Influencia de la nacionalidad en la prevalencia de enfermedades frecuentes en Atención Primaria
Inmaculada Navarro Féleza, Lourdes Martínez Angulob, Milagros Gascó Eguiluzc, Cristina Coy Vidald, Margarita García Canelae, Celia Tajada Vitalesf, José Antonio de la Fuente Cadenasg
aEnfermera. EAP Santa Coloma de Gramenet 6. Instituto Catalán de la Salud (ICS). Barcelona. España .
bEnfermera. EAP Santa Coloma de Gramenet 1. Instituto Catalán de la Salud (ICS). Barcelona. España.
cPediatra. EAP Santa Coloma de Gramenet 6. Instituto Catalán de la Salud (ICS). Barcelona. España.
dOdontóloga. EAP Badalona 5. Instituto Catalán de la Salud (ICS). Barcelona. España.
eTrabajadora social. Dirección de Atención Primaria Barcelona Ciudad. Instituto Catalán de la Salud (ICS). Barcelona. España.
fMédico de Familia. EAP Santa Coloma de Gramenet 1. Instituto Catalán de la Salud (ICS). Barcelona. España.
gMédico de Familia. Servicio de Atención Primaria Barcelonés Nord i Maresme. Instituto Catalán de la Salud (ICS). Barcelona. España.
Correspondencia: JA de la Fuente . Correo electrónico: jadelafuente.bnm.ics@gencat.cat
Cómo citar este artículo: Navarro Félez I, Martínez Angulo L, Gascó Eguiluz M, Coy Vidal C, García Canela M, Tajada Vitales C, et al. Influencia de la nacionalidad en la prevalencia de enfermedades frecuentes en Atención Primaria. Rev Pediatr Aten Primaria. 2020;22:e1-e11.
Publicado en Internet: 18-02-2020 - Número de visitas: 15935
Resumen
Introducción: la prevalencia de determinadas enfermedades es diferente en función de factores socioeconómicos o culturales. El objetivo del estudio es describir la frecuencia registrada de exceso de peso, caries, anemia ferropénica (AF) y eccema atópico (EA) en nuestra población infantil en función del país de origen y analizar si existen diferencias entre las diversas nacionalidades.
Material y métodos: se realizó un estudio descriptivo de los diagnósticos registrados en la historia clínica de Atención Primaria. Se valoró la edad, género, nacionalidad y nivel socioeconómico.
Resultados: la población total fue de 81 541 niños de 0 a 14 años. La mayoría eran españoles (84,1%), seguidos de magrebíes (6,9%) e indopakistaníes (3%). La prevalencia de exceso de peso fue del 14,2%, sin diferencias entre españoles e inmigrantes, excepto los iberoamericanos que tenían una mayor prevalencia (22,47%). La prevalencia de caries fue del 17,8% con diferencias significativas entre la población española y la de otros orígenes (15,13 frente a 28,4%). La prevalencia de AF fue del 0,75% apreciándose diferencias en función de la nacionalidad; la AF era diez veces más frecuente en población indopakistaní (5,4%). La prevalencia de EA fue del 15,46%, con diferencias en función de la nacionalidad; el EA era significativamente más frecuente en la población china (20,46%) y magrebí (18,58%).
Conclusión: existen diferencias importantes en la prevalencia de las enfermedades estudiadas en función del país de origen del niño. La Atención Primaria debería abordar la implementación de estrategias preventivas adaptadas a la realidad multicultural de nuestros centros.
Palabras clave
● Anemia ferropénica ● Caries dental ● Eccema atópico ● Epidemiología ● Exceso de peso ● InmigraciónINTRODUCCIÓN
La multiculturalidad y la inmigración representan retos importantes para los profesionales de la salud.
A pesar de la actual crisis económica, España (especialmente Cataluña) sigue siendo un país de acogida de personas y familias que vienen en búsqueda de mejores condiciones de vida, aunque estos últimos años la inmigración ha descendido. En 2016, era de origen inmigrante el 13,6% de la población de Cataluña y el 13,94% de la población entre 0 y 14 años (datos del Instituto Nacional de Estadística, 2016).
La población de orígenes diferentes es un colectivo heterogéneo1,2. Al mismo tiempo, hemos de tener en cuenta que la población autóctona también es absolutamente heterogénea. Los dispositivos asistenciales deben aspirar a ofrecer atención de la misma calidad a todos los usuarios, independientemente de su pertenencia a un grupo cultural u otro3.
Los problemas de salud de la población de otros orígenes no se diferencian básicamente de los de la población autóctona, si excluimos las enfermedades importadas3. Las principales causas de las desigualdades en salud de esta población son el bajo nivel socioeconómico, la irregular situación jurídico-administrativa y las deficientes condiciones de sus viviendas4,5. Esto no es óbice para que determinados factores de la cultura de origen puedan influir en la mayor prevalencia de determinadas enfermedades.
La alimentación está determinada por la cultura propia, las creencias religiosas y el nivel socioeconómico6,7. La alimentación familiar más próxima a la del país de procedencia puede constituir un factor protector frente a la obesidad7,8. El proceso de integración cultural suele provocar cambios en los hábitos alimentarios de la población infantil, aumentando el consumo de alimentos transformados y podría aumentar el riesgo de obesidad6,8,9.
