necesidad de la participación de los PAP en estos cuidados, el aumento exponencial de este tipo de pacientes y la falta de publicaciones que demuestren esta realidad cambiante de los CPP en el ámbito de la AP; se justifica la realización de este estudio.
El objetivo principal del estudio es analizar la situación actual y global de los CPP en el ámbito de AP en la Comunidad de Madrid (CM) desde el punto de vista de los propios PAP.
MATERIAL Y MÉTODOS
Se realizó un estudio descriptivo, observacional y transversal.
Población a estudio
Se consideró el conjunto de médicos especialistas (sin distinción de pediatras y médicos de familia) que están ejerciendo como PAP en la Comunidad de Madrid en el momento de del muestreo.
Ante la falta de datos oficiales actualizados, se tomó como referencia la última cifra oficial publicada en la memoria de la Gerencia de AP a través de Intranet (diciembre de 2017), en la que habría 911 plazas de PAP en la Comunidad de Madrid.
Muestreo y tamaño muestral
El contacto con la población a estudio se realizó mayoritariamente a través de la lista de correo corporativo de la Asociación Madrileña de Pediatría de Atención Primaria, donde se incluyen de manera voluntaria los socios de esta entidad (un total de 742 profesionales). También se empleó como divulgación los propios contactos de los sanitarios que habían recibido la encuesta, a través de grupos de WhatsApp, correo electrónico, etc.
El muestreo utilizado fue de tipo no probabilístico accidental consecutivos. Los sujetos incluidos en la muestra fueron profesionales que cumplían los criterios de la población a estudio y que contestaron a la encuesta voluntariamente a lo largo del intervalo de tiempo preestablecido.
Método de recogida de datos
Para la recogida de información se diseñó un cuestionario no validado pilotado previamente por pediatras (Tabla 1). El formulario fue autocumplimentado de forma anónima por los profesionales entre el 1 y el 15 de junio de 2019.
| Tabla 1. Encuesta | ||||
|---|---|---|---|---|
| Datos de filiación | ||||
| 1. Sexo | ||||
| 2. Edad | ||||
| 3. Años de ejercicio como pediatra de Atención Primaria | ||||
| 4. Lugar actual de trabajo (indicar centro de salud) | ||||
| 5. Número aproximado de niños incluidos en tu cupo | ||||
| Conocimiento y formación sobre cuidados paliativos pediátricos | ||||
| 6. ¿Qué respuesta define mejor, desde tu punto de vista, al paciente pediátrico que necesita atención y cuidados paliativos? | ||||
| 7. ¿Qué grupo de pacientes crees que son atendidos con mayor frecuencia por las unidades de cuidados paliativos pediátricos? | ||||
| 8. ¿Qué hospitales en la Comunidad de Madrid tienen unidad de cuidados paliativos pediátricos? (puedes marcar varias opciones) | ||||
| 9. ¿Has asistido en alguna ocasión a algún curso o jornada sobre cuidados paliativos pediátricos en los últimos 5 años? | ||||
| 10. Si la anterior respuesta es no: ¿cuáles, entre otros, han sido el motivo? (puedes marcar varias opciones) | ||||
| Cuidados paliativos pediátricos en su práctica profesional habitual | ||||
| 11. Dentro de tu cupo: ¿identificas algún niño que necesita atención y cuidados paliativos? | ||||
| 12. Si la respuesta anterior es afirmativa: ¿te consideras el pediatra responsable de alguno de ellos? (entendiendo responsable al profesional que atiende al niño y a la familia de forma integral y global, independientemente de que esté en seguimiento por otros especialistas) | ||||
| 13. Si la respuesta 11 es afirmativa: ¿sabes si alguno de estos pacientes recibe atención por una unidad de cuidados paliativos pediátricos? | ||||
| 14. En tu experiencia como pediatra de Atención Primaria en la Comunidad de Madrid: ¿alguna vez has contactado tú con la unidad de cuidados paliativos pediátricos para un mejor abordaje de algún paciente? | ||||
