Factores socioeducativos asociados a la agudeza visual baja en escolares de Perú
Mary Marcela Araujo Chumaceroa, FE Solano Zapataa, MA Vilela Estradab, Mario J. Valladares Garridoc, M Chumacero Aguilard, Christian R Mejiae
aEstudiante de Medicina. Universidad Nacional de Piura. Sociedad Científica de Estudiantes de Medicina Universidad Nacional de Piura (SOCIEMUNP). Piura. Perú.
bEstudiante de Medicina. Universidad Privada Antenor Orrego Campus Piura. Sociedad Científica de Estudiantes de Medicina Universidad Privada Antenor Orrego (SOCEM UPAO-PIURA). Piura. Perú.
cUnidad de Investigación en Enfermedades Emergentes y Cambio Climático (Emerge). Universidad Peruana Cayetano Heredia. Lima. Federación Latinoamericana de Sociedades Científicas de Estudiantes de Medicina (FELSOCEM). Unidad de Apoyo a la Docencia e Investigación(UADI). Hospital de la Amistad Perú Corea II-2. Santa Rosa. Piura. Perú.
dMédico en Jefe. CS San José. Piura. Perú.
eEscuela de Medicina Humana. Universidad Continental. Huancayo. Escuela de Postgrado. Universidad Privada Antenor Orrego. Trujillo. Perú.
Correspondencia: MM Araujo. Correo electrónico: marymarcela06@gmail.com
Cómo citar este artículo: Araujo Chumacero MM, Solano Zapata FE, Vilela Estrada MA, Valladares Garrido MJ, Chumacero Aguilar M, Mejia CR. Factores socioeducativos asociados a la agudeza visual baja en escolares de Perú. Rev Pediatr Aten Primaria. 2015;17:e261-e266.
Publicado en Internet: 23-11-2015 - Número de visitas: 28996
Resumen
Introducción: para que los estudiantes puedan adquirir el conocimiento adecuadamente, deben tener una correcta salud física y mental. Se realizó un estudio para determinar los factores socioeducativos asociados a la agudeza visual baja en escolares de educación primaria del Colegio Nacional de San Pedro (Piura, Perú).
Material y métodos: mediante un estudio transversal analítico que incluyó a estudiantes de Educación Primaria. La variable principal fue la agudeza visual baja, considerando así a los que tenían valores mayores a 20/25 según la evaluación con la cartilla de Snellen. Se obtuvieron los valores p, las razones de prevalencia y sus intervalos de confianza al 95% mediante los modelos lineales generalizados.
Resultados: en total se evaluaron 599 estudiantes, el 17% (99) mostraron agudeza visual baja. El sexo no estaba relacionado con la agudeza visual baja (p=0,832). Al aumentar la edad se observó que los niños que tuvieron entre 8-10 y 11-15 años tuvieron un 46% (p=0,005) y un 68% (p<0,001) menos de prevalencia de agudeza visual baja, respectivamente, en comparación con los de 5-7 años. Conforme fue aumentando el grado académico hubo menos prevalencia de agudeza visual baja.
Conclusiones: se concluye que uno de cada seis estudiantes tuvo una discapacidad visual y se asoció a su edad y grado académico. Esto los hace más propensos a problemas en sus calificaciones, que puede repercutir para el resto de su vida. Esto debe ser tomado en cuenta por las instituciones que vigilen la correcta educación de los menores.
Palabras clave
● Agudeza visual ● Emetropía ● Estudiantes ● PerúINTRODUCCIÓN
La agudeza visual baja es un problema educativo de interés mundial1, evitable con métodos de detección temprana y cooperación activa por parte de los padres2. El Modelo de Atención Integral de Salud (MAIS), que constituye el actual marco de referencia para la atención en salud de Perú, provee de cuidados esenciales para atender las necesidades de salud del niño y el adolescente haciendo uso de una evaluación integral, la que incluye la agudeza visual como un indicador trazador del estado de salud ocular de un individuo1,3.