La prevalencia de obesidad en los estudios varía según los criterios diagnósticos empleados10. Actualmente existen básicamente tres estándares diagnósticos de obesidad-sobrepeso en niños: los estándares de la Organización Mundial de la Salud (OMS)11, los de la Internacional Obesity Task Force (IOTF)12 y las tablas de Orbegozo en la población española13. Las cifras más bajas de sobrepeso y obesidad se observan al emplear las tablas de referencia para la población española (26,4%)14, mientras que las más elevadas se obtienen al considerar los estándares de la OMS (41,3%)15.
Existen diferencias entre los estudios en los factores asociados con el sobrepeso en niños. En general, se relaciona con el sexo masculino15-17, el nivel socioeconómico bajo15-17 y el nivel de estudios de los padres15,18,20. El origen inmigrante se asocia en bastantes estudios con una mayor prevalencia de obesidad8,17,19,20, pero en otros estudios esta relación no se ha confirmado15,17.
El estudio Aladino 201515 en población española muestra una prevalencia de sobrepeso del 23,2 % y de obesidad del 18,1 %, utilizando los estándares de la OMS. La prevalencia de sobrepeso es similar en niños y niñas, pero la de obesidad es mayor en los niños. Orsola et al.19 observan un aumento discreto de la prevalencia de obesidad en población infantil inmigrante especialmente de origen sudamericano. El proyecto POIBA17 realizado en Barcelona halla una prevalencia de sobrepeso de 24,0% y de obesidad de 12,7%; la de obesidad fue mayor en niños.
Escartín et al.20 encuentran una prevalencia de obesidad y sobrepeso significativamente mayor en población inmigrante frente a la de origen español (del 39,4 frente al 28,9%) en niños de 6 años; estas diferencias se mantienen al ajustar por nivel socioeconómico, nivel educativo de los progenitores, hábito tabáquico y ganancia de peso durante el embarazo. Una revisión sistemática18 obtiene que la prevalencia de obesidad infantil se relaciona con el nivel de estudios de los padres y el género, pero no halla diferencias significativas por su lugar de origen.
La caries es, actualmente, la enfermedad crónica más frecuente en la infancia21. Es una enfermedad de origen multifactorial relacionada con una higiene oral insuficiente o inadecuada21-23, la alimentación nocturna especialmente en lactantes24, el alto consumo de azúcares24,25, y el bajo nivel socioeconómico de los padres17,24-26. Prácticamente todos los estudios realizados en España muestran una mayor prevalencia de caries en población de origen inmigrante25-28, incluyendo la Encuesta de Salud Oral de España 201525.
El estudio de Barriuso et al.29 y la Encuesta de Salud Oral en España25 muestran que los hábitos higiénicos bucodentales de la población española distan mucho de las recomendaciones. Hemos de asumir que los enfoques restauradores no han conseguido totalmente su objetivo de disminución de la caries30-31.
La anemia por déficit de hierro o ferropénica (AF) en niños es un problema importante en muchos países32. En España, la AF es frecuente en los niños inmigrantes (10%)2. La población más afectada son los niños en periodo de crecimiento (6-24 meses) y las mujeres en edad fértil2. En el estudio de Sánchez et al.33 se detecta una mayor proporción de niños menores de seis años con déficit de hierro y de AF en poblaciones de origen inmigrante, excepto centroamericanos. Saunders et al.34 no encuentran diferencias significativas en la prevalencia de AF según el país de origen de la madre.
Los profesionales de Atención Primaria han detectado una mayor frecuencia de consulta por dermatitis atópica (DA) en niños de origen inmigrante. En diversos estudios realizados en consultas especializadas, la DA es uno de los motivos de consulta más frecuentes35,36. Cantarutti et al.37 revisan las consultas por problemas de la piel en Pediatría de Atención Primaria y observan que la incidencia y prevalencia de DA aumenta de 2006 a 2012, siendo el motivo de consulta dermatológica más frecuente.
Pérez-Crespo et al.38 encontraron que la dermatitis atópica (odds ratio [OR]: 1,65; intervalo de confianza del 95% [IC 95]: 1,19-2,31) fue más frecuente en la población inmigrante en una consulta de dermatología. Otros estudios39,40 muestran que la DA es la causa de consulta dermatológica más frecuente en niños inmigrantes, pero no detectan diferencias con la población autóctona.
En el presente estudio se planteó conocer si existen diferencias en la prevalencia de un grupo de enfermedades frecuentes en la consulta pediátrica en función del país de origen de los niños.
MATERIAL Y MÉTODOS
Se estudió toda la población de 0 a 14 años asignada a los Equipos de Atención Primaria (EAP) del Barcelonés Norte y Maresme del ICS. Se realizó un estudio descriptivo transversal.
Los datos se recogieron del sistema de historia clínica electrónica (eCAP).
Las variables dependientes fueron la presencia de determinadas patologías definidas como:
- Exceso de peso: todos los niños con el código CIE 10 (E66: obesidad o R63.5: sobrepeso) o todos aquellos que tuvieran un índice de masa corporal (IMC) diagnóstico de obesidad o sobrepeso según las tablas de Orbegozo13. Se excluyeron del análisis de esta variable los niños en que no constaba ningún IMC ni diagnóstico.
- Caries: se consideró que el niño presenta caries cuando conste el código K02 (caries) o esté registrado un índice CAOD ≥1 o un índice COD ≥1. Si no existía ningún registro se consideró que el niño no presentaba caries.