| 15. En tu experiencia como pediatra de Atención Primaria en la Comunidad de Madrid: ¿alguna vez han contactado contigo la Unidad de Cuidados Paliativos pediátricos para el abordaje conjunto y coordinado de algún paciente o su familia con necesidad de atención y cuidados paliativos? | ||||
| 16. En tu experiencia como pediatra de Atención Primaria en la Comunidad de Madrid: ¿en alguna ocasión has realizado visita a domicilio para atender a algún paciente con patología crónica y compleja o con necesidad de cuidados y atención paliativa | ||||
| 17. Si la anterior respuesta es no: ¿cuáles son los principales motivos? | ||||
| Reflexión y opinión personal | ||||
| 18. ¿Crees que actualmente los niños con patologías que requieren de cuidados paliativos y sus familias son correctamente atendidos en la Comunidad de Madrid? | ||||
| 19. ¿Crees que las unidades específicas de cuidados paliativos pediátricos integran al pediatra de AP en el equipo encargado de la atención de estos pacientes? | ||||
| 20. ¿Cómo crees que debería organizarse la atención de los pacientes pediátricos que necesitan atención y cuidados paliativos? | ||||
| 21. ¿Con la formación o experiencia que tienes actualmente te sientes cómodo para atender en tu consulta a pacientes con patología crónica-compleja o a que necesitan atención y cuidados paliativo? | ||||
| 22. ¿Y para manejar pacientes con traqueotomía o ventilación mecánica domiciliaria? | ||||
| 23. ¿Y para manejar pacientes con gastrostomía y soporte nutricional enteral? | ||||
| 24. ¿Y para prescribir opioides a pacientes pediátricos? | ||||
| 25. ¿Qué cosas consideras fundamentales para poder manejar adecuadamente a estos pacientes en tu consulta de Atención Primaria? | ||||
| 26. De forma global y tras realizar cambios en la organización asistencial, una mejora en la formación continuada y un apoyo directo de los equipos específicos de Cuidados Paliativos pediátricos ¿te gustaría y estarías dispuesto a atender en la consulta o en los domicilios a pacientes que necesiten atención y cuidados paliativos? | ||||

En él se incluyó información sobre filiación, conocimientos y formación básica en CPP; implicación y actividad asistencial habitual relacionada con CPP y problemas detectados en relación con CPP desde la AP.
Este cuestionario fue realizado por el investigador principal utilizando como ejemplos y guías encuestas empleadas en estudios previos19,23.
Una vez realizada la encuesta definitiva, se transcribió al formato de la plataforma “Formularios Google Docs”, y se difundió.
Estrategia de análisis estadístico
Con los resultados de la Plataforma Google Docs se realizó una base de datos en formato Microsoft Excel. A continuación se empleó el estadístico Stata para el cálculo de distribución de frecuencia de los porcentajes de las variables cualitativas y cuantitativas a estudio. También se calcularon indicadores de tendencia central y distribución.
RESULTADOS
Se obtuvieron un total de 199 encuestas.
Perfil de los PAP
El 84,8% fueron mujeres, siendo el grupo mayoritario el de más de 50 años (48,2%) y el de mayor experiencia profesional (59,3% con 15 años o más) (Fig. 1). La mayoría (60,3%) tenían cupos entre 1000-1500 pacientes.
| Figura 1. Datos demográficos de los profesionales encuestados (porcentaje [%] de PAP por edades y años trabajados en AP) |
|---|
![Figura 1. Datos demográficos de los profesionales encuestados (porcentaje [%] de PAP por edades y años trabajados en AP)](/files/1117-4696-fichero/rpap_1798_paliativos_ap_figura_1.jpg) |

Conocimientos y formación en CPP
Todos los encuestados contestaron saber, desde su punto de vista, el significado de “paciente con necesidad de CPP” y respondiendo prácticamente todos (97%, 195/199) la definición considerada la correcta.
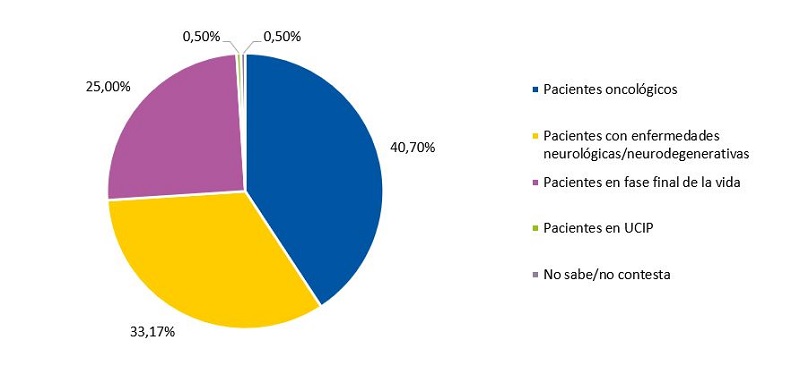
A la hora de identificar los pacientes que con más frecuencia son atendidos por las Unidades Específicas de CPP (UCPP), el 40,7% contestó que pacientes oncológicos (Fig. 2).
