Vol. 15 - Num. 58
Originales
Evaluación de los conocimientos paternos sobre asma con el Newcastle Asthma Knowledge Questionnaire
M.ª Teresa Leonardo Cabelloa, E Oceja-Setienb, L García Higueraa, M. J. Caberoa, E Pérez Belmontea, I Gómez-Aceboc
aServicio de Pediatría. Hospital Universitario Marqués de Valdecilla. Santander. España.
bGrupo de Medicina Preventiva y Salud Pública. Facultad de Medicina. Universidad de Cantabria. Santander. España.
cGrupo de Medicina Preventiva y Salud Pública. Facultad de Medicina. Universidad de Cantabria. CIBER Epidemiología y Salud Pública (CIBERESP). Instituto de Formación e Investigación Marqués de Valdecilla (IFIMAV). Santander. España.
Correspondencia: MT Leonardo. Correo electrónico: maiteleonardo@hotmail.com
Cómo citar este artículo: Leonardo Cabello MT, Oceja-Setien E, García Higuera L, Cabero MJ, Pérez Belmonte E, Gómez-Acebo I. Evaluación de los conocimientos paternos sobre asma con el Newcastle Asthma Knowledge Questionnaire. Rev Pediatr Aten Primaria. 2013;15:117-26.
Publicado en Internet: 20-06-2013 - Número de visitas: 36492
Resumen
Objetivo: determinar el grado de conocimiento sobre asma de los padres de niños/as asmáticos seguidos en una consulta de Neumología infantil.
Material y método: estudio descriptivo y transversal, mediante encuestas autocumplimentadas. Los conocimientos sobre asma se evaluaron usando el Newcastle Asthma Knowledge Questionnaire (NAQK). Se realizó el cuestionario a padres y otros familiares de niños asmáticos atendidos en la consulta de Neumología infantil de un hospital terciario. Las encuestas fueron realizadas entre septiembre y noviembre de 2009.
Resultados: la muestra quedó conformada por 344 cuestionarios. Un 72,7% fue contestado por la madre del paciente, un 14,9% por el padre, en un 6,7% fueron ambos progenitores los que rellenaron el cuestionario y en un 5,8% fue otra persona diferente. Los pacientes fueron 203 niños (59%) y 141 niñas (41%) con una edad media de 8±4 años. La puntuación media fue de 18,5±3,7 sobre 31.
Conclusiones: nuestros encuestados han obtenido mayor puntuación media en comparación con muestras similares en otros estudios. A pesar de ello, consideramos que una intervención educativa puede mejorar los conocimientos sobre asma y contribuir a disminuir la morbilidad de esta enfermedad crónica.
Palabras clave
● Asma ● Conocimiento de asma ● Cuestionario The Newcastle Asthma Knowledge QuestionnaireINTRODUCCIÓN
El asma es la enfermedad crónica más frecuente en la infancia en los países desarrollados, motivo por el que adquiere una enorme repercusión no solo a nivel individual y familiar, sino también a nivel social y económico1.
El carácter crónico indica que no tiene curación y, por tanto, el objetivo del tratamiento se ciñe a alcanzar un adecuado control de los síntomas, mantener una actividad física y una función pulmonar normales, así como prevenir las reagudizaciones2.
En los últimos años se está insistiendo en la necesidad de la mayor dedicación por parte de los sanitarios hacia los aspectos educativos que, como en toda enfermedad crónica, requiere el asma2.
La mejora en los conocimientos, la adquisición de las habilidades necesarias y el cambio en la actitud y los comportamientos de los pacientes, familiares y cuidadores facilitan una mayor adhesión a los tratamientos y permiten un mejor manejo de los síntomas y de la enfermedad3. Es por eso que las principales guías y consensos de manejo del asma actuales recomiendan la intervención educativa como un pilar más de manejo y tratamiento del asma4-6.
El objetivo de este estudio es determinar el grado de conocimiento sobre el asma y su manejo entre los padres y familiares de niños asmáticos seguidos en nuestra consulta de atención especializada, utilizando para ello una encuesta elaborada y validada con ese fin.
MATERIAL Y MÉTODOS
Estudio descriptivo y transversal, mediante encuestas autocumplimentadas, sobre los conocimientos de asma infantil y su manejo. Se realizó el cuestionario a padres y familiares de niños/as asmáticos atendidos en la Consulta de Neumología infantil del Hospital Universitario Marqués de Valdecilla (Santander, España). Las encuestas fueron realizadas entre los meses de septiembre y noviembre de 2009.
