Vol. 18 - Num. 69
Originales
Mortalidad e ingresos hospitalarios por violencia de los menores de 15 años en la Comunidad Valenciana (2007-2011)
M.ª Luisa Carpio Gestaa, M.ª Jesús Redondo Gallegob, Ferrán Ballester i Diezc
aDirección General de Salud Pública. Conselleria de Sanitat. Generalitat Valenciana. Valencia. España.
bUnidad Mixta de Investigación. Universitat de València-FISABIO-UJI. Valencia. España.
cUnidad Mixta de Investigación. Universitat de València-FISABIO-UJI. CIBERESP. Valencia. España.
Correspondencia: ML Carpio. Correo electrónico: carpio_mar@gva.es
Cómo citar este artículo: Carpio Gesta ML, Redondo Gallego MJ, Ballester i Diez F. Mortalidad e ingresos hospitalarios por violencia de los menores de 15 años en la Comunidad Valenciana (2007-2011). Rev Pediatr Aten Primaria. 2016;69:25-33.
Publicado en Internet: 30-03-2016 - Número de visitas: 17241
Resumen
Introducción: la violencia contra la infancia jamás es justificable y puede prevenirse actuando sobre los desencadenantes de comportamientos violentos. Conocer su magnitud y características posibilita emprender cambios que contribuyan a reducir su frecuencia y gravedad.
Métodos: se analiza la mortalidad y los ingresos hospitalarios por violencia en menores de 15 años en el periodo 2007-2011 en la Comunitat Valenciana.
Resultados: se contabilizaron 12 defunciones y 156 ingresos. Murieron tres veces más niños que niñas. Los fallecimientos fueron más frecuentes en los menores de un año, seguido del grupo de 10-14 años. Los seis casos de suicidio ocurrieron en el grupo de 10-14 años y los métodos utilizados fueron: ahorcamiento, estrangulamiento o sofocación y saltar desde lugar elevado. Los homicidios fueron el doble en niños y niñas de 0-9 años.
Ingresaron por violencia dos veces más las niñas, siete veces más en el grupo de 10-14 años, tres veces más los extranjeros, dos veces más los residentes en medio rural y dos veces más si tenían riesgo de exclusión social, siendo estas diferencias estadísticamente significativas. Los ingresos por violencia autoinfligida fueron el doble (intento de suicidio) que por agresiones.
Conclusiones: el número de casos es de gran importancia epidemiológica y de salud pública. En la violencia contra la infancia se manifiestan los ejes de desigualdad en salud y la necesidad de mejorar la declaración y la coordinación de todos los ámbitos de la atención a los menores. Es relevante relacionar las distintas fuentes de información, devolverla a los profesionales y formarlos.
Palabras clave
● Maltrato infantil ● Mortalidad infantil ● Niños hospitalizados ● Violencia domésticaINTRODUCCIÓN
Para la Organización Mundial de la Salud (OMS), la violencia contra los niños y niñas jamás es justificable y es evitable. En 1996, la 49.ª Asamblea Mundial de la Salud adoptó la resolución WHA49.25, que declara que la violencia es un problema de salud pública fundamental y creciente en todo el mundo e insta a los Estados a abordarla desde la perspectiva de la salud pública1.
Las recomendaciones internacionales aconsejan a los Estados utilizar indicadores nacionales basados en normas acordadas internacionalmente y garantizar la compilación, análisis y difusión de los datos para comprobar los progresos en el tiempo. Los datos deberían desglosarse por sexo, edad, medio urbano o rural, características de los hogares y familiares, educación y etnia2.
Sin embargo, una característica singular de la violencia es su ocultamiento. En los niños/as víctimas de violencia, por vergüenza, miedo al rechazo social, sentimiento de culpa y ausencia de canales de denuncia asequibles. Por miedo al castigo legal o la posibilidad de perder la custodia de los menores en los actores y espectadores de violencia en menores. Y en los profesionales, a pesar de su obligación legal, además de moral, de hacerlo4, por miedo a los “falsos positivos” (equivocarse en el diagnóstico y sus posibles repercusiones sociales y legales)3, la desconfianza en la actuación eficaz de los sistemas oficiales de protección de menores y la probabilidad de verse inmersos en litigios.
