Vol. 19 - Num. 76
Originales
Aspectos socioculturales de la lactancia materna en niños mayores
José Ignacio Perales Martíneza, Beatriz Pina Marquésb
aPediatra. CS Calatayud Norte. Calatayud. Zaragoza. España.
bMatrona. Hospital Universitario Miguel Servet. Zaragoza. España.
Correspondencia: JI Perales. Correo electrónico: josiperales@hotmail.com
Cómo citar este artículo: Perales Martínez JI, Pina Marqués B. Aspectos socioculturales de la lactancia materna en niños mayores. Rev Pediatr Aten Primaria. 2017;19:337-44.
Publicado en Internet: 25-10-2017 - Número de visitas: 30101
Resumen
Introducción y objetivos: la lactancia materna por encima del año o “prolongada” es una práctica habitual en muchas culturas, aunque en países occidentales es poco frecuente. Nuestro objetivo es analizar, desde un punto de vista social, las experiencias de estas madres.
Material y métodos: encuesta a 35 madres que han mantenido o mantienen lactancia materna por encima del año de vida. Se investigan aspectos básicos de la misma. En una segunda parte valoramos al apoyo de los profesionales de la salud, la perspectiva social de la lactancia materna prolongada, así como los obstáculos que han aparecido.
Resultados: el 60% de las madres estaba amamantando, siendo la media de edad del hijo de 32,5 meses. La mayoría querían mantenerla hasta la decisión del hijo. Todas tenían claro comenzarla y volverían a elegirla como primera opción. En caso de dudas, los principales soportes han resultado los profesionales de la salud (58%) y los grupos de apoyo (42%). Hasta el 65,7% refiere haber podido contar con ayuda de profesionales, siendo la matrona y el pediatra los mejor valorados. La mayoría refiere gran satisfacción con la lactancia materna prolongada, pero hasta el 50% indican algún grado de rechazo social. La familia, amigos y compañeros de trabajo han supuesto obstáculos en algún momento para actuar de forma espontánea.
Conclusiones: el grado de satisfacción y confianza de estas madres es elevado. Los profesionales de salud juegan un papel importante. La propia sociedad todavía mantiene algunos prejuicios que obstaculizan y limitan la generalización de esta opción.
Palabras clave
● Lactancia maternaINTRODUCCIÓN
Los beneficios de la leche materna, tanto para la madre como para el niño, son ampliamente reconocidos1. En niños amamantados existe menor riesgo de otitis media, infecciones respiratorias, diarrea y atopias. En las madres favorece la pérdida de peso, disminuye el riesgo de anemia y a largo plazo disminuye el riesgo de osteoporosis y cánceres de mama y ovario. En conjunto, tiene un gran impacto psicológico –mediante el refuerzo del vínculo madre-hijo–, económico y social2. La mayoría de los trabajos demuestran estas afirmaciones, pero se limitan a niños menores de un año, por lo que se podría llegar a pensar que únicamente es necesaria durante la primera infancia. Sin embargo, estos efectos beneficiosos permanecen en el tiempo y se adaptan a cada momento. En consecuencia, las principales asociaciones científicas, como la Organización Mundial de la Salud (OMS), Unicef, la Asociación Española de Pediatría (AEP) o American Academy of Pediatrics (AAP) entre otras, recomiendan que la lactancia materna (LM) sea el único aporte de alimento durante los primeros 6 meses de vida y complementarla posteriormente con otros, al menos hasta los 12-24 meses, pudiendo mantenerla tanto tiempo como madre e hijo deseen3-5.
La LM por encima del año de vida o LM prolongada (LMP) es una práctica habitual en muchas culturas, pese a que en los países occidentales es poco frecuente. En ocasiones, sobre todo en niños más mayores, no deja de llamar la atención e incluso provocar cierto rechazo en la sociedad6, los profesionales sanitarios o la propia familia7. Desde el Comité de LM de la AEP indican que el término LMP puede llevar a confusión al considerarse algo que está más allá de las recomendaciones. Por este motivo, algunos autores defienden hablar únicamente de LM, sin más apellidos, con el fin de normalizar esta situación.
