Vol. 18 - Num. 69
Originales
¿Quién realiza los controles de salud en la Comunidad Valenciana? Propuestas de mejora
Javier Soriano Fauraa, Carlos Labordena Barcelób, M.ª Dolores Gutiérrez Siglerc, Elena Fabregat Ferrerd, Julia Colomer Revueltae, Francesc Bargall Lleonartf
aPediatra. CS Fuensanta. Valencia. España.
bPediatra. CS Fernando el Católico. Castellón. España.
cPediatra. CS Nou Molés. Valencia. España.
dPediatra. CS Gran Vía. Castellón. España.
eDepartamento de Pediatría, Obstetricia y Ginecología. Unidad de Pediatría. Universidad de Valencia. Valencia. España.
fPediatra. CS Almenara. Castellón. España.
Cómo citar este artículo: Soriano Faura J, Labordena Barceló C, Gutiérrez Sigler MD, Fabregat Ferrer E, Colomer Revuelta J, Bargall Lleonart F. ¿Quién realiza los controles de salud en la Comunidad Valenciana? Propuestas de mejora. Rev Pediatr Aten Primaria. 2016;69:17-24.
Publicado en Internet: 30-03-2016 - Número de visitas: 20088
Resumen
Introducción: el objetivo principal es conocer la cobertura de la enfermería pediátrica en el Programa de Salud Infantil (PSI) y como objetivos secundarios analizar la aceptación, competencia y necesidades formativas de los equipos de Pediatría y enfermería en la Comunidad Valenciana (CV).
Material y métodos: estudio transversal, descriptivo, de los datos recogidos mediante encuesta online anónima realizada a pediatras y enfermeros de la CV durante dos meses de 2014 sobre quién realiza y quién debería realizar los controles del PSI y las aptitudes y necesidades formativas detectadas.
Resultados: un 87% de los encuestados refirió disponer en su centro de enfermería pediátrica. Realizan controles conjuntamente, enfermera y pediatra, en un 70% de los casos. Las habilidades principales de la enfermería se consideran: consejo sobre alimentación, hábitos saludables y vacunación. La mitad de encuestados reconocen necesidades formativas. El 95% de los encuestados considera que es necesario disponer de enfermería pediátrica en los centros de salud. Uno de cada cuatro de los controles que realizan los pediatras en solitario se corresponde con las visitas iniciales del recién nacido, en la primera semana y el mes de vida.
Conclusión: todas las unidades asistenciales deben estar constituidas por personal de enfermería y pediatra. Las agendas de citación de enfermería tienen que ser flexibles para permitir su participación en los controles de salud de la primera semana y primer mes de vida del niño. En los programas de formación continuada deben implementarse contenidos acordes a las necesidades detectadas en este estudio para el desempeño de su actividad en el PSI.
Palabras clave
● Enfermeras pediátricas ● Prevención primaria ● Salud infantilINTRODUCCIÓN
La sociedad española ha experimentado importantes cambios sociodemográficos, económicos y culturales desde la creación de los primeros centros de salud en la década de los ochenta del siglo XX, cuando los pediatras se incorporaron a los equipos de Atención Primaria. Desde entonces, con la implantación en las diferentes autonomías del Programa de Salud Infantil (PSI), se han conseguido importantes avances en la prevención y promoción de la salud infantil. Ha sido uno de los programas con más aceptación entre los usuarios y existe un amplio consenso entre los profesionales sobre sus beneficios, aunque para la mayoría de actividades no se disponga de pruebas que demuestren su impacto mensurable en términos de salud1. Es una magnífica oportunidad para conocer al niño, la familia, sus condiciones de vida y representa un proceso continuado y valioso de prevención y promoción de la salud.
Las visitas del PSI son el marco adecuado para abordar los temas relacionados con el desarrollo, la conducta, el aprendizaje y la salud psicosocial. Todos estos aspectos han ganado relevancia con la nueva morbilidad derivada del aumento de las enfermedades crónicas y discapacidad en los niños, estructuras familiares heterogéneas, el estilo de vida de los países desarrollados y una mayor exigencia por parte de las familias y la sociedad en general.
Esta situación ha generado una mayor complejidad en el primer nivel de atención, que ha sido afrontada con voluntarismo por los equipos pediátricos de Atención Primaria (AP), como un reto asistencial y organizativo ante la falta de inversión por parte de la Administración Sanitaria2.