| Figura 2. Porcentajes (en orden decreciente) de los distintos grupos de pacientes que son considerados por los PAP como los mayoritariamente atendidos en las unidades específicas de CPP |
|---|
 |

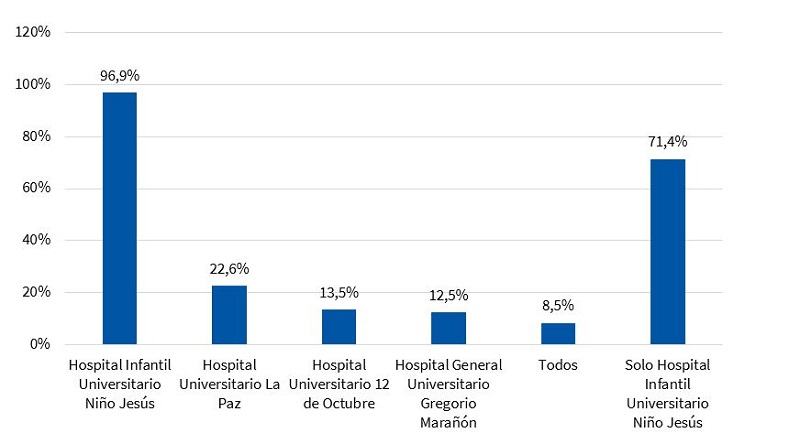
En relación con los hospitales en la Comunidad de Madrid que tienen UCPP, prácticamente toda la muestra (96,9%) identificó al Hospital Universitario Niño Jesús (HNJ) como uno de ellos. De aquellos que contestaron el HNJ, el 26,4% (51/193) creía que también había UCPP en otros hospitales (principalmente la combinación de HNJ y Hospital Infantil Universitario La Paz: 17 personas).
Hay que destacar que 97 encuestados (48,7%) contestaron que hospitales diferentes al HNJ (y en diferentes combinaciones) tienen UCPP y 17 pediatras (8,5%) respondieron que todos los hospitales de tercer nivel de la Comunidad de Madrid tienen una UCPP (Fig. 3).
| Figura 3. Porcentajes de PAP (respecto al total de la muestra), que identifican cada uno de los hospitales de la Comunidad de Madrid como centros con UCPP |
|---|
 |

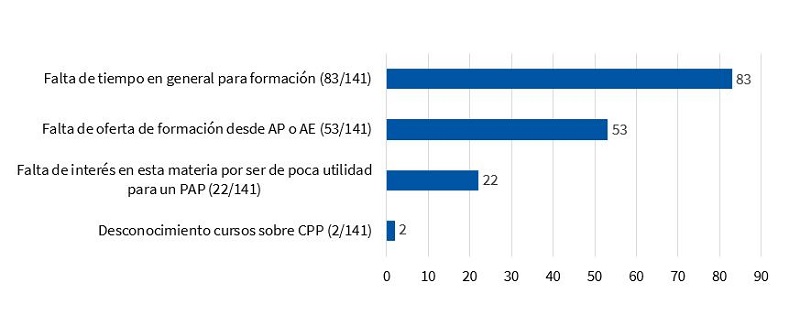
El 70,8% (141/199) reconoció que nunca había asistido a un curso o jornada sobre CPP en los últimos 5 años. Entre los principales motivos destacan la falta de tiempo para formación (58,8%) y la falta de oferta de formación desde AP o Atención Especializada (AE) (37,5%) (Fig. 4). El grupo de pediatras que habían acudido con más frecuencia a algún curso o jornada fueron los mayores de 50 años (44,8%; p = 0,008),
| Figura 4. Principales motivos de no recibir formación en CPP identificados por los propios profesionales (expresado en número total de contestaciones) |
|---|
 |

Incorporación y presencia de los CPP en la práctica profesional habitual de los PAP
Solo el 24,6% (49/199) de los profesionales, identificó en su cupo algún niño con necesidad de atención y CP; 46 de ellos detectaron entre uno y tres niños, lo que correspondería a un total estimado de niños atendidos en AP de entre 46 (como mínimo) y 138 (como máximo). Solo tres pediatras identificaron más de tres pacientes subsidiarios en sus cupos. Hay que recalcar que seis profesionales admitieron no saber reconocer a estos niños.