Una cita bíblica del segundo libro de los Macabeos dice: “Hijo, ten compasión de mí, que te llevé en el seno por nueve meses, te amamanté por tres años y te crie y eduqué hasta la edad que tienes”8. Esta referencia histórica sirve de ejemplo para contemplar cómo los niños han mantenido la LM por encima de los dos y los tres años de forma habitual desde tiempos inmemoriales.
Sin embargo, la modernización de la medicina en el siglo XX ha reflejado un progresivo descenso de las tasas de LM en todo el mundo desarrollado. Medidas como la adopción de métodos calorimétricos para la alimentación infantil o el desarrollo de la bacteriología para avanzar en una “campaña de leche limpia” no hicieron otra cosa que promocionar la alimentación con sucedáneos. En 1950, los pediatras recomendaron la introducción de vegetales en la dieta a los cuatro meses de edad, interfiriendo en la LM de forma inevitable. A todo este asesoramiento profesional moderno tenemos que añadir la llegada de intereses comerciales, que también han sido un importante impulso para la alimentación de “fórmula” o incorrectamente llamada “lactancia artificial”. En EE. UU., por ejemplo, se comenzaron a poner algunas contraindicaciones para las nodrizas, excluyendo a las drogadictas y a las que tenían evidencia de infección por viruela, y sugiriendo que debían tener “buenos pezones”. A veces se incluían algunos requisitos un tanto frívolos, como por ejemplo el color del cabello. Con este descenso de LM reaparecieron las deficiencias nutricionales con mayor morbilidad, como escorbuto y raquitismo. Asimismo, el censo estadounidense reveló que los niños amamantados tenían una tasa de mortalidad un 40% menor que sus compañeros alimentados con sucedáneos9.
Teniendo en cuenta estas referencias históricas y sabiendo cuál es la postura mayoritaria de la sociedad actual, nos hemos planteado el trabajo con un doble objetivo:
- Observar el papel que juegan los profesionales de la salud en la LM y cuál es su posición a la hora de ayudar y fomentar la LMP.
- Analizar la perspectiva sociocultural de las madres que siguen amamantando a los niños más mayores. Para ello evaluamos el grado de satisfacción personal y valoramos las dificultades que surgen en los distintos ámbitos de su vida.
MATERIAL Y MÉTODOS
Se ha encuestado a 35 mujeres que han realizado o están realizando una LM superior a los 12 meses. El cuestionario consta de tres apartados:
- Datos personales maternos: se han registrado únicamente la edad y el número de hijos.
- Experiencias sobre su LM: en primer lugar, se investiga si mantienen la LM actualmente y las experiencias previas con la misma. También hemos preguntado sobre la intención inicial respecto a la duración de la LM y hasta cuándo querían mantenerla en la actualidad. A continuación se valoran los antecedentes personales del hijo al que se refieren (sexo, peso de recién nacido, edad gestacional, tipo de parto, si existió sufrimiento fetal, la posibilidad de piel con piel tras el nacimiento y el tiempo transcurrido hasta el inicio de la LM). Otros aspectos reflejados son: LM exclusiva los primeros seis meses, el colecho o experiencias de LM en el embarazo o en tándem.
- Aspectos socioculturales sobre LM y LMP: experiencias de las madres en su entorno social. Lugar donde acuden en caso de dudas o problemas relacionados con la LM. Nivel de ayuda por parte de los profesionales de la salud, mediante puntuación numérica del 1 al 5. Por último, las experiencias sociales que han tenido estas madres respecto a la LMP en su propio ámbito. Para ello, se pregunta, entre otras cosas, por el grado de satisfacción (puntación del 1 al 5), si han vivido algún tipo de rechazo u obstáculo, o si han tenido que ocultar la LMP en algún momento. A su vez, mediante puntuación numérica del 1 al 5, cómo interpretan las madres que se percibe su LMP en los diferentes ámbitos de su vida cotidiana.
La muestra se ha obtenido de madres con un nivel sociocultural similar y mayoritariamente relacionadas con el ambiente sanitario, lo que indica que el conocimiento y el grado de aceptación de la LM es elevado. El cuestionario se ha remitido por correo electrónico y ha sido realizado de forma individual y anónima.
Todas las variables han sido recogidas mediante el programa SPSS versión 15.0 y se ha realizado un estudio descriptivo.