Hay una fuerte evidencia de que en la mayoría de los casos de maltrato o cualquier otro tipo de violencia contra los menores no se informa, incluso en los países en los que existe obligatoriedad legal de notificar. Las estadísticas de maltrato basadas en las fuentes oficiales de los servicios públicos (sanitario, escolar, judicial, bienestar social, policial) subestiman la prevalencia de violencia contra la infancia, como se sugiere cuando se las compara con encuestas basadas en autoinformes de ámbito comunitario2. Se estima que los organismos públicos declaran entre el 6% y el 10% de la magnitud del fenómeno y que solo alrededor del 1% de los niños/as que sufren violencia presentan lesiones que requieren atención médica5.
Las manifestaciones de la violencia contra la infancia varían con la edad, existiendo mayor riesgo de lesiones graves en los bebés y menores de cinco años debido a su mayor vulnerabilidad, por la dificultad diagnóstica al carecer del testimonio de la víctima y por la invisibilización de estos en la sociedad, al moverse habitualmente solo en el ámbito de lo privado. Entre la mortalidad por violencia más difícil de identificar están los infanticidios por asfixia, envenenamiento o ahogamiento presentados como muerte súbita en la infancia6,7.
En relación a las diferencias por sexo, se referencia más abuso físico en niños y abuso sexual en niñas, con influencia del modelo social de género8.
En estudios comunitarios realizados en Europa, la prevalencia de abuso sexual observada es del 9,6%, siendo de 13,4% en chicas y 5,7% en chicos; del 22,9% para el maltrato físico y del 29,1% para el abuso emocional. Hay pocos estudios disponibles sobre negligencia, pero su prevalencia estimada en estudios a nivel internacional es de 16,3% para la física y 18,4% para la emocional9.
En España, diversos estudios sitúan la prevalencia del abuso sexual infantil entre el 7 y el 15% en varones y entre el 13 y el 22% en mujeres10-13. El 11,4% de los menores de entre 11 y 18 años declaran haber sido golpeados, pateados, empujados, zarandeados o encerrados en el colegio/instituto alguna vez en los dos últimos meses14.
Según el Centro Reina Sofía para el estudio de la violencia, la mortalidad por maltrato infantil se ha triplicado entre 1997 y 2001, con una distribución semejante entre género. Además, los niños sufren más maltrato físico y negligencia que las niñas, y estas más abusos sexuales15.
En el estudio en menores de 15 años de la Comunitat Valenciana (CV) correspondiente al periodo 2001-2006 se encontró que la mortalidad por violencia era más frecuente en varones y aumentaba con la edad, con predominio de los homicidios. En cambio, los ingresos hospitalarios por violencia fueron más frecuentes en niñas, con predominio de la violencia autoinfligida (intentos de suicidio) y en el grupo de 10-14 años16.
Conocer las características de la violencia, su magnitud y los factores asociados a la misma (desigualdades en salud) en nuestro ámbito es fundamental para planificar y evaluar las actuaciones de los diversos ámbitos de atención relacionados con los menores (sanitario, educación, servicios sociales, policial…)17. Nos permite emprender los cambios necesarios para disminuir su frecuencia y gravedad. El sistema sanitario dispone de fuentes de información rutinarias y sistemáticas (boletines de defunción e informes de altas hospitalarias) que recogen datos codificados homogéneamente sobre las consecuencias en salud de la violencia (Clasificación Internacional de Enfermedades) y permiten su análisis y la comparabilidad. Utilizando estas fuentes, se realiza este trabajo, cuyos objetivos son el análisis de la mortalidad y los ingresos hospitalarios (en centros públicos) por violencia en los menores de 15 años de la CV entre 2007-2011.
MATERIAL Y MÉTODO
Diseño
Estudio observacional y retrospectivo de las bases de datos sanitarias rutinarias del Registro de Mortalidad de la CV y del Conjunto Mínimo Básico de Datos (CMBD) de las altas hospitalarias de los hospitales públicos de la CV.