Somos conscientes de que el número de recomendaciones ha aumentado muchísimo y se extendería mucho más allá de lo que puede acometerse en una visita típica. Esto quizás también está contribuyendo a la amplia variación de la calidad y cantidad de servicios recibidos3. Percibimos que no se cubren todas las necesidades de las familias, que abandonan las consultas con dudas no resueltas, preocupaciones que no han podido plantear, incluso cribados para detección precoz de retrasos del desarrollo sin completar. A pesar del esfuerzo realizado por los profesionales, con nuestro sistema actual, la oportunidad que ofrece el PSI se desaprovecha y las familias no reciben todo el apoyo y la atención necesaria para asegurar que sus hijos desarrollen al máximo sus potenciales.
A partir de esta necesidad, detectada por los centros de AP, se ha revisado la bibliografía científica disponible y, aunque a nivel nacional no hay trabajos originales, hemos encontrado nuestra misma inquietud en países como EE. UU., donde los pediatras trabajan en AP y afrontan circunstancias similares con escasez de personal médico. Los investigadores y clínicos han propuesto opciones para mejorar la atención centrándose en cambios en los elementos estructurales, personal y su organización4. Estos cambios incluyen la asunción de tareas con amplia autonomía por el personal de enfermería y la oferta de formatos no convencionales, como las visitas grupales del PSI y la incorporación de las nuevas tecnologías de comunicación para consejo, guía anticipatoria y educación para la salud.
OBJETIVOS
El objetivo principal que nos planteamos es conocer la cobertura y autonomía de la enfermería pediátrica en el PSI realizado en los centros de salud de la Comunidad Valenciana.
Como objetivos secundarios, analizar la aceptación, preparación, competencia y necesidades formativas de los equipos de Pediatría en los controles de salud del PSI realizados en nuestra comunidad.
MATERIAL Y MÉTODOS
El diseño del estudio es transversal, descriptivo y no aleatorizado, mediante encuesta online anónima y autoadministrada a pediatras y enfermeros de la Comunidad Valenciana.
La población estimada de pediatras y enfermeros que atienden a la infancia en AP es de 1200, según datos del 20085, estimándose en 221 el tamaño de la muestra para un intervalo de confianza (IC) del 90% y para un 50% +/-5 de frecuencia de resultados de la variable principal: cobertura de enfermería pediátrica en los centros de salud.
El reclutamiento se realizó acudiendo a las listas de distribución de los Colegios de Enfermería de la Comunidad Valenciana, de las sociedades de Pediatría de las tres provincias y de la lista de centros de Atención Primaria de la provincia de Valencia.
El cuestionario online se diseñó mediante un formulario en formato Google Docs®. El contenido de las preguntas se consensuó entre los profesionales del Grupo Asesor Técnico para la Pediatría de Atención Primaria (GATap). Siguiendo las recomendaciones de la bibliografía científica, se definieron cuatro dominios a estudiar en la encuesta, según los objetivos propuestos:
- La cobertura de enfermería pediátrica en los centros de salud.
- Controles de salud realizados solo por enfermería o Pediatría.
- Grado de aceptación, preparación y competencia, según criterio de los pediatras y personal de enfermería.
- Necesidades formativas detectadas por los pediatras y personal de enfermería.
Los datos se recogieron en el periodo del 22 de abril al 20 de junio de 2014. Con los resultados obtenidos se realizó un estudio estadístico aplicando el software SPSS+ v.15.0®, análisis descriptivo y analítico, tablas de contingencia, con estimación de χ2, estimación de riesgo, odds ratio (OR), con un IC del 95%.
RESULTADOS
Colaboraron en el estudio 253 profesionales, siendo mayor la representación de pediatras, que supuso el 65% (175), que de enfermeros/as, del 35% (78). Algo más de las tres cuartas partes de quienes participaron (210) trabajaban en centros de salud, y en menor proporción en consultorios auxiliares (26), clínicas privadas (11) y hospitales (6). El 87% de los encuestados refirió disponer en su centro de enfermería pediátrica específica.
La aportación proporcional de los profesionales que ejercían en la provincia de Valencia alcanzó el 65% (164), siendo del 21% para Castellón (52) y del 15% para Alicante (37).
¿Quién realiza los controles de salud?
