Vol. 17 - Num. 67
Originales
Enuresis nocturna. Estudio epidemiológico en población escolar
Carmelo Gutiérrez Abada, M. N. San José Callejaa, M Castroviejo Espinosab, R Sánchez Gutiérrezc, E Ardela Díezd, J. A. Cordero Guevarae
aPediatra. CS Las Huelgas. Burgos. España.
bEnfermera. CS Las Huelgas. Burgos. España.
cEnfermera. HospitalHospital Universitario de Burgos. Burgos. España.
dCirujano Pediátrico. Hospital Universitario de Burgos. Burgos. España.
eTécnico de Salud. Gerencia de Atención Primaria de Burgos. Burgos. España.
Correspondencia: C Gutiérrez. Correo electrónico: cgapalencia@yahoo.es
Cómo citar este artículo: Gutiérrez Abad C, San José Calleja MN, Castroviejo Espinosa M, Sánchez Gutiérrez R, Ardela Díez E, Cordero Guevara JA. Enuresis nocturna. Estudio epidemiológico en población escolar. Rev Pediatr Aten Primaria. 2015;17:227-34.
Publicado en Internet: 03-09-2015 - Número de visitas: 20619
Resumen
Introducción: la enuresis nocturna (EN) es un problema de salud infantil frecuente, con repercusión personal y social, que requiere un manejo adecuado y personalizado por parte de los profesionales sanitarios. Se ha realizado un estudio cuyo objetivo es establecer la prevalencia de EN en la ciudad de Burgos (España) en población pediátrica entre siete y diez años de edad.
Pacientes y métodos: estudio observacional transversal en el que se han obtenido datos de una muestra aleatoria de niños escolarizados entre segundo y quinto curso de Educación Primaria Obligatoria en la ciudad de Burgos mediante la cumplimentación de una encuesta.
Resultados: se ha obtenido una prevalencia de EN del 7,3%. La EN es más frecuente en varones, con antecedentes familiares de enuresis nocturna, con algún tipo de enfermedad crónica, que asocian trastornos del sueño y del comportamiento y con bajo rendimiento escolar.
Conclusiones: la prevalencia es menor a la de otras poblaciones de características similares. Los niños con EN de Burgos presentan características epidemiológicas semejantes a las de otras poblaciones. La EN es un problema de salud infradiagnosticado en nuestro medio.
Palabras clave
● Enuresis nocturna ● Epidemiología ● Factor de riesgo ● NiñosINTRODUCCIÓN
La enuresis nocturna (EN) es una entidad clínica definida según la International Children's Continence Society (ICCS) en su última revisión como los episodios de incontinencia urinaria producidos durante el sueño en niños de cinco o más años1. La EN se clasifica en varias entidades dependiendo del momento de aparición de los escapes de orina (primaria o secundaria) y de la asociación o no a algún tipo de patología orgánica que la origine (no monosintomática o monosintomática, respectivamente). Aún hoy existen discrepancias en cuanto a la edad de diagnóstico, aunque en general se consideran los cinco años como la edad a partir de la cual podemos hablar propiamente de EN1-4.
Es un problema frecuente en las consultas de pediatría de Atención Primaria (AP), con una prevalencia estimada entre el 8 y el 15%4-6. El origen o la causa de la EN es aún desconocido y, en general, se considera multifactorial (agregación familiar, disfunción esfinterovesical, alteración neurohormonal, factores psicológicos, factores socioeconómicos, alteraciones del patrón del sueño, etc.). Esto supone que al abordar en la consulta de Pediatría a un paciente con EN nos enfrentemos a un problema de salud complejo cuyo planteamiento terapéutico ha de ser individualizado4,5,7. Excluyendo la posible afectación física (alteraciones en genitales, vías urinarias, columna vertebral, etc.), existe la afectación psicológica que la EN puede originar y que, en ocasiones, es difícil de valorar y abordar4.
Se ha diseñado un estudio epidemiológico para conocer mejor las características de la población infantil de la ciudad de Burgos (España) que padece EN y evidenciar los principales factores de riesgo asociados a ella.