Periodo de estudio
Del año 2007 al 2011, ambos inclusive. Se agrupó un periodo de cinco años al ser acontecimientos poco frecuentes, para reducir el error aleatorio y ganar en poder estadístico.
Ámbito de estudio
La Comunitat Valenciana. El número de casos hallados no aconseja mayor desagregación territorial.
Población de referencia
La población de referencia son los niños y niñas menores de 15 años empadronados que constan en el Sistema de Información Poblacional (SIP) de la Conselleria de Sanitat de la CV en el periodo de estudio (3 956 448). Para el análisis por nacionalidad de los ingresados, se utilizó como denominador las personas-año según el Instituto Nacional de Estadística (3 274 039 españoles frente 554 310 no españoles). Para el tamaño del municipio de residencia y clase social, el denominador se obtiene a partir de los datos de población que ofrece Eurostat/OCDE para 2009, año de mitad del periodo de estudio (3 521 239 urbana frente a 435 209 rural y 3 082 073 sin riesgo de exclusión social frente a 874 375 con riesgo).
Clasificación de las variables resultado
Las causas de muerte son codificadas con la Clasificación Internacional de Enfermedades, 10.ª revisión (CIE-10) mediante los códigos del capítulo 20 de “Causas externas de morbilidad y mortalidad para violencia” (X60-X99, Y00-Y09 e Y87). Se desestima un caso de un niño de cuatro años que muere como consecuencia de un suicidio (código X72 CIE-10: Lesión autoinfligida intencionalmente por disparo de arma corta), al no considerarlo congruente con la literatura científica al respecto de la atribución de intencionalidad antes de los 5-6 años18.
Los diagnósticos de ingreso hospitalario son codificados con la Clasificación Internacional de Enfermedades, 9.ª revisión, modificación clínica (CIE-9MC) mediante los códigos de causas externas para violencia (E950-E969). Los niños podían haber ingresado más de una vez en el periodo de estudio, aunque no se dio esta circunstancia en ningún caso. Se encontró que, en dos casos, había habido un traslado desde un hospital comarcal a uno general y, en uno de ellos, por el mismo proceso, un traslado de vuelta al hospital comarcal. Se recodificaron los datos para su tratamiento epidemiológico como un único proceso con una estancia sumatoria y los diagnósticos y procedimientos completos. Se excluyen los ingresos de dos niñas del grupo de 1-4 años de edad codificadas como suicidio (código E950.3: Suicidio por ingestión de tranquilizantes y código E-958: Suicidio por otros medios) al considerar los errores de codificación, ya que se considera que por debajo de los cinco o seis años, los niños tienen un concepto muy rudimentario de lo que es la muerte o el morir, por lo que resulta prácticamente improbable que se participe activamente de la muerte18.
Clasificación de las variables explicativas
Se consideró municipio rural si su población era menor o igual a 10 000 habitantes y los de mayor población se clasificaron como urbanos.
El riesgo de exclusión social se obtuvo a partir del índice APSIG que construye el SIP y que en su dígito 26 refleja la situación de riesgo social. Se considera que existe riesgo de exclusión social cuando está presente cualquiera de las cinco categorías siguientes: desempleados, extranjeros irregulares, sin recursos beneficiarios y no beneficiarios e indefinido, que se han agrupado para el estudio (no frente a sí).
Análisis
Los datos se trabajaron de forma anónima mediante un identificador que permite relacionarlos con otras fuentes de información del Sistema Sanitario como el SIP, manteniendo la confidencialidad de los mismos.
Se realizó un análisis descriptivo de las variables de resultado con las tasas de mortalidad, de frecuentación hospitalaria y la estancia media hospitalaria. A continuación, se estudió la distribución de las variables de resultado según las siguientes variables explicativas: edad agrupada, sexo y tipo de violencia (autoinfligida o agresión), tanto para mortalidad como para hospitalización. Además, para las hospitalizaciones se analizó la relación con nacionalidad (españoles frente a no españoles), lugar de residencia (rural frente a urbano) y riesgo de exclusión social. Se han calculado sus correspondientes razones de tasas con sus intervalos de confianza (IC) y la significación estadística para un nivel de confianza del 95% (IC 95).
