Vol. 18 - Num. 71
Originales
Déficit de vitamina D: situación en un centro urbano de la costa mediterránea
Ramona Martín Martína, Antoni Collado Cucòb
aServicio de Pediatría. ABS Marià Fortuny. Reus. Tarragona. España.
bMédico Adjunto. CAP Riudoms. Riudoms. Tarragona. España.
Correspondencia: R Martín. Correo electrónico: rmartin@grupsagessa.com
Cómo citar este artículo: Martín Martín R, Collado Cucò A. Déficit de vitamina D: situación en un centro urbano de la costa mediterránea. Rev Pediatr Aten Primaria. 2016;18:213-8.
Publicado en Internet: 08-09-2016 - Número de visitas: 19478
Resumen
Introducción: en los últimos años han surgido propuestas diferentes sobre la necesidad de suplementar la dieta con vitamina D. Estamos asistiendo a un repunte del déficit relacionado con situaciones que aumentan el riesgo: prematuridad, lactancia materna exclusiva prolongada, personas de piel oscura, baja exposición solar.
Objetivo: averiguar si el déficit de vitamina D es un problema frecuente en los niños de un núcleo urbano de la costa mediterránea.
Material y métodos: estudio observacional. Determinación de la vitamina D en niños de 0 a 15 años, durante un periodo de 18 meses, de un cupo urbano de Atención Primaria, coincidiendo con una extracción sanguínea por cualquier causa. Análisis estadístico: estadística descriptiva e inferencial, análisis de conformidad de la muestra.
Resultados: se realizaron 145 determinaciones. Un 42,1% fueron niños inmigrantes y un 57,9% nacionales. Del total de la muestra, el 37,9% presentaban algún grado de déficit de vitamina D: leve el 67,3%, moderado el 21,8% y grave el 10,9%. El 30% de los varones y el 44% de las mujeres tenían déficit. Un 20% de los niños autóctonos presentaba déficit de vitamina D frente al 62% de los niños inmigrantes (p < 0,001%). Entre los niños nacionales tenía déficit el 15% de los varones y el 24% de las mujeres; entre los inmigrantes el 45% de los varones y el 82% de las mujeres.
Conclusiones: el déficit de vitamina D es muy frecuente en nuestro medio. Los inmigrantes de sexo femenino, sobre todo si son adolescentes, son los que tienen más probabilidad de presentarlo.
Palabras clave
● Déficit de vitamina D ● Vitamina DINTRODUCCIÓN
En los últimos años han surgido propuestas diferentes en la comunidad pediátrica sobre la necesidad de suplementar o no la dieta con vitamina D (VD). La controversia se explica por la falta de un marcador bioquímico y de criterios universales que definan el estado óptimo de VD y su deficiencia. La falta de estandarización de los métodos de medida y los distintos umbrales de normalidad utilizados en investigación son responsables de que las prevalencias descritas sean muy variables. Además, hay variables que son difíciles de evaluar: la síntesis endógena dependiente de la exposición solar y el consumo de alimentos enriquecidos con VD. Aun con estas limitaciones, los hallazgos recientes sugieren que la hipovitaminosis D puede afectar cada vez a más niños de todas las edades.
Las recomendaciones de suplementar varían según la entidad y el país. Algunos han tenido en cuenta su influencia sobre el tejido esquelético y el desarrollo de enfermedades crónicas1.
Recientemente se ha definido nuevas funciones de la VD, como la prevención del cáncer, su influencia en el desarrollo de enfermedades cardiovasculares e hipertensión arterial, diabetes, síndrome metabólico, respuesta inmunitaria, estados neuropsicológicos patológicos y la salud reproductiva1-5.
Aunque se consideraba que el déficit de VD en los países desarrollados era muy bajo, estamos asistiendo a un repunte relacionado con situaciones que aumentan el riesgo del déficit: prematuridad, lactancia materna exclusiva prolongada, inmigración de etnias de piel oscura, falta de exposición solar por motivos culturales, religiosos o cambios en el estilo de vida1.
El objetivo del estudio es conocer la frecuencia del déficit de VD en los niños de un núcleo urbano de un país desarrollado pero en crisis económica, de la costa mediterránea.