PACIENTES Y MÉTODOS
La población de referencia fueron los niños de entre siete y diez años de edad escolarizados en centros públicos, concertados y/o privados de la ciudad de Burgos en el curso escolar 2013/2014. Dicha población según datos del Instituto Nacional de Estadística (INE) del año 2012 se estimó en unos 5500 niños. Para obtener el tamaño muestral se calculó una prevalencia estimada del 15%, una precisión del 2%, un intervalo de confianza del 95%, un porcentaje de pérdidas del 30% y el efecto de aleatorización por estratos. Con dichos datos se obtuvo un tamaño muestral de 1485 niños.
La Dirección Provincial de Educación de Burgos aportó el listado de centros escolares de la ciudad de Burgos en los que se impartían clases de Educación Primaria Obligatoria (EPO). Del total de centros existentes, 41, y tras obtener la conformidad por parte de los directores de los centros escolares, se obtuvo un total de 31 centros escolares participantes. Cada centro escolar participante aportó información sobre el número y el tamaño de las aulas entre 2.º y 5.º de EPO. Con dicha información se hizo una estratificación por tamaño de las aulas, tras la cual se realizó la selección aleatoria de las mismas.
Las encuestas fueron entregadas en los centros escolares a los niños y sus familias y fueron completadas tras obtener el consentimiento informado por parte de sus representantes legales. Las encuestas eran anónimas, incluían 43 ítems y se estructuraron en cuatro apartados: datos de filiación del paciente y su familia, datos sanitarios del paciente, datos relacionados con los escapes de orina y datos familiares en relación con los escapes de orina.
Una vez recogidas las encuestas, se desecharon las que estaban sin contestar o mal completadas y aquellas que no cumpliesen criterios de inclusión (mayores de diez años). Posteriormente se incluyeron los datos en una base de datos informatizada y se procesaron mediante el programa informático SPSS® v17.0. Para las variables cualitativas se utilizó el estadístico χ2 y para las cuantitativas la t de Student. Con las variables cualitativas estadísticamente significativas se realizó cálculo de odds ratio y con las cuantitativas el coeficiente de correlación de Pearson. Se consideró estadísticamente significativo un valor de “p” menor de 0,05.
RESULTADOS
El número final de encuestas entregadas fue de 1468. La tasa de respuesta fue del 80,1%. Posteriormente se invalidaron 95 encuestas por estar mal o no contestadas y por edad mayor a diez años. Finalmente se obtuvieron 1081 encuestas válidas, lo que supone un 73,6% del total de encuestas entregadas y un 19,6% del total de población entre siete y diez años de la ciudad de Burgos.
La muestra presentó una distribución simétrica con respecto al sexo (49,2% varones y 50,8% mujeres), con una edad media de 9,07 años. El número medio de hermanos era de 1,56 (un 18,2% no tenían hermanos). La mayor parte de los individuos era de nacionalidad española (94,7%), un 1,1% de nacionalidad china, otro 1,1% de nacionalidad rumana y el resto (3,1%) de otras nacionalidades. El 90,8% de los padres de los niños estaban casados o eran pareja de hecho, el 6,8% separados o divorciados y el 2,4% eran hijos de progenitor único. En cuanto a los antecedentes personales de los niños, se evidenció que un 11,2% habían padecido alguna infección de orina, un 1,7% padecían algún tipo de enfermedad renal o de vías urinarias, un 6,3% eran prematuros (igual o menos de 36 semanas de gestación), un 22,3% padecían algún tipo de trastorno del sueño (pesadillas frecuentes, terrores nocturnos, apneas respiratorias, dificultades importantes para la conciliación del sueño), un 3,7% estaban diagnosticados de algún tipo de alteración del comportamiento (el 84% de ellos de trastorno por déficit de atención e hiperactividad [TDAH]) y hasta un 6,5% de los padres consideraban que sus hijos presentaban bajo rendimiento escolar.
El número de niños con algún tipo de escape de orina fue de 99 (9,2%). De ellos, un 42,4% presentaban escapes de orina a diario, un 6,1% al menos uno a la semana, un 24,2% dos o tres escapes al mes y un 27,3% un escape al mes o menos. La prevalencia de EN en la muestra fue del 7,3%: el 2% corresponde a enuresis nocturna primaria monosintomática (ENPM), un 4,1% a enuresis nocturna primaria no monosintomática (ENPNoM) y un 1,2% a enuresis nocturna secundaria (ENS). El resto de niños con escapes de orina se distribuyó en incontinencia urinaria diurna (0,9%) e incontinencia urinaria diurna y nocturna (1,1%).