La mayoría de estudios del tema realizan descripciones, como un estudio en nuestro medio, que encontró que el 46% de niños de una población escolar en Lima mostraban ametropías4, reflejando que los defectos visuales no son solo un asunto de adultos y ancianos, sino también se presentan desde edades tempranas. Por otro lado, un estudio en Cuba dio a conocer que un 70% de las consultas de niños al oftalmólogo eran debido a alteraciones en la agudeza visual5. No se han encontrado muchos estudios que determinen los factores asociados a los problemas de visión, pero sí aquellos que describen problemas específicos, como un estudio sobre la retinopatía congénita que fue realizado en el Hospital Las Mercedes de Chiclayo (Perú)6.
Existe poca bibliografía médica sobre el tema, a pesar de ser este de gran importancia para el campo preventivo y promocional en la salud de niños y adolescentes, ya que afecta directamente al ámbito académico de los mismos7,8. Por ello se convierte en un problema latente para la salud pública; es por todo lo anteriormente mencionado que nuestro objetivo fue el determinar los factores socioeducativos asociados a la agudeza visual baja en alumnos de Primaria de un colegio público del norte peruano.
MATERIAL Y MÉTODOS
Se realizó un estudio transversal analítico en el Colegio Nacional San Pedro de Piura, Perú. La muestra estuvo constituida por 655 escolares con edades comprendidas entre 5 a 15 años, de los cuales se incluyeron a todos aquellos que tenían consentimiento de sus padres y/o tutores, excluyendo a los estudiantes que no asistieron el día del examen y a aquellos que no pudieron entender y/o seguir estrictamente las instrucciones. Se calculó un tamaño muestral mínimo de 439 estudiantes para una población infinita, con una frecuencia de problemas visuales del 46%4 e hipotetizando una diferencia estadística entre grupos del 10%, con una significancia estadística del 95% y una potencia del 99% (cálculo realizado con el programa Epitable® versión 3.1). Se encuestó a un total de 599 niños y adolescentes (tasa de rechazo del 8,5%).
La variable dependiente fue la agudeza visual, calificada mediante el uso de los principios de la tabla de Snellen, que aporta la detección de los defectos visuales de manera sencilla (con una sensibilidad del 85% y especificidad del 96% para los optotipos de la E Snellen)9; además, se usaron diseños de letras y la E Snellen, esta último en caso de que el niño tuviera dificultad para reconocer las letras o no supiera leer. Se consideró a los que tuvieran una medida de 20/20 como agudeza visual óptima y la normal hasta 20/25; todos los otros valores se consideraron como agudeza visual baja.
Para la estadística analítica se consideró como variable resultado el tener agudeza visual baja; esto se cruzó con el sexo, la edad (categorizada en 5-7 años, 8-10 años y 11-15 años) y el grado académico (de primero a sexto año).
La recolección de datos preprueba se realizó durante cinco días y por aulas. La prueba fue realizada por estudiantes de Medicina (previa capacitación por médicos especialistas) y tuvo lugar en el patio del colegio. Para esto se contó con una apropiada iluminación natural, se colocó a los niños a una distancia de seis metros respecto al tablero de Snellen y se evitaron las distracciones; se evaluó cada ojo por separado, empleando un oclusor en el ojo contrario10.
Todos los datos se pasaron a una ficha de recolección en el programa Microsoft Excel® (versión 2010 para Windows®). El análisis de los datos se realizó mediante el programa Stata® v.11.1. Se aplicó estadística descriptiva, para las variables cualitativas se usó distribución de frecuencias absolutas y relativas, para las variables cuantitativas se realizaron medias con desviación estándar o mediana con sus rangos intercuartílicos, según corresponda a su tipo de distribución.
Para la estadística analítica, se usaron los modelos lineales generalizados (con la familia Poisson y la función de enlace log) para encontrar los valores p, las razones de prevalencia (RP) y sus respectivos intervalos de confianza al 95% (IC 95). Se consideró un valor p<0,05 como estadísticamente significativo.