Los conocimientos sobre el asma fueron evaluados usando el Newcastle Asthma Knowledge Questionnaire (NAQK)7, traducido y adaptado al castellano y validado por Praena et al.8.
Este cuestionario consta de 31 ítems y valora conocimientos sobre síntomas, desencadenantes y tratamiento del asma. Tiene 25 preguntas con respuesta tipo verdadero/falso y seis preguntas abiertas.
Las respuestas correctas puntúan 1 y las incorrectas 0. La puntuación total del cuestionario se obtiene sumando la puntuación asignada a cada pregunta. La puntuación final será entre 0 y 31, una mayor puntuación indica un mayor grado de conocimiento.
Las respuestas abiertas del cuestionario fueron interpretadas por dos médicos residentes de Pediatría en su último año de formación, siguiendo de forma uniforme los criterios de valoración del cuestionario.
La pregunta número uno lleva implícito en el texto que la respuesta incluya los tres síntomas principales del asma, por tanto se ha considerado correcta solo cuando estos tres síntomas han sido enumerados.
La respuesta a la pregunta número seis se ha evaluado como correcta si se nombraba al menos uno de los tres desencadenantes que se dan como respuestas posibles.
Las preguntas 10, 11, 21 y 23 se han considerado correctas cuando el encuestado ha contestado al menos dos de las que ofrece el cuestionario como posibles respuestas, tal y como indican las normas de corrección del cuestionario original7,8.
A su llegada al hospital, se entregaba el cuestionario a los padres o familiares que acompañaban al niño/a, para que lo rellenaran en los minutos de espera previos a la consulta. La decisión de rellenar la encuesta era voluntaria y a todos los participantes se les entregó información escrita junto al cuestionario sobre la intención de realizar un estudio con los datos obtenidos.
En cada formulario, además, se pedía al encuestado que anotara de forma voluntaria su parentesco con el niño, su nivel de estudios y si tenía otros hijos asmáticos.
Se recogieron otros datos epidemiológicos, como edad del paciente, tiempo de seguimiento en consulta (desde la fecha de la primera consulta), diagnóstico (según la clasificación de la Guía Española del Manejo de Asma) y si el paciente había tenido ingresos hospitalarios por asma.
Se realizó un análisis descriptivo de todas las variables recogidas. Para las variables numéricas se calculó su media, desviación típica, mediana y rango intercuartílico. Las variables cualitativas se describieron mediante las correspondientes frecuencias y su intervalo de confianza al 95%.
El análisis estadístico de los datos se realizo mediante el programa estadístico SPSS® versión 20.0.
RESULTADOS
Se entregaron 500 cuestionarios, de los que fueron cumplimentados 387, obteniendo un nivel de participación del 77,5%.
Se eliminaron los cuestionarios que no pertenecían a pacientes asmáticos y que acudían a la consulta por otros motivos (fibrosis quística, control posneumonía, bronquiectasias, etc.), así como aquellos que por diferentes motivos habían quedado incompletos.
La muestra quedó conformada por 344 cuestionarios. Fueron los padres quienes cumplimentaron el cuestionario, concretamente un 72,7% fue contestado por la madre del paciente, un 14,9% por el padre, un 6,7% por ambos progenitores y 5,8% por otra persona diferente que acompañaba al niño (en su mayoría abuelas).
Los pacientes fueron 203 niños (59%) y 141 niñas (41%) con una edad media de 8±4 años. En la Tabla 1 se muestran las características principales de la muestra estudiada.
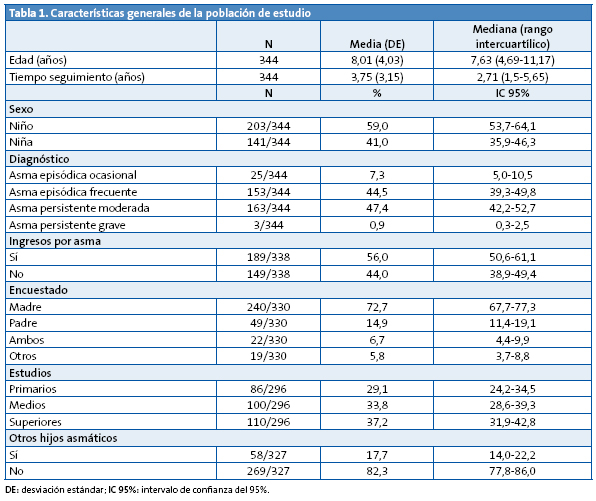
La media de puntuación del cuestionario fue de 18,5±3,7 puntos.