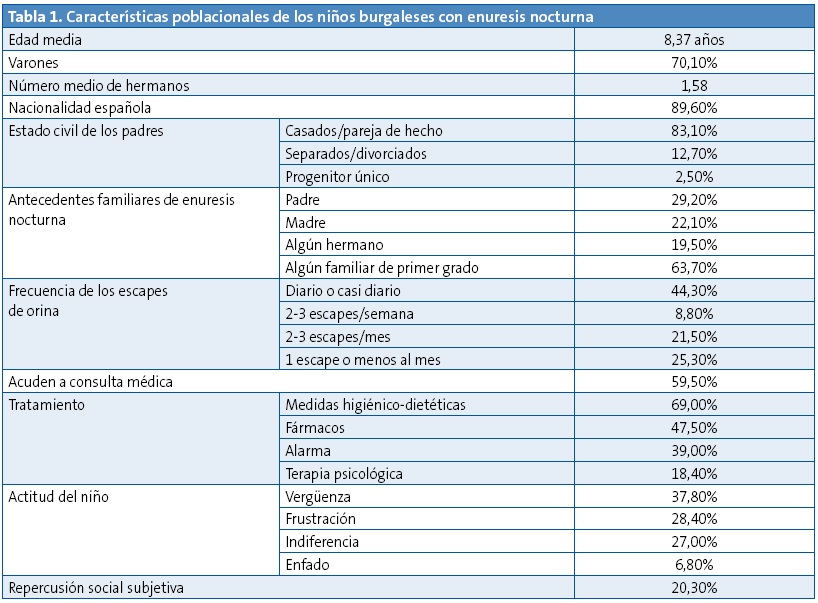
Las características poblacionales de los niños con EN se exponen en la Tabla 1. Cabe destacar, en comparación con el resto de la muestra, que hay mayor proporción de varones, de hijos de padres separados o divorciados y de antecedentes familiares de EN. Por el contrario, no hubo diferencias significativas en cuanto a la edad media de los niños con enuresis con respecto a los del resto de la muestra ni tampoco en el número medio de hermanos ni la nacionalidad. Además, cabe destacar que solo un 59,5% de los niños con escapes de orina habían acudido alguna vez a la consulta de Pediatría o de enfermería pediátrica por dicho problema. De ellos, un 69% de los niños habían recibido algún tipo de tratamiento, destacando las medidas higiénico-dietéticas y la desmopresina como tratamientos más frecuentes. Por último es reseñable que solo un 20,3% de los niños con EN reflejasen de forma subjetiva que los escapes de orina les repercutían personalmente produciéndoles algún tipo de perjuicio (inseguridad o baja autoestima, limitación de vida social, etc.).
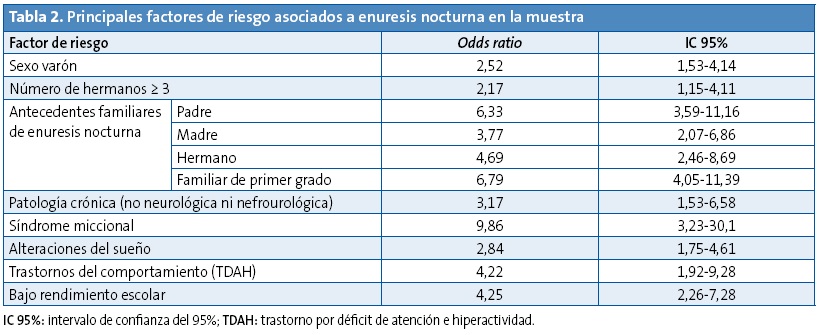
En cuanto a los factores de riesgo asociados a la EN evaluados, se evidenció relación estadísticamente significativa con varios de ellos. Destaca especialmente la relación con los antecedentes familiares de EN, la presencia de síndrome miccional y la existencia de trastornos del comportamiento (casi exclusivamente TDAH) y bajo rendimiento escolar (Tabla 2). No se evidenció relación con otros factores como el estreñimiento, la obesidad, la prematuridad ni con la existencia de antecedentes de infección de orina o enfermedad renal (seguramente por bajo número de niños con dichas afecciones). En cuanto a la edad, se objetivó relación estadísticamente significativa con un coeficiente de correlación de Pearson negativo (-2,53; p < 0,01).
