Vol. 21 - Num. 83
Originales
Salidas laborales de los residentes de Pediatría. Datos del periodo 2014-2017
María Álvarez Casañoa, Pedro J. Gorrotxategi Gorrotxategib, Lourdes Castillo Camposc, Amaia Cámara Oteguid, Rocío Martín Moyae, Talía Fuentes Redondof, María Letona Luquig
aPediatra. CS Alcolea. Córdoba. España .
bPediatra. CS Pasaia San Pedro. Pasajes. Guipúzcoa. España.
cMIR-Pediatría. Hospital Clínica Benidorm. Benidorm. Alicante. España.
dMIR-Pediatría. Hospital Universitario Donostia. San Sebastián. Guipúzcoa. España.
eMIR-Pediatría. Hospital Materno-Infantil de Jaén. Jaén. España.
fMIR-Pediatría. Complejo Hospitalario de Toledo. Hospital Virgen de la Salud. Toledo. España.
gCAP de Usurbil. Usurbil. Gipuzkoa. España.
Correspondencia: PJ Gorrotxategi. Correo electrónico: pedro.gorrotxa@gmail.com
Cómo citar este artículo: Álvarez Casaño M, Gorrotxategi Gorrotxategi PJ, Castillo Campos L, Cámara Otegui A, Martín Moya R, Fuentes Redondo T, et al. Salidas laborales de los residentes de Pediatría. Datos del periodo 2014-2017. Rev Pediatr Aten Primaria. 2019;21:247-53.
Publicado en Internet: 06-09-2019 - Número de visitas: 12287
Resumen
Introducción: dada la escasez de pediatras de nuestro sistema de salud y la necesidad de estos en Atención Primaria, donde cerca del 25% de las plazas están ocupadas por no especialistas en Pediatría, se quiso conocer el destino laboral inicial de los residentes que habían finalizado su periodo de formación en los últimos cuatro años.
Metodología: se han recogido las salidas laborales de los residentes que han finalizado su periodo de rotación durante los años 2014-2017 en los hospitales españoles. La recogida se ha realizado por medio de los representantes de residentes de las comunidades autónomas y los vocales autonómicos de la Asociación de Pediatría de Atención Primaria.
Resultados: se han recogido datos de las salidas laborales del 75,7% de los residentes, lo que supone conocer el destino laboral de 1263 residentes de los últimos cuatro años. La elección de Atención Primaria en el transcurso de estos años ha disminuido del 30,77 al 24,5%; igualmente han disminuido los trabajos en hospitalización o consultas hospitalarias que han descendido de un 43,8 a un 32,85%, mientras que la realización de guardias o cobertura de Urgencias ha aumentado y también ha subido el porcentaje de los que se dedican a la medicina privada.
Conclusiones: el porcentaje de residentes que acude a Atención Primaria es insuficiente. El trabajo del pediatra está siendo de peor calidad, con aumento de los contratos de guardias y Urgencias. Está aumentando el porcentaje de residentes que se dirigen hacia la sanidad privada.
Palabras clave
● Atención Primaria ● Residentes ● Salidas profesionalesINTRODUCCIÓN
Desde hace años se ha constatado un déficit de pediatras en Atención Primaria. Una proporción de las consultas de Pediatría de Atención Primaria están cubiertas por médicos no especialistas en Pediatría. Eso lleva a una atención no especializada en el primer nivel asistencial que podría tener sus repercusiones en el cuidado infantil1. El déficit se había estimado en cerca de un 30%2, aunque un estudio reciente lo sitúa en el 25,1%3.
Conocedora de esta situación, la Asociación Española de Pediatría de Atención Primaria, su vocalía de residentes y su grupo de trabajo laboral-profesional se propusieron conocer el destino laboral de los residentes de Pediatría de los últimos años.
Este trabajo se inició en 2017, recogiendo los datos de los tres años anteriores, y se presentó como comunicación tipo póster en el 65.º Congreso de la Asociación Española de Pediatría4. Ese primer análisis se continuó con un seguimiento en la recogida de datos5 que es lo que se presenta en el presente estudio.