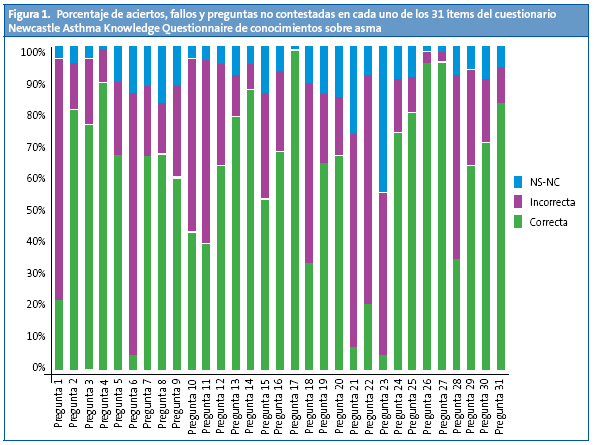
La Fig. 1 muestra el porcentaje de fallos y respuestas no contestadas en el cuestionario.
La Tabla 2 muestra el porcentaje de aciertos de cada uno de los 31 ítems que componen el NAKQ.
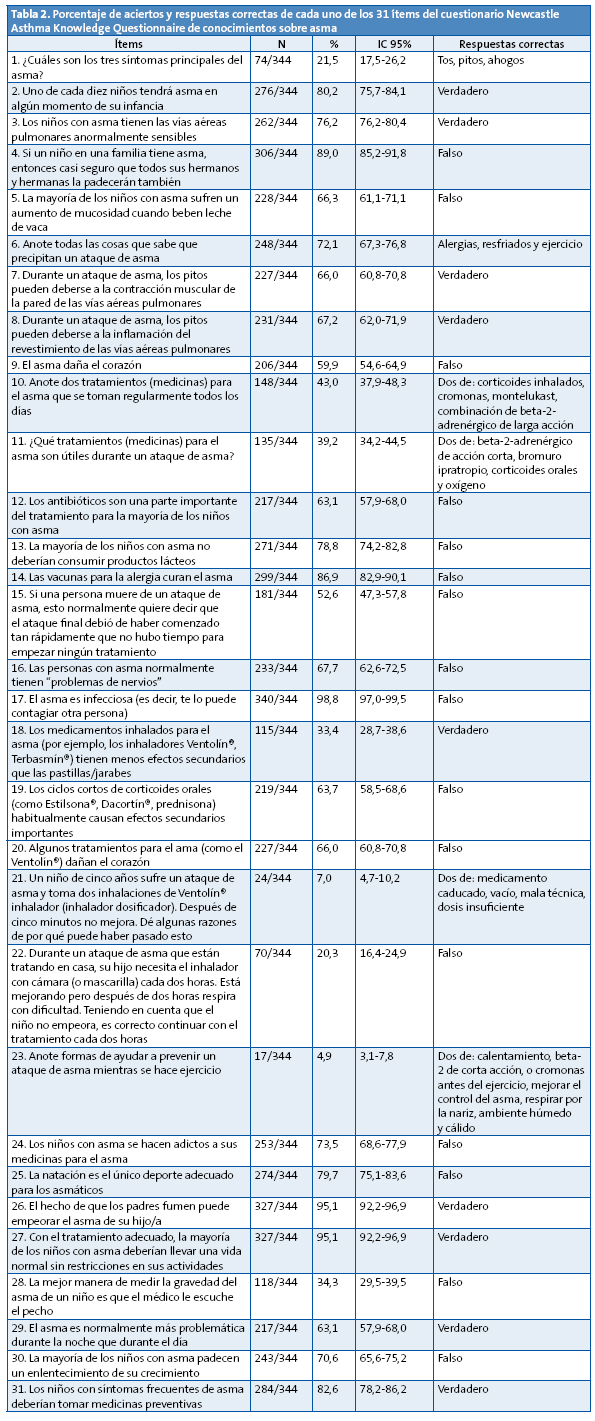
De su análisis detallado podemos decir lo siguiente:
Conocimientos generales sobre el asma (preguntas 1, 2, 3, 25, 26, 28 y 29)
En relación a los conocimientos generales sobre el asma, el 80,2% de los encuestados conoce cuál es la prevalencia del asma en la infancia, el 76,2% sabe que los niños con asma tienen las vías aéreas pulmonares anormalmente sensibles y un 60% afirma que el asma no daña al corazón.