Se calculó la mortalidad proporcional hospitalaria por violencia, su comparación con la general y su significación estadística mediante la prueba exacta de Fisher.
Se describieron también las circunstancias al alta y la existencia de la correspondiente hoja de notificación para la atención sociosanitaria infantil y la protección de menores (HNASIPM).
El trabajo cuenta con la aprobación del Comité ético de la Dirección General de Salud Pública y Centro Superior de Investigación en Salud Pública (27/12/2013) de la CV.
RESULTADOS
En el periodo 2007-2011 hubo 1370 defunciones, 12 de ellas por violencia, que constituyen un 0,95% del total de fallecimientos en menores de 15 años de la CV.
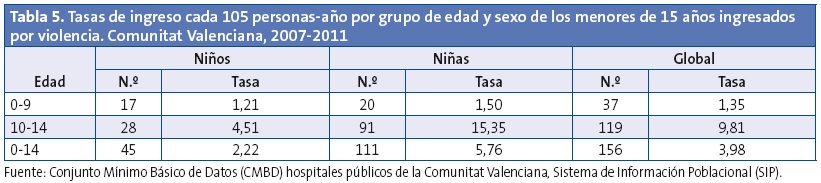
Las tasas específicas de mortalidad por violencia por grupo de edad y sexo (Tabla 1) muestran a los menores de un año como los de mayor riesgo de muerte por violencia, con una tasa de mortalidad por violencia de 0,7385/105 personas-año, seguido del grupo de 10-14 años: 0,5768/105 personas-año. En este grupo de 10-14 años, la mortalidad por violencia fue 3,16 veces más frecuente que en los de 0-9 años (IC 95 de la razón de tasas: 0,86-12,64, sin significación estadística). En cuanto a la distribución por sexos, las muertes por violencia fueron 2,85 veces más frecuentes en niños que en niñas (IC 95 de la razón de tasas: 0,71-16,37, sin significación estadística).
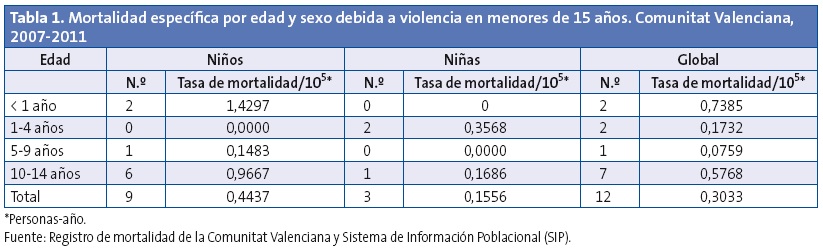
En cuanto a la tipología de las muertes por violencia, se distribuyeron al 50% entre autoinflingida (suicidios) y agresiones (homicidios). Su descripción se presenta en la Tabla 2.
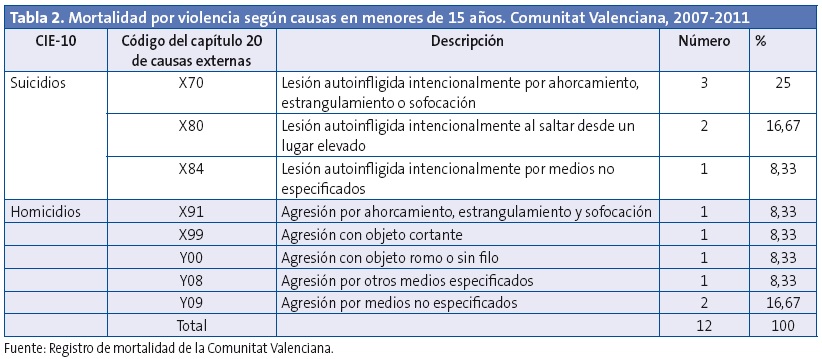
Los suicidios se produjeron todos en el grupo de 10-14 años, ocurriendo en niños 4,75 veces más que en niñas (IC 95 de la razón de tasas: 0,53-224,73, sin significación estadística).