- Anemia ferropénica: código D50.
- Eccema atópico: código L20.
Se analizaron como variables independientes: la edad, el género, el país de origen y el nivel socioeconómico. Respecto a la edad se agruparon los niños en dos grupos de 0 a 5 y de 6 a 14 años.
Se consideró país de origen el que constaba en el campo nacionalidad del programa eCAP; se agruparon los países en los siguientes grupos: España; Magreb; Indopakistaní; China-Sudeste Asiático; Iberoamérica; África Subsahariana; Europa Oriental; Europa Occidental; otros.
El nivel socioeconómico no se ha podido obtener a nivel individual. Se ha utilizado el nivel socioeconómico calculado por el Departamento de Salud de la Generalitat de Cataluña42. Se agruparon los EAP en dos niveles: nivel socioeconómico muy bajo; nivel socioeconómico bajo-medio-alto.
Se realizó un análisis descriptivo de las variables comparando la prevalencia de las enfermedades entre las diferentes nacionalidades, utilizando como medidas de significación estadística el test de chi cuadrado para variables cualitativas y el cálculo del IC 95.
Los datos han sido extraídos de manera centralizada y anonimizada; no se ha podido obtener ninguna información de carácter personal. El estudio está basado en las normas de buena práctica clínica de acuerdo con la declaración de Helsinki. El protocolo de estudio fue aprobado por el Comité de Ética e Investigación Clínica del Institut d’Investigació en Atenció Primària (IDIAP) Jordi Gol, institución de referencia para la Investigación en Atención Primaria del ICS (Código: P18/066).
RESULTADOS
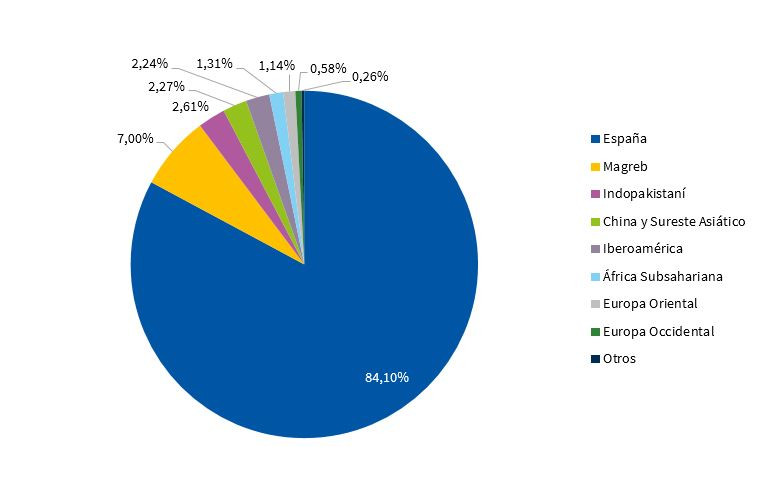
La población total fue de 81 541 niños. La nacionalidad más frecuente fue la española con el 84,1%, seguida del Magreb e indopakistaníes (Fig. 1).
El 48,3% eran niñas. La edad media fue de 7,48 años (IC 95: 7,45-7,51). Los niños iberoamericanos fueron un poco mayores que los españoles, mientras los indopakistaníes y del Magreb eran más jóvenes.
La prevalencia global de exceso de peso fue del 14,2%. Analizando globalmente los niños españoles frente a los de otros orígenes, la prevalencia de exceso de peso no mostró diferencias significativas: 14,1 frente a 14,7% (p = 0,120). El grupo de mayores de cinco años tenían una prevalencia mayor que el de los niños menores, 15,6 frente a 11,3% (p <0,000). La Tabla 1 muestra la distribución del exceso de peso según el país de origen y grupos de edad. Se aprecia que la prevalencia de exceso de peso fue superior en los niños iberoamericanos a cualquier edad.
| Tabla 1. Prevalencia de exceso de peso por país de origen y por grupos de edad | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Total niños | Niños 0-5 años | Niños 6-14 años | |||||||
| Prevalencia | IC 95 | Prevalencia | IC 95 | Prevalencia | IC 95 | ||||
| España | 14,12% | 13,84% | 14,41% | 10,69% | 10,24% | 11,13% | 15,73% | 15,37% | 16,09% |
| Magreb | 12,29% | 11,28% | 13,29% | 14,21% | 12,49% | 15,94% | 11,08% | 9,85% | 12,31% |
| Indopakistaní | 14,49% | 12,88% | 16,09% | 12,30% | 9,84% | 14,76% | 15,76% | 13,67% | 17,84% |
| China y Sureste Asiático | 14,32% | 12,54% | 16,10% | 11,90% | 8,86% | 14,94% | 15,33% | 13,15% | 17,51% |
| Iberoamérica | 22,47% | 20,36% | 24,58% | 21,45% | 17,56% | 25,33% | 22,88% | 20,37% | 25,39% |
| África Subsahariana | 15,42% | 13,12% | 17,72% | 14,95% | 10,92% | 18,98% | 15,63% | 12,83% | 18,44% |
| Europa Oriental | 13,57% | 11,03% | 16,11% | 11,01% | 6,94% | 15,09% | 14,80% | 11,60% | 18,00% |
| Europa Occidental | 11,14% | 7,85% | 14,44% | 12,90% | 6,09% | 19,72% | 10,51% | 6,76% | 14,25% |
| Otros | 16,67% | 11,13% | 22,20% | 16,36% | 6,59% | 26,14% | 16,81% | 10,09% | 23,53% |
| Total | 14,21% | 13,95% | 14,47% | 11,30% | 10,89% | 11,72% | 15,60% | 15,27% | 15,93% |

Los niños tenían significativamente una mayor prevalencia de exceso de peso que las niñas, 15,8 frente a 12,5% (p <0,000). En todos los orígenes la prevalencia fue mayor en niños, con diferencias significativas excepto en Europa Occidental. Destaca la gran diferencia por sexos en los niños de origen chino (21,24 frente a 7,3%).