Tan solo un 21,5% de los encuestados es capaz de enumerar los tres síntomas principales en una crisis asmática. En un porcentaje elevado de casos, los padres enumeraron hasta dos síntomas, pero las normas de corrección del cuestionario indican que para que esta respuesta sea válida se tienen que enumerar los tres síntomas (tos, pitos y ahogo).
Un porcentaje muy alto de los encuestados (95,1%) tiene claro que ser fumadores puede empeorar el asma de sus hijos. El 63% sabe que el asma normalmente es más problemática durante la noche que durante el día. Sin embargo, un 65,7% de los padres cree que la mejor manera de medir la gravedad del asma es que un médico le escuche el pecho.
Crisis aguda: reconocimiento, desencadenantes y manejo (preguntas 6, 7, 8, 11, 15, 18, 19, 20, 21, 22 y 23)
En relación a la crisis aguda de asma, solo un 4,4% es capaz de identificar los tres desencadenantes principales de una crisis (resfriados, alergias y ejercicio), pero hasta el 29,6% de encuestados nombra al menos dos de estos desencadenantes. Un 66% sabe que los pitos se deben a la contracción muscular de las vías aéreas pulmonares o bien que pueden deberse a la inflamación del revestimiento de las vías aéreas, como afirma el 67,2% de los encuestados.
En cuanto a su manejo, cabe destacar que tan solo el 39,2% ha contestado correctamente acerca de los fármacos que se usan en una crisis aguda y solo un 5% conoce formas de prevenir un ataque en el caso del asma de esfuerzo.
Solo el 33,4% sabe que los medicamentos inhalados tienen menos efectos secundarios que los orales, un 63,7% conoce que los ciclos cortos de corticoides no tienen efectos secundarios importantes y el 66% afirma que el Ventolín® no daña el corazón.
La pregunta en la que se plantea una crisis aguda de asma que no mejora y se pide razones de ello ha obtenido un nivel de participación muy bajo y un porcentaje de acierto mínimo (7%).
Tratamiento de mantenimiento (preguntas 10, 12, 14, 19, 27 y 31)
Respecto al tratamiento de mantenimiento del asma, el 63,1% sabe que los antibióticos no son una parte importante del tratamiento y un 86,9% tiene claro que las vacunas para la alergia no curan el asma.
En las preguntas referentes a tratamientos aceptamos que respondieran tanto con nombre genérico o principio activo como con nombre de marcas comerciales, pues entendemos que se trata de personal no sanitario. Aun así, son más los padres (hasta un 57%) que no son capaces de indicar dos tratamientos de mantenimiento para el asma, lo cual llama la atención, pues la práctica totalidad de los niños seguidos en la consulta toman en la actualidad o han tomado tratamientos de este tipo. Muchos padres, además, creen que el salbutamol es un tratamiento de mantenimiento en el asma.
El 95% sabe que con el tratamiento adecuado un niño asmático puede llevar una vida normal, sin restricciones, y el 82,6% afirma que los niños con síntomas frecuentes de asma deberían tomar tratamiento preventivo.
Falsos mitos (preguntas 4, 5, 9, 13, 16, 17, 24 y 30)
En relación a mitos o creencias en torno al asma, el 66,3% de los encuestados sabe que los niños con asma no sufren un aumento de mucosidad cuando beben leche de vaca y, por tanto, el 78,8% tiene claro que pueden tomarla.
El 67,7% sabe que los asmáticos normalmente no tienen problemas de nervios, el 70,6% que no padecen un enlentecimiento de su crecimiento y un 73,5% niega que los niños asmáticos se hagan adictos a sus medicinas.
Prácticamente la totalidad de los encuestados (98,8%) sabe que la etiología del asma no es infecciosa.