De todos los pediatras con algún paciente de CPP (N = 49), el 40% declararon no sentirse responsables de ellos.
Vinculación entre los PAP y las UCPP
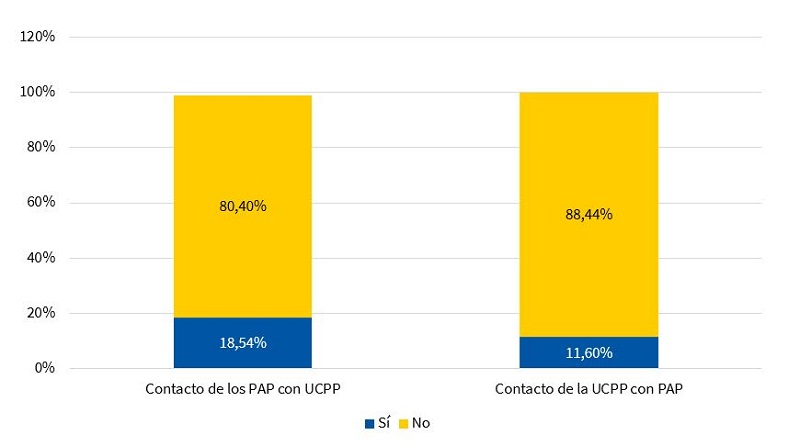
Al preguntarles sobre si habían tenido en alguna ocasión comunicación con una UCPP para el abordaje de algún paciente pediátrico desde AP, solo un 18,5% (37/199) respondieron que sí. Un 11,6% (22/199) habían recibido contacto por parte de una UCPP (Fig. 5).
| Figura 5. Porcentajes de pediatras de Atención Primaria, considerando el total de encuestados (N: 199). que han tenido algún contacto con unidades de CPP (en la primera columna se refleja el contacto establecido desde AP a AE y en la segunda desde AE a AP) |
|---|
 |

Considerando solo los 49 pediatras que identifican algún paciente con necesidad de CPP, en el 34,6% fueron ellos los que contactaron con la UCPP (17/49, Fisher: 0,007), y en el 22,4% (11/49, Fisher: 0,02) fue al revés. 21 pediatras (42%) contestaron no tener ningún tipo de vinculación con la UCPP (incluyéndose seis profesionales que recocieron no saber si sus pacientes reciben o no algún tipo de atención específica).
Atención domiciliaria
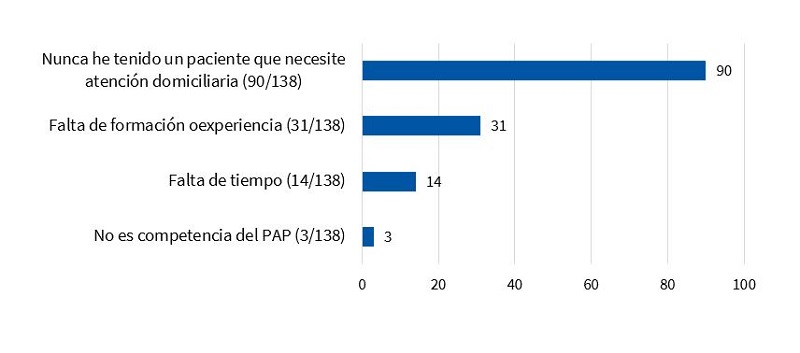
Solo el 30,6% (61/199) han realizado asistencia domiciliaria para el cuidado y atención de pacientes con PPCC o necesidades de CPP (considerando toda su experiencia profesional como PAP). De entre los motivos mayoritarios que justificaron para no realizar domicilios (138/199), excluyendo como la principal causa la carencia de este tipo de pacientes (90/138), se identificó la falta de formación y experiencia y la falta de tiempo concreto para este tipo de atención (22,4 y 10,4% respectivamente) (Fig. 6).
| Figura 6. Motivos identificados por los PAP de no hacer domicilios para el cuidado de pacientes pediátricos con necesidades de CP (expresado en número total de contestaciones entre los que respondieron no hacer domicilio) |
|---|
 |

Opinión personal y autovaloración de los PAP
Más de la mitad de los PAP (55,7%, 111/199) contestaron no sentirse integrados por las UCPP de la Comunidad de Madrid.