Se consideró el consentimiento informado del padre o tutor por escrito, además de la aprobación de cada estudiante, que se obtuvo antes del examen (asentimiento informado). Todo niño que en la valoración de la agudeza visual no se encontrara en el rango de lo normal fue derivado a un oftalmólogo especialista, para la determinación de sus causas y su corrección visual.
RESULTADOS
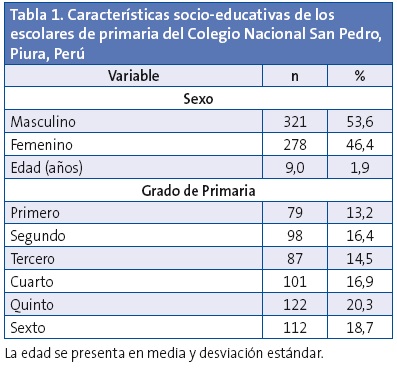
De los 599 alumnos, la edad promedio fue de 8,99 años (desviación estándar [DE] de 1,86) y el 53,6% fueron hombres. El grado con mayor número de alumnos fue el quinto (20,3%) (Tabla 1).
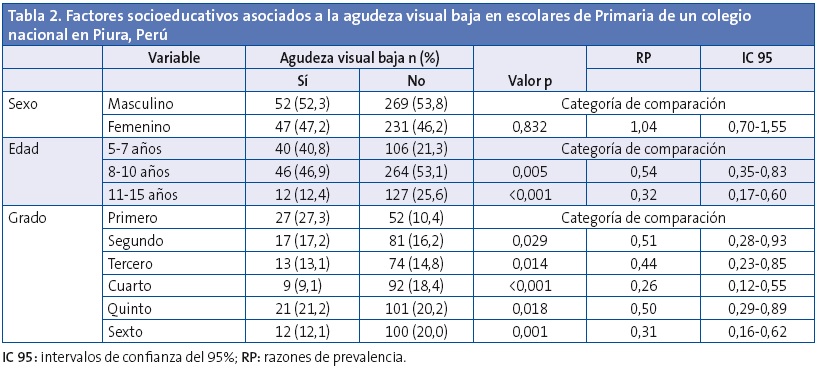
Cuando se obtuvieron los valores de asociación de la agudeza visual baja según las características socioeducativas, se encontró que el sexo no estaba relacionado con la agudeza visual baja (p=0,832). Al aumentar la edad se encontró una asociación estadísticamente significativa; los niños de los grupos etarios de 8-10 y 11-15 años tuvieron 46% (p=0,005) y 68% (p<0,001) menos prevalencia de tener agudeza visual baja, respectivamente, en comparación con los niños de 5-7 años de edad. Por último, según el grado de estudio, conforme fue aumentando el grado académico, hubo menos prevalencia de agudeza visual baja, en segundo un 49% menos, en tercero un 56% menos, en cuarto un 74% menos, en quinto un 50% menos y en sexto un 69% menos. Los valores se muestran en la Tabla 2.
DISCUSIÓN
De acuerdo con los resultados de nuestro estudio, el 16,5% de niños presentó agudeza visual baja; esto se contrapone con estudios similares realizados en poblaciones extranjeras, como en el caso de la India (4,3%)11 y Argentina (10,7%)2. También contradice un estudio realizado en Apurímac, Perú, en el cual apenas un poco más del 6% presentó defectos refractivos, pero fue realizado en una población con un menor rango de edades que nuestro estudio (entre 3 y 11 años de edad)12. Nuestros resultados sí han coincidido con lo encontrado por un estudio que se realizó en Colombia en niños de 7 a 11 años, cuya prevalencia de agudeza visual baja fue 14,2%13. Otro estudio encontró una frecuencia similar a la nuestra (18,1%), cuando comparaba dos tipos de cartilla para la evaluación de la agudeza visual14.