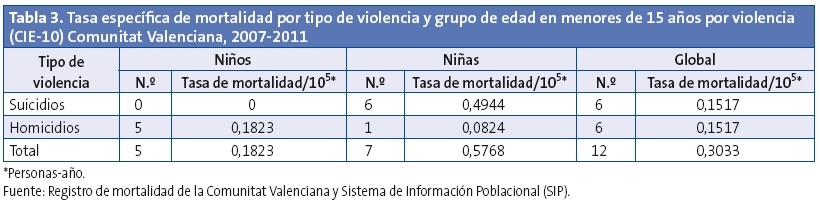
Los homicidios fueron 2,21 veces más frecuentes en los menores de diez años con respecto al grupo de 10-14 años (IC 95 de la razón de tasas: 0,24-104,64) y 1,90 veces más frecuentes en niños respecto a niñas (IC 95 de la razón de tasas: 0,27-21,01), resultando en ambos casos estas diferencias sin significación estadística (Tablas 3 y 4).
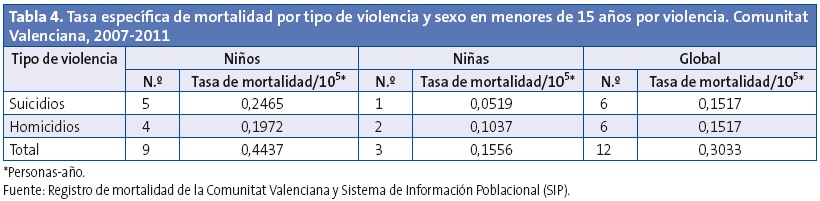
De las 198 067 altas de hospitales públicos en nuestro estudio, 156 fueron por ingresos por violencia (0,078%).
Las tasas de ingreso por violencia por grupo de edad y sexo (Tabla 5) muestran el predominio del grupo de 10-14 años, 7,26 veces más frecuente que en los menores de diez años (IC 95 de la razón de tasas: 5,02-10,51) y 2,59 veces más frecuentes en niñas que en niños (IC 95 de la razón de tasas: 1,83-3,67), ambos resultados con significación estadística (p<0,0001), mientras que para el conjunto de ingresos por todas las causas son mayoría los niños y su frecuencia disminuye con la edad (Tabla 6).
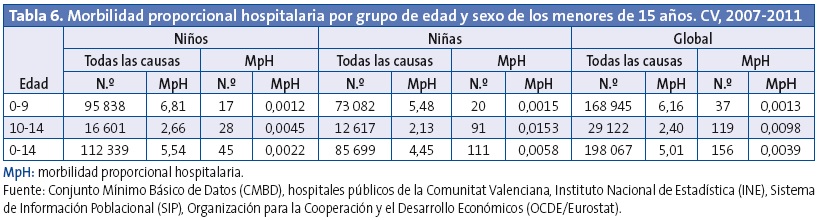
Las causas de ingreso por violencia fueron en el 63,5% (99 casos) por lesión autoinfligida, fundamentalmente mediante ingesta de medicamentos (77 casos); y el 36,5% restante (57 casos) por agresión (27 apaleamientos, cinco apuñalamientos, tres violaciones, etc.). En el 17% de los casos de lesión autoinfligida hubo asociado un diagnóstico de enfermedad mental.
El 61,5% de las altas por violencia se correspondían a menores de 15 años de nacionalidad española (Tabla 7). La razón de tasas de ingreso por nacionalidad muestra que los ingresos por violencia fueron 3,56 veces más frecuentes en los de nacionalidad no española respecto a los españoles (IC 95 de la razón de tasas: 2,57-4,94), con significación estadística (p<0,0001).