De la misma manera, y a modo de autocrítica, solo el 14% respondieron sentirse capacitados o cómodos/as para atender adecuadamente a estos niños (siendo los de menos de cinco años y los de más de 15 años de experiencia los que manifestaron sentirse más cómodos: 42,8 y 46,4%, respectivamente).
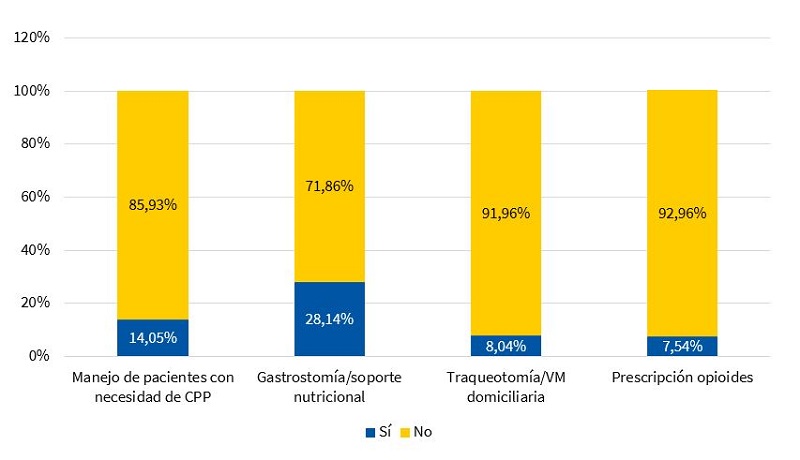
El 28,1% (56/199) reconocieron tener un adecuado manejo de las gastrostomías y la nutrición enteral. En contraposición únicamente 15 pediatras (8%) reconocieron sentirse cómodos con las traqueotomías y la ventilación mecánica domiciliaria. Hay que destacar que solo 15 (7,5%) se consideraron capaces de prescribir opioides (Fig. 7).
| Figura 7. Porcentaje de PAP que reconocen sentirse cómodos (registrado como sí/no) para el manejo de pacientes con necesidades de CPP y para cada una de las actividades señaladas |
|---|
 |

Independientemente de las cuestiones anteriores, la mayor parte de los PAP manifiestan una opinión positiva acerca del manejo de los pacientes con necesidad de CP (solo 34 del total de 199 pediatras respondieron que estos niños no son atendidos correctamente).
Necesidades, problemas y barreras identificadas por los PAP
Prácticamente la totalidad de los encuestados manifestaron que se debería hacer una atención más integral e integrada de estos pacientes, con responsabilidad conjunta y coordinada de los PAP y los profesionales de las UCPP específicas (99,5%).
El 91,9% refieren estar dispuestos y que les gustaría atender en sus consultas o en domicilio a esta población.
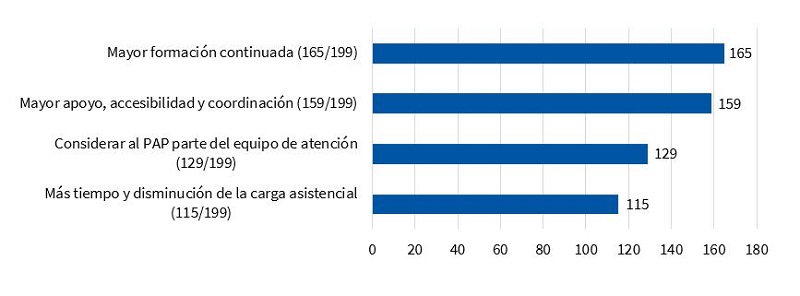
Para ello, la mayoría (165/199, 83%) consideran que es imprescindible una mayor formación continuada impartida desde AP y AE. Además, en un número significativamente alto (155/199, 77,8%) reclaman mayor apoyo, accesibilidad y coordinación con las unidades de CPP, para poder así mejorar la asistencia (Fig. 8).
| Figura 8. Necesidades manifestadas por los PAP para mejorar la atención de los niños con necesidad de CPP (expresada en número total de contestaciones) |
|---|
 |

DISCUSIÓN
Los pediatras de AP constituyen una pieza fundamental e imprescindible en el cuidado y atención de los niños con necesidad de cuidados paliativos, constituyendo el nivel de atención más básico y cercano a la población.
Pese a que cada vez más son los documentos que reflejan la importancia de ello, todavía son necesarias muchas e importantes mejoras para lograr este objetivo.
Analizando los datos obtenidos, los PAP parecen estar bastante familiarizados con el concepto de paciente pediátrico que necesita CPP, lo que podría contribuir de manera positiva en una mayor capacidad para identificar este tipo de niños.