En cuanto a la actitud de los padres en relación a los escapes de orina, se evaluó la reacción que estos tenían ante los escapes (indiferencia, frustración, vergüenza, enfado o refuerzo positivo). No se encontró preeminencia de ninguna de las actitudes ni en la madre ni el padre, distribuyéndose de forma irregular en los niños con escapes de orina. Tampoco se evidenció diferencia en cuanto al nivel de estudios de los padres comparando el grupo de niños con EN y el resto de niños.
DISCUSIÓN
Cuando hablamos de enuresis nocturna nos encontramos primero ante la dificultad de definirla. Diversos son los criterios utilizados para ello dependiendo de la definición que utilicemos dentro de las emitidas por los diversos organismos y sociedades competentes (ICCS, Manual diagnóstico y estadístico de los trastornos mentales [DSM-5], Clasificación internacional de enfermedades [CIE-10], etc.)1-4,8. Esta disparidad de criterios hace complejo comparar distintos estudios y obtener conclusiones totalmente válidas.
En nuestro caso hemos utilizado la última definición realizada por uno de estos organismos, la del ICCS de 20141. La prevalencia obtenida en la ciudad de Burgos es menor a la de otras poblaciones de características similares9-19. Esta diferencia es mayor si la comparamos con poblaciones rurales o procedentes de países en vías de desarrollo. Esta peculiaridad hace relevante el hecho de que la prevalencia de EN dependa en gran medida de factores culturales y sociales. Estos factores socioculturales hacen que se comience de manera más tardía el control de esfínteres y que se considere la EN como un problema exclusivamente de desarrollo o maduración sin repercusiones psicosociales15,20.
Si comparamos las características poblacionales de los niños con EN nos encontramos que la mayoría son varones (70,1%), circunstancia frecuentemente observada en otros estudios, especialmente a edades tempranas, ya que en niños mayores la proporción de sexos se va igualando. Esto parece tener relación con un desarrollo psicomotor y de adquisición de habilidades más lento en los niños que en las niñas9,11,12,16,18-20. Otra circunstancia que se ha relacionado con la EN es el hecho de tener más hermanos12,16,17. Parece haber una relación entre el número de hermanos y la EN, como hemos observado también en nuestro estudio. La existencia de antecedentes familiares de EN es otro factor etiopatogénico estudiado. En nuestro estudio hemos encontrado un porcentaje de antecedentes familiares de EN alto (2/3 de los niños con EN tienen antecedentes de EN en algún familiar de primer grado), siendo mayor cuando es el padre el que presenta el antecedente enurético. Este aspecto coincide con lo observado en la literatura médica, aunque en ella hay disparidad de porcentajes y, en nuestro caso, es uno de los más altos9,11-13,16,17,21. Esto evidencia la existencia de agregación familiar en relación a la EN, aunque se duda en cuanto al verdadero origen de la misma. Se han postulado factores genéticos como los causantes de dicha asociación, pero también se han planteado factores culturales. Estos factores culturales condicionan que cada familia afronte la EN desde un planteamiento distinto y con una importancia o relevancia particular. De esta manera se determina que el comienzo tardío en el entrenamiento del control de esfínteres pueda condicionar el retraso del mismo y dar lugar a la existencia de EN9,21,22.
Es destacable la asociación entre la EN y la existencia de síndrome miccional (polaquiuria, tenesmo vesical, urgencia miccional, maniobras de retención). Es el factor de riesgo con mayor potencia de asociación de los estudiados, mayor también que lo observado en otros estudios10. Dicha asociación plantea la duda de la existencia o no de problemas urovesicales que puedan ser origen también de la enuresis. Estos niños con presencia de síndrome miccional y enuresis se etiquetarían dentro de la enuresis primaria no monosintomática y la enuresis secundaria.