RESULTADOS
Descripción de la muestra y características de los niños amamantados
Se ha realizado la encuesta a 35 madres con una edad media de 34,59 ± 8,41 años (rango: 27-48 años). El número de hijos medio ha resultado 1,8 ± 0,93. La mediana de edad del hijo sobre el que se refería la encuesta ha sido 32,5 meses, rango intercuartil 14-72.
Los aspectos perinatales más relevantes son: el 65,7% son varones. La tasa de cesárea se sitúa en el 31,4%, con un 58,3% de partos eutócicos. El 85,7% resultaron gestaciones a término (> 37 semanas). Únicamente apareció sufrimiento fetal en el 8,5% de los casos y ninguno precisó reanimación avanzada. El inicio de LM ha sido del 80% en las primeras tres horas (el 54% en la primera hora de vida). También se valoran aspectos relevantes como el contacto piel con piel (CPP) al nacimiento, la alimentación con LM exclusiva durante los primeros seis meses, así como la práctica habitual del colecho en las primeras semanas de vida, obteniendo porcentajes del 91,4, 97,1 y 54,3% respectivamente (Tabla 1).
| Tabla 1. Aspectos perinatales más relevantes de nuestros niños amamantados | |
|---|---|
| Sexo | Varón 65,7%, mujer 34,3% |
| Tipo de parto | Cesárea 31,4%, eutócico 58,3%, instrumental 10,3% |
| Inicio de la lactancia materna | 80% primeras 3 horas, 54% primera hora, 5,7% más de 6 horas |
| Lactancia materna exclusiva 6 meses | 91,4% |
| Colecho | 97,1% |
| Contacto piel con piel | 54,3% |

Aspectos iniciales de la lactancia materna
El 60% de las madres estaban amamantando en el momento del estudio, mientras que el 57,1% tenía experiencia previa con la LM.
Todas tenían claro comenzar con LM y volverían a elegirla como primera opción. En cuanto al momento de retirarla, el 85,7% quiere mantenerla hasta que el propio niño decida. Otros datos de interés son las experiencias de LM durante el embarazo y en tándem, cifradas en un 34,2% y 20% respectivamente.
Aspectos socioculturales de la lactancia materna y de la lactancia materna prolongada
Los principales soportes para resolver las dudas en el curso de la LM, tanto en la instauración como en el mantenimiento, han resultado los profesionales de la salud (58%) y los grupos de apoyo (42%).
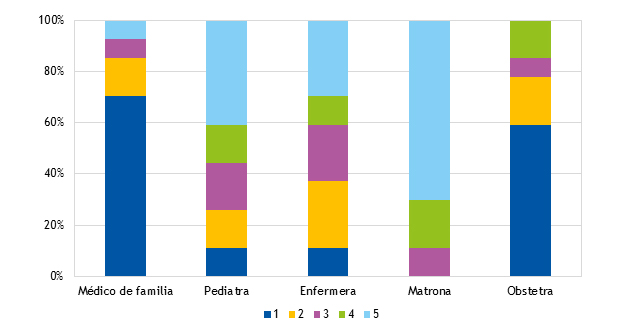
Respecto al nivel de ayuda en los distintos profesionales de la salud, el 65,7% de las madres refieren haber podido contar con algún tipo de apoyo de este colectivo. Los mejor valorados resultan la matrona (4,39 ± 0,69) y el pediatra (3,28 ± 1,44) y los que menos el médico de familia (1,27 ± 1,15) y el obstetra (1,58 ± 1,12) (Fig. 1).
Para completar el estudio, se ha puesto especial interés en la LM a partir del año de vida, incorrectamente llamada LMP. Se evalúan aspectos relevantes a nivel social, con el objetivo de valorar los sentimientos y preocupaciones que tienen las madres en diferentes entornos. Es importante destacar que en el 50% de las madres encuestadas, el mantenimiento de la LM por encima de los 12 meses resulta habitual en su entorno. El nivel de satisfacción con esta experiencia en muy elevado (4,37 ± 0,51 puntos, máximo 5), pero hasta el 48,6% indican algún grado de rechazo social. El 51,4% han tenido algún obstáculo, siendo familia y amigos los más frecuentes. Además, el 45,7% indica haberla tenido que ocultar en algún momento, sobre todo ante familiares o compañeros de trabajo.