En los niños de los EAP con nivel socioeconómico más bajo, la prevalencia de exceso de peso era más alta, 16,7 frente a 13,3% (p <0,000). La Tabla 2 muestra las diferencias de exceso de peso según el nivel socioeconómico y la nacionalidad. Se puede apreciar que las diferencias se deben prácticamente a los niños españoles.
| Tabla 2. Prevalencia de exceso de peso por país de origen y nivel socioeconómico | |||||||
|---|---|---|---|---|---|---|---|
| Nivel socioeconómico bajo | Nivel socioeconómico medio-alto | ||||||
| Prevalencia | IC 95 | Prevalencia | IC 95 | ||||
| España | 17,76% | 17,10% | 18,41% | 13,08% | 12,76% | 13,39% | |
| Magreb | 11,76% | 10,42% | 13,10% | 12,91% | 11,39% | 14,42% | |
| Indopakistaní | 14,20% | 12,32% | 16,08% | 15,21% | 12,14% | 18,28% | |
| China y Sureste Asiático | 14,57% | 12,19% | 16,95% | 14,00% | 11,32% | 16,68% | |
| Iberoamérica | 23,96% | 20,41% | 27,52% | 21,60% | 18,98% | 24,22% | |
| África Subsahariana | 15,80% | 12,77% | 18,83% | 14,87% | 11,34% | 18,40% | |
| Europa Oriental | 9,40% | 6,08% | 12,71% | 16,67% | 13,02% | 20,31% | |
| Europa Occidental | 11,90% | 2,11% | 21,70% | 11,04% | 7,54% | 14,54% | |
| Otros | 22,92% | 11,03% | 34,81% | 14,29% | 8,18% | 20,40% | |
| Total | 16,65% | 16,12% | 17,18% | 13,30% | 13,00% | 13,59% | |

La prevalencia global de caries fue del 17,8%. Un 15,13% en los niños españoles frente a un 28,4% en la población de otras nacionalidades (p <0,000). La Tabla 3 muestra la prevalencia de caries por país de origen y edad. Los niños de todas las nacionalidades, salvo los de Europa Occidental, tenían significativamente más prevalencia de caries que los niños españoles. No se observaron diferencias significativas por género. La prevalencia aumenta con la edad (3,4 frente 25,5%). Todas las nacionalidades mantuvieron las diferencias en los distintos grupos de edad (Tabla 3).
| Tabla 3. Prevalencia de caries por país de origen y por grupos de edad | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Total niños | Niños 0-5 años | Niños 6-14 años | |||||||
| Prevalencia | IC 95 | Prevalencia | IC 95 | Prevalencia | IC 95 | ||||
| España | 15,13% | 14,86% | 15,40% | 2,19% | 2,01% | 2,38% | 22,08% | 21,69% | 22,46% |
| Magreb | 37,27% | 35,85% | 38,69% | 10,50% | 9,07% | 11,93% | 54,64% | 52,77% | 56,51% |
| Indopakistaní | 30,17% | 28,22% | 32,12% | 9,26% | 7,26% | 11,26% | 43,02% | 40,35% | 45,69% |
| China y Sureste Asiático | 38,61% | 36,39% | 40,82% | 12,81% | 9,96% | 15,65% | 48,98% | 46,28% | 51,67% |
| Iberoamérica | 23,90% | 21,95% | 25,86% | 6,69% | 4,61% | 8,77% | 31,39% | 28,84% | 33,94% |
| África Subsahariana | 28,22% | 25,53% | 30,92% | 4,66% | 2,43% | 6,90% | 39,34% | 35,79% | 42,89% |
| Europa Oriental | 28,33% | 25,43% | 31,22% | 11,52% | 8,07% | 14,96% | 37,54% | 33,67% | 41,41% |
| Europa Occidental | 7,63% | 5,23% | 10,02% | 2,16% | 0,26% | 4,57% | 9,91% | 6,70% | 13,12% |
| Otros | 28,77% | 22,68% | 34,87% | 17,65% | 8,59% | 26,71% | 34,03% | 26,29% | 41,77% |
| Total | 17,78% | 17,52% | 18,04% | 3,37% | 3,16% | 3,57% | 25,53% | 25,16% | 25,90% |

La prevalencia de caries en los equipos de índice socioeconómico bajo fue del 27,82 frente al 14,1% en el resto (p <0,000). La Tabla 4 muestra la prevalencia de caries por nacionalidades y nivel socioeconómico. En todos los casos la prevalencia fue menor en los niños residentes en zonas con mayor nivel socioeconómico, aunque, en algunos casos, los intervalos de confianza no llegaron a mostrar diferencias significativas. También destaca que, en los dos niveles socioeconómicos, las diferencias entre países de origen se mantienen.