DISCUSIÓN
Existen varios estudios en España que utilizan el cuestionario NAKQ traducido y adaptado al español por el profesor Praena et al.8 para evaluar los conocimientos sobre distintos aspectos del asma en padres y profesores9-12.
En nuestro estudio utilizamos este mismo cuestionario traducido al español en padres/madres de niños asmáticos. La puntuación media obtenida fue de 18,5 puntos, superior a la obtenida por los profesores (17,9 puntos), los adolescentes asmáticos (17,24 puntos) y los no asmáticos (16,23 puntos) del estudio sobre asma en centros escolares de Praena9 y también superior a la media de puntuación obtenida por los profesores del Estudio sobre el Asma en los Centros Escolares Españoles (EACEE)11 (16 puntos).
Algunos estudios en otros países, utilizando el mismo cuestionario en adolescentes asmáticos12 y en profesores13, obtuvieron también puntuaciones menores.
En el estudio original de validación del cuestionario, realizado en el año 1990 por Fitzclarence y Henry7, se reclutaron dos grupos de encuestados con alto y bajo conocimiento en asma, cuyas puntuaciones medias en el cuestionario fueron de 25 y 13 puntos, respectivamente.
En comparación con el estudio que se realizó para la validación de la traducción a nuestro idioma del cuestionario8, en una población de padres con altos conocimientos sobre la enfermedad (padres de niños con asma que se habían beneficiado de una intervención educativa), frente a padres con bajos conocimientos de la enfermedad (padres sin relación con la enfermedad ni con sus tratamientos), la puntuación que obtuvieron fue de 23 y 16,8, respectivamente. Por consiguiente, los resultados obtenidos por los padres de nuestro estudio se encuentran en un nivel intermedio respecto a los padres con alto y bajo conocimiento de los estudios de Praena8 y Fitzclarence7.
Un estudio realizado en Malasia en el año 2002 muestra resultados de puntuación del cuestionario NAKQ en padres de niños asmáticos que ingresaban en el hospital por una agudización14. Esta muestra de padres obtuvo una puntuación más baja (15,5 puntos) que los de nuestro estudio. También en el estudio de Henry15 los padres obtuvieron puntuaciones menores.
En el reciente estudio de García Luzardo16 realizado a padres de niños asmáticos con una crisis aguda en un Servicio de Urgencias, la puntuación media obtenida del cuestionario NAKQ fue de 16,14, un valor inferior en comparación con nuestros resultados.
Por tanto, en relación con otros estudios realizados en padres de niños asmáticos, nuestra muestra de padres tiene un mayor conocimiento, reflejado en unas puntuaciones mayores en el cuestionario. Aun así, llama la atención que, a pesar de tratarse de un grupo de pacientes seguidos en una consulta de atención hospitalaria especializada y que a priori podría sobreentenderse un mayor tiempo de evolución de la enfermedad y/o nivel de gravedad, en algunos aspectos su nivel de conocimiento acerca del asma es escaso y francamente mejorable.
En relación a la pregunta 10, un 43% identificó correctamente dos medicinas que se utilizan como tratamiento preventivo del asma, cifra superior a la obtenida en el EACEE11, que fue de un 3%, en el estudio de Korta10, que fue del 2,6% de los profesores, y a la obtenida por alumnos y profesores del estudio de Praena9. En cierto modo, es lógico que la puntuación obtenida por los padres de nuestro estudio sea superior a la obtenida por los profesores del resto de los estudios mencionados, porque esta medicación se administra principalmente en casa y fuera del horario escolar.
Ocurre lo mismo en relación al tratamiento necesario en una crisis de asma. En nuestro estudio, lo conocía un 39,2% de los padres encuestados, cifra también superior al 8,6 del EACEE, al 11% de Korta y al 7,9% de los profesores del estudio de Praena 2012.
Nos parece interesante aportar a la literatura los resultados obtenidos con este cuestionario sobre conocimiento del asma en una muestra amplia de padres de niños asmáticos, pues en España el NAKQ ha sido utilizado sobre todo para evaluar conocimientos en personal docente9-11. De esta manera, aportamos datos con los que poder comparar otras muestras de padres en condiciones similares.
Acerca del cuestionario: puntos fuertes y débiles del cuestionario
El uso de cuestionarios validados es importante para poder realizar comparaciones entre diferentes estudios17.