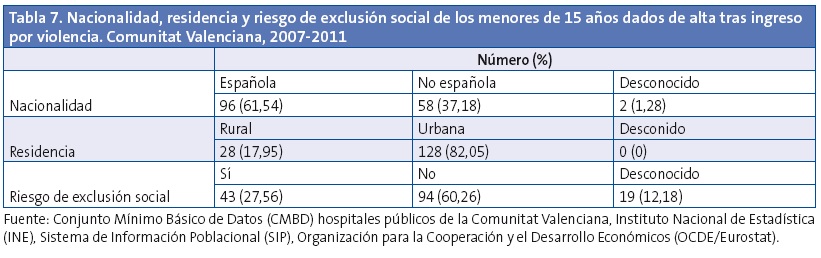
Por tamaño del municipio de residencia, el 82% de los menores de 15 años hospitalizados por violencia residían en municipios de más de 10 000 habitantes (Tabla 7). La razón de tasas de ingreso por tamaño del municipio de residencia muestra que los ingresos por violencia fueron 1,76 veces más frecuentes en los residentes en medio rural respecto a los residentes en medio urbano (IC 95: 1,17-2,66), con significación estadística (p=0,0081).
El 27,6% de los ingresos producidos en el periodo se correspondían a menores de 15 años que vivían en riesgo de exclusión social (Tabla 7). La razón de tasas de frecuentación por riesgo de exclusión social muestra que los ingresos por violencia fueron 1,61 veces más frecuentes en los menores de 15 años con riesgo con respecto a los que no presentaban riesgo de exclusión (IC 95: 1,12-2,31), con significación estadística (p=0,0118).
Tras una estancia media por violencia de 3,9 días (moda: un día) frente a 4,9 por todas las causas (moda: 20 días), el 89,7% de los casos (140 casos) regresan a su domicilio.
Se producen dos defunciones entre los ingresados por violencia, correspondientes a dos niñas de 11 y 14 años de edad (1,28%), por suicidio con ingestión de medicamentos. Esta mortalidad proporcional hospitalaria por violencia es 4,4 veces mayor a la de por todas las causas, que fue del 0,29% (565 casos) para nuestra población de estudio, aunque sin significación estadística (prueba exacta de Fisher, p=0,075).
En los ingresos por violencia, únicamente se encontró antecedente de las preceptivas HNASIPM desde el ámbito sanitario en 13 casos (8,3%).
DISCUSIÓN Y CONCLUSIONES
La mortalidad por violencia en los menores de 15 años observada en la CV es superior al 0,6% de la mortalidad general estimada para el conjunto de España15,19. Hay que señalar que el número de efectivos puede estar condicionando los resultados del análisis epidemiológico.
El mayor riesgo de muerte por violencia se da en el primer año de vida, al igual que sucede en otros países europeos20. Sin embargo, en este grupo etario, hay que tener en cuenta la dificultad para el diagnóstico diferencial6,7.
Mueren más niños que niñas por violencia, tanto por suicidios como por homicidios, hecho puesto de manifiesto a nivel mundial por la OMS, y también observado en España y en la CV15,16,19.
Las causas de muerte se distribuyeron al 50% entre violencia autoinfligida y agresiones, habiendo aumentado el porcentaje de los suicidios con respecto al quinquenio anterior en la CV (22%). Este aumento de suicidios coincide con las previsiones de la OMS16,19.
En los suicidios, la causa más frecuente de muerte es el ahorcamiento, estrangulamiento o sofocación, seguido de saltar desde un lugar elevado, métodos todos ellos contundentes y resolutivos, coincidiendo con lo observado en la población general española21.
En los ingresos hospitalarios por violencia en los menores de 15 años en la CV, los patrones por edad y sexo fueron distintos a los de la mortalidad por violencia. Así, ingresan más niñas que niños por violencia y la frecuencia de ingresos por violencia aumenta con la edad.
Llama la atención que los ingresos por lesiones autoinfligidas (suicidios consumados o tentativas) fueron significativamente dos veces más frecuentes que las agresiones, lo que debe hacernos reflexionar acerca del sufrimiento que viven nuestros menores.
En cuanto a factores predisponentes de las conductas suicidas, mientras que en otros estudios predominan la existencia de trastornos psiquiátricos21,22, en nuestro estudio solo el 17% de los ingresos por autoagresión en niños/as tuvieron asociado un diagnóstico de salud mental, lo que hace sospechar un infradiagnóstico de la salud mental infantil en nuestro medio.