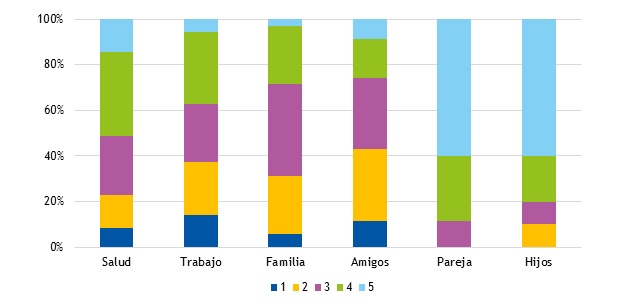
En la Fig. 2 se expresa cómo interpretan las madres que se percibe su LMP en los diferentes ámbitos de su vida cotidiana. La pareja (4,29 ± 0,70) y los otros hijos (4,10 ± 1,03) son los mejor valorados y la familia (2,29 ± 1,16), amigos (2,42 ± 1,17) y compañeros de trabajo (2,36 ± 0,78) reciben puntuaciones más bajas.
| Figura 2. Percepción de la lactancia materna prolongada en los distintos ámbitos de la vida |
|---|
 |

DISCUSIÓN
Duración de la lactancia materna, edad del destete
En las sociedades más tradicionales, que no tienen extendido el uso de fórmulas artificiales de leche, la duración media de LM es de tres a cuatro años, según los textos etnográficos10. En estos pueblos, con escasos contactos externos, la edad del destete es variable, oscilando desde los cuatro meses en los hotentotes africanos hasta los cinco años en tribus hawaianas y los siete o más en ciertas poblaciones esquimales11. En el año 1989, de un total de 46 sociedades no industrializadas en el mundo, el destete se situaba entre los dos y los tres años en el 75%, siendo a los 18 meses en el resto; únicamente en un país la media era de seis meses10.
Las últimas recomendaciones indican mantener la lactancia tanto tiempo como madre e hijo deseen, al igual que el 85,7% de nuestras madres encuestadas. Cuando una mujer cree que ha llegado el momento de destetar, se aconseja no hacerlo bruscamente ni con engaños. La mejor estrategia es la del destete gradual, sin ofrecer ni negar el pecho, pudiendo negociar las condiciones con el niño (por ejemplo, solo pecho en ciertos lugares o situaciones, o con una duración limitada de la toma). Durante la etapa del destete es importante ofrecer alternativas a la necesidad de contacto del niño, ya que la relación que se establece a través de la lactancia es un vínculo muy estrecho que debe ir reorientándose paulatinamente12.
Inicio y mantenimiento de la lactancia materna en España
Pese a los conocidos beneficios y a los esfuerzos en su promoción, los porcentajes de LM en nuestro medio han sido bajos durante las últimas décadas. Los datos de la Encuesta Nacional de Salud (ENS) del Ministerio de Sanidad y Consumo exponen una tasa de LM exclusiva muy pobre a los seis meses, con un 15 y 21% en los años 1995 y 1997 respectivamente13. Uno de los estudios más amplios sobre prevalencia de LM realizados en España fue el impulsado por el Comité de LM de la AEP en 1997, en el que se realizó una encuesta transversal en 18 provincias. La mediana de duración de LM en los más de 10 000 cuestionarios registrados fue de 3,0 meses (intervalo de confianza del 95% [IC 95]: 2,93 a 3,07). La tasa de LM (exclusiva más mixta) fue del 77,6% al primer mes de vida, el 54,6% a los tres meses, el 25% a los seis meses y el 7% al año de vida. Quizá lo más llamativo fue que únicamente el 55% de las madres superaron los tres meses dando alguna toma de pecho14. Otros estudios en distintas comunidades autónomas revelan porcentajes muy similares15,16. Según los últimos datos publicados por el Instituto Nacional de Estadística en la ENS de 2011, la prevalencia de LM exclusiva en España es de 63% a las seis semanas y 26% a los seis meses17. Parece observarse una discreta mejoría, sobre todo en el mantenimiento de la LM, en los últimos 15 años en el territorio español. Esta mejoría se representa todavía mejor en Aragón, donde las cifras superan la media nacional, tras la puesta en marcha del programa IHAN en el Hospital de Alcañiz, perdurando la LM en un 41,8% a los seis meses y en un 12,2% al año de vida, prácticamente el doble que en estudios más antiguos18. El estudio CALINA intentó evaluar la prevalencia de LM mediante el seguimiento longitudinal durante 12 meses a 1602 lactantes nacidos entre marzo de 2009 y marzo de 2010. Los autores indicaron que el mantenimiento de la LM en conjunto (exclusiva más mixta) fue del 82,5% al mes de vida, el 71,8% al tercero, el 54,3% al sexto y el 27,8% al año19. En Zaragoza, en una revisión retrospectiva de 550 madres e hijos nacidos entre 2010-2012 y controlados durante 12 meses, la duración media de la LM exclusiva y total fue de 2,5 y 5,1 meses respectivamente. Las tasas de LM se mantuvieron elevadas, aunque algo inferiores al estudio CALINA: el 74% al mes de vida, el 40,7% al sexto y el 14,2% al año. Los factores que más influyeron en el descenso de las tasas de LM fueron: las dificultades en su instauración en el primer mes y la incorporación de la madre al mundo laboral entre el cuarto y sexto mes20.