MATERIAL Y MÉTODOS
Se analizan los valores de vitamina D (25-OH-vitamina D) durante un periodo de 18 meses, entre el 1 de febrero de 2013 y el 31 de julio de 2014, de todos los niños de 0 a 15 años de un cupo de Pediatría de Atención Primaria, situado en un núcleo urbano de la costa mediterránea de 100 000 habitantes a los que se les realiza una analítica sanguínea por cualquier causa.
Se asume como nivel de corte para establecer el déficit de VD en niños el de 20 ng/ml, por ser el más aceptado por la comunidad científica en los últimos años. Siguiendo este mismo criterio, los niveles de 25-OH-vitamina D se clasifican como: óptimo (30-80 ng/ml), insuficiente (20-30 ng/ml), déficit leve (10-20 ng/ml), déficit moderado (5-10 ng/ml), déficit grave (< 5 ng/ml)6-8.
Se realizó un análisis estadístico: estadística descriptiva (distribución de frecuencias y medias de posición y dispersión), estadística inferencial (comparación de medias, análisis de la varianza y regresión logística multivariante) y análisis de conformidad de la muestra.
RESULTADOS
Se realizaron 145 determinaciones de vitamina D (54,5% mujeres y 45,5% varones). Un 42,1% eran niños inmigrantes (61) y un 57,9% nacionales (84). Esta distribución no difiere, significativamente de la encontrada en el conjunto de la población diana (37% de inmigrantes de un total de 1360 niños). La distribución por procedencia de los niños inmigrantes fue la siguiente: Marruecos, un 78,7%; Rumanía, un 9,8%; Latinoamérica un 6,4% y Asia un 4,8%.
Del total de la muestra, el 37,9% presentaban algún grado de déficit de vitamina D: leve el 67,3%, moderado el 21,8% y grave el 10,9%.
Los valores de calcio y fósforo de todos los niños fueron normales. Los valores de fosfatasa alcalina estaban elevados en el 25,5% de los casos sin relación con el nivel de déficit (diferencia no estadísticamente significativa; p > 0,1). Un 11% presentaba síntomas inespecíficos (astenia, anorexia o dolores musculares), casos sin relación con el nivel de déficit (diferencia estadísticamente no significativa; p > 0,1).
Al analizar la totalidad de la muestra por sexos, el 30% de los varones y el 44% de las mujeres presentaban déficit de vitamina (p > 0,05).
Al analizar la muestra según el origen, el 20% de los niños españoles tenía déficit de vitamina D frente al 62% de los niños inmigrantes, con una diferencia estadísticamente significativa (p < 0,001%).
Entre los niños nacionales presentaron déficit el 15% de los varones y el 24% de las mujeres, sin diferencias estadísticas significativas (p > 0,1). Entre los niños inmigrantes, lo tenían el 45% del sexo masculino y el 82% del femenino (p = 0,02).
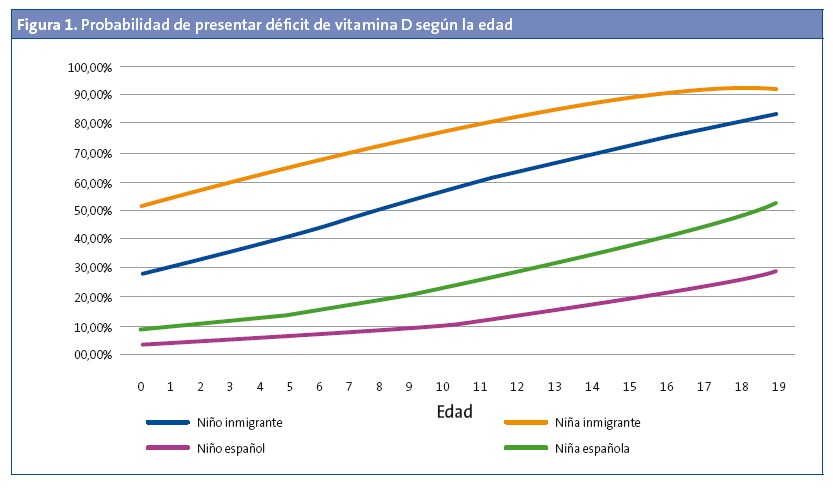
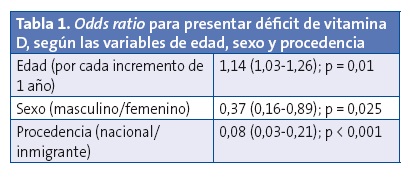
Respecto a la distribución por grupos de edad, el 26% de los niños menores de cinco años presentaba déficit frente al 38% de los niños entre cinco y diez años. El grupo con mayor déficit, con un 44%, se situó entre los 11 y 15 años. En la Fig. 1 se puede observar la probabilidad de padecer déficit de vitamina D según la edad y en la Tabla 1 se muestra la odds ratio para las diferentes variables.