Murieron dos de las niñas ingresadas por violencia, por ingesta no accidental de medicamentos, suponiendo una mortalidad proporcional hospitalaria por violencia 4,4 veces superior a la observada en los ingresos por todas las causas en menores de 15 años. La diferencia no es estadísticamente significativa, quizás por el número de casos.
En nuestro estudio, los factores que aumentan significativamente el riesgo de ingresar por violencia son: no ser español (tres veces), residir en ámbito rural (casi dos veces) y estar en riesgo de exclusión social (casi dos veces).
Tanto en la mortalidad como en los ingresos hospitalarios se han atribuido suicidios a niños de cuatro años de edad, lo que no se sostiene con la evidencia científica18. Este hecho nos hace plantearnos dudas respecto a la calidad de la codificación de estos eventos, en ocasiones por la dificultad de identificar los infanticidios por asfixia, envenenamiento o ahogamiento presentados como muerte súbita en la infancia6,7.
La mayoría de los niños ingresados por violencia vuelven a casa al alta donde, si era necesaria una intervención familiar o de protección y no se ha puesto en marcha a través de la correspondiente notificación, la violencia puede entrar en su circuito de repetición, acercamiento entre episodios y agravamiento habituales.
Constatamos que solo en el 8% de los casos de niños hospitalizados por violencia se había realizado la notificación correspondiente mediante la HNASIPM. Esta situación evidencia la necesidad de sensibilización profesional acerca de la importancia de integrar la promoción del buen trato en la vigilancia de la salud infantil y garantizar el derecho de los menores a que se inicie un procedimiento que ayude a mejorar su situación. Es conocida la asociación entre intento de suicidio en niños y el maltrato físico y los abusos sexuales21.
Queda mucho por hacer en cuanto a la prevención y abordaje de la violencia contra los menores en el ámbito sanitario. La planificación de estrategias de actuación eficaces requiere mejorar la declaración de los casos de violencia atendidos, relacionar la información de distintas fuentes (hoja de notificación, morbilidad grave y mortalidad) y devolver esta información a los distintos profesionales encargados de la salud de los/as niños/as, junto con apoyo y formación y establecer cauces formales de coordinación con otros ámbitos de la atención a los menores.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS: CIE-10: Clasificación Internacional de Enfermedades, 10.ª revisión · CIE-9MC: Clasificación Internacional de Enfermedades, 9.ª revisión, modificación clínica · CMBD: Conjunto Mínimo Básico de Datos · CV: Comunitat Valenciana · HNASIPM: hoja de notificación para la atención sociosanitaria infantil y la protección de menores · IC: intervalo de confianza · IC 95: intervalo de confianza del 95% · OMS: Organización Mundial de la Salud · SIP: Sistema de Información Poblacional.
BIBLIOGRAFÍA
- Organización Panamericana de la Salud, Oficina Sanitaria Panamericana, Oficina Regional de la Organización Mundial de la Salud. Informe mundial sobre la violencia y la salud. En: Organización Mundial de la Salud [en línea] [consultado el 29/03/2016]. Disponible en who.int/violence_injury_prevention/violence/world_report/en/summary_es.pdf
- Pinheiro PS. Word report on violence against children. En: UNICEF [en línea] [consultado el 29/03/2016]. Disponible en www.unicef.org/lac/full_tex(3).pdf
- Ley de los Derechos de Salud de Niños y Adolescentes. Ley 8/2008 de 20 de junio. Diari Oficial de la Generalitat Valenciana, nº 5793, (26/06/2008).
- Skellern C. Medical experts and the law: safeguarding children, the public and the profession. J Paediatr Chile Health. 2008;44:736-42.
- Gilbert R, Kemp A, Thoburn J, Sidebotham P, Radford L, Glaser D, et al. Recognising and responding to child maltreatment. 2009;373:167-80.
- Levene S, Bacon CJ. Sudden unexpected death and covert homicide in infancy. Arch Dis Child. 2004;89:443-7.