Beneficios y riesgos de la LM en niños mayores
La leche materna no pierde sus propiedades con el paso del tiempo21. A partir del primer año de lactancia, la cantidad de grasa en la leche aumenta con respecto a los primeros meses22, resultando un alimento completo y nutritivo, que cubre aproximadamente un tercio de las necesidades calóricas y proteicas diarias (a veces más, sobre todo durante periodos de enfermedad), proporcionando además una cantidad muy importante de vitaminas y minerales. A su vez, los beneficios inmunológicos de la leche materna se siguen manteniendo, con una menor incidencia de infecciones para su edad respecto a los que no son amamantados. Estos beneficios no solo se observan a corto plazo, sino años después del destete, ya que se ha observado una menor incidencia de ciertos tipos de cáncer (leucemia), enfermedades metabólicas y autoinmunes (como la diabetes tipo 1)23,24. Otro estudio ha constatado un mayor desarrollo intelectual a mayor tiempo y exclusividad de la LM, efecto que permanece durante años y que incluso puede llevar a alcanzar un mayor nivel de estudios y de ingresos económicos en la vida adulta25. Numerosos trabajos relacionan la duración de la LM con un mejor desarrollo emocional y psicosocial del niño26. Por último, se han descrito múltiples ventajas para la madre que amamanta, como menor riesgo de diabetes tipo 2, cáncer de mama, cáncer de ovario, hipertensión e infarto de miocardio cuanto mayor sea el tiempo total de lactancia.
En cuanto a los riesgos, no se han publicado riesgos físicos ni psicológicos en niños que toman pecho por encima de los 2-3 años de edad. Tampoco se ha encontrado relación entre LMP y malnutrición en países en desarrollo27 o con la caries infantil.
La LM en el embarazo (el 34,2% en nuestro estudio), si es el deseo de la madre, no conlleva ningún riesgo demostrado, aunque hay que individualizar y valorar el destete en caso de amenaza de aborto o parto prematuro, así como en otras situaciones especiales28. La LM en tándem (el 20% en nuestro estudio) es posible, ya que la producción de leche se adapta según la demanda. El principal problema puede ser la sobrecarga materna ante las demandas de ambos niños y los sentimientos encontrados que le puede producir amamantar al mayor29.
Sin duda, el mayor problema de la LM más allá del año de edad es el rechazo social y profesional por prejuicios o desconocimiento de la evidencia científica actual. Este hecho queda completamente reflejado en esta encuesta. Inicialmente, hay que destacar un dato relevante: el 58% de las madres encuestadas acuden a los profesionales de la salud para pedir ayuda/consejo. De esta manera, debemos tomar conciencia del papel fundamental que jugamos como profesionales de la salud y por ello, es nuestro deber y obligación actualizarnos en LM para que cada familia y cada madre tome decisiones informadas. Si su deseo es mantener la LM, nuestro deber es apoyarlas en su decisión y aportar herramientas para superar las dificultades que puedan surgir. Resumiendo, los profesionales de la salud debemos aportar información y respeto. En los datos presentados, únicamente la matrona y el pediatra han obtenido buenas puntuaciones a la hora de prestar ayuda a las madres, por lo que hay que seguir mejorando en este sentido. Además, el otro 42% acudieron a los grupos de apoyo a la LM, estrategia que también se ha demostrado útil para apoyar y fortalecer la decisión de amamantar por encima de los 12-24 meses30.