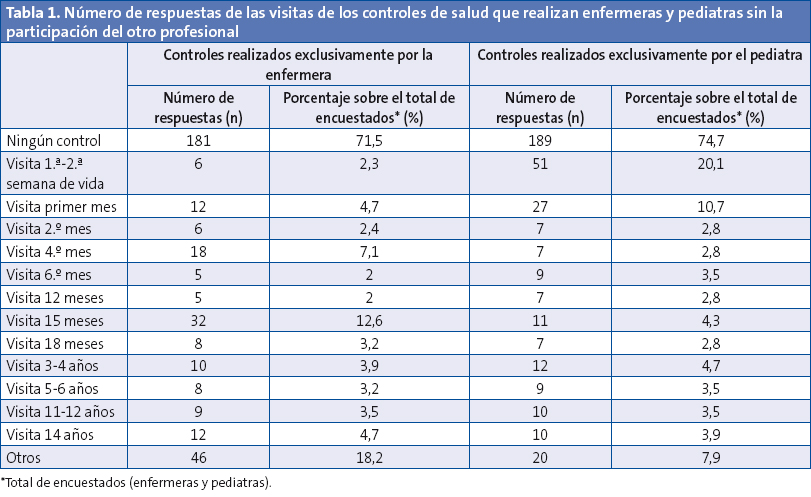
Más del 70% de los profesionales declararon que los controles de salud eran realizados conjuntamente por el pediatra y la enfermera.
Aproximadamente uno de cada cuatro de los controles que realizan los pediatras en solitario se corresponde con las visitas iniciales del recién nacido, en la primera semana y el mes de vida.
La visita de los 15 meses era la que en mayor porcentaje realizaban las enfermeras de forma exclusiva. Un 18,2% de estas profesionales ejecutaba alguna otra visita no incluida en el programa oficial (Tabla 1).
¿Quién debería realizar los controles de salud?
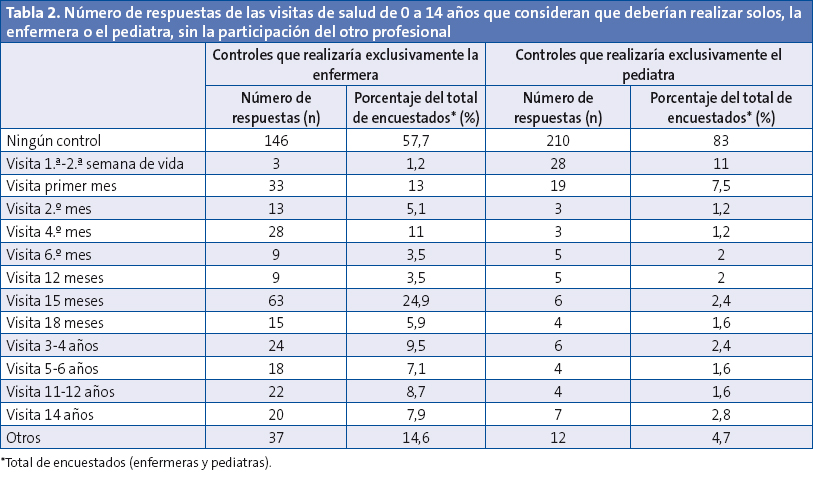
Según el 57,7% de los participantes en el estudio, ningún control lo debería realizar la enfermera de forma exclusiva (sin participación del pediatra). El 83% de los participantes consideran que los pediatras no deberían realizar ningún control sin la colaboración de enfermería.
Coincidiendo con la práctica, descrita en el apartado anterior, son las primeras visitas del recién nacido en el caso de los pediatras, y la de los 15 meses en el de las enfermeras, las que se consideran que deberían ser realizadas por un solo perfil profesional (Tabla 2).
Habilidades y necesidades formativas del profesional de enfermería para la realización de los controles de salud
La relación entre las diferentes habilidades que los encuestados consideran que tiene enfermería para la realización de los controles de salud y sus necesidades de formación aparecen en la Tabla 3.