| Tabla 4. Prevalencia de caries por país de origen y nivel socioeconómicoh | ||||||
|---|---|---|---|---|---|---|
| Nivel socioeconómico bajo | Nivel socioeconómico medio-alto | |||||
| Prevalencia | IC 95 | Prevalencia | IC 95 | |||
| España | 24,20% | 23,52% | 24,89% | 12,60% | 12,31% | 12,88% |
| Magreb | 40,74% | 38,79% | 42,69% | 33,12% | 31,08% | 35,16% |
| Indopakistaní | 31,47% | 29,12% | 33,82% | 27,07% | 23,59% | 30,55% |
| China y Sureste Asiático | 41,54% | 38,54% | 44,53% | 34,85% | 31,57% | 38,13% |
| Iberoamérica | 28,29% | 24,88% | 31,71% | 21,37% | 19,00% | 23,73% |
| África Subsahariana | 28,50% | 24,99% | 32,02% | 27,82% | 23,61% | 32,03% |
| Europa Oriental | 31,40% | 26,93% | 35,87% | 25,87% | 22,10% | 29,64% |
| Europa Occidental | 19,35% | 9,52% | 29,19% | 5,85% | 3,58% | 8,13% |
| Otros | 50,91% | 37,70% | 64,12% | 21,02% | 14,65% | 27,39% |
| Total | 27,82% | 27,23% | 28,42% | 14,12% | 13,84% | 14,40% |

La prevalencia de AF registrada fue de 0,75%. La prevalencia de anemia en niños españoles fue de 0,5 frente al 1,9% en otros orígenes (p <0,000). La Tabla 5 muestra la distribución de la prevalencia de AF por origen y nivel socioeconómico. La prevalencia en niños indopakistaníes fue aproximadamente diez veces más alta que en niños españoles. También fue significativamente más elevada la prevalencia en niños del Magreb y subsaharianos mientras que es menor en niños chinos. Los niños residentes en zonas con nivel socioeconómico bajo tienen una mayor prevalencia de AF. La prevalencia de AF fue mayor en niños que en niñas (0,9 frente a 0,6; p <0,000). También fue mayor en niños de 6 a 14 años que en los menores de esta edad: 0,8% frente a 0,6% (p = 0,009).
| Tabla 5. Prevalencia de anemia ferropénica por país de origen y nivel socioeconómico | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Total niños | Nivel socioeconómico bajo | Nivel socioeconómico medio-alto | |||||||
| Prevalencia | IC 95 | Prevalencia | IC 95 | Prevalencia | IC 95 | ||||
| España | 0,52% | 0,47% | 0,57% | 0,66% | 0,53% | 0,79% | 0,48% | 0,42% | 0,54% |
| Magreb | 1,92% | 1,52% | 2,32% | 1,93% | 1,38% | 2,47% | 1,91% | 1,32% | 2,51% |
| Indopakistaní | 5,40% | 4,44% | 6,36% | 5,60% | 4,44% | 6,76% | 4,94% | 3,24% | 6,63% |
| China y Sureste Asiático | 0,16% | 0,02% | 0,35% | 0,10% | -0,09% | 0,28% | 0,25% | -0,09% | 0,59% |
| Iberoamérica | 0,71% | 0,33% | 1,10% | 0,90% | 0,18% | 1,61% | 0,61% | 0,16% | 1,05% |
| África Subsahariana | 2,06% | 1,21% | 2,91% | 2,52% | 1,30% | 3,74% | 1,38% | 0,28% | 2,48% |
| Europa Oriental | 0,97% | 0,34% | 1,59% | 1,21% | 0,16% | 2,26% | 0,77% | 0,02% | 1,53% |
| Europa Occidental | 0,21% | 0,20% | 0,63% | 0,00% | 0,00% | 0,00% | 0,24% | -0,23% | 0,72% |
| Otros | 0,94% | 0,36% | 2,24% | 3,64% | -1,31% | 8,58% | 0,00% | 0,00% | 0,00% |
| Total | 0,75% | 0,69% | 0,80% | 1,19% | 1,05% | 1,34% | 0,58% | 0,52% | 0,64% |

La prevalencia de EA fue de 15,46%. No se observaron diferencias por género. La prevalencia de eccema atópico fue más baja en los niños residentes en zona socioeconómicas deprimidas: 13,8 frente a 16,1% (p <0,000). Los niños de 6-14 años tienen una mayor prevalencia que los menores de esta edad: 15,8 frente a 14,8% (p = 0,007). Los niños chinos y del Magreb tienen una prevalencia mayor mientras los indopakistaníes y de Europa Oriental tienen una prevalencia menor (Tabla 6).
| Tabla 6. Prevalencia de eccema atópico por país de origen y nivel socioeconómico | |||
|---|---|---|---|
| Total niños | |||
| Prevalencia | IC 95 | ||
| España | 15,31% | 15,04% | 15,58% |
| Magreb | 18,58% | 17,44% | 19,72% |
| Indopakistaní | 11,70% | 10,34% | 13,07% |
| China y Sureste Asiático | 20,46% | 18,63% | 22,30% |
| Iberoamérica | 14,86% | 13,23% | 16,49% |
| África Subsahariana | 17,10% | 14,85% | 19,36% |
| Europa Oriental | 9,01% | 7,17% | 10,85% |
| Europa Occidental | 15,89% | 12,59% | 19,19 |
| Otros | 16,04% | 11,10% | 20,98% |
| Total | 15,46% | 15,21% | 15,70% |

DISCUSIÓN
Los estudios sobre base de datos informatizada, como el presente, tienen la ventaja de que el número de sujetos a analizar es elevado. Uno de los principales sesgos de estos estudios es el infrarregistro de diagnósticos. En nuestro caso, creemos que el infrarregistro será mayor en población de origen inmigrante, por lo cual las diferencias observadas podrían ser incluso mayores, aunque en algún caso podríamos no detectar diferencias significativas cuando en realidad sí existen.