Sin embargo, esta hipótesis no concuerda con los datos obtenidos en los que se pone de manifiesto, una vez más, las claras dificultades para identificar a estos pacientes. Si estimamos la prevalencia hipotética de pacientes con enfermedades subsidiarios de CPP en la Comunidad de Madrid utilizando la tasa publicada por la European Association for Palliative Care en 201717 (10 a 16 niños de menos de 20 años con estas características por cada 100 000 niños), obtendríamos según el último censo poblacional de 2016, un total de 1316 a 2105 niños comprendidos entre estas edades.
A esta cifra añadimos como dato importante el número de pacientes incluidos anualmente en el programa de CPP del HNJ que son un total de 300 pacientes (cifras facilitadas por la propia unidad).
Ambos resultados se alejan significativamente de los valores obtenidos en el estudio, en el que se identifican un máximo de 138 niños con estas características.
Pese a estas diferentes obtenidas, destacar que un número insignificante de encuestados reconocen no saber identificar a estos pacientes, valor que muy probablemente sea mayor.
Los PAP demuestran seguir teniendo conceptos erróneos sobre los CPP. Los pacientes oncológicos son identificados como el grupo más prevalente en los programas de CPP, cuando en la práctica diaria no superan el 30%17. La mayoría de los pacientes incluidos en estos programas son pacientes no oncológicos con clínica predominantemente neurológica (hasta el 70%17), incluyéndose en este grupo pacientes con enfermedades neurodegenerativas, metabólicas, genéticas y síndromes polimalformativos.
Además, un alto el porcentaje de profesionales continúa considerando la existencia de UCPP en hospitales que carecen de estos servicios (el caso de la combinación de HNJ y Hospital La Paz probablemente este en relación con identificar la unidad de PPCC de este centro como una UCPP). Pese a este hecho, es importante señalar que, si comparamos los datos obtenidos en el estudio actual con los obtenidos en el realizado en el 2010 en esta comunidad18, se produce un incremento significativo de los profesionales de AP que identifican la UCPP del HNJ, pasando de solo un 35% a un 96,9% de pediatras.
Entre otras de las conclusiones importantes del estudio es la relación y vinculación deficitaria que se detecta entre los equipos de PAP y los de AE.
En relación con esto último, son muchos los pediatras (algo más del 50%) que expresan su sentimiento de falta de integridad por parte de las UCPP. Los contactos establecidos entre ambos niveles asistenciales para el manejo conjunto resultan muy escasos (siendo esta relación algo más evidente entre los pediatras que si identifican pacientes de CPP en sus cupos, pero en ningún caso en más del 35% de los profesionales).
Según nuestro trabajo, los encuestados manifiestan mayoritariamente sentirse inseguros, incomodos y con escasos recursos para atender a estos pacientes.
Hay que destacar también, y en concordancia con los resultados obtenidos en el estudio de 201819, el número tan bajo de pediatras que reconocen sentirse cómodos y tener un manejo básico de la traqueotomía y de la ventilación mecánica domiciliaria. Mencionar también la falta prácticamente total de experiencia en la prescripción de opioides (no alcanzando el 15%). Por otro lado, la escasa experiencia en domicilios probablemente se relacione con la poca familiarización con tecnología y dispositivos como traqueotomías, respiradores o dispositivos de alimentación enteral; lo cual debería ser parte de las funciones de estos profesionales (como demuestran varios estudios de adultos).
Lo que es evidente y justificaría en gran medida las importantes limitaciones de los PAP detectadas tanto por las encuestas como por los propios profesionales, es la falta de formación en CPP (cifra que incluso supera los registros de estudios anteriores18,19).
Puede que esta situación sea reflejo de un sentimiento por parte de los propios pediatras de poca necesidad de su colaboración en el cuidado de estos niños, ya que la mayoría consideran que estos pacientes son manejados correctamente (independientemente de su participación en el cuidado).
Sin embargo, esto contrasta con su deseo paralelo de aprender e implicarse en sus cuidados, para lo que resulta indiscutible la necesidad de formación en la materia. De esta forman adquirirían las competencias necesarias para: identificar pacientes subsidiarios de CP, colaborar en el manejo y en la toma de decisiones y mejorar su integración en los equipos multi e interdisciplinares.