En este estudio se ha observado también una mayor presencia de trastornos del sueño y del comportamiento en los niños enuréticos. Como trastornos del sueño incluimos cualquier alteración relacionada con el sueño y que altera la calidad y/o cantidad del mismo. De esta manera se incluyeron las pesadillas, terrores nocturnos, ronquidos importantes, apneas o dificultades importantes en la conciliación del sueño. En nuestra serie obtuvimos un 44% de niños con EN que presentan estos trastornos del sueño. Este dato es superior al del resto de la muestra (22,3%) y también mayor que lo observado en otros estudios13,22-24.
En relación con los trastornos del comportamiento, observamos que en los niños enuréticos que tenían además diagnosticados trastornos del comportamiento, todos eran TDAH. En concreto había 14 niños con TDAH, un 18% de los niños enuréticos, porcentaje muy superior al del total de la muestra (3,7%). Este aspecto nos ha resultado llamativo. Parece establecerse una cierta relación entre la EN y el TDAH, circunstancia observada en otros estudios13. No está claro cuál es el fenómeno primario, si la EN o el TDAH, pero parece razonable que si nos encontramos un niño en la consulta con EN interroguemos sobre la existencia de síntomas de TDAH y viceversa. De la misma manera, hemos podido establecer relación en nuestros niños entre la EN y el bajo rendimiento escolar. Este aspecto era determinado por los padres de manera subjetiva mediante una pregunta directa, no establecimos criterios objetivos de bajo rendimiento escolar. De la misma manera que sucede con el TDAH, evidenciamos que hay más niños enuréticos con bajo rendimiento escolar que niños no enuréticos con bajo rendimiento escolar (21% frente a 6,5%). Como con el TDAH, resulta difícil establecer cuál es la causa y cuál la consecuencia17,22. Seguramente sean dos circunstancias relacionadas entre sí, en las que unas veces sea la causa la EN (que origine baja autoestima o inseguridad que dé lugar a un menor rendimiento escolar del esperado) y otras veces sea el origen el bajo rendimiento escolar secundario a algún trastorno del aprendizaje o un desarrollo psicomotor retrasado que además cause la EN.
Hubo otros factores de riesgo estudiados en los que no se objetivó relación estadísticamente significativa, como el estreñimiento, la obesidad, la prematuridad y el antecedente de infección de orina.
Al evaluar la actitud seguida por los padres de niños enuréticos, se observó que solo el 59% de los niños con EN habían acudido alguna vez al pediatra o a la enfermera por dicho motivo. Parece haber todavía en nuestro medio circunstancias que limitan el acceso de estos niños a la consulta. Creemos que esto es debido a falta de información de los padres sobre la EN y a un cierto grado de reticencia o tabú de estos para consultar al pediatra sobre los escapes de orina. En otros estudios también se ha visto esta circunstancia que unida, en algunos casos, a un nivel de estudios bajo de los padres (no en nuestro estudio) hace que la EN sea infradiagnosticada15,17,18,20,25. Por otra parte, no todos los niños que acuden a consulta son evaluados y tratados de forma adecuada por los profesionales sanitarios. Solo a un 71% de estos niños se les realiza algún tipo de prueba médica, lo cual limita en cierto modo el adecuado manejo del niño y, por tanto, disminuye la eficacia del tratamiento pautado4,5. Además, solo a un 73% de los niños enuréticos vistos en las consultas se les da algún tipo de tratamiento. Estas dos circunstancias indican que no siempre los niños enuréticos de nuestro medio son adecuadamente evaluados y tratados11.
Otro fin de este estudio era valorar el grado de afectación que la EN producía en los niños de nuestra ciudad y sus padres. Sorprende encontrar solo un 20,1% de niños con EN que referían que dicho problema les suponía algún tipo de perjuicio o les repercutía en su vida social, cuando solo un 27% de ellos expresaba un sentimiento de indiferencia ante los escapes de orina. El resto (73%) expresaban que los escapes de orina les producía algún tipo de sentimiento desagradable (enfado, frustración o vergüenza). Este aspecto nos ha parecido complejo de valorar sin poder llegar a obtener una conclusión clara. Quizás pueda ser debido a un retraso en el inicio de actividades colectivas (campamentos, excursiones, etc.) que no haya hecho relevante aún la existencia de la EN. En otros estudios los datos obtenidos a este respecto han sido dispares, pero en general se objetivaba una mayor repercusión en los niños que en nuestro medio11.