RESULTADOS
Se han recogido datos de las salidas laborales del 74% de los residentes que han finalizado su periodo de formación, lo que supone conocer el destino laboral de 1668 residentes de los últimos cuatro años (Tabla 1).
| Tabla 1. Datos sobre el porcentaje de salidas laborales de los residentes obtenidas | |||
|---|---|---|---|
| Año | Número de plazas de MIR | Datos obtenidos | Porcentaje |
| 2014 | 419 | 278 | 66% |
| 2015 | 418 | 307 | 73% |
| 2016 | 413 | 331 | 80% |
| 2017 | 418 | 347 | 83% |
| Total | 1668 | 1263 | 75,7% |

La elección de Atención Primaria como salida profesional en el transcurso de estos años ha disminuido del 30,77 al 24,5% (más de un 6%); igualmente han disminuido los trabajos en hospitalización o consultas hospitalarias, que de un 43,8 han bajado a 32,85% (un 11%), mientras que la realización de guardias o cobertura de Urgencias ha aumentado: comparando los dos primeros años con los dos últimos una media del 8,5% y también aumenta el porcentaje de los que orientan su labor profesional a la medicina privada en un 7%. En cuanto a la media de los cuatro años, la salida laboral más frecuente es la hospitalaria (37%), seguida de Atención Primaria (28%) y las Urgencias o guardias (15,5%) (Tabla 2).
| Tabla 2. Salidas profesionales de los residentes de Pediatría del 2014 al 2017 | ||||||
|---|---|---|---|---|---|---|
| Atención Primaria | Urgencias, guardias | Unidades de hospitalización | Formación: máster, becas, etc. | Medicina privada | Otros | |
| 2014 | 30,77 | 8,36 | 43,81 | 2,34 | 3,01 | 4,68 |
| 2015 | 30,29 | 15,96 | 41,69 | 6,19 | 6,19 | 2,61 |
| 2016 | 26,20 | 23,79 | 30,42 | 10,84 | 3,01 | 5,12 |
| 2017 | 24,5 | 17,5 | 32,2 | 8,5 | 10,7 | 6,6 |
| Media | 27,94 | 15,50 | 37,03 | 6,97 | 5,73 | 4,75 |

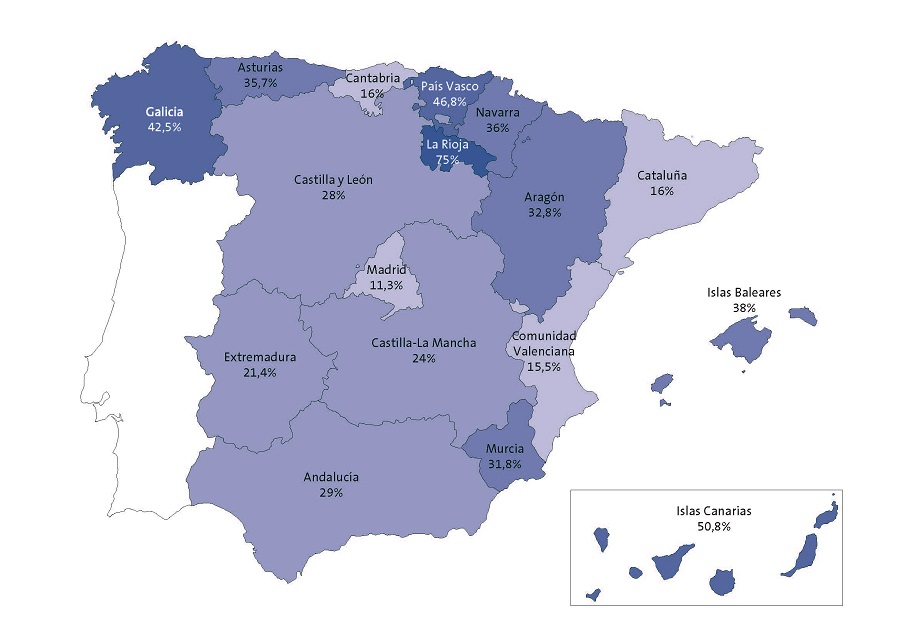
En cuanto a la situación de las salidas de Atención Primaria en las diversas comunidades autónomas, existen notables diferencias entre unas y otras. Varía entre el 75% de la Rioja y el 11,3% de Madrid, con una media del 27,94% (Fig. 1).