- Bajanowski T, Vennemann M, Bohnert M, Rauch E, Brinkmann B, Mitchell EA. Unnatural causes of sudden unexpected deaths initially thought to be sudden infant death syndrome. Int J Legal Med. 2005;119:213-6.
- Ruíz Díaz MA. Registro de casos: la experiencia de la comunidad de Madrid-Ámbito sanitario. En: Cuadernos Pediatría Social [en línea] [consultado el 29/03/2016]. Disponible en pediatriasocial.es/HtmlRes/Files/Cuadernos16.pdf
- Sethi D, Bellis M, Hughes K, Gilbert R, Mitis F, Galea G. European report on preventing child maltreatment. En: Organización Mundial de la Salud [en línea] [consultado el 29/03/2016]. Disponible en: www.euro.who.int/__data/assets/pdf_file/0019/217018/European-Report-on-Preventing-Child-Maltreatment.pdf
- López F. Los abusos sexuales a menores. Lo que recuerdan de mayores. Madrid: Ministerio de Asuntos Sociales; 1994.
- De Paúl J, Arruabarrena MI. Behavior problems in school-aged physically abused and neglected children in Spain. Child Abuse Negl. 1995;19:409-18.
- Pereda N, Guilera G, Fons M, Gómez-Benito J. The prevalence of child sexual abuse in community and student samples: a meta-analysis. Clinical Psychol Rev. 2009;29:328-38.
- Cortés Arboleda MR, Cantón Duarte J, Cantón-Cortés D. Naturaleza de los abusos sexuales a menores y consecuencias en la salud mental de las víctimas. Gac Sanit. 2011;25:157-65.
- González-Bueno G, Bello A. La infancia en España 2014. El valor social de los niños: hacia un Pacto de Estado por la infancia. En: UNICEF Comité Español [en línea] [consultado el 29/03/2015]. Disponible en unicef.es/sites/www.unicef.es/files/infancia-espana/unicef_informe_la_infancia_en_espana_2014.pdf
- Centro Reina Sofía para el estudio de la violencia. Maltrato infantil en la familia en España. Madrid: Ministerio de Sanidad, Política Social e Igualdad; 2011.
- Violencia en la Infancia en la Comunitat Valenciana. Informes de salud nº 107, 2008 En Conselleria de Sanitat, Generalitat Valenciana [en línea] [consultado el 29/03/2015]. Disponible en sp.san.gva.es/biblioteca/publicacion_dgsp.jsp?cod_pub_ran=70134
- Plan de calidad para el sistema Nacional de Salud. En: Ministerio de Sanidad, Política Social e Igualdad [en línea] [consultado el 29/03/2015]. Disponible en msssi.gob.es/organizacion/sns/planCalidadSNS/pdf/pncalidad/PlanCalidad2010.pdf
- Factores de riesgo suicida en la niñez. En: Psicología online. Formación, autoayuda y consejo online [en línea] [consultado el 29/03/2015]. Disponible en psicologia-online.com/ebooks/suicidio/ninez.shtml
- Krug EJ, Dahlberg LL, Mercy JA, Zwi AB, Lozano R. Word report on violence and health. En: Organización Mundial de la Salud [en línea] [consultado el 29/03/2015]. Disponible en who.int/violence_injury_prevention/violence/world_report/en/summary_es.pdf
- Preventing child maltreatment in Europe: a public health approach. Policy Briefing. En: Organización Mundial de la Salud [en línea] [consultado el 29/03/2015]. Disponible en euro.who.int/__data/assets/pdf_file/0012/98778/E90618.pdf
- Ayuso-Mateos JL, Baca-García E, Bobes J, Giner J, Giner L, Pérez V, et al. Grupo RECOMS. Recomendaciones preventivas y manejo del comportamiento suicida en España. Rev Psiquiatr Salud Ment. 2012;5:8-23.
- Joiner TE Jr, Sachs-Ericsson NJ, Wingate LR, Brown JS, Anestis MD, Selby EA. Childhood physical and sexual abuse and lifetime number of suicide attempts: a persistent and theoretically important relationship. Behav Res Ther. 2007;45:539-47.