DISCUSIÓN
Hemos realizado un estudio de corte para evidenciar la existencia o no de un problema, guiados por la literatura científica de los últimos años, que sugiere que este déficit vitamínico está repuntando de nuevo. Tras la mejora de la alimentación a partir de los años cincuenta y el alto número de días soleados anuales, en nuestro país se consideraba el déficit de VD como un problema prácticamente erradicado. Nuestro estudio no permite establecer ninguna relación de causa-efecto, pero teniendo en cuenta lo sabido sobre los factores que influyen en la carencia y nuestros conocimientos sobre los hábitos de la población que atendemos, podríamos tratar de clarificar los factores que han contribuido a nuestros resultados.
Para los niños menores de un año se ha establecido unas necesidades de 400 U/día. Por encima de esa edad, 600 U/día9. Estas cifras son difíciles de conseguir exclusivamente con la dieta, lo que ha llevado a muchas sociedades científicas a emitir recomendaciones de suplementar.
Según las últimas recomendaciones de la Asociación Americana de Pediatría7, el grupo de trabajo PrevInfad1,10 y el Comité de Lactancia Materna de la Asociación Española de Pediatría9, se debería suplementar la dieta de lactantes menores de un año alimentados al pecho o con fórmula cuando su consumo no alcance un litro diario o la cantidad que según su contenido en VD no llegue a 400 UI; después del año, cuando la ingesta de productos lácteos y alimentos suplementados sea insuficiente, y en niños con niveles de 25-OH-vitamina D inferiores a 20 ng/ml hasta su normalización9.
Desde el año 2007, la Sociedad Pediátrica de Canadá recomienda una dosis de vitamina D de 400 U/día para todos los niños durante su primer año de vida, elevando la dosis a 800 U/día en invierno en aquellos niños que vivan en latitudes por encima de 55° Norte y entre las latitudes 40° y 55° Norte si presentan algún otro factor de riesgo de déficit11.
Los niveles plasmáticos de VD varían según el tiempo de radiación solar, las horas del día, la latitud, altitud y estación del año, la edad, la pigmentación de la piel, la superficie corporal expuesta y la aplicación de protectores solares. El aporte a través de la dieta y otros factores también pueden modificarlos (Tabla 2)10.

Pocos alimentos incluyen VD entre sus componentes. Principalmente productos lácteos. Los huevos y algunos pescados azules tienen cantidades significativas, aunque varían de una especie a otra, de un tejido a otro y en las diferentes épocas del año. Pero la dieta solo representa el 10% de los niveles plasmáticos que pueden alcanzarse frente al 90% que aporta la síntesis cutánea.
La lactancia materna aporta una cantidad variable, estimada entre 25-136 U/litro, dependiendo de la alimentación y la exposición solar de la madre12. Las fórmulas infantiles adaptadas comercializadas en nuestro país están fortificadas y contienen 200 U por cada 300-500 ml. Serían necesarios más de dos litros de leche materna o uno de fórmula para alcanzar las 400 U/día12. En nuestro entorno, a partir de los 12 meses, en la población inmigrante y los 18-24 meses en la población autóctona, se introduce la leche de vaca entera (no fortificada) que contiene 240 U por litro. Serían necesarios 1600 ml al día de esta leche o 13 yogures para conseguir las 400 U/día recomendadas. Estos volúmenes de ingesta son difícilmente alcanzables. En nuestra población, el consumo de leche, yogures o productos lácteos está entre 500-1000 ml de leche al día y/o 1-2 yogures.