DISCUSIÓN
Se va a tratar de responder a tres preguntas: ¿existe demanda de formación en Pediatría?, ¿dónde hay más necesidad de pediatras, en los hospitales o en Atención Primaria? y ¿podría la enfermería pediátrica colaborar en la solución del problema?
¿Existe demanda de formación en la especialidad de Pediatría?
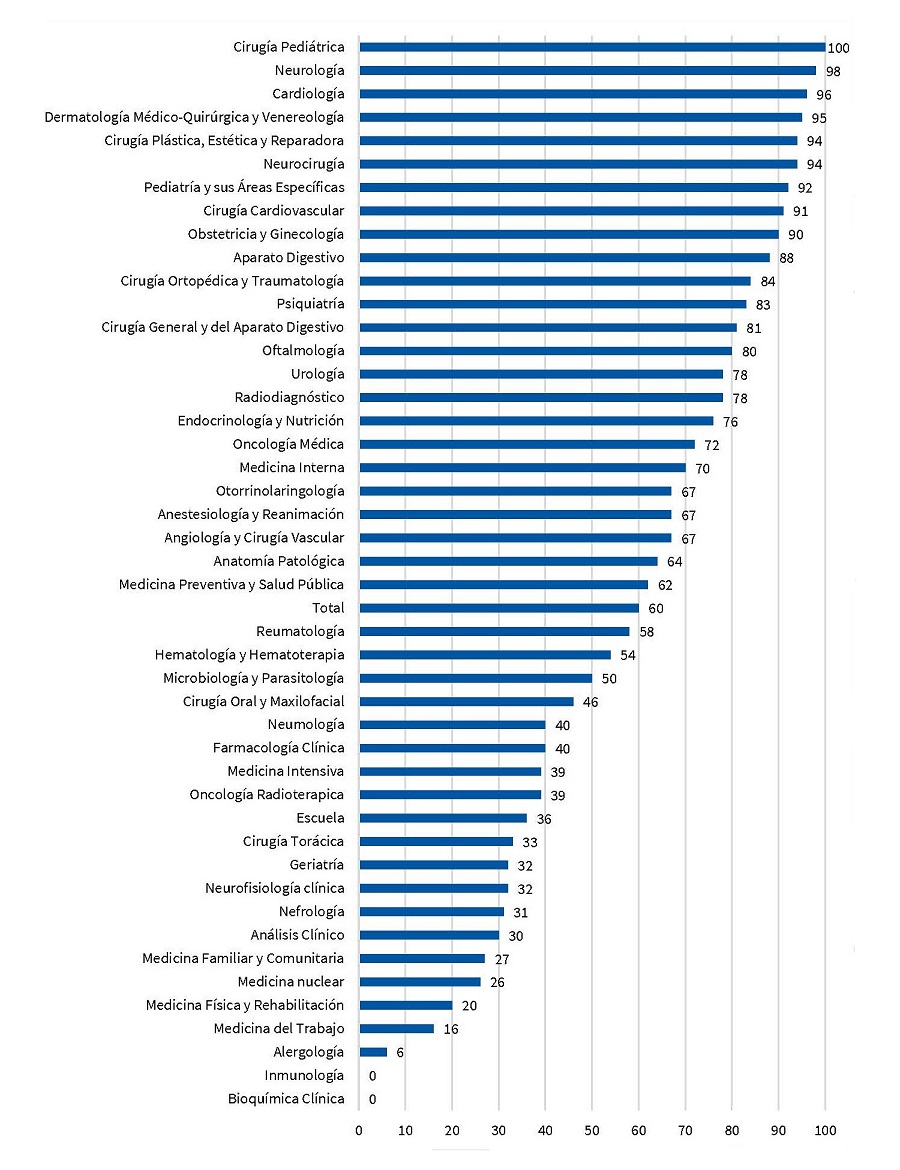
Según el informe descriptivo de la encuesta MIR R1 20146, se considera “éxito del sistema de adjudicación” al porcentaje de individuos que han podido elegir su especialidad preferida. Para ello, se plantean qué especialidad y centro hubieran elegido de no tener ninguna restricción de nota, es decir, como si eligieran con todas las plazas y centros disponibles. En el caso de la Pediatría, la tasa de éxito es del 92%, y se encuentra un déficit de plazas de forma que hubiese sido elegida en mayor proporción si hubiera plazas disponibles, la séptima de todas las especialidades (Fig. 2).