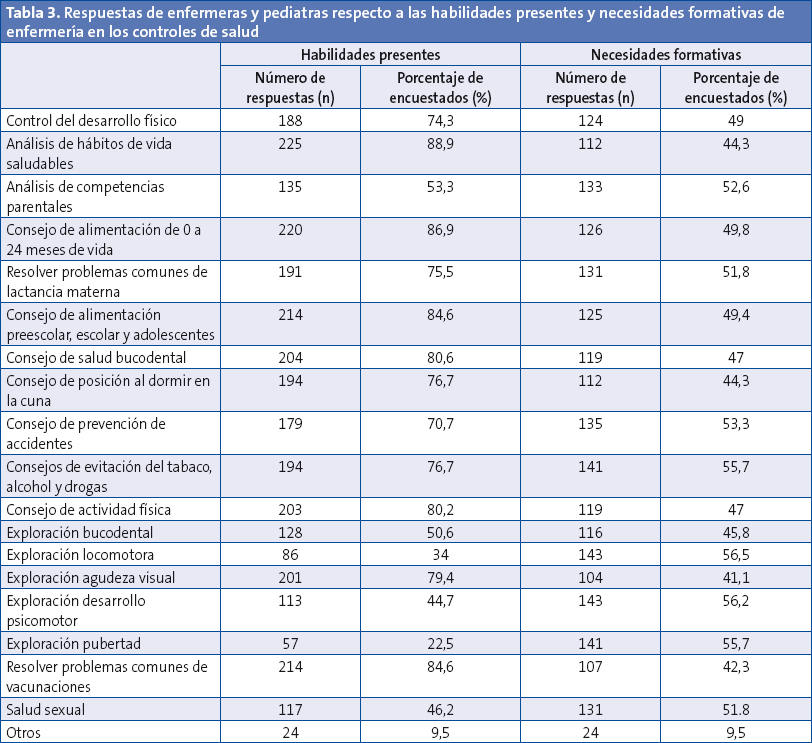
En cuanto a las habilidades de enfermería, los porcentajes más elevados de atribución se corresponden a las relacionadas con el análisis de hábitos de vida saludable (88,9%), el consejo (especialmente sobre alimentación) y la resolución de problemas comunes de vacunación. Sin embargo, la consideración de su preparación está por debajo del 50% cuando se trata de la realización de exploraciones, a excepción de la correspondiente a la agudeza visual que es cercana al 80%.
Respecto a las necesidades formativas, cerca del 50% de los profesionales indicaban carencias para las 19 actividades propuestas, sin preferencia marcada respecto a ninguna de ellas.
Necesidad de enfermería pediátrica específica
La necesidad de disponer de enfermería pediátrica fue declarada por casi la totalidad, el 95% de los profesionales participantes (241). Los pediatras estuvieron 3,3 veces más de acuerdo con la figura de la enfermería pediátrica que los enfermeros (intervalo de confianza del 95% [IC 95]: 1,02-0,9; p: 0,041).
Los centros que cuentan con profesionales de enfermería pediátrica son más proclives a manifestar la necesidad de su trabajo (OR: 12,09; IC 95: 5,55-40,97).
En los centros en los que no existe la figura de enfermería específica de Pediatría, el pediatra tiene más posibilidad de realizar algún control de salud solo, sin colaboración de enfermería. Tener enfermera pediátrica se identificó como factor protector para la colaboración de pediatra-enfermera en la realización de los controles de salud (OR: 0,47; IC 95: 0,19-0,95).
Aquellos pediatras que habitualmente no realizan los controles de salud en colaboración con la enfermera están menos de acuerdo con que la enfermera los realice sola, sin su colaboración (OR: 0,43; IC 95: 0,24-0,78).
Las enfermeras que realizan los controles de salud junto al pediatra opinan con mayor frecuencia, que dichos controles deben realizarse con la participación conjunta del pediatra (OR: 7,16; IC 95: 3,84-13,36).
DISCUSIÓN
Con los datos obtenidos podemos afirmar que la cobertura de enfermería pediátrica es mejorable ya que es inferior al 90%.
Por otra parte, hay una aceptación prácticamente unánime para que enfermería se integre en los equipos de Pediatría: el 95% de los encuestados consideran importante este tema, considerándose imprescindible este modelo allí donde ese modelo está establecido, con una probabilidad de apoyo al modelo “binomio enfermera-pediatra” superior a 12 (OR: 12,09; IC 95: 5,5-40,97).
Respecto a la autonomía de la enfermería en el PSI, los hallazgos encontrados demuestran que, en casi todos los controles, intervienen ambos profesionales. No se organizan los recursos humanos en aras a alcanzar una mayor cobertura en aspectos psicosociales, educativos y relativos al desarrollo. En consonancia con este hallazgo, y probablemente como causa del mismo, advertimos que existe un acuerdo discreto, de cerca del 43% de los encuestados, con que la enfermería debería realizar algunos controles de salud sin la colaboración de Pediatría. Un porcentaje ligeramente superior, el 52%, apoyaría un cambio de modelo de trabajo en el que algunos controles de salud fueran realizados solo por enfermería.