Existe suficiente evidencia científica que avala que la máxima producción de vitamina D se deriva de la síntesis cutánea y que con la exposición solar de 15 minutos al día sería suficiente para garantizar la necesidad diaria, pero ninguna revisión sistemática aclara si hay un nivel de exposición suficiente y seguro para mantener unos niveles óptimos. Sí está demostrado que su exclusión habitual es un riesgo de deficiencia. Teniendo esto en cuenta, algunas sociedades científicas y grupos de expertos han publicado recomendaciones. PrevInfad en 2010 refiere que, a los niños mayores de un año o adolescentes, de forma general, se les recomienda para la adecuada producción de VD la exposición diaria al sol de mediodía sin protección durante 10-15 minutos durante la primavera, el verano y el otoño (recomendación grado I)1,10. Si durante ese tiempo, en verano, se expusieran solo los brazos, manos y cara, alcanzaría para liberar 1000 unidades y, por tanto, estarían cubiertas las necesidades diarias10.
En la síntesis de VD por la piel, además de las horas de exposición solar, también influye la latitud geográfica. Hay un nivel umbral de luz UVB requerido para inducir la producción. El nivel de umbral ideal se sitúa en el ecuador y va disminuyendo en dirección norte, haciendo que no se alcance, generalmente durante el invierno, en áreas con latitudes por encima de los 40° Norte. Por encima de los 42° Norte en invierno la producción sería nula1. Algunas zonas del norte de España se sitúan por encima de estos 42° Norte.
Nuestra ciudad goza de un clima benigno que permite actividades al aire libre desde el mes de mayo al mes de octubre y una situación geográfica privilegiada a 10 kilómetros de la playa. Esto facilita que nuestra población pueda estar expuesta al sol los 15 minutos diarios que la recomendación sugiere durante esos meses. Pero nuestra situación geográfica, a 41° de latitud Norte, haría que la intensidad de la radiación no sea tan adecuada para la síntesis de la vitamina, sobre todo en invierno.
La población inmigrante representa un 37% del cupo y es mayoritariamente marroquí. Los niños y las niñas de nuestro centro visten mayoritariamente de forma occidental. En la adolescencia, las mujeres inician el uso de prendas de vestir tradicional y pañuelo dejando expuesta solo la piel de la cara y las manos. La forma de vestir podría explicar el mayor déficit de vitamina D en mujeres adolescentes, pero no en niñas y niños, que, en nuestro trabajo, es superior a la población nacional.
Esta población tiene una piel más oscura, sobre todo, la de origen bereber y sahariano, mayoritaria en nuestra población, frente a la de origen árabe. La pigmentación de la piel afecta al tiempo que se necesita para producir un cierto nivel de VD. Una persona de etnia indo-asiática requiere tres veces más tiempo de exposición solar para alcanzar el mismo nivel de VD que otra de piel clara y las personas de etnia afroamericana de piel muy pigmentada diez veces más1.
En los últimos años, tanto en los centros de Atención Primaria como en las Unidades de Dermatología de nuestro entorno, se ha hecho mucha promoción del uso de medidas de protección solar (uso de gorra, camisetas, sombrilla, cremas con filtro de protección solar, etc.) y actualmente están ampliamente implementadas. Por recomendación de las Unidades de Dermatología aconsejamos el uso de un filtro de protección solar con factor 30 o superior, ya sea físico o químico. Algunos estudios sugieren que el uso de filtros solares con factor de protección superior a 8 disminuye la síntesis de la vitamina D en la piel en más de un 95%1.
A pesar de que el tiempo de exposición solar de nuestra población puede ser suficiente la mayor parte del año, presenta altos índices de déficit vitamínico. La dieta no ayuda a paliar el problema, ya que el consumo de lácteos, aunque adecuado en volumen, se realiza con productos lácteos no fortificados, ya que en nuestro entorno el consumo de fórmulas de crecimiento (1-3 años) que llevan suplementación estaba poco extendido y ha disminuido con la crisis económica.