| Figura 2. Porcentaje de elección de la especialidad preferida, según especialidad |
|---|
 |

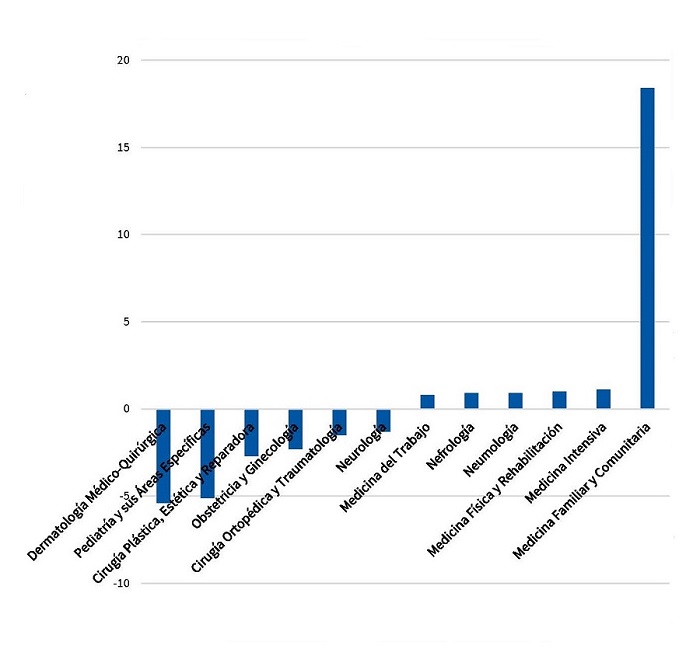
Otro aspecto que se analiza este estudio es la diferencia entre las plazas deseadas y las elegidas. Hay cinco especialidades en las que se cogerían más plazas, y de ellas la segunda especialidad con más déficit de residentes, un 5,1, es la Pediatría (Fig. 3), solo por debajo de Dermatología, que es la más demandada, de forma que si se ofrecieran más plazas se cubrirían todas con satisfacción para los residentes.
| Figura 3. Déficit-superávit: diferencia porcentual plazas MIR 2013-2014 elegidas y deseadas |
|---|
 |

¿Dónde hay más necesidad de pediatras, en los hospitales o en Atención Primaria?
Para ver si se adecuan las salidas profesionales a las necesidades de pediatras se tendrá en cuenta el número de puestos de trabajo en cada ámbito y las salidas profesionales que se han observado. En España hay, según datos oficiales de 2016, 6410 pediatras en Atención Primaria7 y 4154 en Atención Hospitalaria8, lo que supone respectivamente el 60,7 y el 39,3% respectivamente. Esto contrasta con las salidas profesionales de los pediatras, que son en el sentido opuesto: el 52% se queda en el hospital, y el 28% va a Atención Primaria, con lo que el problema de déficit de pediatras en Atención Primaria se irá agravando.
En una encuesta realizada a residentes de todo el Estado9, el 75% piensan que trabajarán en Atención Primaria, un 43% lo desean y a un 55% no les importaría hacerlo. Los problemas que observan del trabajo de Primaria son la escasez de pruebas diagnósticas (30%), la excesiva demanda por parte de los padres en patologías banales (20%) y el deseo de continuar haciendo guardias (20%).
Hay también residentes que se sienten entusiasmados por la Atención Primaria. Uno de ellos titulaba así su intervención en una reunión de la AEPap: “El residente de Pediatría: entusiasmo por la Atención Primaria”10, y decía: “mi entusiasmo es quizá porque supone una atención integral al paciente, al mismo tiempo que te hace partícipe de crecimiento y desarrollo y se puede seguir el rumbo de los niños de ‘tu cupo’, conociendo sus características personales y familiares; de forma que se genera más confianza en la relación médico-paciente y una mayor implicación entre ambos”.
¿Podría la enfermería pediátrica colaborar en la solución del problema?