Para este fin es imprescindible un compromiso tanto de los PAP, como de los equipos de atención especializada y la propia gerencia asistencial; para poder garantizar y reforzar la formación, favorecer una fácil y estrecha colaboración entre niveles asistenciales y ayudar en el desarrollo de un trabajo en red de calidad.
Todo ello permitirá conseguir a un abordaje más integral, integrado, coordinado y multidisciplinar que mejore la calidad de vida de los niños y sus familias.
CONCLUSIONES
Los CPP se caracterizan por realizar un abordaje integral, integrado, multimodal y multidisciplinar del paciente y su familia, en el que los profesionales de AP deben participar de una manera activa, con el fin de lograr un objetivo común: el mayor bienestar y calidad de vida del niño y su familia.
Los PAP que ejercen actualmente en la Comunidad de Madrid demuestran importantes carencias y limitaciones para contribuir de manera adecuada y de calidad en el cuidado de los pacientes con necesidades de CPP.
Estos profesionales, aunque algo más sensibilizados con los CPP, demuestran una vez más la escasa formación y la persistencia de errores conceptuales en esta materia. Además, reflejan falta de capacidades para detectar este tipo de pacientes y limitaciones en las competencias para poder hacer un manejo adecuado.
La mayoría de los PAP no identifican ningún paciente con necesidad de CPP, lo que contrasta con la bibliografía y los registros de los propios centros especializados, en los que la incidencia de pacientes incluidos en estos programas es cada vez mayor. Hay que destacar que, pese a lo anterior, los profesionales que identifican niños con estas características reconocen una implicación y responsabilidad en el seguimiento de estos pacientes bastante heterogénea.
Los pediatras de AP manifiestan una escasa integración en los programas de CPP de las UCPP. Además se plasma una falta de comunicación recíproca entre ambos niveles asistenciales. Sin embargo, y pese a poder parecer algo contradictorio, la mayoría de ellos, valoran la atención de los pacientes por parte de estas UCPP como buena.
Hay que destacar que los PAP manifiestan su un deseo de implicación en el cuidado de estos pacientes y para ello identifican algunos puntos fundamentales para la mejora de la atención destacando: mayor formación en la materia, mayor implicación del PAP en los programas de CPP, mayor apoyo y accesibilidad por parte de las UCPP y más tiempo para estos pacientes.
CONFLICTO DE INTERESES
Las autoras declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS
AE: Atención Especializada · AP: Atención Primaria · CM: Comunidad de Madrid · CP: cuidados paliativos · CPP: cuidados paliativos pediátrico · EAP: Equipos de Atención Primaria · HNJ: Hospital Universitario Niño Jesús · PAP: pediatras de Atención Primaria · PPCC: pacientes con patología crónica y complejidad · UCPP: unidades específicas de cuidados paliativos pediátrico.
BIBLIOGRAFÍA
- Fortalecimiento de los cuidados paliativo como parte del tratamiento integral a lo largo de la vida. 67.ª Asamblea Mundial la Salud, 24 de mayo de 2014. En: Organización Mundial de la Salud [en línea] [consultado el 01/09/2021]. Disponible en https://apps.who.int/gb/ebwha/pdf_files/WHA67/A67_R19-sp.pdf
- Benítez del Rosario MA, Asensio Fraile A. Fundamentos y objetivos de los cuidados paliativos. Aten Primaria. 2002;29:50-2.
- Steering Committee of the EAPC, Task Force on Palliative Care for Children and Adolescents. IMPaCCT: estándares para cuidados paliativos pediátricos en Europa. Med Pal (Madrid). 2008;15:175-80.