El otro sesgo inherente a estos estudios es el relacionado con la fiabilidad de los diagnósticos. Al utilizar registros anteriores al estudio y múltiples observadores, no podemos garantizar la uniformidad de los criterios diagnósticos.
En este caso, el registro del país de origen también podría ser una limitación, al no tener claro cómo se registra la nacionalidad en casos de doble nacionalidad, niños nacidos en España pero de familias inmigradas…
Al no disponer de indicadores socioeconómicos fiables a nivel individual, hemos adjudicado a cada niño el índice socioeconómico de su barrio de residencia al igual que en otros estudios19.
La prevalencia de exceso de peso observada, según se muestra en la Tabla 1, fue de 14,2 en niños entre 0-14 años, notablemente inferior a la descrita en la literatura. Los estudios que utilizan los estándares de la OMS muestran prevalencias entre el 31-41%15,16,19, aunque son difícilmente comparables. El estudio enKid14, usando las tablas de Orbegozo de 1988, encuentra una prevalencia del 26,3% en niños de 2 a 24 años que también es notablemente superior al 15,6% en niños de 6 a 14 años de nuestro estudio. Creemos que estas diferencias pueden deberse a un infrarregistro en nuestra población y a que nosotros utilizamos les tablas de Orbegozo de 2011, que minimizan las cifras de niños con sobrepeso.
En nuestro estudio se detecta una mayor prevalencia de exceso de peso en población iberoamericana, como en los estudios de Cheikk et al.8 y Orsola et al.18.
Se observa una mayor prevalencia de obesidad en varones, similar a la descrita en la literatura médica14-17. Destaca mucho que la obesidad en varones chinos es superior a la de los niños autóctonos, mientras en niñas es claramente inferior.
Al igual que en la mayoría de estudios15-17, el nivel socioeconómico bajo se asocia a una mayor frecuencia de exceso de peso. Esta diferencia solo llega a ser significativa en los niños españoles, probablemente debido al menos número de sujetos en cada subgrupo. Destaca que en niños de Europa Oriental de nivel socioeconómico bajo la prevalencia de obesidad es significativamente inferior a la de los de nivel socioeconómico alto.
La prevalencia de caries registrada en nuestro estudio es aproximadamente la mitad de la encontrada en la Encuesta de Salud Oral 201525. En nuestra población la prevalencia en niños de 0 a 14 años es del 15,13% en niños españoles y del 28,4% en niños de otros orígenes, frente a la prevalencia encontrada en la Encuesta de Salud Oral que, dependiendo del grupo de edad, oscila entre 30-42% en los niños españoles y 51,5-55% en los niños de otros orígenes.
En coincidencia con la literatura médica, observamos mayor prevalencia de caries en niños de origen inmigrante25-28 de todas las nacionalidades, excepto Europa Occidental, y de nivel socioeconómico bajo17,24-26. La prevalencia de caries, como es lógico, aumenta con la edad.
La prevalencia de anemia ferropénica es inferior a otros estudios2,33. Probablemente esta diferencia sea debida a infrarregistro o infradiagnóstico. Al igual que Sánchez et al.33, encontramos mayor prevalencia de anemia ferropénica en la población indopakistaní. A pesar de que en la literatura médica está descrito que la AF afecta más a niños entre 6 y 24 meses2, en nuestro caso el registro es mayor en niños de 6 a 14 años.
La dermatitis atópica es uno de los motivos más frecuentes de consulta dermatológica en la infancia39,40. Nuestros datos confirman la sensación de los profesionales de una elevada prevalencia en niños de origen chino, que coinciden con los datos del estudio de Horii et al.41.
Nuestros datos confirman que algunas patologías son más prevalentes en poblaciones de origen no español. Especialmente preocupante es la elevada incidencia de caries en prácticamente toda la población de origen inmigrante. En el resto de las patologías, las diferencias se establecen en unos orígenes concretos: obesidad en población sudamericana; anemia ferropénica en indopakistaníes y dermatitis atópica en población china y magrebí. Estas prevalencias justifican el diseño de intervenciones para mejorar la prevención, adaptadas al origen multicultural de nuestra población42.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS
AF: anemia ferropénica · CAOD (índice): número de dientes cariados, ausentes y obturados dividido por el total de dientes (en dentición permanente) · CIE: Clasificación internacional de enfermedades · COD (índice): número de dientes cariados y obturados dividido por el total de dientes, en dentición temporal · DA: dermatitis atópica · EAP: Equipos de Atención Primaria · ICS: Institut Català de la Salut · IC 95: intervalo de confianza del 95% · IDIAP: Institut d’Investigació en Atenció Primària · IMC: índice de masa corporal · IOTF: Internacional Obesity Task Force · OMS: Organización Mundial de la Salud (OMS) · OR: odds ratio.