A pesar de que en 2010 se realizó el plan de formación de enfermería pediátrica y se definió su perfil profesional, que consistía en “proporcionar cuidados de enfermería especializados de forma autónoma, durante la infancia y adolescencia, en todos los niveles de atención, incluyendo la promoción de la salud, la prevención de la enfermedad y la asistencia al recién nacido, niño o adolescente sano o enfermo y su rehabilitación”11, su presencia en nuestro sistema sanitario es muy escaso.
Así, en una encuesta realizada a nivel nacional, llama la atención que en Andalucía no exista la enfermería con dedicación preferente a niños y en Madrid solo en entre el 30 y 50% de los cupos. En el País Vasco y Murcia este porcentaje sigue siendo escaso, del 50-70%. En Aragón, Castilla-La Mancha, Galicia, Extremadura, La Rioja, Navarra y Valencia es del 70-90% y en Galicia es del 81%. En Navarra, la mayoría de los cupos pediátricos tiene asignada una enfermera específica, salvo en algunos pueblos pequeños donde una parte del tiempo ve niños y otra adultos. Y, por último, en Castilla y León, Cataluña, Baleares, Canarias y Asturias la gran mayoría de consultas de Pediatría (más del 90%) cuenta con el apoyo de una enfermera con dedicación infantil exclusiva12. Con lo que en el momento actual la colaboración en la asistencia infantil es limitada.
En España, según el informe 201613, la Atención Primaria cuenta con 34 888 médicos y 29 441 enfermeras. Debería haber 0,8 enfermeras por pediatra de Atención Primaria, lo que no se cumple en casi en ninguna de las autonomías.
El número de plazas de enfermería pediátrica convocadas anualmente son alrededor de 13014, cuyo destino es tanto la Atención Hospitalaria como la Atención Primaria, lo que es claramente insuficiente para las necesidades de enfermería especializada.
También existe una discrepancia entre la enfermería que atiende exclusivamente a niños, enfermería pediátrica, y la que atiende también a pacientes adultos, enfermería de familia o mixta. En un estudio en el que participaron 34 enfermeros, 11 pediatras y 1004 padres y madres de niños, el 99,6% de las madres o padres encuestados prefiere un enfermero con dedicación exclusiva a los niños. La totalidad de los pediatras opinó en el mismo sentido. En cuanto a la enfermería, solo siete (20,6%) prefieren un sistema de organización mixto (enfermería de familia), con lo que se puede concluir que, en este estudio, una mayoría cualificada de los profesionales y la población prefiere un modelo de enfermería pediátrica específica15.
CONCLUSIONES
El porcentaje de residentes que acude a Atención Primaria es insuficiente. El trabajo de pediatra está siendo de peor calidad, con aumento de los contratos de guardias y Urgencias. Está aumentando el porcentaje de residentes que se dirigen hacia la sanidad privada.
La única salida para el problema del déficit de pediatras es aumentar las plazas de formación MIR y, en el caso de la Atención Primaria, hacer más atractivas las plazas para los residentes que finalizan el periodo de formación en Pediatría y sus Áreas Específicas.
CONFLICTO DE INTERESES
Los autores declaran no presentar conflictos de intereses en relación con la preparación y publicación de este artículo. La información que recoge fue parcialmente presentada como comunicación oral al 66.º Congreso de la Asociación Española de Pediatría, celebrado en Zaragoza los días 6-9 de junio de 2018.
BIBLIOGRAFÍA
- Buñuel Álvarez JC, García Vera C, González Rodríguez P, Aparicio Rodrigo M, Barroso Espadero D, Cortés Marina BR, et al. ¿Qué profesional médico es el más adecuado para impartir cuidados en salud a niños en Atención Primaria en países desarrollados? Revisión sistemática. Rev Pediatr Aten Primaria. 2010;12:s9-s72.
- Comité Ejecutivo de la AEP. Construyendo la Pediatría del futuro. En: Asociación Española de Pediatría [en línea] [consultado el 03/09/2019]. Disponible en www.aeped.es/sites/default/files/noticiasaep/noticiasaep.62.3.pdf
- Gorrotxategi Gorrotxategi P, García Vera C, Graffigna Lojendio A, Sánchez Pina C, Palomino Urda N, Rodríguez Fernández-Oliva CR, et al. Situación de la Pediatría de Atención Primaria en España en 2018. Rev Pediatr Aten Primaria. 2018;20:e89-e104.