Existen varios cuestionarios creados para analizar los conocimientos en asma17-19. El NAKQ ha probado ser un instrumento válido para evaluar los conocimientos sobre asma en padres y cuidadores de pacientes asmáticos7,8.
La accesibilidad al cuestionario NAKQ ha sido fácil y barata, pues se encuentra en la red y es de distribución gratuita.
Hemos encontrado dificultades en la interpretación de algunas preguntas y, en nuestra opinión, su respuesta no refleja el mayor o menor nivel de conocimiento por parte de los encuestados, se trata de las preguntas 15 y 22.
Hay que tener en cuenta que el nivel cultural influye como factor independiente en el número de respuestas acertadas, tal y como se demuestra en los trabajos de validación del cuestionario, tanto en inglés7 como en español8.
Además, en el artículo original existen hasta cinco preguntas (4, 7, 17, 36 y 27) en las que tras el análisis no se encuentran diferencias estadísticamente significativas entre los grupos de alto y bajo conocimiento de asma. Lo mismo ocurre en el estudio de validación al español, donde el número de ítems en los que no se encuentran diferencias significativas asciende hasta diez (preguntas 2, 3, 4, 7, 17, 22, 26, 28, 29 y 30). Tal y como recomiendan los autores de ambos artículos, sería deseable realizar una revisión del cuestionario con el fin de mejorarlo y eliminar algunas preguntas que no parecen ser discriminativas.
Cabe destacar que, tanto en nuestro trabajo como en todos los estudios publicados que han utilizado este cuestionario9-13, las preguntas abiertas (1, 6, 10, 11, 21 y 23), referidas a los principales síntomas de asma, medicación a administrar y la actitud ante una crisis o ante el ejercicio, fueron las que obtuvieron menor tasa de respuestas correctas (Fig. 1). Esto puede deberse a la mayor dificultad que plantea a priori una pregunta abierta con respecto a una respuesta dicotómica o incluso a respuestas de tipo elegir opciones como demuestra el estudio realizado por Bruzzesse20, en el que los padres fueron capaces de identificar un mayor número de desencadenante de una crisis asmática al plantearles diferentes opciones que ellos tenían que elegir en lugar de ser una cuestión abierta.
En nuestro estudio, solo un 21,5% fue capaz de identificar los tres síntomas principales del asma, un porcentaje bastante superior al 8,6% obtenido por los profesores del EACEE y al 3,4% obtenido por los profesores antes de una intervención educativa del estudio de Korta10, y muy similar (20,8%) al de los profesores del estudio de Praena9 y a los publicados en el artículo de Gibson12 (21,7%).
Sin embargo, nuestra cifra es menor que el 45,3% obtenido por los padres del estudio de Bell18, lo que puede deberse a una diferencia de criterios a la hora de corregir.
Nuestras conclusión principal tras el análisis de los resultados es que, aunque en comparación con la mayoría de los estudios realizados en condiciones similares nuestros encuestados tienen mayor nivel de conocimiento acerca del asma –reflejado en una puntuación media mayor–, deberíamos centrar parte de nuestra atención en realizar una mayor intervención educativa al paciente asmático y a sus cuidadores, lo que probablemente llevaría a mejorar el control de su enfermedad, con menos recaídas, menos ingresos hospitalarios y, en definitiva, una mejora en la calidad de vida de estos pacientes.
AGRADECIMIENTOS
Agradecemos la colaboración de los padres de los niños seguidos en nuestra consulta que rellenaron las encuestas, así como al resto de personal que colaboró durante la entrega y recogida de las mismas.
Agradecemos también al Dr. Praena et al. la amabilidad que mostraron permitiendo el uso del cuestionario.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo.
ABREVIATURAS: EACEE: Estudio sobre el Asma en los Centros Escolares Españoles • NAQK: Newcastle Asthma Knowledge Questionnaire.
BIBLIOGRAFÍA
- Masoli M, Fabian D, Holt S, Beasley R. Global burden of asthma. Developed for the global initiative for asthma. Medical Research Institute of New Zealand. Wellington, New Zealand 2006 [en línea] [actualizado en noviembre de 2011; consultado el 19/04/2013]. Disponible en www.ginasthma.org/local/uploads/files/GINABurdenReport_1.pdf
- Korta Murua J, López-Silvarrey Varela A. Asma, educadores y escuela. An Pediatr (Barc). 2011;74(3):141-4.