CONCLUSIONES
La enuresis nocturna se ha convertido en los últimos años en un trastorno más conocido por parte de los pediatras y enfermeras de pediatría. Además, los padres están más sensibilizados ante dicho problema. Pero aún estamos lejos de considerar a la enuresis nocturna como un problema de salud de diagnóstico precoz y de manejo adecuado, como hemos visto en este estudio.
En la ciudad de Burgos, la prevalencia de EN ha sido menor que lo observado en la literatura médica. Esto puede ser debido a un mayor conocimiento y control del problema en las consultas pediátricas. Pero aún existe un margen amplio de mejora, como demuestra el alto porcentaje de ausencia de consultas por dicho problema. Las características poblacionales y los factores de riesgo de los pacientes con EN son similares a los de otras poblaciones similares. Únicamente cabe destacar la mayor presencia de síndrome miccional en nuestro medio, con una importancia y repercusión sobre el paciente con EN difícil de medir.
Es importante que la EN sea bien conocida por parte de los profesionales sanitarios que atienden a los niños (pediatras, enfermeras de pediatría, etc.) y por parte también de los padres y personal educativo. Esto requiere que los profesionales sanitarios hagamos un esfuerzo por comunicar de forma adecuada a los niños, padres y profesores la importancia de la enuresis nocturna. Además, hemos de romper el tabú o la reticencia en torno a la EN existente aún en nuestra sociedad. Todo ello debe ir dirigido a aumentar el bienestar del niño que padece la EN con el fin de que mejore o desaparezca precozmente.
En ningún momento hemos de olvidar la posible repercusión personal y/o social que la EN puede tener en el niño que la padece. Es fundamental que el niño se encuentre seguro y libre de estigmas que puedan influir en su autoestima. De esta manera además de permitir una infancia más confortable ayudará a que el niño consiga adquirir más rápidamente el control de esfínteres.
FINANCIACIÓN
Estudio financiado con ayuda GRS 738/B/13 de los Proyectos de Investigación en Biomedicina de la Gerencia Regional de Salud de Castilla y León del año 2013.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS: AP: Atención Primaria (AP) • EN: enuresis nocturna • ENPM: enuresis nocturna primaria monosintomática • ENPNoM: enuresis nocturna primaria no monosintomática • ENS: enuresis nocturna secundaria • EPO: Educación Primaria Obligatoria • ICCS: International Children's Continence Society • INE: Instituto Nacional de Estadística • TDAH: trastorno por déficit de atención e hiperactividad.
AGRADECIMIENTOS
A la Dirección Provincial de Educación de la provincia de Burgos. A los centros escolares de la ciudad de Burgos participantes en el estudio por su magnífica disposición y colaboración.
BIBLIOGRAFÍA
- Austin PF, Bauer SB, Bower W, Chase J, Franco I, Hoebeke P, et al. The standardization of terminology of lower urinary tract function in children and adolescents: update report from the Standardization Committee of the International Children's Continence Society. J Urol. 2014;191:1863-1865.e13.
- American Psychiatric Association. Enuresis. Diagnostic and statistical manual of mental disorders. 5.ª edición. Washington, DC: Author; 2013.
- International Statistical Classification of Diseases and related health problems. 10th revision. En: Organización Mundial de la Salud [en línea] [consultado el 24/08/2015]. Disponible en www.who.int/classifications/icd/en/
- Van de Walle J, Rittig S, Bauer S, Eggert P, Marschall-Kehler D, Tekgul S. Practical consensus guidelines for the management of enuresis. Eur J Pediatr. 2012;171:971-83.
- Nevéus T. Nocturnal enuresis-theoretic background and practical guidelines. Pediatr Nephrol. 2011;26:1207-14.
- Ramírez-Backhaus M, Arlandis Guzmán S, García-Fadrique G, Martínez Agulló M, Martínez García R, Jiménez-Cruz JF. La enuresis nocturna. Un trastorno frecuente con una prevalencia difícil de estimar. Actas Urol Esp. 2010;34:460-6.
- Lottmann HB, Alova I. Primary monosymptomatic nocturnal enuresis in children and adolescents. Int J Clin Pract Suppl. 2007;(155):8-16.