- Castillo Campos L, Gorrotxategi Gorrotxategi P, Cámara Otegi A, Muñoz Calonge A, Lasa Aransti A, Laka Iñurrategi A. ¿A dónde van los residentes cuando terminan su periodo de formación? En: 65.º Congreso de la AEP [en línea] [consultado el 03/09/2019]. Disponible en www.congresoaep.org/AEP2017
- Álvarez Casaño M, Gorrotxategi Gorrotxategi P, Castillo Campos L, Martín Moya MR, Fuentes Redondo T. Salidas laborales de los residentes de Pediatría. Datos 2014-2017. En: 66.º Congreso de la AEP [en línea] [consultado el 03/09/2019]. Disponible en www.congresoaep.org/AEP2018
- Grupo de Investigación EcoSalud de la Universidad de Las Palmas de Gran Canaria. Tercer Informe descriptivo de la encuesta MIR-R1. Convocatoria 2013-2014. En: Ministerio de Sanidad, Servicios Sociales e Igualdad [en línea] [consultado el 03/09/2019]. Disponible en www.mscbs.gob.es/profesionales/formacion/necesidadEspecialistas/doc/ACT2015InforDesMIR_convocatoria_2013_14.pdf
- Portal Estadístico. Área de Inteligencia de Gestión. Sistema de Información de Atención Primaria (SIAP). En: Ministerio de Sanidad, Consumo y Bienestar Social [en línea] [consultado el 03/09/2019]. Disponible en http://pestadistico.inteligenciadegestion.msssi.es/publicoSNS/comun/Cubo.aspx?IdNodo=6407
- Portal Estadístico. Sistema de Información de Atención Especializada (SIAE). Actualizado el 22/06/2018 -Datos desde 2010 en adelante. En: Ministerio de Sanidad, Consumo y Bienestar Social [en línea] [consultado el 03/09/2019]. Disponible en http://pestadistico.inteligenciadegestion.msssi.es/publicoSNS/comun/Cubo.aspx?IdNodo=140
- Álvarez Casaño M, Castillo Campos L, Gorrotxategi Gorrotxategi P, García Uzquiano R, Igarzabal Irizar A, Berridi Etxeberria A. ¿Qué opinan los residentes de la rotación por Atención Primaria? En: 66.º Congreso de la AEP [en línea] [consultado el 03/09/2019]. Disponible en www.congresoaep.org/AEP2018
- López García R. El residente de Pediatría: entusiasmo por la Atención Primaria. Rev Pediatr Aten Primaria. 2012;14:s71-6.
- Orden SAS/1730/2010, de 17 de junio, por la que se aprueba y publica el programa formativo de la especialidad de Enfermería Pediátrica. BOE 157, de 29 de junio de 2010, páginas 57251 a 57276. Disponible en: www.boe.es/diario_boe/txt.php?id=BOE-A-2010-10365
- Sánchez Pina C, Palomino Urda N, de Frutos Gallego E, Valdivia Jiménez C, Rodríguez Fernández-Oliva CR, Miranda Berrioategortua I, et al. “Puntos negros” de la asistencia a la población infantojuvenil en Atención Primaria en España (primera parte). Rev Pediatr Aten Primaria. 2011;13:15-31.
- Informe anual del Sistema Nacional de Salud 2016. En: Ministerio de Sanidad, Servicios Sociales e Igualdad [en línea] [consultado el 03/09/2019]. Disponible en www.msps.es/estadEstudios/estadisticas/sisInfSanSNS/tablasEstadisticas/InfAnualSNS2016/Resumen.pdf
- El EIR 2019 ya tiene propuesta oficial: estas son todas las plazas. En: Redacción Médica [en línea] [consultado el 03/09/2019]. Disponible en www.redaccionmedica.com/secciones/formacion/el-eir-2019-ya-tiene-propuesta-oficial-estas-son-todas-las-plazas-8871
- García Callejo V, Domínguez Pérez L. Enfermería pediátrica versus Enfermería de familia; opiniones de los profesionales y los padres de los niños de San Sebastián de los Reyes (Madrid). Rev Pediatr Aten Primaria. 2012;14:27-30.
Comentarios
Este artículo aún no tiene comentarios.