Hemos constatado un desacuerdo amplio, del 83%, en que el pediatra realice algunos controles de salud sin la participación de enfermería, con especial atención a los controles de la primera semana y el primer mes de vida.
Respecto a la preparación y necesidades formativas de los equipos, nuestros resultados apoyan la consideración de que enfermería tiene suficientes conocimientos para atender los contenidos de los controles de salud. También existe acuerdo, de entre el 70 y el 89% según las áreas de conocimientos encuestadas, en que las habilidades requeridas están presentes en buena parte de estas intervenciones. Todo ello sin renunciar a mejorar o actualizar la formación en las áreas de cribado, consejo e intervención de los controles, sobre todo en exploración del aparato locomotor, la pubertad y las conductas adictivas.
En la bibliografía de origen anglosajón se encuentran referencias a la figura de la enfermera de Pediatría desde mediados de los años setenta, hace 40 años, con buena aceptación por las familias y una mayor atención a los problemas de conducta y el desarrollo psicomotor. Trabajos más recientes ofrecen resultados en salud similares y apoyan una mayor asunción de responsabilidades por los profesionales de enfermería de Atención Primaria6,7. Desde los propios colegios profesionales de enfermería se reclama una mayor autonomía y reconocimiento de su trabajo, así como más visibilidad social, y exigen apoyo de la administración y del colectivo médico8. En este sentido, las agendas personalizadas de enfermería permiten al usuario la identificación de su enfermera de referencia, ofrecen una alternativa de acceso a los cuidados diferente de la consulta de Pediatría, que suponía, hasta hace poco, el único acceso posible al sistema tanto para tareas administrativas como derivaciones, demandas, concertadas, PSI, etc.
En el año 2010, cuando se publicó en el BOE el Plan de Formación de la especialidad de Enfermería Pediátrica (Orden SAS/1730/2010, de 17 de junio) con amplias competencias en el PSI, existía ya en la práctica real una implantación de la figura de la enfermera de Pediatría de un 80% o superior en 12 comunidades autónomas, entre las que se encuentra la nuestra9.
La bibliografía revisada coincide en que el PSI puede ser realizado por enfermeras especialmente entrenadas trabajando en coordinación con Pediatría. La enfermera puede disponer o adquirir las habilidades necesarias para desempeñar con corrección el PSI casi en su totalidad. El pediatra debe, por lo menos, realizar la exploración del niño en momentos clave de su desarrollo y recibir información del profesional de enfermería sobre los problemas que haya detectado, para su correcto encauzamiento.
Encontramos en la literatura científica nuestra misma preocupación acerca de cómo ofrecer a la población una visita completa que abarque los aspectos mencionados en este artículo y vemos que se plantean modelos innovadores, incluyendo una amplia variedad de proveedores de salud. En primer lugar, la enfermería, por supuesto, liderando equipos que se completan con trabajador social o educadores infantiles10.
También se ha estudiado proporcionar algunos servicios en un formato menos convencional que la visita individual presencial, como las visitas preventivas grupales (PSI grupal) que han demostrado ser al menos tan efectivas como la atención individual y con mayor contenido, sin incrementar el tiempo invertido. Las visitas grupales permiten un aprendizaje centrado en la familia, mayor participación de los padres, etc., y el valor añadido aportado por otros profesionales. El tamaño de los grupos más operativo oscila entre 4-5 familias4.
En otros países desarrollados la provisión de servicios no recae exclusivamente en los centros de Atención Primaria, sino que existen centros escolares con financiación variada que desarrollan actividades como: educación nutricional, consejo sobre el abuso de sustancias, salud mental-desarrollo y salud bucodental11.
“La estructura y organización de los centros de salud deben posibilitar espacios físicos y temporales para el trabajo en equipo y complementario entre Pediatría y enfermería; un modelo basado en la cooperación y la complementariedad”5. Avanzar en el desarrollo de este modelo colaborativo supondrá una revitalización del PSI, mejorando su calidad y coste-efectividad y dotándolo de la flexibilidad necesaria para captar a la población más vulnerable, equilibrar las desigualdades y perseguir la equidad12.
Algunas de las limitaciones en la generalización de los resultados del presente estudio están relacionadas con la ausencia de aleatorización de los encuestados, la menor representación en la muestra de enfermería respecto a pediatras, y por provincias, menor participación de centros de AP de Alicante.