Resulta muy importante aclarar este tipo de dudas, porque al final el grado de satisfacción de las encuestadas respecto a la LMP ha sido muy elevado y relatan la experiencia como muy positiva. Además, todas las madres volverían a elegir la LM como primera opción.
Hay que destacar cifras demasiado elevadas respecto a diversos conflictos sociales, ya que aproximadamente la mitad de las madres encuestadas refieren algún grado de rechazo social, haber tenido obstáculos para la práctica de LMP o incluso tener que ocultarla en algún momento. Los entornos más hostiles en este sentido siguen siendo los clásicos, como familiares, amigos o compañeros de trabajo.
CONCLUSIONES
La LM sigue siendo el mejor y más completo alimento para el recién nacido, pero también es altamente beneficioso a partir del año de vida, sin conllevar ningún riesgo. El destete debería producirse cuando madre e hijo deseen. Las madres se sienten altamente satisfechas manteniendo la LM a sus hijos mayores. Los profesionales de la salud somos una de las principales fuentes de apoyo y nuestra obligación es informar y respetar. Todavía aparecen numerosos prejuicios respecto a las madres que amamantan a sus hijos más mayores, que les impiden llevarla a cabo con mayor naturalidad.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS
AAP: American Academy of Pediatrics • AEP: Asociación Española de Pediatría • CPP: contacto piel con piel • IC 95: intervalo de confianza del 95% • LM: lactancia materna • LMP: lactancia materna prolongada • OMS: Organización Mundial de la Salud.
BIBLIOGRAFÍA
- Ip S, Chung M, Raman G, Chew P, Magula N, DeVine D, et al. Breastfeeding and maternal and infant health outcomes in developed countries. Evid Rep Technol Assess (Full Rep). 2007;153:1-186.
- Gartner LM, Morton J, Lawrence RA, Naylor AJ, O’Hare D, Schanler RJ, et al. Breastfeeding and the use of human milk. Pediatrics. 2005;115:496-506.
- Nutrición del lactante y del niño pequeño. Estrategia mundial para la alimentación del lactante y del niño pequeño. Informe de la Secretaría. 55.ª Asamblea Mundial de la Salud. En: Organización Mundial de la Salud [en línea] [consultado el 24/10/2017]. Disponible en http://apps.who.int/iris/bitstream/10665/81907/1/sa5515.pdf
- Innocenti Declaration on the Protection, Promotion and Support of Breastfeeding. En: Unicef [en línea] [consultado el 24/10/2017]. Disponible en www.unicef.org/programme/breastfeeding/innocenti.htm
- Comité de Lactancia Materna de la AEP. Recomendaciones sobre lactancia materna. En: Asociación Española de Pediatría [en línea] [consultado el 24/10/2017]. Disponible en www.aeped.es/sites/default/files/recomendaciones_lm_26-1-2012.pdf
- Dowling S, Brown A. An exploration of the experiences of mothers who breastfeed long-term: what are the issues and why does it matter? Breastfeed Med. 2013;8:45-52.
- Cockerham-Colas L, Geer L, Benker K, Joseph MA. Exploring and influencing the knowledge and attitudes of health professionals towards extended breastfeeding. Breastfeed Med. 2012;7:143-50.
- Paricio JM. Lactancia prolongada… ¿Hasta cuándo es normal? Perspectiva histórico-antropológica. VII Congreso español de Lactancia Materna. Madrid; 2014.
- Piovanetti Y. Breastfeeding beyond 12 months: an historical perspective. Pediatr Clin North Am. 2001;48:199-206.
- Stuart-Macadm P, Dettwyker KA. Breastfeeding. Biocultural perspectives. Nueva York: Ed. Aldine de Gruyter; 1995.
- Wickes IG. A history of infant feeding. I. Primitive peoples; ancient works; Renaissance writers. Arch Dis Child. 1953;28:151-8.
- Gribble KD. “As good as chocolate” and “better than ice cream”: how toddler, and older, breastfeeders experience breastfeeding. Early Child Dev Care. 2009;179:1067-82.