A la vista de nuestros resultados, las características de nuestra población, el contenido en vitamina D de los productos lácteos consumidos y nuestra situación geográfica, podríamos plantearnos recomendar suplementos de VD como estrategia nutricional para evitar o reducir dicha carencia, dada la escasez de efectos adversos de los suplementos en las dosis recomendadas7. Otra opción sería aumentar la ingesta de alimentos fortificados, pero en nuestro país esta medida tendría una influencia casi anecdótica por el escaso número de este tipo de alimentos que se pueden encontrar en el mercado. En otros países, todos los productos lácteos comercializados y gran cantidad de zumos y cereales se suplementan.
Al implantar esta medida, seguiríamos las líneas que marcan las principales Asociaciones Pediátricas, ya que prácticamente la totalidad de nuestra población cumple, al menos, con uno de los supuestos para suplementar. Pero nuestros niños presentan un déficit aislado de VD sin repercusión sobre los marcadores del metabolismo óseo y están clínicamente asintomáticos. Ante estos datos cabe preguntarse si la suplementación con VD es realmente necesaria. En los últimos tiempos están surgiendo trabajos en este sentido. Esperamos que la evidencia científica aclare nuestras dudas.
CONCLUSIONES
Nuestro trabajo evidencia que el déficit de vitamina D, con los niveles de corte aceptados actualmente, es muy frecuente en nuestro medio. Los inmigrantes, el sexo femenino y los adolescentes son los que tienen más probabilidad de presentar este déficit vitamínico, sobre todo, cuando coinciden los tres factores.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS: VD: vitamina D.
BIBLIOGRAFÍA
- Alonso López C, Ureta Velasco N, Pallás Alonso CR, Grupo PrevInfad Infancia y Adolescencia. Vitamina D profiláctica. Rev Pediatr Aten Primaria. 2010;12:495-510.
- Rosen CJ. Vitamina D Insufficiency. N Engl J Med. 2011;364:248-54.
- Manson JE, Mayne ST, Clinton SK. Vitamin D and prevention of cancer: ready for prime time? N Engl J Med. 2011;364:1385-7.
- Elamin MB, Abu Elnour NO, Elamin KB, Fatourechi MM, Alkatib AA, Almandoz JP, et al. Vitamin D and cardiovascular outcomes: a systematic review and meta-analysis. J Clin Endocrinol Metab. 2011;96:1931-42.
- Wang L, Manson JE, Song Y, Sesso HD. Systematic review: vitamina D and calcium supplementation in prevention of cardiovascular events. Ann Intern Med. 2010;152:315-23.
- Wagner CL, Taylor SN, Hollis BW. Does vitamin D make the World go “round”? Breastfeed Med. 2008;3:239-50.
- Wagner CL, Greer FR. Prevention of rickets and vitamin D deficiency in infants, children, and adolescents. Pediatrics. 2008;122:1142-52.
- Holick MF, Chen TC. Vitamin D deficiency: a wordwide problem with health consequences. Am J Clin Nutr. 2008;87:1080S-6S.
- Martínez Suárez V, Moreno Villares JM, Dalmau Serra J, Comité de Nutrición de la Asociación Española de Pediatría. Recomendaciones de ingesta de calcio y vitamina D: posicionamiento del Comité de Nutrición de la Asociación Española de Pediatría. An Pediatr (Barc). 2012;77:57.e1-e8.
- Merino Moína M, Grupo PrevInfad. Prevención del cáncer de piel y consejo de protección solar. En: PrevInfad (AEPap)/PAPPS infancia y adolescencia [en línea] [consultado el 05/09/2016]. Disponible en www.aepap.org/previnfad/pdfs/previnfad_fotoproteccion_rec.pdf
- Vitamin D supplementation: recommendations for Canadian mothers and infants. Paediatr Child Health. 2007;12:583-98.
- Silva Rico JC, Silva Higuero N. Raquitismo carencial y otras formas de raquitismo. Pediatr Integral. 2011;XV:654-68.