- Ley 16/2003, de 28 de mayo, de cohesión y calidad del Sistema Nacional de Salud. BOE núm. 128 de 29 de enero de 2003. En: BOE [en línea] [consultado el 01/09/2021]. Disponible en www.boe.es/buscar/act.php?id=BOE-A-2003-10715
- Real Decreto 1030/2006, de 15 de septiembre, por el que se establece la cartera de servicios comunes del Sistema Nacional de Salud y el procedimiento para su actualización. BOE núm. 222 de 16 de septiembre de 2006. En: BOE [en línea] [consultado el 01/09/2021]. Disponible en www.boe.es/buscar/act.php?id=BOE-A-2006-16212
- Estrategia en Cuidados Paliativos del Sistema Nacional de Salud. Actualización 2010-2014. En: Ministerio de Sanidad, Política Social e Igualdad [en línea] [consultado el 01/09/2021]. Disponible en www.mscbs.gob.es/organizacion/sns/planCalidadSNS/docs/paliativos/cuidadospaliativos.pdf
- Cuidados paliativos pediátricos en el Sistema Nacional de Salud: criterios de atención. En: Ministerio de Sanidad, Política Social e Igualdad [en línea] [consultado el 01/09/2021]. Disponible en www.mscbs.gob.es/organizacion/sns/planCalidadSNS/pdf/01-Cuidados_Paliativos_Pediatricos_SNS.pdf
- Aparicio Rodrigo M, Arana Navarro T, Bras i Marquillas J, Callejas Pozo JE, Kóvacs A, Kubátová G, et al. Currículum de formación en Pediatría de Atención Primaria. En: AEPap [en línea] [consultado el 01/09/2021]. Disponible en www.aepap.org/sites/default/files/documento/archivos-adjuntos/curriculo_europeo_traducido.pdf
- Santos Herráiz P, Losa Frías V, Labarga BH. Cuidados paliativos en Pediatría. Form Act Pediatr Aten Prim. 2017;10:109-14.
- Quiroga Cantero E. Cuidados paliativos: qué debe saber un pediatra de Atención Primaria. Rev Pediatr Aten Primaria. 2014;(23):45-8.
- Ortiz San Román L, Martino Alba RJ. Enfoque paliativo en Pediatría. Pediatr Integral. 2016;XX(2):131.e1-131.e7.
- Blay C, Martori JC, Limon E, Oller R, Vila L, Gómez-Batiste X. Busca tu 1%: prevalencia y mortalidad de una cohorte comunitaria de personas con enfermedad crónica avanzada y necesidades paliativas. Aten Primaria. 2019;51:71-9.
- Herrera Molina E, Rocafort Gil J, Cuervo Pinna MÁ, Redondo Moralo MJ. Primer nivel asistencial en cuidados paliativos: evolución del contenido de la cartera de servicios de Atención Primaria y criterios de derivación al nivel de soporte. Aten Primaria. 2006;38:85-8.
- Vega T, Arrieta E, Lozano JE, Miralles M, Anes Y, Gómez C, et al. Atención sanitaria paliativa y de soporte de los equipos de Atención Primaria en el domicilio. Gac Sanit. 2011;25:205-10.
- Rocafort Gil J, Herrera Molina E, Fernández Bermejo F, Grajera Paredes María ME, Redondo Moralo MJ, Díaz Díez F, et al. Equipos de soporte de cuidados paliativos y dedicación de los equipos de Atención Primaria a pacientes en situación terminal en sus domicilios. Aten Primaria. 2006;38:316-23.
- Meléndez Gracia A. Cuidados Paliativos en AP. ¿Sola, soportada o sustituida? AMF. 2014;10:241-2.
- Cochrane H, Liyanage S, Nantambi R. Palliative Care Statistics for Children and Young Adults. Health and Care Partnerships Analysis. Londres: Department of Health, 2007.
- Astray San Martín A. Encuesta sobre cuidados paliativos a pediatras de Atención Primaria en un área sanitaria de Madrid. Rev Pediatr Aten Primaria. 2010;12:33-40.
- Caballero Pérez V, Rigal Andrés M, Beltrán García S, Parra Plantagenet-Whyte F, Moliner Robredo MC, Gracia Torralba L, et al. Influencia de los recursos especializados en cuidados paliativos pediátricos en los pediatras de Atención Primaria. Rev Pediatr Aten Primaria. 2018;20:133-42.
- Jünger S, Vedeer AE, Milde S, Fischbach T, Zernikow B, Radbruch L. Paediatric palliative home care by general paediatricians: a multimethod study on perceived barriers and incentives. BMC Palliat Care. 2010;9:11.
- Foster CC, Mangione-Smith R, Simon TD. Caring for Children with Medical Complexity: Perspectives of Primary Care Providers. J Pediatr. 2017;182:275-282.e4.
- Verberne LM, Kars MC, Schepers SA, Schouten-Van Meeteren AYN, Grootenhuis MA, Van Delden JJM. Barriers and facilitators to the implementation of a paediatric palliative care team. BMC Palliat Care. 2018;17(1).
- Calleja Gero ML, Rus Palacios M, Martino Alba R, Monleón Luque M, Conejo Moreno D, Ruiz-Falcó Rojas ML. Cuestionario sobre cuidados paliativos a neuropediatras. Neurologia. 2012;27:277-8.