Encontramos que la edad de los participantes estuvo asociada a su agudeza visual: a mayor edad se halló menor prevalencia de agudeza visual baja. Esto difiere con estudios similares realizados en poblaciones de Asia (China y Arabia Saudí), que señalan que la agudeza visual baja incrementa conforme avanza la edad de los niños15,16. Asimismo, no se encontró una diferencia estadística entre la agudeza visual baja con respecto a la edad de los niños en un grupo de niños menores de 15 años de Oceanía17 ni en otro estudio realizado en Vietnam18. No se encontraron estudios con poblaciones similares a la nuestra para comparar los resultados hallados según la variación de la edad, lo que deja abierta la posibilidad a realizar mayor cantidad de investigación y con mayor número de poblaciones.
El porcentaje además varió según el rango de edad, en nuestro estudio, tres cuartas partes de la población con agudeza visual baja son niños, lo que manifiesta un deterioro visual en comparación de los adolescentes. Específicamente, a los seis años de edad se encontró una prevalencia del 35% de agudeza visual baja, lo cual verificó estudios anteriores, que toman como referencia los seis años como punto determinante para la aparición de problemas visuales2,16,19,20. Se encontró una asociación directa entre los problemas de agudeza visual y el el grado académico. Esto es corroborado con los hallazgos en un país en vías de desarrollo de África, en donde encontraron que los errores de refracción se asociaron con el mayor grado académico de los niños21.
No se encontró asociación entre la agudeza visual baja y el sexo del niño, lo cual también fue observado en un estudio similar en la isla de Fiji17.
Se tuvieron las siguientes limitaciones: no se pudieron medir mayor cantidad de variables o hacer comparaciones con otras poblaciones; además, el tipo de muestreo genera que los valores p y los intervalos de confianza se utilicen solo como referencia para la fuerza de asociación. A pesar de esto, nuestros resultados son importantes por ser uno de los pocos en nuestra región que buscan asociaciones, lo que puede servir para futuros trabajos.
En base a los datos analizados, se concluye que la frecuencia de agudeza visual baja es alta en los escolares de un colegio del norte peruano; además, esto se asocia con la edad y el grado académico de los estudiantes.
Estos resultados ayudarán a incentivar más trabajos de investigación, que engloben otros aspectos relacionados con la agudeza visual, como es el campo del aprendizaje y el rendimiento escolar. Se recomienda a las instituciones encargadas el supervisar la valoración oftalmológica de los educandos, para la detección y tratamiento temprano de estos defectos con la ayuda de un profesional de la salud, para así evitar su progreso y las consecuencias generadas de una mala recepción de la educación básica.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS: DE: desviación estándar; IC 95: intervalo de confianza del 95%; MAIS: Modelo de Atención Integral de Salud; SIS: Seguro Integral de Salud.
AGRADECIMIENTOS
Los autores agradecen a la directiva del Colegio Nacional San Pedro (Piura, Perú) que permitió hacer esta investigación. También al personal del centro de salud de San Pedro (Piura, Perú) que nos proporcionó los instrumentos necesarios para la evaluación de la agudeza visual, nos capacitó en la evaluación de esta y colaboró con la recogida de los datos.
BIBLIOGRAFÍA
- Guía Nacional de Operativización del Modelo de Atención Integral de Salud. En: Ministerio de Salud [en línea] [consultado el 17/11/2015]. Disponible en http://goo.gl/gffUXD
- Verrone P, Simi M. Prevalencia de agudeza visual baja y trastornos oftalmológicos en niños de seis años de la ciudad de Santa Fe. Arch Argent Pediatr. 2008;106:328-33.
- Medicus Mundi. MAIS. Un modelo incluyente e integral bajo un concepto de derecho a la salud (2011-2014). En: Salud Integral Incluyente [en línea] [consultado el 17/11/2015]. Disponible en http://saludintegralincluyente.com/previos/mais-peru.html
- Carrión C, Gálvez F, Morales J, Guevara V, Jaramillo R, Gazzani M. Ametropía y ambliopía en escolares de 42 escuelas del programa Escuelas Saludables en la DISA II, Lima. Perú, 2007-2008. Acta Med Per. 2009;26:17-21.