BIBLIOGRAFÍA
- Pla de la Diversitat. Recomanacions per a l’Atenció Primària dirigida a usuaris immigrants extracomunitaris. En: Institut Català de la Salut [en línea] [consultado el 17/02/2020]. Disponible en http://canalsalut.gencat.cat/web/.content/_A-Z/I/immigracio_i_salut/documents/arxius/recopriextra2007.pdf
- Masvidal RM, Canadell D, Grupo de Cooperación, Inmigración y Adopción de la AEPap. Actualización del Protocolo de Atención a las Niñas y Niños Inmigrantes. Revisión 2016. Form Act Pediatr Aten Prim. 2017;10:3-15.
- Comité Consultivo de Bioética de Catalunya. Orientaciones sobre la diversidad cultural y salud. En: Organización Médica Colegial de España [en línea] [consultado el 17/02/2020]. Disponible en https://www.ffomc.org/CursosCampus/Intercultural/Modulo3/curso/03/pdf/anexo4.pdf
- Vázquez ML, Vargas I, Aller MB. Reflexiones sobre el impacto de la crisis en la salud y la atención sanitaria de la población inmigrante. Informe SESPAS 2014. Gac Sanit. 2014;28:142-6.
- Malmusi D, Borrell C, Benach Migration-related health inequalities: showing the complex interactions between gender, social class and place of origin. Soc Sci Med. 2010;71:1610-9.
- Ferrer B, Vitoria I, Dalmau J. La alimentación del niño inmigrante. Riesgos y carencias nutricionales. Acta Pediatr Esp. 2012;70:147-4.
- Vidal M, Ngo J. Recomanacions per al consell alimentari en un entorn de diversitat cultural. Pla Director d’Immigració en l’Àmbit de la Salut: Departament de Salut. Generalitat de Catalunya. Barcelona: Direcció General de Planificació i Avaluació; 2007 [en línea] [consultado el 17/02/2020]. Disponible en https://scientiasalut.gencat.cat/bitstream/handle/11351/1914/recomanacions_consell_alimentari_entorn_diversitat_cultural_2007.pdf?sequence=1
- Cheikh K, Sanz-Valero J, Wanden-Berghe C. Los determinantes sociales de la inmigración infanto-juvenil y su influencia sobre el estado nutricional: revisión sistemática. Nutr Hosp. 2014;30:1008-19.
- Gualdi-Russo E, Zaccagni L, Manzon VS, Masotti S, Rinaldo N, Khyatti M. Obesity and physical activity in children of immigrants. Eur J Public Health. 2014;24:40-6.
- Sánchez Echenique M. Aspectos epidemiológicos de la obesidad infantil. Rev Pediatr Aten Primaria Supl. 2012;(21):9-14.
- Índice de masa corporal para la edad (5-19 años); 2013. En: Organización Mundial de la Salud [en línea] [consultado el 17/02/2020]. Disponible en www.who.int/growthref/who2007_bmi_for_age/en/
- Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ. 2000;320:1240-3.
- Fernández C, Lorenzo H, Vrotsou K, Aresti U, Rica I, Sánchez E. Estudio de crecimiento de Bilbao. Curvas y tablas de crecimiento. Estudio transversal. Bilbao: Fundación Faustino Orbegozo Eizaguirre; 2011.
- Serra L, Ribas L, Aranceta L, Pérez C, Saavedra P, Peña L. Obesidad infantil y juvenil en España. Resultados del Estudio enKid (1998-2000). Med Clin (Barc). 2003;121:725-32.
- Estudio ALADINO 2015: Estudio de vigilancia del crecimiento, alimentación, actividad física, desarrollo infantil y obesidad en España 2015. En: Agencia Española de Consumo, Seguridad Alimentaria y Nutrición; Ministerio de Sanidad, Servicios Sociales e Igualdad [en línea] [consultado el 17/02/2020]. Disponible en www.aecosan.msssi.gob.es/AECOSAN/docs/documentos/nutricion/observatorio/Estudio_ALADINO_2015.pdf
- Sánchez-Cruz JJ, Jiménez-Moleón JJ, Fernández-Quesada F, Sánchez MJ. Prevalence of child and youth obesity in Spain in 2012. Rev Esp Cardiol (Engl Ed). 2013;66:371-6.
- Sánchez-Martínez F, Torres P, Serral G, Valmayor S, Castell C, Ariza C. Factores asociados al sobrepeso y la obesidad en escolares de 8 a 9 años de Barcelona. Rev Esp Salud Publica. 2016;90:e1-e11.
- Font-Ribera L, García-Continente X, Davó-Blanes MC, Ariza C, Díez E, García MM, et al. El estudio de las desigualdades sociales en la salud infantil y adolescente en España. Gac Sanit. 2014;28:316-25.
- Orsola Lecha E, Pérez Pérez I. Obesidad: estudio de casos en una población infanto-juvenil inmigrante. Rev Pediatr Aten Primaria. 2005;7:41-8.
- Escartín L, Mayor EA, Samper MP, Labayen I, Álvarez ML, Moreno LA, et al. Inmigración y riesgo de sobrepeso y obesidad en niños en edad escolar. Acta Pediatr Esp. 2017;75:36-42.
- Casals Peidró E, García Pereiro MA. Guía de práctica clínica para la prevención y tratamiento no invasivo de la caries dental. RCOE. 2014;19:189-248.