Consideramos, con los resultados obtenidos y a pesar de las limitaciones comentadas, que la unidad básica de asistencia en Pediatría debe estar formada por enfermera y pediatra en todos los centros de salud.
Hacen falta estudios que nos permitan conocer los obstáculos que existen y las soluciones probables para que el PSI tenga eficiencia, eficacia y efectividad en el empleo de recursos humanos, evitando duplicidades en la atención.
RECOMENDACIONES
- Todas las unidades asistenciales de atención al Programa de Salud Infantil (PSI) deben estar constituidas por personal de enfermería y Pediatría.
- Las agendas de citación de enfermería tienen que ser más flexibles, para permitir su participación junto a Pediatría en los controles de salud de la primera semana y primer mes de vida del niño.
- En los programas de formación continuada deben implementarse contenidos formativos para enfermería, acordes a las necesidades detectadas en este estudio para el desempeño de su actividad en el PSI. Aumentar la formación de los profesionales de enfermería no solo aumentaría la aceptación del modelo por parte de los pediatras, sino que también habría más confianza en enfermería para asumir estas funciones.
- Proponemos debatir en los foros adecuados, asociaciones profesionales, servicios técnicos de salud infantil, etc., qué controles del PSI debe realizar enfermería y cuales enfermería y Pediatría conjuntamente.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS AP: Atención Primaria • CV: Comunidad Valenciana • GATPap: Grupo Asesor Técnico para la Pediatría de Atención Primaria • IC 95: intervalo de confianza del 95% • IC: intervalo de confianza • OR: odds ratio • PSI: Programa de Salud Infantil.
BIBLIOGRAFÍA
- Galbe Sánchez-Ventura J. ¿Son eficaces las revisiones de salud de los niños? Evid Pediatr. 2008;4:47.
- Ruiz-Canela Cáceres J. El modelo de Pediatría de Atención Primaria. Rev Pediatr Aten Primaria. 2010;12:s139-s148.
- Belamarichi PF, Gandica R, Stein RE. Drowning in a sea of advice: pediatricians and American Academy of Pediatrics Policy Statements. 2006;118:4e964-e978.
- Coker TR, Windon A, Moreno C, Schuster MA, Chung PJ. Well-child care clinical practice redesign for young children: a systematic review of strategies and tools. 2013;131:S5-25.
- Sistema Nacional de Salud España 2010. Principales datos y cifras de la Sanidad Española. Anexo 4. En: Ministerio de Sanidad y Política Social [en línea] [consultado el 29/03/2016]. Disponible en msssi.gob.es/organizacion/sns/docs/sns2010/Sistema_Nacional_de_Salud_2010.pdf
- Domínguez Aurrecoechea B, Valdivia Jiménez C. La Pediatría de Atención Primaria en el sistema público de salud del siglo XXI. Informe SESPAS 2012. Gac Sanit. 2012;26:82-7.
- Laurant M, Reeves D, Hermens R, Braspenning J, Grol R, Sibbald B. Sustitución de médicos por enfermeras en la Atención Primaria (revisión Cochrane traducida). En: La Biblioteca Cochrane Plus [en línea] [consultado el 29/03/2016]. Disponible en: www.bibliotecacochrane.com/BCPGetDocumentForPrint.asp?DocumentID=CD001271
- Poghosyan L, Nannini A, Stone PW, Smaldone A. Nurse practitioner organizational climate in Primary Care settings: implications for professional practice. J Prof Nurse. 2013;29:338-49.
- Esparza Olcina MJ. ¿Quién hace qué en el Programa de Salud Infantil? En: AEPap (ed.). Curso de Actualización Pediatría 2011. Madrid: Exlibris Ediciones; 2011. p. 29-33.
- Yoshida H, Fenick AM, Rosenthal MS. Group well-child care: an analysis of cost. Clin Pediatr (Phila). 2014;53:387-94.
- Yeung LF, Shapira SK, Coates RJ, Shaw FE, Moore CA, Boyle CA, et al. Rationale for periodic reporting on the use of selected clinical preventive services to improve the health of infants, children, and adolescents - United States. MMWR Suppl. 2014 Sep 12;63:3-13.
- Newhouse RP, Stanik-Hutt J, White KM, Johantgen M, Bass EB, Zangaro G, et al. Advanced practice nurse outcomes 1990-2008: a systematic review. Nurs Econ. 2011;29:230-50.