- Korta Murua J, Valverde Molina P, Praena Crespo M, Figuerola Mulet J, Rodríguez Fernández-Oliva CR, Rueda Esteban S, et al. La educación terapéutica en el asma. An Pediatr (Barc). 2007;66:496-551.
- National Hearth Lung and Blood Institute, National Asthma Education and Prevention Program. Expert Report 3 (NAEP EPR-3). Guidelines for the Diagnosis and Management of Asthma. Bethesda, MD: National Institute of Health, 2007 [en línea] [consultado el 19/04/2013]. Disponible en www.nhlbi.nih.gov/guidelines/asthma/asthgdln.htm
- Global Initiative for Asthma (GINA). Global Strategy for Asthma Management and Prevention. Updated 2009 [en línea] [consultado el 19/04/2013]. Disponible en www.ginasthma.org
- Castillo Laita LA, de Benito Fernández FJ, Escribano Montaner A, Fernández Benítez P, García de la Rubia S, Garde Garde, et al. Consenso sobre el tratamiento del asma en pediatría. An Pediatr (Barc). 2007;67:257-73.
- Fitzclarence CA, Henry RL. Validation of an asthma knowledge questionnaire. J Paediatr Child Health. 1990;26:200-4.
- Praena Crespo M, Lora Espinosa L, Aquino Linares N, Sánchez Sánchez A, Jiménez Cortés A. Versión española del NAKQ. Adaptación transcultural y análisis de fiabilidad y validez. An Pediatr (Barc). 2009;70:209-17.
- Praena Crespo M, Fernández Truan JC, Aquino Llinares N, Murillo Fuentes A, Sánchez Sánchez A, Gálvez González J, et al. Situación de los conocimientos, las actitudes y la calidad de vida en asma de adolescentes y profesorado. Necesidad de educar en los centros de enseñanza. An Pediatr (Barc). 2012;77(4):236-46.
- Korta Murua J. Impacto de una intervención educativa sobre asma en los profesores. An Pediatr (Barc). 2012;77(4):226-35.
- López-Silvarrey Varela A. Estudio sobre el asma en los centros escolares españoles (EACEE) 2009-2010. A Coruña: Fundación María José Jove; 2011 [en línea] [consultado el 19/04/2013]. Disponible en www.fundacionmariajosejove.org/media/upload/files/Maqueta_final_publicacin_resultados_Estudio_Asma_Nacional_FMJJ_FBBVA_en_11.pdf
- Gibson PG, Henry RL, Vimpani GV, Halliday J. Asthma knowledge, attitudes, and quality of life in adolescents. Arch Dis Child. 1995;73:321-6.
- Henry RL, Gibson PG, Vimpani GV, Francis JL, Hazell J. Randomized controlled trial of a teacher-led asthma education program. Pediatr Pulmonol. 2004;38:434-42.
- Fadzil A, Norzila MZ. Parental Asthma Knowledge. Med J Malaysia. 2002;57:474-81.
- Henry RL, Cooper DM, Halliday JA. Parental asthma knowledge: its association with readmission of children to hospital. J Paediatr Child Health. 1995;31:95-8.
- García-Luzardo MR, Aguilar-Fernández AJ, Rodríguez-Calcines N, Pavlovic-Nesic S. Conocimientos acerca del asma de los padres de niños asmáticos que acuden a un servicio de urgencias. Acta Pediatr Esp. 2012;70(5):196-203.
- Rodríguez Martínez C, Sossab MP. Validación de un cuestionario de conocimientos acerca del asma entre padres o tutores de niños asmáticos. Arch Bronconeumol. 2005;41:419-24.
- Bell HM, Mcelnay JC, Hughes CM, Gleadhill I. Primary schoolteachers' knowledge of asthma: the impact of pharmacist intervention. J Asthma. 2000;37:545-55.
- Clark NM, Mitchell HE, Rand CS. Effectiveness of educational and behavioral asthma interventions. Pediatrics. 2009;123(suppl 3):S185-S192.
- Bruzzese JM, Unikel LH, Evans D, Bornstein I, Surrence K, Mellins RB. Asthma knowledge and asthma management behaviour in urbanelementary school teachers. J Asthma. 2010;47:185-91.