- Encuesta sobre discapacidades, deficiencias y estado de salud 1999. En: Instituto Nacional de Estadística [en línea] [consultado el 24/10/2017]. Disponible en www.ine.es/dyngs/INEbase/es/operacion.htm?c=Estadistica_C&cid=1254736176782&menu=resultados&idp=1254735573175)
- García Vera C, Martín Calama J. Lactancia materna en España. Resultado de una encuesta de ámbito estatal. Rev Pediatr Aten Primaria. 2000;2:373-87.
- Ortega JA, Pastor E, Martínez I, Bosch V, Quesada J, Hernández F, et al. Proyecto Malama: medio ambiente y lactancia materna. An Pediatr (Barc). 2008;68:447-53.
- González M, Toledano J. La lactancia materna en nuestro medio: análisis de la situación. Acta Pediatr Esp. 2007;65:123-5.
- Ministerio de Sanidad, Servicios Sociales e Igualdad. Encuesta Nacional de Salud 2011. En: Instituto Nacional de Estadística [en línea] [consultado el 24/10/2017]. Disponible en www.ine.es/prensa/np770.pdf
- Guerrero C, Garafulla J, Lozano D, García C, Bielsa A. Estudio lactancia en Área Hospital de Alcañiz. ¿Merece la pena poner en práctica los diez pasos de la Iniciativa Hospital Amigo de los Niños en un hospital comarcal? Bol Pediatr Arag Rioj Sor. 2006;36:20-6.
- Oves B, Escartín L, Samper MP, Cuadrón L, Álvarez ML, Lasarte JJ, et al. Inmigración y factores asociados con la lactancia materna. Estudio CALINA. An Pediatr (Barc). 2014;81:32-8.
- Giménez V, Jimeno B, Valles MD, Sanz E. Prevalencia de la lactancia materna en un centro de salud de Zaragoza (España). Factores sociosanitarios que la condicionan. Rev Pediatr Aten Primaria. 2015;17:17-26.
- Boediman D, Ismail D, Iman S, Ismangoen, Ismadi SD. Composition of breast milk beyond one year. J Trop Pediatr Environ Child Health. 1979;25:107-10.
- Mandel D, Lubetzky R, Dollberg S, Barak S, Mimouni FB. Fat and energy contents of expressed human breast milk in prolonged lactation. Pediatrics. 2005;116:e432-5.
- Amitay EL, Keinan-Boker L. Breastfeeding and childhood leukemia incidence: a meta-analysis and systematic review. JAMA Pediatr. 2015;169:e151025.
- Patelarou E, Girvalaki C, Brokalaki H, Patelarou A, Androulaki Z, Vardavas C. Current evidence on the associations of breastfeeding, infant formula, and cow’s milk introduction with type 1 diabetes mellitus: a systematic review. Nutr Rev. 2012;70:509-19.
- Belfort MB, Rifas-Shiman SL, Kleinman KP, Guthrie LB, Bellinger DC, Taveras EM, et al. Infant feeding and childhood cognition at ages 3 and 7 years: effects of breastfeeding duration and exclusivity. JAMA Pediatr. 2013;167:836-44.
- Lawrence RA. Supporting breastfeeding/early childhood social and emotion development. En: Encyclopedia on Early Childhood Development [en línea] [consultado el 24/10/2017]. Disponible en www.child-encyclopedia.com/breastfeeding/according-experts/supporting-breastfeedingearly-childhood-social-and-emotion
- Cousens S, Nacro B, Curtis V, Kanki B, Tall F, Traore E, et al. Prolonged breast-feeding: no association with increased risk of clinical malnutrition in young children in Burkina Faso. Bull World Health Organ. 1993;71:713-22.
- Cetin I, Assandro P, Massari M, Sagone A, Gennaretti R, Donzelli G, et al. Breastfeeding during pregnancy: position paper of the Italian Society of Perinatal Medicine and the Task Force on Breastfeeding, Ministry of Health, Italy. J Hum Lact. 2014;30:20-7.
- Bryant T. Tandem nursing: a review and guidelines. Int J Childbirth Educ. 2012;27:84-8.
- Thomson G, Crossland N, Dykes F. Giving me hope: women’s reflections on a breastfeeding peer support service. Matern Child Nutr. 2012;8:340-53.