- García E, Estrada Y, Aparicio A. Frecuencia de ametropías en niños. Rev Cubana Pediatr. 2010;82:28-37.
- Gutiérrez C, Wekselman EFV, Herrerera PR, Palacios CL. Retinopatía de la prematuridad en el Hospital Regional Docente Las Mercedes. Chiclayo 2007-2009. Rev Cuerpo Méd. HNAAA. 2012;5:30-2.
- Toledo C, Paiva A, Camilo G, Maior M, Leite I, Guerra M. Early detection of visual impairment and its relation with school effectiveness. Rev Assoc Med Bras. 2010;56:415-9.
- Costa Lança C, Serra H, Prista J. Reading performance in children with visual function anomalies. Int J Ophthalmol Clin Res. 2014;1:1-5.
- Méndez M, Delgado J. Oftalmología: exploración del niño estrábico; detección precoz. Detección precoz de los trastornos de refracción y ambliopía. Rev Pediatr Aten Primaria. 2011;13:163-80.
- Manual de Atención Primaria de salud ocular. En: Instituto Nacional de Oftalmología [en línea] [consultado el 17/11/2015]. Disponible en www.ino.org.pe/menu/pnlcc/manual_atencion_salud_ocular.pdf
- Ghosh S, U Mukhopadhyay, Maji D, Bhaduri G. Visual impairment in urban school children of low-income families in Kolkata, India. Indian J Public Health. 2012;56:163-7.
- Latorre S, Gil D, Enciso O, Phelan A, Garcia A, Kohler J. Reducing visual deficits caused by refractive errors in school and preschool children: results of a pilot school program in the Andean region of Apurimac, Peru. Glob Health Action. 2014;7:22656.
- López Ceromeca M. Evaluación de la agudeza visual en estudiantes de una institución educativa de la ciudad de Santiago Cali 2011. Rev Medica Fusm. 2013;1:33-8.
- Peña J, Rubiano D, López M. Concordancia entre el test de números de Snellen y el test de números de Lea en niños entre cuatro y siete años. Cien Tecnol Salud Vis Ocul. 2012;10:115-21.
- Wu JF, Bi HS, Wang SM, Hu YY, Wu H, Sun W, et al. Refractive error, visual acuity and causes of vision loss in children in Shandong, China. The Shandong Children Eye Study. PLoS ONE. 2013;8:e82763.
- Wadaani FAA, Amin TT, Ali A, Khan AR. Prevalence and pattern of refractive errors among primary school children in Al Hassa, Saudi Arabia. Glob J Health Sci. 2012;5:125-34.
- Cama A, Sikivou B, Keeffe J. Childhood visual impairment in Fiji. Arch Ophthalmol. 2010;128:608-12.
- Paudel P, Ramson P, Naduvilath T, Wilson D, Phuong HT, Ho SM, et al. Prevalence of vision impairment and refractive error in school children in Ba Ria – Vung Tau province, Vietnam. Clin Experiment Ophthalmol. 2014;42:217-26.
- García L, Bernardo J. Prevalencia y caracterización de errores refractivos en niños de 6 a 12 años, que viven en la Delegación Gustavo A. Madero del Distrito Federal. En: Instituto Politécnico Nacional [en línea] [consultado el 17/11/2015]. Disponible en http://goo.gl/ZIBRQ0
- Figueroa LF, Molina N, López Y, Bermúdez M. Agudeza visual, error refractivo, curvatura corneal, visión cromática y estereopsis en niños entre tres y siete años en la localidad de Chapinero de la ciudad de Bogotá. Cien Tecnol Salud Vis Ocul. 2013;11:55-65.
- Sewunet SA, Aredo KK, Gedefew M. Uncorrected refractive error and associated factors among primary school children in Debre Markos District, Northwest Ethiopia. BMC Ophthalmol. 2014;14:95.