- Alm A. On dental caries and caries-related factors in children and teenagers. Swed Dent J Suppl. 2008;195:7-63.
- Gibson S, Williams S. Dental caries in pre-school children: associations with social class, toothbrushing habit and consumption of sugars and sugar-containing foods. Further analysis of data from the National Diet and Nutrition Survey of children aged 1.5-4.5 years. Caries Res. 1999;33:101-13.
- Declerck D, Leroy R, Martens L, Lesaffre E, García-Zattera MJ, Vanden Broucke S, et al. Factors associated with prevalence and severity of caries experience in preschool children. Community Dent Oral Epidemiol. 2008;36:168-78.
- Bravo M, Almerich JM, Ausina V, Avilés P, Blanco JM, Canorea E, et al. Encuesta de Salud Oral en España 2015. RCOE. 2016;21:8-48..
- Cortés FJ, Artázcoz J, Rosel E, González P, Asenjo MA, Sáinz de Murieta I, et al. La salud dental de los niños y adolescentes de Navarra, 2007 (4.ª edición). An Sist Sanit Navar. 2009;32:199-215.
- Paredes V, Paredes C, Mir B. Prevalencia de la caries dental en el niño inmigrante: estudio comparativo con el niño autóctono. An Pediatr (Barc). 2006;65:337-41.
- Almerich-Silla JM, Montiel-Company JM. Oral health survey of the child population in the Valencia Region of Spain (2004). Med Oral Patol Oral Cir Bucal 2006; 11:E369-81.
- Barriuso L, Sanz B, Hernando L. Prevalencia de hábitos bucodentales saludables en la población infanto-juvenil residente en España. An Pediatr (Barc). 2012;76:140-7.
- Protocolo de diagnóstico, pronóstico y prevención de la caries de la primera infancia. Revisión julio 2017. Sociedad Española de Odontopediatría [en línea] [consultado el 17/02/2020]. Disponible en www.odontologiapediatrica.com/wp-content/uploads/2018/06/SEOP_-_Caries_precoz_de_la_infancia_fin4.pdf
- WHO Expert Consultation on Public Health Intervention against early childhood caries: report of a meeting, Bangkok, Thailand, 26-28 January 2016. En: Organización Mundial de la Salud [en línea] [consultado el 17/02/2020]. Disponible en http://apps.who.int/iris/bitstream/10665/255627/1/WHO-NMH-PND-17.1-eng.pdf?ua=1
- De Benoist B, McLean E, Egli I, Congswewll M (eds.). Worldwide prevalence of anaemia 1993-2005. WHO Global Database on Anaemia. En: Organización Mundial de la Salud [en línea] [consultado el 17/02/2020]. Disponible en https://apps.who.int/iris/bitstream/handle/10665/43894/9789241596657_eng.pdf
- Sánchez JM, Yeste D, Marín A, Fernández M, Audí L, Carrascosa A. Evaluación de la anemia ferropénica en niños menores de 6 años de edad de diferentes etnias. Acta Pediatr Esp. 2015;73:120-5.
- Saunders NR, Parkin PC, Birken CS, Maguire JL, Borkhoff CM; TARGet Kids! Collaboration. Iron status of young children from immigrant families. Arch Dis Child. 2016;101:1130-6.
- Hayden GF. Skin diseases encountered in a pediatric clinic. A one-year prospective study. Am J Dis Child. 1985;139:36-8.
- Albares MP, Ramos JM, Belinchón I, Betlloch I, Pastor N, Botella R. Análisis de la demanda asistencial en dermatología de la población inmigrante. Gac Sanit. 2008;22:133-6.
- Cantarutti A, Donà D, Visentin F, Borgia E, Scamarcia A, Cantarutti L, et al. Epidemiology of frequently occurring skin diseases in italian children from 2006 to 2012: a retrospective, population-based study. Pediatr Dermatol. 2015;32:668-78.
- Pérez-Crespo M, Ramos-Rincón JM, Albares-Tendero MP, Betlloch-Más I. Estudio comparativo epidemiológico de la enfermedad cutánea en población infantil inmigrante y autóctona en Alicante. Actas Dermosifiliogr. 2014;105:394-400.
- Katsarou A, Armenaka M, Kosmadaki M, Lagogianni E, Vosynioti V, Tagka A, et al. Skin diseases in Greek and immigrant children in Athens. Int J Dermatol. 2012;51:173-7.
- Pérez-Crespo M, Ramos-Rincón JM, Albares-Tendero MP, Betlloch-Más I. Dermatoses in Latin American immigrant children seen in a universitary hospital of Spain. J Immigr Minor Health. 2016;18:16-20.
- Horii KA, Simon SD, Liu DY, Sharma V. Atopic dermatitis in children in the United States, 1997-2004: visit trends, patient and provider characteristics, and prescribing patterns. Pediatrics. 2007;120:e527-34.
- Revisió de la dimensió socioeconòmica de l’assignació de recursos de l’Atenció Primària. En: Agència d’Avaluació i Qualitat Sanitàries de Catalunya [en línea] [consultado el 17/02/2020]. Disponible en http://observatorisalut.gencat.cat/web/.content/minisite/observatorisalut/ossc_crisi_salut/Fitxers_crisi/Revisio_dimensio_socioeconomica_formula_241116.pdf