- Schultz-Lampel D, Steuber C, Hoyer PF, Bachmann CJ, Marschall-Kehler D, Bachmann H. Urinary incontinence in children. Dtsch Arztebl Int. 2011;108:613-20.
- Lapeña López de Armentia S, Rodríguez Fernández LM, Marugán de Miguelsanz JM, Palau Benavides MT, Reguero Celada S, Gutiérrez Fernández M, et al. Enuresis nocturna primaria y secundaria. ¿Son entidades diferentes? An Esp Pediatr. 1996;44:345-50.
- Butler RJ, Golding J, Northstone K, ALSPAC Study Team. Nocturnal enuresis at 7.5 years old: prevalence and analysis of clinical signs. BJU Int. 2005;96:404-10.
- Ramírez Backhaus M, Martínez Agulló E, Arlandis Guzmán S, Gómez Pérez L, Delgado Oliva F, Martínez García R, et al. Prevalencia de la enuresis nocturna en la Comunidad Valenciana. Sección infantil del Estudio Nacional de Incontinencia. Estudio EPICC. Actas Urol Esp. 2009;33:1011-8.
- Semolic N, Ravnikar A, Meglic A, Japelj-Pavesić B, Kenda RB. The occurrence of primary nocturnal enuresis and associated factors in 5-yer-old outpatients in Slovenia. Acta Pediatr. 2009;98:1994-8.
- Sanjuan S, Pérez A, González R, Vargas I, Davara L, Luque M, et al. Enuresis primaria monosintomática. Estudio de 100 casos. Rev Pediatr Aten Primaria. 2000;2:29-45.
- Karni&cbreve;nik K, Koren A, Kos N, Mar&cbreve;un Varda N. Prevalence and quality of life of slovenian children with primary nocturnal enuresis. Int J Nephrol. 2012;2012:509012.
- Hashem M, Morteza A, Mohammad K, Ahmad-Ali N. Prevalence of nocturnal enuresis in school aged children: the role of personal and parents related socioeconomic and educational factors. Iran J Pediatr. 2013;23:59-64.
- Kanaheswari Y. Epidemiology of childhood nocturnal enuresis in Malaysia. J Paediatr Child Health. 2003;39:118-23.
- Carman KB, Ceran O, Kaya C, Nuhoglu C, Karaman MI. Nocturnal enuresis in Turkey: prevalence and accompanying factors in different socioeconomic environments. Urol Int. 2008;80:362-6.
- Lee SD, Sohn DW, Lee JZ, Park NC, Chung MK. An epidemiological study of enuresis in Korean children. BJU Int. 2000;85:869-73.
- Butler RJ, Heron J. The prevalence of infrequent bedwetting and nocturnal enuresis in childhood. A large British cohort. Scand J Urol Nephrol. 2008;42:257-64.
- Wang QW, Wen JG, Song DK, Su J, Zhu QH, Liu K, et al. Bed-wetting in Chinese children: epidemiology and predictive factors. Neurourol Urodyn. 2007;26:512-7.
- Marugán de Miguelsanz JM, Lapeña López de Armentia S, Rodríguez Fernández LM, Palau Benavides MT, Torres Hinojal MC, Menau Martín G, et al. Análisis epidemiológico de la secuencia de control vesical y prevalencia de enuresis nocturna en niños de la provincia de León. An Esp Pediatr. 1996;44:561-7.
- Rodríguez Fernández LM, Marugán de Miguelsanz JM, Lapeña López de Armentia S, Palau Benavides MT, Alvaro Iglesias E, Naveira Gómez C, et al. Estudio epidemiológico sobre enuresis nocturna en escolares: Análisis de factores asociados. An Esp Pediatr. 1997;46:252-8.
- Cohen-Zrubavel V, Kushnir B, Kushnir J, Sadeh A. Sleep and sleepiness in children with nocturnal enuresis. Sleep. 2011;34:191-4.
- Waleed Fe, Samia AF, Samar MF. Impact of sleep-disordered breathing and its treatment on children with primary nocturnal enuresis. Swiss Med Wkly. 2011;141:w13126.
- Martínez García R. Tiempo de reflexión sobre la enuresis. Actas Urol Esp. 2009;33:935-8.




